
Table of Contents
Opioids are a class of drugs primarily used to treat moderate to severe pain. They are naturally found in the opium poppy plant. Some opioid medications are made from the plant directly. Others are, however, made by scientists in laboratories.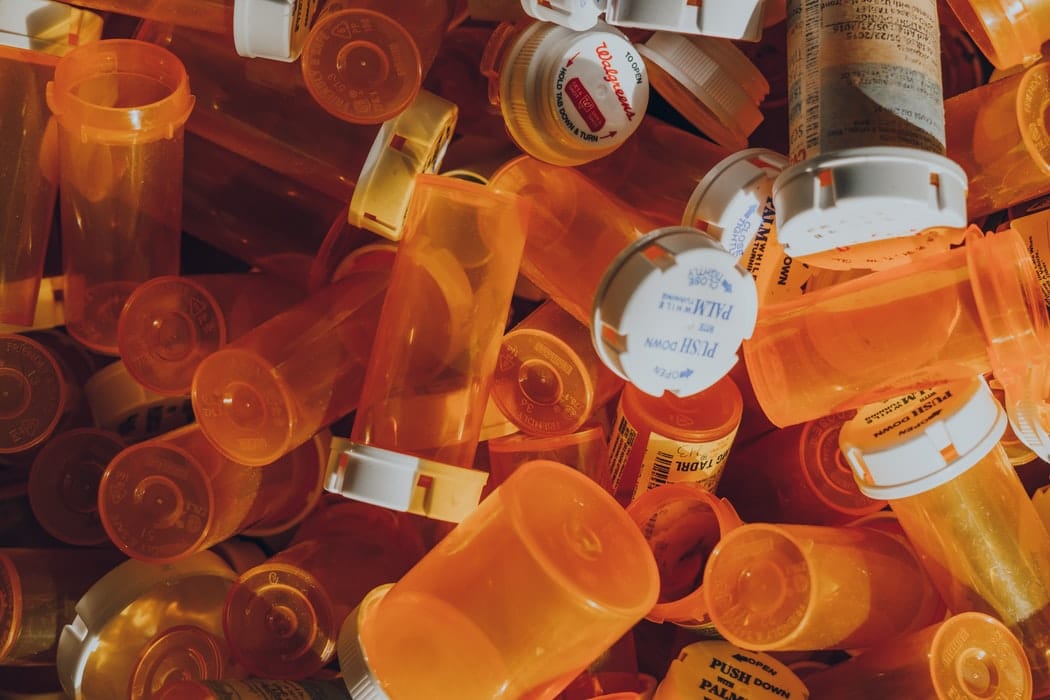 These drugs act on opioid receptors to produce different effects. Opioid receptors are found in the brain, spinal cord, and the gastrointestinal tract (gut). They are often referred to as narcotics.
These drugs act on opioid receptors to produce different effects. Opioid receptors are found in the brain, spinal cord, and the gastrointestinal tract (gut). They are often referred to as narcotics.
Opioids can be prescription medications or street drugs. Those prescribed by healthcare professionals are often called “painkillers.” Examples are hydrocodone and oxycontin. On the contrary, street opioids do not come as a prescription. Heroin is an example of a street opioid.
Prescription opioids block pain signals between the brain and the body. They are typically used to treat moderate to severe pain. Though helpful, these medications also have side effects.
In addition to helping with pain, this substance can cause a “high.” This effect is known as euphoria. Unfortunately, some people use these drugs for this effect. Over time, addiction can become a problem. Dependence on opioids, therefore, makes overdoses a risk. As is well documented, the opioid epidemic remains a huge problem in the United States.
According to the Centers for Disease Control and Prevention (CDC), opioid overdose deaths remain an issue in the United States. Also, deaths from drug overdose are up among both men and women, all races, and adults of nearly all ages. In addition, research data shows the following:
 Statistics by States in the U.S.
Statistics by States in the U.S.

Counties with higher opioid prescribing tend to have the following characteristics:
There are many different types of opioids. In general, most opioids fall under these two categories:
Opioids obtained from plants are called opiates. These come from the flowering opium poppy plant. Examples are opium, morphine, heroin, and codeine. This means that all opiates are opioids. On the contrary, not all opioids are opiates.
Did you know that your body also produces opioids? Your brain makes opioids known as endorphins. These chemicals are similar to morphine and activate the opioid receptors. As a result, they can help minimize discomfort.
In addition, endorphins also bring about feelings of happiness and general well-being. Because of this, they are sometimes referred to as the “feel-good hormones.”
To simplify this discussion, we will talk about opioids under these headings:
Most prescription opioids treat moderate to severe pain. Healthcare providers can prescribe these drugs. Even though they are helpful, side effects can occur. There is also the risk of tolerance, dependence, and addiction.
The adverse effects of opioid misuse apply not only to the individual but also to those around them. To a large extent, it affects family and friends. Also, society as a whole. In a way, these effects are similar to secondhand drinking.
There are many prescription opioids. These include:
The side effects of most of the prescription opioids tend to be similar. These effects are due to their similar actions on the body. They include:
There are many street names for prescription opioids. Because there are several different types of prescription opioids, the street names are numerous. The changes in the language for these substances help drug users evade the detection of their habitual use. By using these various slangs, people can, therefore, remain discreet and hide their habits from family and friends.
Some common slangs for some prescription opioids include:
Of course, these names depend on the type of prescription pill. For details of specific drugs, “Street Names of Drugs: How Many Do You Know” gives a good account.
Even though fentanyl is a prescription opioid, it needs a discussion of its own. This is because illegal production is rife. Also, deaths from fentanyl are in epidemic proportions.  So, what is fentanyl? This drug is a synthetic opioid pain reliever. It is similar to morphine, but it is 50 to 100 times stronger. Fentanyl is a powerful prescription drug. It is also made and used illegally. The typical use of fentanyl is for severe pain, especially after surgery. In addition, it is helpful for severe cancer pain.
So, what is fentanyl? This drug is a synthetic opioid pain reliever. It is similar to morphine, but it is 50 to 100 times stronger. Fentanyl is a powerful prescription drug. It is also made and used illegally. The typical use of fentanyl is for severe pain, especially after surgery. In addition, it is helpful for severe cancer pain.
In some cases, fentanyl is used to treat people with chronic pain who are physically tolerant to other opioids. Tolerance occurs when you need a higher amount of a drug to get the desired effect. Thus, the longer you use an opioid, the more likely you are to become tolerant. Also, higher doses contribute to tolerance.
Synthetic opioids are the most common drugs involved in overdose deaths in the United States. In 2017, 59.8 percent of deaths from opioids were due to fentanyl. This number is a considerable increase from 14.3 percent in 2010.Click To TweetPrescription fentanyl is marketed by names such as:
Many drugs have street names. By using these various slangs, people can remain discreet and hide their habits from family and friends. Illegal fentanyl has several street names. Some examples are:
Prescription fentanyl is given in the following ways:
On the other hand, illegal fentanyl is sold in the following ways:
Furthermore, drug dealers sometimes mix fentanyl with other drugs. For example, it can be combined with cocaine, methamphetamine, heroin, and ecstasy. Dealers make such mixtures as it takes only a tiny amount of fentanyl to produce a “high.” This makes it cheaper for them, hence increasing their profits.
Unfortunately, this trend is hazardous. There have been many overdoses and deaths as a result of this.
 How does fentanyl affect the brain?
How does fentanyl affect the brain?
Just like other opioids, this drug works by binding to opioid receptors in the body. This reaction causes changes in the way the body perceives pain, and also emotions.
Over time, the brain adapts to the effects of this drug. More and more of this substance is needed to achieve the same effect. This is known as tolerance. As a result, dependence on fentanyl occurs. Continuous use leads to addiction, which can take over people’s lives.
Dependence on fentanyl can cause severe withdrawals if this drug is stopped. These symptoms include:
The withdrawal symptoms can be extremely uncomfortable. Hence, the difficulty in stopping fentanyl without medical supervision. This, therefore, stresses the importance of professional treatment.
 Overdosing on fentanyl is relatively common. One of the reasons for this is because of the potency of this substance. In simple terms, this means fentanyl is a very powerful drug.
Overdosing on fentanyl is relatively common. One of the reasons for this is because of the potency of this substance. In simple terms, this means fentanyl is a very powerful drug.
Also, to maximize profits, drug dealers mix it with other drugs. This means people end up taking fentanyl without even realizing it.
When people overdose on fentanyl, it can slow down their breathing. In addition to this, pinpoint pupils, coma, and even death can occur. Naloxone is a medicine that can quickly reverse the effects of fentanyl. Because of the quick action of naloxone, it is thus crucial to have it readily handy. Opioid users should have access but, also, family members and friends.
Detoxification is the first step in the treatment of opioid use disorders. Medication-Assisted Treatment (MAT) remains the gold standard for treating opioid use disorders long term.
MAT is an evidence-based treatment that involves the use of medications and behavioral therapy. Ultimately, the goal is to provide individualized whole-patient treatment.
There are three medications approved by the FDA for the treatment of opioid use disorders. These are buprenorphine, methadone, and naltrexone. In addition to medications and behavioral therapy, support from family and friends is essential to recovery.
For details on treatment, please refer to the section on Opioid Addiction Treatment below.
Heroin is a very addictive opioid. This rapidly acting opioid is classified as a Schedule I substance by the Drug Enforcement Administration (DEA). The reason for this is because of its extreme risk of addiction.
Heroin comes as a white powder, brown powder, or a black sticky substance known as black tar heroin. The use of this drug can quickly cause physical and psychological dependence.
It initially creates “a high” that users find attractive. Eventually, though, the high may not be as obvious. The withdrawals which follow not using can, however, be very uncomfortable. Because of this, people continue using to avoid the ensuing discomfort. For this reason, stopping “cold turkey” has very low success rates.
Common street names for heroin include:
 Heroin is made from morphine, a natural substance from the opium poppy plant. This plant is common in Southwest Asia, Southeast Asia, Mexico, and South America.
Heroin is made from morphine, a natural substance from the opium poppy plant. This plant is common in Southwest Asia, Southeast Asia, Mexico, and South America.
People use this drug by injecting, snorting, sniffing, and smoking. As a way to make it work faster, some people burn the substance and inhale the fumes.
Also, injecting heroin directly into the blood (IV use) is another way people quickly gain its effects. This IV use, unfortunately, leads to many complications. Furthermore, there is a practice of mixing heroin and cocaine known as speedballing.
Even though purer heroin is now more common, most heroin from the streets is “cut” with other substances. These substances can be other drugs, starch, sugar, quinine, or even powdered milk. Drug dealers probably add these to heroin to increase their profit margins. Unfortunately, this puts users of such mixtures at risk. This danger is, therefore, yet another reason to stay away from this drug.
People who use heroin are aware of the adverse effects. Despite this, they continue to use it. Why is this?
Heroin enters the brain very quickly. Because of this, it is very addictive. People like the rush or intense high this drug produces. Heroin users report feeling a profound sense of happiness, peace, and relaxation. Also, some people describe a “slowing down” of the world and portray a dream-like state.
How do people become addicted to heroin?
Firstly, tolerance develops. Tolerance means you have to use more of the drug to get the same effects. Secondly, physical and psychological dependence occurs. This means that without heroin, people develop withdrawals. These are very uncomfortable. Because of this discomfort, users tend to continue using it. This continuous use, therefore, helps the cycle of addiction.
Addiction can occur very quickly. Many factors play into how quickly people become addicted. These include the dose of heroin, method of use, frequency, the individual, and circumstances around using.
The body breaks down heroin into morphine. This substance enters the brain very quickly. Morphine attaches to cells in the brain known as opioid receptors.
Consequently, this attachment causes the release of large amounts of a brain chemical called dopamine. This chemical is regarded as a feel-good chemical and produces feelings of happiness. Heroin has effects on brain cells involved in feelings of pain, pleasure, heart rate, sleeping, and breathing.
The duration depends on several factors. Firstly, the amount used is essential. Secondly, the method of using contributes to this. Also, your body metabolism can contribute to how long it stays in your system.
Ultimately, heroin and its byproducts (metabolites) can remain in your body for one to three days.
The use of heroin causes an extreme high, described as “a rush.” In addition to this, there are many other effects of this drug:
Heroin users do not always know the exact amount they use. The reason for this is because heroin is often “cut” with other substances. Also, the other ingredients are mostly unknown.
Consequently, overdoses and complications are frequent. The death rate from heroin overdose is high. Unfortunately, deaths from heroin and other opioids continue to increase. The effects of heroin overdose include:
Detoxification is the first step in the treatment of opioid use disorders. Medication-Assisted Treatment (MAT) remains the gold standard for treating opioid use disorders long term. 
MAT is an evidence-based treatment that involves the use of medications and behavioral therapy. Ultimately, the goal is to provide individualized whole-patient treatment.
There are three medications approved by the FDA for the treatment of opioid use disorders. These are buprenorphine, methadone, and naltrexone.Click To TweetIn addition to medications and behavioral therapy, support from family and friends is essential to recovery. For details on treatment, please refer to the section on Opioid Addiction Treatment below.
Purple heroin is a combination of heroin and carfentanil or fentanyl. This mixture is relatively new on the drug scene. Unfortunately, there have been complications and deaths from using this substance.
Fentanyl is a powerful drug. Did you know, however, that carfentanil is even much stronger than fentanyl? Veterinarians use carfentanil for enormous animals like elephants, rhinos, and gorillas. That is, indeed, how strong it is.
According to the Drug Enforcement Administration (DEA), carfentanil is about 100 times stronger than fentanyl. It is also 5,000 times stronger than heroin and 10,000 times stronger than morphine! That is mind-boggling.
There is documentation of many overdose deaths from abusing purple heroin. Unfortunately, this number continues to grow.
Common street names for purple heroin are:
Overdoses are common with purple heroin. It is also more likely that people will overdose on purp than on heroin. This likelihood is because of the potency of fentanyl and carfentanil.
Overdose symptoms can present as:
Combining heroin with carfentanil or fentanyl is one thing. However, mixing them up in unknown amounts is another issue altogether.
People using purp don’t know the exact amount of the ingredients in the drug. As a result, this makes taking purple heroin similar to playing Russian roulette. Thus, the high number of deaths from this drug.
The best way to stay safe from the effects of purple heroin is to abstain. Staying away is, however, easier said than done for people who have an addiction to this drug. Because addiction is a brain disease, stopping drug use is more complicated than the moral angle suggests.
As a result of this, consideration of other techniques is crucial. Harm reduction for purple heroin is one of such modalities to consider.
The Community Drug Strategy is a Canadian initiative. This organization aims to improve health and also address drug-related issues. As a way to be safer, these are some of their recommendations:
The above advice is in keeping with harm reduction. Again, it is best to abstain from purple heroin and other drugs. However, for people who use, caution must be utilized. The aim is to avoid life-threatening complications from using purple heroin.
To clarify, abstinence or safer alternatives should be the goal. Medication-Assisted Treatment remains a gold standard for treating opioid use disorders.
In the United States, the ingredients of purple heroin are all controlled substances:
Detoxification is the first step in the treatment of opioid use disorders. Medication-Assisted Treatment (MAT) remains the gold standard for treating opioid use disorders long term.
MAT is an evidence-based treatment that involves the use of medications and behavioral therapy. Ultimately, the goal is to provide individualized whole-patient treatment.Click To TweetThere are three medications approved by the FDA for the treatment of opioid use disorders. These are buprenorphine, methadone, and naltrexone.
In addition to medications and behavioral therapy, support from family and friends is essential to recovery.
For details on treatment, please refer to the section on Opioid Addiction Treatment below. In summary, though, a comprehensive treatment approach is key.
Is carfentanil dangerous? Yes, it is! Very dangerous. Carfentanil is about a hundred times stronger than fentanyl. It is also thousands of times stronger than heroin.
This potency means very tiny doses can be hazardous. An amount as small as a grain of salt (about 20 mcg) can be fatal. Hence, the need to be very careful with this substance.
Carfentanil is a synthetic opioid first made in 1974. It is a very potent drug. Because of this, veterinarians use carfentanil to put huge animals to sleep. It can knock out an elephant quite quickly! The brand name for this drug is “Wildnil.” Due to its potency, it is a component of some tranquilizer darts.
In 2016, Time wrote an article titled “Heroin is Being Laced With a Terrifying New Substance: What to Know About Carfentanil.” This article reported over 300 overdoses and multiple deaths related to this drug.
Carfentanil is probably added to heroin because it is cheaper than heroin. It is also easier to get and make than heroin. Furthermore, carfentanil has no smell or taste. This property makes it impossible to tell if your drug has carfentanil in it. It comes as liquid, blotter, powder, and pill.
Carfentanil can get to the brain very quickly. This ability is because of how easily it crosses the blood-brain-barrier. It thus works fast, but it is also short-acting.
When an opioid is taken, it travels through the blood and gets into the brain. This chemical then attaches to specific receptors called opioid receptors. Also, opioids bind to receptors in the spinal cord and gut.
 The chemical response of this drug binding to receptors in the brain decreases the body’s perception of pain. Opioids are used to treat moderate to severe pain that does not respond well to other pain medications.
The chemical response of this drug binding to receptors in the brain decreases the body’s perception of pain. Opioids are used to treat moderate to severe pain that does not respond well to other pain medications.
The brain produces a chemical called dopamine. Because opioids target the brain’s reward system, they increase dopamine in the brain. The overstimulation of this system causes the high that comes with using these drugs. Due to this feeling, there is a tendency for people to continue to use to experience this euphoria.
The brain’s reward center is responsible for the reactions to intense pleasure. Opioids, like all drugs of abuse, triggers the release of dopamine in excess amounts. The amounts released are far beyond what is needed to provide pleasure in typical situations.
Opioids are most commonly used to treat moderate to severe pain. The origin of such pain may be following surgery or trauma. In some cases, pain may be due to chronic conditions like arthritis or even cancer.
Other than pain, opioids are also used for treating other conditions. Codeine was once the “gold standard” in cough suppressants. Not so much currently, though. Loperamide is an opioid for treating diarrhea due to irritable bowel syndrome. Opioids may also help with shortness of breath in advanced cases of cancer and other terminal conditions.
Opioid use leads to tolerance over time. Tolerance means you need an increase in the amount of opioids to achieve the same effect. It also infers that the effect decreases with continued use of the same amount of the drug. This makes the brain function more or less normally when the drug is present. On the other hand, there is abnormal functioning when the drug is absent.
Continuous use may lead to dependence. This occurs when the body adapts to the presence of opioids. As a result, withdrawal symptoms develop when the drug is decreased or stopped. Addiction may also occur. Addiction is defined as the compulsive and uncontrollable use of drugs despite adverse consequences.
Initially, people who abuse opioids may experience a high and pleasure. Regular use of this drug, however, causes the effect to diminish. At this point, people continue to use to avoid withdrawal symptoms.
To make a diagnosis of an opioid use disorder, specific criteria have to be met. According to the DSM-5, there must be a problematic use of opioids, causing significant impairment or distress. The DSM-5 requires at least two of such of impairments that occur within 12 months. These impairments or difficulty include:
How can you tell if you or a loved one is struggling with opioid addiction? It is important to note that someone struggling with opioid use disorder may develop symptoms slowly. Over time, however, it becomes more evident that they need help.
Common signs of opioid addiction include:
Several factors determine how long opioids stay in your system. Also, because there are many different types of opioids, the length of stay will vary somewhat. However, the following factors generally affect the duration of most opioids:
In general, detection of opioids in the body is as follows:
Note, though, that these are all averages. The half-lives vary from one opioid to another. Besides, opioids build up in fatty tissues after long-term use. Thus, these averages tend to be longer in heavy, chronic users.
Does eating poppy seeds cause a false positive urine screen for opioids? This question is a genuine concern for a lot of people. The answer to this question is, yes, it can.
 Poppy seeds do not contain morphine. However, the seeds can become coated by opium extract during harvesting. Consequently, the poppy seeds end up with some opium. Such poppy seeds may end up on muffins or bagels.
Poppy seeds do not contain morphine. However, the seeds can become coated by opium extract during harvesting. Consequently, the poppy seeds end up with some opium. Such poppy seeds may end up on muffins or bagels.
Eating pastries with poppy seeds can cause the urine to test positive for morphine and codeine. Indeed, they can be found in urine samples for as long as two days after eating foods containing poppy seeds. When large amounts of the seeds are consumed, opiates may last up to 60 hours in the urine.
Previously, there were many false-positive tests from eating poppy seeds. However, since they contain low amounts of opioids, many current tests now have a higher threshold to avoid false positives.
An opioid overdose occurs when an individual takes high doses of opioids. This can lead to slowing or stopping of breathing. Consequently, this may lead to death.
Opioid overdoses are relatively common. An overdose can occur for a few reasons. Examples are when someone accidentally takes an extra dose, intentionally misuses a prescription opioid, or mixes opioids with other medications. Also, alcohol and over the counter medications may be involved.
In some cases, people take medications meant for someone else. For example, children may overdose if they accidentally take their parents’ medications.
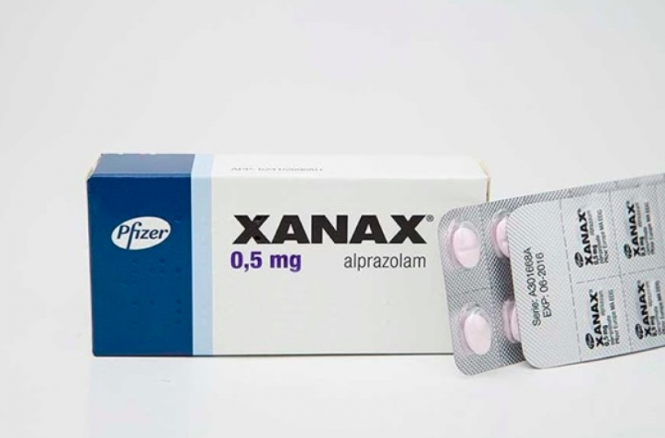
Prescription opioid overdose deaths often involve benzodiazepines. These are medications that help with anxiety, sleep, and seizures. Examples are Xanax, Ativan, and Valium.
The combination of benzodiazepines and opioids can cause difficulty breathing, thus, leading to coma or death. So, avoid mixing these medications.Click To Tweet
Overdosing on opioids is life-threatening. This situation requires immediate emergency attention. For this reason, it is important to be able to recognize the signs.
The chance of survival is dependent on how quickly the person receives emergency treatment. Consider the following actions:
Naloxone is a medication that can treat an opioid overdose when given immediately. It is an opioid antagonist with FDA approval for opioid overdose. This drug is a lifesaver. In view of this, it is readily available to individuals who use opioids. In addition, friends and family members can easily get this medication.
This medication blocks opioid receptors in the brain. As a result, it reverses the toxic effects of the overdose. Naloxone administration is by:
Naloxone is readily available from healthcare providers. In some states, pharmacists can dispense naloxone without a prescription. Hence, friends, family, and others can administer this drug in emergencies. The auto-injector (Evzio) and nasal spray (Narcan) versions of naloxone are easy to use.
Training for naloxone administration is available. So, people with opioid use disorder should get this training and carry this life-saver with them. In addition, friends and family should consider having this emergency medication available. Ultimately, it is people around who rescue overdose victims.
The following groups of people will benefit from carrying naloxone:
Note that some people may require multiple naloxone doses. Overdosing on stronger opioids like fentanyl makes this even more likely. In such cases, dosing every two to three minutes may be necessary.
Furthermore, it is essential to monitor people who receive naloxone closely. The recommendation is to observe for up to two hours after the last dose of naloxone. This is because breathing can still slow or even stop afterward.
Because naloxone blocks opioid receptors, it can cause symptoms of opioid withdrawal. Naloxone also has side effects:
Opioid addiction is a chronic brain disease. In a way, it is similar to other medical conditions like high blood pressure and diabetes. What this means is that there is no cure. Opioid addiction can, however, be managed, and people with addiction can recover.
Treatment using safe and proven methods can lead to a healthy, positive life. This healthy way of life is known as recovery. Several studies have been done to find out the most effective choice for opioid addiction treatment. Medications, along with behavioral therapies, are the gold standard for treating this disorder.
Unlike stopping heavy alcohol use, quitting opioids is not particularly risky. Withdrawal from alcohol and benzodiazepines can be fatal. This is, however, not the case with opioids. Still, opioid withdrawals can be extremely uncomfortable.
Opioid addiction treatment can occur in several different settings. The place of treatment will depend on the medications, the person’s situation, home environment, and other factors. There are three primary treatment settings:
Addiction is a chronic disease. Given this, it is essential to note that the treatment will be ongoing. In addition, avoiding persons, places, and situations that can lead to relapse is crucial. Relapse means using a substance again after a period of not using.
In general, opioid addiction treatment involves the following:
Medically assisted detoxification is commonly known as detox. It is only the first stage of addiction treatment. By itself, it does little to change long-term drug abuse. Thus, the need for comprehensive treatment to maintain sobriety. 
Detox helps to manage the symptoms of withdrawal safely. This treatment is a crucial step in the process of recovery. Opioid withdrawal refers to a wide range of symptoms that occur after stopping the use of opioid medications. These symptoms can last up to 10 days. In most cases, however, opioid withdrawals last between three to five days.
Withdrawals from opioids can be extremely uncomfortable without proper management. It is rarely life-threatening, though. Using medications to treat withdrawals is generally known as withdrawal management or detoxification. Also, some people refer to it as detox.
The success rates for opioid addiction treatment are much higher when detoxification is done. Quitting “cold turkey” is less successful and is usually very uncomfortable. Albeit challenging, some people have success stopping without any medical intervention. This is, however, not recommended.
Commonly used medications for opioid detox are buprenorphine and clonidine. These medications help make withdrawal symptoms more manageable. They also make detox safer and more successful. Note, however, that opioid-dependent people can start methadone maintenance immediately. They do not require withdrawal management. Similarly, buprenorphine maintenance requires an induction and stabilization initially. After this, an individual can go on a maintenance dose.
Codeine phosphate is sometimes used for detox. It does not affect 2-10 percent of people, however. It tends to be an option when there is breathing difficulty and liver damage. In addition, Lofexidine has FDA approval for treating opioid withdrawal symptoms. It is a non-opioid medication.
Also, the NSS-2 Bridge device is a small electrical nerve stimulator for opioid withdrawals. The placement of this device is behind the person’s ear. It eases symptoms for up to five days during the acute withdrawal phase. Some studies have shown the benefits of this device.
In addition to the above treatments, other medicines may be prescribed for sleep, nausea, vomiting, and anxiety.
Medication-Assisted Treatment (MAT) is an evidence-based treatment approach that involves the use of medications with counseling and behavioral therapies to treat substance use disorders. The goal of Medication-Assisted Treatment is to provide a “whole-patient” approach to treatment.
Note that withdrawal management alone does not treat opioid addiction adequately. Many people relapse after having just detox. Hence, the need for comprehensive treatment to ensure recovery.
Maintenance medication in combination with counseling and other support is the recommended treatment for opioid addiction. Click To TweetWhat are maintenance medications? These are medications on a consistent schedule for people with addiction. There are three main choices for medications to treat opioid addiction. These are buprenorphine, naltrexone, and methadone.
Everyone’s condition is different. Thus, the best option will depend on the person, situation, and environment. This decision is made between the person and the clinician. It is, therefore, essential to be open with your treatment professionals.
Buprenorphine is used in medication-assisted treatment to treat opioid use disorder. It was approved by the Food and Drug Administration (FDA) in 2002.
This medication is the first medication for opioid addiction that can be prescribed in an office setting. On the contrary, methadone requires a highly structured clinic. Thus, buprenorphine significantly increases access to treatment.
Under the Drug Addiction Treatment Act of 2000 (DATA 2000), U.S physicians and mid-level practitioners can offer buprenorphine for opioid addiction. Such professionals have to qualify and get an X-license to prescribe. Settings for such prescriptions include offices, community hospitals, health departments, and correctional facilities.
Buprenorphine prescription is always done as part of a comprehensive treatment plan that includes counseling and social support programs. The following buprenorphine products have FDA approval for opioid addiction:
In addition, some buprenorphine products also come as generics. The dose of buprenorphine depends on the type. Most of the tablets and films are given once or twice a day. Sublocate injection is administered under the skin (subcutaneously) once a month. Probuphine is a skin implant that lasts for six months.
Buprenorphine is a partial opioid agonist. This means that it has similar actions to opioids. Thus, it produces effects such as feeling a “high” or breathing difficulties. However, these effects are weaker than full opioid agonists such as methadone and heroin.
The use of buprenorphine is NOT replacing one addiction with another. This medication can lower the potential for misuse of opioids. It also decreases the effects of physical dependence on opioids, such as withdrawals and cravings. Furthermore, it increases safety in cases of overdose.
The effects of buprenorphine increase with each dose until it gets to moderate doses. At this point, it levels out. Thus, further increases do not yield any effects. This “ceiling effect” lowers the risk of misuse, dependence, and side effects.
The side effects of this medication are similar to those of opioids. These include:
Due to the opioid effects of buprenorphine, some people misuse it. As a result of this, naloxone is a component of some buprenorphine products. Suboxone, Zubsolv, and Bunavail all contain this compound.
Naloxone is an antagonist (or blocker) at opioid receptors. It has no effect when products containing it are taken as prescribed. However, if someone with opioid dependence injects a product containing naloxone, severe withdrawal symptoms will occur. Thus, this combination decreases the likelihood of misuse and diversion.
It is not advisable to take buprenorphine with alcohol, other illicit drugs, sleep medications, or drugs that slow breathing. This is to avoid the possibility of overdose or death. So, care should be taken after buprenorphine administration.
Buprenorphine treatment requires a diagnosis of opioid use disorder. This treatment occurs in three phases:
Note, though, that not all clinicians can prescribe buprenorphine. So, it is vital to find a healthcare provider with the certification to prescribe this medication. Many certified prescribers can be found in the Buprenorphine Practitioner Locator.
Methadone use for opioid addiction spans several decades. It is helpful as medication-assisted treatment for opioid use disorder. The goal of methadone is to sustain long-term success. This, therefore, helps people live healthier and more fulfilling lives.
The brand names of methadone include Diskets, Dolophine, and Methadose.
Methadone acts on the opioid receptors in the brain. It, thus, decreases opioid cravings and withdrawals. This drug is taken once a day. It is available as liquid, tablets, powder, and diskettes.
Medication-assisted treatment involves medications, counseling, and social support. Similarly, the prescription of methadone is part of a comprehensive treatment plan.
Methadone prescriptions come with tight regulations. It is available only via SAMHSA-certified opioid treatment programs.
Again, just like with buprenorphine, the length of treatment with methadone is variable. According to the National Institute on Drug Abuse (NIDA), the duration of methadone treatment should be a minimum of 12 months. Even though this minimum is recommended, many people take methadone for several years.
Methadone is safe when taken as prescribed. It has a very long half-life. Because of this, it stays in the body long after the effects wear off. Thus, it is essential to avoid medications that can cause an overdose. Sharing a list of your other medications with your healthcare provider is vital.
Naltrexone is a medication used to treat opioid and alcohol use disorders. It has approval by the FDA for use in medication-assisted treatment. The most common prescription is the pill form. Brand names for the tablets are ReVia and Depade. It, however, also comes as an injectable – Vivitrol.
Naltrexone tablet dosing is usually 50mg daily. Higher doses are sometimes necessary. Vivitrol, the injectable extended-release form, is dosed as 380mg monthly.
Unlike buprenorphine and methadone, naltrexone prescriptions are more readily available. Any healthcare provider licensed to prescribe can write scripts for naltrexone.
Abstaining from any opioids at least 7-10 days before taking naltrexone is necessary. This helps to avoid precipitated withdrawals. It is, therefore, important to get a proper timeline before treatment.
Naltrexone blocks the opioid receptors in the brain. As a result, it stops opioids from working. This action removes the ability to get high from using drugs like heroin, codeine, and morphine.
Due to the way naltrexone works, it may not stop all drug cravings. It is, however, a good option for preventing relapse.
On the contrary, medications like buprenorphine and methadone activate the opioid receptors. They are, therefore, better at suppressing cravings.
One massive advantage of naltrexone, though, is that there is no abuse and diversion potential. Also, for those who relapse while on naltrexone, it prevents the feeling of getting high.
Discontinuing naltrexone can lead to a decrease in tolerance to opioids. This can cause an increase in sensitivity to opioids. This means lower doses of opioids have more effects on them than previously. Thus, doses of opioids that were previously tolerated can lead to an overdose. People must be aware of this.
Again, as with other MAT medications, naltrexone is usually part of a comprehensive treatment plan. Counseling and social support are vital components of success.
There is no specialized training for healthcare providers to prescribe naltrexone or Vivitrol. Detox from opioids must, however, be done before administration. At least 7-10 days should be given before treatment starts.
Naltrexone decreases cravings. It also minimizes the feeling of intoxication if people drink on it. Note, though, that it is not advisable to drink on this medication. In addition, naltrexone is not addictive.Click To TweetResearch shows long-term naltrexone beyond three months to be most effective. It can also be used indefinitely. The duration of treatment will depend on the individual and personal circumstances.
So, which of the various medications is your best choice? Picking a medication for opioid addiction depends on a few factors. Firstly, it depends on the individual. Secondly, the circumstances and environment play a huge role. In addition, the choice of medication is made together with a healthcare provider.
A NIDA study comparing the effectiveness of these two medications is available. It compares buprenorphine/naloxone and extended-release naltrexone (Vivitrol) in treating opioid use disorder. This study shows that both medications are similarly effective once treatment is initiated.
Because naltrexone requires full detoxification, initiating treatment among active opioid users was more difficult. However, once detox was complete, naltrexone had similar effectiveness as the buprenorphine/naloxone combination.
Behavioral therapy is an essential component of treatment. In addition to medications, counseling is recommended for patients with opioid addiction. Counseling helps people modify their attitudes and behaviors related to opioid use. Also, it increases a healthy lifestyle and helps with taking medications regularly.
Counseling also helps people address personal, social, or other issues that can contribute to their addiction. For example, improving self-worth, stressful situations at home or work, and spending time in the same environment.
Behavioral therapies are quite useful in opioid addiction. This usefulness is especially evident when combined with medications. Such therapies include cognitive-behavioral therapy, motivational enhancement, and contingency-management interventions.
Cognitive-behavioral therapy is a type of counseling that helps people understand the thoughts and feelings that influence their behaviors. In this case, these behaviors are those that cause their addiction to opioids.
Contingency management interventions refer to providing incentives in exchange for treatment engagement and being able to maintain abstinence.
Motivational enhancement therapy attempts to initiate a change in behavior. It does this by encouraging people to resolve their doubts about stopping the use of opioids. Furthermore, it also helps individuals engage in treatment.
These behavioral treatment approaches have proven effective, especially when used along with medicines. Given this, it is essential to have this as a component of treatment.
In 2018, the FDA cleared a mobile medical application (app) for opioid use disorder. The reSET-O app is a prescription cognitive behavioral therapy. It is helpful for treatment together with treatment that includes buprenorphine and contingency management. It, thus, helps increase retention in outpatient treatment programs.
In addition to counseling, support groups are beneficial. They usually consist of other people who are also in recovery. These groups help people share their personal experiences. Support groups provide community encouragement to assist in the recovery process. Examples of such groups are Narcotics Anonymous and Pills Anonymous.
For people who use opioids and other drugs, recovery is ongoing. Cravings may develop from time to time, even after treatment. Support groups can provide emotional guidance and encouragement when cravings become intense.
Support groups exist not just for people in recovery, but also their friends and family. Remember, addiction affects people around those who use drugs. So, collective help goes a long way to help recovery.
Coping with addiction is tough. Despite proper treatment, maintaining sobriety can be quite tasking. It is, therefore, vital to have good social support. Growing and strengthening ties with family and friends go a long way to help with recovery.
Family and friends play a crucial role in recovery. Moreso, when they are engaging. They should try and learn as much as possible about addiction to improve the chances of maintaining recovery.
People, places, events, and situations associated with opioids may contribute to relapse. Thus, individuals need to avoid such triggers. In some cases, these may be unavoidable. The ability to use coping mechanisms to stop cravings becomes crucial. This also requires support from family and friends. In essence, support from people around the person struggling with opioid addiction is essential for recovery.
Detox, medication-assisted treatment, counseling, and support are helpful for opioid addiction treatment. In addition to these, it is essential to treat underlying mental health disorders. The importance of this should never be underplayed.
Treatment for depression, anxiety, post-traumatic stress disorder, bipolar disorder, ADHD, and other mental conditions must be considered. It is well known that many individuals self-medicate with drugs. Thus, the need to treat these conditions to prevent a relapse and maintain recovery.
There are different classes of medications that help with various mental disorders. Some of these include antidepressants, anti-anxiety medications, mood stabilizers, and antipsychotics. Transcranial Magnetic Stimulation (TMS) is an FDA approved non-drug treatment for depression.
The National Institute of Drug Abuse (NIDA) produced a research-based guide. This guide highlights the principles of effective treatment. These include:
Following the treatment of opioid use disorder, cravings can still occur. In fact, this is a real struggle for many. It is also a reason for multiple relapses.
So, what are opioid cravings? These are physical compulsions or urges to use opioids. The prominent symptom of cravings is the overpowering desire to use the drug.
This drive causes individuals to focus on acquiring the drug. It also leads to a psychological want for the positive effects of the substance.
Cravings are normal and can last for long periods, often causing people to relapse. Cravings may be experienced during the acute withdrawal period and may also occur weeks, months, or even years after use.Click To TweetIn general, though, they tend to decrease in strength and frequency over time. Cravings may last for minutes to even hours but usually will go away eventually, until the next episode.
Cravings do not indicate that there is a problem. It does not mean that you are unable to manage your desires or that you are weak. A previously published article describes cravings as coming in waves – they build up, reach a peak, and then subside.
Relapse triggers are things, people, places, or situations that an individual who struggles with drugs or alcohol associates with the reward of getting high. These triggers may lead to intense cravings.
Ultimately, the goal is to stop or control these cravings. So, how do you do this?
The key to limiting relapse is to manage relapse triggers and cravings.
Often, the talk is about how to stop opioids. Let us not forget, though, that in some cases, people use prescription opioids due to chronic pain. So, what happens when they stop these medications?
Perhaps, alternative treatments for chronic pain may help them continue to stay away from their prescription medications. Indeed, there are quite a few of such treatments.
Ultimately, individuals who suffer from chronic pain should consult with a pain specialist. Even though there are many alternative treatments, pain treatment is specific to each individual. Due to many possible reasons, what works for one person may not work for another. Hence the need for a proper evaluation by a professional.
Opioids are a class of drugs primarily used to treat moderate to severe pain. They are naturally found in the opium poppy plant. Even though they help treat medical conditions, they also have adverse effects. In addition to several possible side effects, addiction to this drug is rife. As a result, opioid overdoses and deaths remain an epidemic in the United States.
Opioids attach to specific sites in the brain known as opioid receptors. This reaction causes a decrease in the body’s perception of pain. Also, opioids can cause an overstimulation of the reward system – also called the pleasure center. This leads to the release of very high amounts of dopamine. Unfortunately, tolerance, dependence, and addiction can develop as a result.
Signs of opioid addiction include the inability to control the use of opioids, intense cravings, drowsiness, new financial problems, and isolating. Furthermore, there is also the risk of overdose and death. Naloxone (Narcan) is a medication that can reverse an opioid overdose. It, however, needs to be given immediately after an individual overdoses.
Due to the many adverse effects of opioid use disorder, it is essential to obtain proper treatment. Management can be done as an inpatient or outpatient. Regardless of the setting of choice, the first step is withdrawal management. This is also called detoxification (detox). Medication-Assisted Treatment (MAT) is the gold standard for opioid addiction.
MAT involves the use of medications with counseling and behavioral therapies. Other than medications and counseling, support from family, friends, and groups is crucial. Also, it is essential to treat underlying mental illness. Self-medication with illicit substances is a common occurrence in people with mental disorders.
The opioid crisis remains a scourge in the United States. Even though it remains a public health crisis, there have been some positive changes in the right direction. This, however, needs to continue with everyone on board. Collectively, we can make a change!
Subscribe to get our latest content by email.
The entire content of AddictionBlueprint, including content on drugs and alcohol, medications, therapies, facilities, spotlights, recommendations, and other features is for informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis or treatment. This does not constitute a physician-patient relationship. Please seek the advice of your physician or other qualified health providers regarding your addiction, mental and medical issues.

May 2019
May 2019

Jun 2019
Jun 2019

Jun 2019

Jun 2019

Jul 2019

Jul 2019

Jul 2019
Jul 2019

Aug 2019

Aug 2019

Aug 2019

Sep 2019

Oct 2019

Oct 2019

Sep 2019

Sep 2019

Oct 2019
Nov 2019

Dec 2019

Nov 2019
Nov 2019

Jan 2020

Jan 2020

Jan 2020
Feb 2020

Feb 2020

Mar 2020
Feb 2020
May 2019
May 2019
As far as I know, since the mid-1990s, the frequency of use of opioids (painkillers) has increased significantly in some countries.
That is correct. There are slight variations from one country to another.
This is precisely what I was searching for; thanks for sharing this valuable insights.
prednisone 2.5 mg cost: http://prednisone1st.store/# prednisone 20mg price in india
dating sites online: top online meeting sites – best websites dating
https://propecia1st.science/# get cheap propecia tablets
buy amoxicillin 500mg buy amoxicillin – antibiotic amoxicillin
canadian king pharmacy onlinepharmaciescanada com
cheapest ed pills: treatment for ed – non prescription ed pills
[url=https://pharmacyreview.best/#]the canadian pharmacy[/url] cross border pharmacy canada
cheap erectile dysfunction: best ed pills non prescription – non prescription ed drugs
Get information now.
best erectile dysfunction pills: herbal ed treatment – herbal ed treatment
Comprehensive side effect and adverse reaction information.
https://pharmacyreview.best/# safe canadian pharmacy
where can i get amoxicillin: [url=http://amoxicillins.com/#]amoxicillin over the counter in canada[/url] amoxicillin 50 mg tablets
order cheap propecia price order cheap propecia
[url=https://propecia1st.science/#]cost of propecia without prescription[/url] propecia without a prescription
erection pills: ed treatment pills – best medication for ed
cheap erectile dysfunction pill: ed meds online – pills erectile dysfunction
https://propecia1st.science/# buy propecia without a prescription
cost of propecia prices get propecia no prescription
canadian pharmacy mall pharmacies in canada that ship to the us
Read information now.
ed drugs list: pills for erection – cheap ed pills
Long-Term Effects.
where can i buy mobic without insurance [url=https://mobic.store/#]can i purchase cheap mobic prices[/url] can you get generic mobic prices
amoxicillin 500 tablet: http://amoxicillins.com/# amoxicillin 500 mg capsule
where to buy amoxicillin pharmacy amoxicillin online without prescription – amoxicillin 500 mg price
can you buy amoxicillin over the counter in canada: [url=https://amoxicillins.com/#]amoxicillin 500mg capsule buy online[/url] price for amoxicillin 875 mg
how to get amoxicillin amoxicillin tablet 500mg – buy amoxicillin 500mg usa
how to cure ed [url=http://cheapestedpills.com/#]best erection pills[/url] non prescription erection pills
order generic propecia without rx get cheap propecia without insurance
https://propecia1st.science/# cheap propecia pill
how to buy generic mobic without rx: where can i buy mobic without insurance – buy cheap mobic pill
Some are medicines that help people when doctors prescribe.
amoxicillin where to get amoxicillin 500mg price canada – amoxicillin generic
Learn about the side effects, dosages, and interactions.
https://pharmacyreview.best/# canada pharmacy reviews
what are ed drugs: best treatment for ed – ed meds online without doctor prescription
п»їbest mexican online pharmacies: п»їbest mexican online pharmacies – mexican pharmaceuticals online
canadian pharmacy no scripts: canadian online drugs – best canadian pharmacy to buy from
pharmacies in mexico that ship to usa medication from mexico pharmacy or medication from mexico pharmacy
http://dynamictiming.com/__media__/js/netsoltrademark.php?d=mexpharmacy.sbs buying prescription drugs in mexico online
[url=http://xactprice.org/__media__/js/netsoltrademark.php?d=mexpharmacy.sbs]mexico drug stores pharmacies[/url] medication from mexico pharmacy and [url=https://bbs.xiaoditech.com/home.php?mod=space&uid=1373694]buying from online mexican pharmacy[/url] mexican pharmaceuticals online
http://certifiedcanadapharm.store/# canadian pharmacy cheap
canadian drugs northwest pharmacy canada or reddit canadian pharmacy
http://lookingbackanddreamingforward.com/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store my canadian pharmacy
[url=http://identitypreservedproducts.com/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store]canadian pharmacy no scripts[/url] canadian pharmacy prices and [url=http://www.lntoxicated.com/home.php?mod=space&uid=1069158]real canadian pharmacy[/url] adderall canadian pharmacy
mexican mail order pharmacies: mexican mail order pharmacies – mexico drug stores pharmacies
https://certifiedcanadapharm.store/# legitimate canadian mail order pharmacy
canadian pharmacy drugs online: global pharmacy canada – onlinepharmaciescanada com
reputable indian online pharmacy cheapest online pharmacy india or mail order pharmacy india
http://pajamagrams.com/__media__/js/netsoltrademark.php?d=indiamedicine.world best online pharmacy india
[url=http://touch909.com/__media__/js/netsoltrademark.php?d=indiamedicine.world]india pharmacy mail order[/url] top 10 pharmacies in india and [url=http://wuyuebanzou.com/home.php?mod=space&uid=323632]top 10 online pharmacy in india[/url] cheapest online pharmacy india
http://indiamedicine.world/# indian pharmacy
canadian drugs pharmacy: canadian pharmacy 365 – pharmacy rx world canada
https://mexpharmacy.sbs/# medicine in mexico pharmacies
canada drugs online review vipps approved canadian online pharmacy or trustworthy canadian pharmacy
http://floridacaviar.com/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store onlinecanadianpharmacy 24
[url=http://lakesliving.com/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store]canadian pharmacy near me[/url] best canadian pharmacy online and [url=http://plixsite.net/forum/member.php?action=profile&uid=2424417]canadianpharmacymeds[/url] online canadian pharmacy review
https://indiamedicine.world/# buy prescription drugs from india
canadian neighbor pharmacy: canadian pharmacy – online pharmacy canada
indianpharmacy com top 10 pharmacies in india or pharmacy website india
http://exilesunglasses.com/__media__/js/netsoltrademark.php?d=indiamedicine.world pharmacy website india
[url=http://euro-entreprises.net/__media__/js/netsoltrademark.php?d=indiamedicine.world]indian pharmacy paypal[/url] indian pharmacies safe and [url=http://www.wjyjh.cn/home.php?mod=space&uid=3512]india online pharmacy[/url] buy prescription drugs from india
best canadian pharmacy to buy from: legit canadian pharmacy – canada online pharmacy
http://mexpharmacy.sbs/# mexico pharmacies prescription drugs
mexican border pharmacies shipping to usa: pharmacies in mexico that ship to usa – medicine in mexico pharmacies
https://mexpharmacy.sbs/# best online pharmacies in mexico
http://mexpharmacy.sbs/# mexican border pharmacies shipping to usa
mexican border pharmacies shipping to usa mexican drugstore online or medication from mexico pharmacy
http://www.valueradar.com/__media__/js/netsoltrademark.php?d=mexpharmacy.sbs mexican border pharmacies shipping to usa
[url=http://richardabbott.com/__media__/js/netsoltrademark.php?d=mexpharmacy.sbs]medicine in mexico pharmacies[/url] mexican pharmaceuticals online and [url=https://quantrinet.com/forum/member.php?u=486011]mexican online pharmacies prescription drugs[/url] mexican drugstore online
canadianpharmacyworld com: canadian pharmacy 1 internet online drugstore – legit canadian pharmacy
buy medicines online in india india pharmacy or cheapest online pharmacy india
http://shorefinds.com/__media__/js/netsoltrademark.php?d=indiamedicine.world buy medicines online in india
[url=http://aetnaabsenceadvocate.info/__media__/js/netsoltrademark.php?d=indiamedicine.world]india pharmacy[/url] top online pharmacy india and [url=http://bbs1.857moli.com/home.php?mod=space&uid=427032]п»їlegitimate online pharmacies india[/url] online pharmacy india
canadian family pharmacy canadian drug stores or buying drugs from canada
http://espressoitalianmarket.net/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store legal to buy prescription drugs from canada
[url=http://occupationz.com/__media__/js/netsoltrademark.php?d=certifiedcanadapharm.store]canadian medications[/url] canadian pharmacy uk delivery and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2925373]canadian pharmacies online[/url] canadian online pharmacy
my canadian pharmacy: legal to buy prescription drugs from canada – best canadian pharmacy
http://certifiedcanadapharm.store/# my canadian pharmacy review
canada drug pharmacy: canadian pharmacy ltd – canadian pharmacy 24h com
http://certifiedcanadapharm.store/# best canadian pharmacy
reputable indian online pharmacy: п»їlegitimate online pharmacies india – indian pharmacy paypal
zithromax online usa: can you buy zithromax online – where to buy zithromax in canada
http://stromectolonline.pro/# ivermectin 400 mg brands
ivermectin 1 topical cream ivermectin 2% or ivermectin price canada
http://snackfact.com/__media__/js/netsoltrademark.php?d=stromectolonline.pro ivermectin tablets
[url=http://e-patient.org/__media__/js/netsoltrademark.php?d=stromectolonline.pro]ivermectin lotion[/url] cost of ivermectin cream and [url=http://www.1nanspa.com/space-uid-7250.html]ivermectin lotion[/url] ivermectin price
neurontin price australia medication neurontin or neurontin price south africa
http://mathtutor.biz/__media__/js/netsoltrademark.php?d=gabapentin.pro neurontin cap 300mg price
[url=http://thefieldsofathenry.com/__media__/js/netsoltrademark.php?d=gabapentin.pro]neurontin 300 mg pill[/url] neurontin 800 mg tablets best price and [url=http://521boy.com/home.php?mod=space&uid=8599]neurontin 150 mg[/url] generic neurontin 600 mg
neurontin cost in singapore: neurontin 200 – neurontin 150 mg
buy neurontin 100 mg gabapentin 100mg or cheap neurontin
http://spinetrac.com/__media__/js/netsoltrademark.php?d=gabapentin.pro neurontin 300 mg cap
[url=http://beklife.com/__media__/js/netsoltrademark.php?d=gabapentin.pro]neurontin canada online[/url] neurontin 300 and [url=http://wuyuebanzou.com/home.php?mod=space&uid=329864]neurontin generic south africa[/url] neurontin 200 mg
ivermectin ebay [url=https://stromectolonline.pro/#]ivermectin 12 mg[/url] ivermectin uk coronavirus
https://gabapentin.pro/# neurontin 300 mg tablets
http://gabapentin.pro/# neurontin 600 mg
where can i get zithromax zithromax 250 mg pill or zithromax 500 mg lowest price pharmacy online
http://sonorabehavioralhealth.com/__media__/js/netsoltrademark.php?d=azithromycin.men zithromax online pharmacy canada
[url=http://kenfisherarbitration.com/__media__/js/netsoltrademark.php?d=azithromycin.men]how to get zithromax over the counter[/url] zithromax tablets and [url=http://lsdsng.com/user/481826]zithromax 500 mg lowest price drugstore online[/url] zithromax 250 mg pill
where to buy zithromax in canada: zithromax online usa – how much is zithromax 250 mg
http://stromectolonline.pro/# ivermectin nz
http://stromectolonline.pro/# ivermectin 2ml
ivermectin lice ivermectin 3mg tablets or oral ivermectin cost
http://passage-premier.net/__media__/js/netsoltrademark.php?d=stromectolonline.pro ivermectin ebay
[url=https://www.merkinvestments.com/enter/?url=https://stromectolonline.pro/]generic ivermectin cream[/url] ivermectin new zealand and [url=https://98e.fun/space-uid-6221329.html]ivermectin price canada[/url] ivermectin gel
neurontin 3 neurontin india or neurontin 100mg caps
http://revitalash.net/__media__/js/netsoltrademark.php?d=gabapentin.pro buy cheap neurontin
[url=http://jibbigo.in/__media__/js/netsoltrademark.php?d=gabapentin.pro]neurontin 2400 mg[/url] neurontin generic cost and [url=http://www.9yuanmoli.com/bbs/home.php?mod=space&uid=371170]neurontin without prescription[/url] neurontin 4000 mg
buy azithromycin zithromax [url=http://azithromycin.men/#]zithromax generic price[/url] buy zithromax canada
neurontin cost in singapore: where can i buy neurontin from canada – neurontin prescription medication
paxlovid pill: buy paxlovid online – Paxlovid over the counter
п»їpaxlovid: п»їpaxlovid – paxlovid generic
erection pills that work best pill for ed or how to cure ed
http://metalltechteam.com/__media__/js/netsoltrademark.php?d=ed-pills.men pills for erection
[url=http://dycsincomplejos.com/__media__/js/netsoltrademark.php?d=ed-pills.men]medications for ed[/url] non prescription ed pills and [url=http://www.sportsannouncing.com/community/profile/vzxlukocef/]best otc ed pills[/url] best drug for ed
http://paxlovid.top/# paxlovid pill
best ed pills online: new treatments for ed – top rated ed pills
https://ed-pills.men/# erectile dysfunction pills
online ed medications top ed pills or ed treatment drugs
http://www.andyspares.com/__media__/js/netsoltrademark.php?d=ed-pills.men best pills for ed
[url=http://oklahomalightning.com/__media__/js/netsoltrademark.php?d=ed-pills.men]best ed treatment[/url] ed drugs and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2933668]best over the counter ed pills[/url] new ed drugs
cure ed: male ed drugs – treatment of ed
buy antibiotics from canada Over the counter antibiotics for infection or over the counter antibiotics
http://udotoo.com/__media__/js/netsoltrademark.php?d=antibiotic.guru get antibiotics without seeing a doctor
[url=http://electrictowelheater.com/__media__/js/netsoltrademark.php?d=antibiotic.guru]buy antibiotics[/url] get antibiotics without seeing a doctor and [url=https://quantrinet.com/forum/member.php?u=492464]over the counter antibiotics[/url] buy antibiotics over the counter
buy cipro no rx: buy cipro – п»їcipro generic
https://avodart.pro/# can i order cheap avodart tablets
buy cipro online canada [url=https://ciprofloxacin.ink/#]buy cipro cheap[/url] ciprofloxacin generic
http://avodart.pro/# generic avodart without insurance
buy cipro online usa buy cipro or ciprofloxacin
http://www.lancasterwasteauthority.com/__media__/js/netsoltrademark.php?d=ciprofloxacin.ink buy cipro without rx
[url=http://commersant.org/__media__/js/netsoltrademark.php?d=ciprofloxacin.ink]purchase cipro[/url] п»їcipro generic and [url=http://bbs.94kk.net/home.php?mod=space&uid=7664739]buy cipro no rx[/url] cipro pharmacy
https://avodart.pro/# can i get cheap avodart pills
http://lipitor.pro/# lipitor buy
http://avodart.pro/# cheap avodart without prescription
canada prescription price lipitor [url=http://lipitor.pro/#]buy lipitor online[/url] lipitor 100mg
buy cytotec in usa: buy cytotec over the counter – order cytotec online
http://misoprostol.guru/# cytotec abortion pill
lisinopril uk [url=http://lisinopril.pro/#]zestoretic 20 mg[/url] order cheap lisinopril
http://lipitor.pro/# atorvastatin lipitor
order cytotec online cytotec pills buy online or cytotec pills buy online
http://lasvegasvenues.com/__media__/js/netsoltrademark.php?d=misoprostol.guru buy cytotec
[url=http://legalpermission.com/__media__/js/netsoltrademark.php?d=misoprostol.guru]п»їcytotec pills online[/url] buy cytotec and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2935213]order cytotec online[/url] buy cytotec pills online cheap
https://misoprostol.guru/# buy misoprostol over the counter
buy cheap lipitor online lipitor 20 mg price in india or buy lipitor with mastercard
http://gearheadnation.com/__media__/js/netsoltrademark.php?d=lipitor.pro lipitor 40 mg price comparison
[url=http://mcneil-family.com/__media__/js/netsoltrademark.php?d=lipitor.pro]buy lipitor 10mg[/url] can i buy lipitor online and [url=http://www.wjyjh.cn/home.php?mod=space&uid=4356]buy generic lipitor online[/url] lipitor drug prices
https://lisinopril.pro/# generic for prinivil
canada prescription price lipitor [url=https://lipitor.pro/#]lipitor brand name price[/url] lipitor 100mg
where to get cheap avodart without a prescription order cheap avodart online or cost generic avodart pill
http://tripsplace.org/__media__/js/netsoltrademark.php?d=avodart.pro cost of generic avodart pill
[url=http://liverpool-shopping.com/__media__/js/netsoltrademark.php?d=avodart.pro]can i order avodart for sale[/url] where to get avodart and [url=https://slovakia-forex.com/members/209315-vyouonzcnu]can i order cheap avodart price[/url] where can i get avodart online
https://avodart.pro/# avodart rx
https://misoprostol.guru/# buy cytotec in usa
http://avodart.pro/# can you get cheap avodart prices
Abortion pills online [url=http://misoprostol.guru/#]buy misoprostol over the counter[/url] cytotec buy online usa
https://lipitor.pro/# drug lipitor
п»їcipro generic: ciprofloxacin 500mg buy online – ciprofloxacin
https://misoprostol.guru/# Cytotec 200mcg price
lisinopril 20 mg tablets [url=https://lisinopril.pro/#]best price for lisinopril 20 mg[/url] lisinopril tab 5 mg price
buy lipitor online generic lipitor or lipitor otc
http://ecktemple.com/__media__/js/netsoltrademark.php?d=lipitor.pro lipitor 10mg
[url=http://lindsaykimmel.com/__media__/js/netsoltrademark.php?d=lipitor.pro]buy cheap lipitor online[/url] lipitor generic coupon and [url=http://www.mmecaw.com/home.php?mod=space&uid=409390]generic lipitor 10 mg[/url] cost of lipitor in mexico
Abortion pills online buy misoprostol over the counter or buy cytotec online
http://lymphaticresearch.com/__media__/js/netsoltrademark.php?d=misoprostol.guru Misoprostol 200 mg buy online
[url=http://www.integratingmindandbody.net/__media__/js/netsoltrademark.php?d=misoprostol.guru]purchase cytotec[/url] purchase cytotec and [url=http://www.sempre-roma.com/bbs/home.php?mod=space&uid=469646]buy cytotec in usa[/url] buy cytotec over the counter
ciprofloxacin order online ciprofloxacin generic or buy ciprofloxacin over the counter
http://that70sshow.threemountain.net/__media__/js/netsoltrademark.php?d=ciprofloxacin.ink cipro
[url=http://natspresso.com/__media__/js/netsoltrademark.php?d=ciprofloxacin.ink]ciprofloxacin over the counter[/url] п»їcipro generic and [url=http://www.aipeople.com.cn/home.php?mod=space&uid=3116324]п»їcipro generic[/url] buy cipro online
best online pharmacy india: indianpharmacy com – indian pharmacy online
canadian pharmacy victoza: best rated canadian pharmacy – canadian pharmacy checker
reputable indian online pharmacy Online medicine order or india pharmacy
http://www.paymyhomeheatingbill.com/__media__/js/netsoltrademark.php?d=indiapharmacy.cheap Online medicine home delivery
[url=http://www.timeclub.com/__media__/js/netsoltrademark.php?d=indiapharmacy.cheap]top online pharmacy india[/url] best india pharmacy and [url=https://quantrinet.com/forum/member.php?u=495352]buy prescription drugs from india[/url] cheapest online pharmacy india
world pharmacy india [url=https://indiapharmacy.cheap/#]buy prescription drugs from india[/url] best online pharmacy india
http://mexicanpharmacy.guru/# purple pharmacy mexico price list
buying prescription drugs in mexico online: mexican border pharmacies shipping to usa – mexican online pharmacies prescription drugs
canadian pharmacy 365 canada drugs reviews or canadian pharmacies online
http://austinchristianschool.com/__media__/js/netsoltrademark.php?d=certifiedcanadapills.pro canadian pharmacy reviews
[url=http://directorofnursing.com/__media__/js/netsoltrademark.php?d=certifiedcanadapills.pro]online canadian pharmacy[/url] canadian pharmacy phone number and [url=https://98e.fun/space-uid-6303323.html]my canadian pharmacy[/url] canadian pharmacy 365
my canadian pharmacy [url=https://certifiedcanadapills.pro/#]canadian pharmacy online ship to usa[/url] online pharmacy canada
pills for ed online ed medications or best over the counter ed pills
http://canadianhunterwhisky.com/__media__/js/netsoltrademark.php?d=edpill.men ed meds online without doctor prescription
[url=http://lefetiche.com/__media__/js/netsoltrademark.php?d=edpill.men]best ed pills[/url] compare ed drugs and [url=https://98e.fun/space-uid-6315586.html]pills for erection[/url] erection pills viagra online
Kamagra Oral Jelly buy online Kamagra Oral Jelly buy online or order kamagra oral jelly
http://msntf.com/__media__/js/netsoltrademark.php?d=kamagra.men order kamagra oral jelly
[url=http://stevenhelfman.com/__media__/js/netsoltrademark.php?d=kamagra.men]kamagra[/url] Kamagra Oral Jelly buy online and [url=https://www.clipsharelive.com/user/sxzstgtzlc/videos]kamagra oral jelly[/url] Kamagra tablets 100mg
buy kamagra online buy kamagra or buy kamagra
http://twiddyrentals.com/__media__/js/netsoltrademark.php?d=kamagra.men Kamagra tablets
[url=http://therockandrollshop.com/__media__/js/netsoltrademark.php?d=kamagra.men]Kamagra tablets[/url] buy kamagra and [url=http://xunshang.cc/home.php?mod=space&uid=4035306]Kamagra tablets 100mg[/url] buy kamagra online
cialis online safe purchase brand cialis or levitra vs cialis side effects
http://driversdirect.com/__media__/js/netsoltrademark.php?d=cialis.science best place to get cialis without pesricption
[url=http://neoras.com/__media__/js/netsoltrademark.php?d=cialis.science]canadian cialis[/url] cheap cialis professional and [url=https://masterbationtube.com/user/qterawtckj/videos]cialis women video[/url] cialis dapoxetine australia
best ed treatment pills ed pill or top ed pills
http://j3partnersllc.com/__media__/js/netsoltrademark.php?d=edpill.men erectile dysfunction medications
[url=http://jobs-rus.com/__media__/js/netsoltrademark.php?d=edpill.men]best treatment for ed[/url] treatments for ed and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2941635]ed medications[/url] best ed treatment
ivermectin buy nz ivermectin 1 or stromectol for sale
http://clmforum.com/__media__/js/netsoltrademark.php?d=ivermectin.auction ivermectin syrup
[url=http://thehearingpill.com/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin 12[/url] stromectol coronavirus and [url=http://www.9yuanmoli.com/bbs/home.php?mod=space&uid=386184]ivermectin where to buy[/url] stromectol online canada
buy stromectol ivermectin lotion or ivermectin cost canada
http://whyna.com/__media__/js/netsoltrademark.php?d=ivermectin.auction ivermectin purchase
[url=http://mirasolgreenhouse.org/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin purchase[/url] cost of ivermectin 1% cream and [url=https://bbs.xiaoditech.com/home.php?mod=space&uid=1386530]ivermectin 8000[/url] buy stromectol online
gabapentin neurontin price india or neurontin generic cost
http://importsofstatecollege.com/__media__/js/netsoltrademark.php?d=gabapentin.tech neurontin online pharmacy
[url=http://microcoolinggarment.com/__media__/js/netsoltrademark.php?d=gabapentin.tech]neurontin cost generic[/url] neurontin medicine and [url=http://tc.k33888.cn/home.php?mod=space&uid=2145452]neurontin coupon[/url] neurontin pill
stromectol tablets uk ivermectin syrup or ivermectin coronavirus
http://dearbornfederalsavingsbank.com/__media__/js/netsoltrademark.php?d=ivermectin.auction ivermectin purchase
[url=http://macro-shares.com/__media__/js/netsoltrademark.php?d=ivermectin.auction]stromectol 0.5 mg[/url] buy ivermectin uk and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=2336211]buy stromectol canada[/url] stromectol covid 19
ivermectin price comparison ivermectin cream or ivermectin 4 tablets price
http://www.holidayseasonvillage.com/__media__/js/netsoltrademark.php?d=ivermectin.auction stromectol 3 mg
[url=http://wisn.info/__media__/js/netsoltrademark.php?d=ivermectin.auction]stromectol 3mg[/url] ivermectin 5 mg and [url=http://bbs1.857moli.com/home.php?mod=space&uid=448228]ivermectin generic name[/url] ivermectin pills human
ivermectin uk ivermectin 3mg pill or ivermectin pills
http://jwarchitects.com/__media__/js/netsoltrademark.php?d=ivermectin.auction generic ivermectin cream
[url=http://okusuri.biz/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin new zealand[/url] stromectol ireland and [url=http://bbs.94kk.net/home.php?mod=space&uid=7719002]ivermectin 1 topical cream[/url] ivermectin eye drops
neurontin 400 mg capsule how to get neurontin cheap or order neurontin online
http://redpointventures.net/__media__/js/netsoltrademark.php?d=gabapentin.tech buy gabapentin
[url=http://simcomp.com/__media__/js/netsoltrademark.php?d=gabapentin.tech]neurontin 2018[/url] neurontin 900 mg and [url=http://uued.cn/space-uid-695238.html]neurontin 100mg caps[/url] buying neurontin without a prescription
cytotec abortion pill cytotec online or purchase cytotec
http://berkshiretriadrealestate.net/__media__/js/netsoltrademark.php?d=cytotec.auction buy cytotec in usa
[url=http://dustylane.com/__media__/js/netsoltrademark.php?d=cytotec.auction]buy cytotec pills online cheap[/url] buy cytotec over the counter and [url=http://cos258.com/home.php?mod=space&uid=883350]buy cytotec online[/url] cytotec buy online usa
stromectol tablets uk ivermectin stromectol or ivermectin usa
http://fuzzybutz.net/__media__/js/netsoltrademark.php?d=ivermectin.auction cost of ivermectin cream
[url=http://hecho-en-colombia.com/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin pills[/url] stromectol 3 mg price and [url=http://521boy.com/home.php?mod=space&uid=10839]buy ivermectin nz[/url] ivermectin otc
stromectol for humans generic ivermectin for humans or ivermectin 4 tablets price
http://www.thespaceshowclassroom.biz/__media__/js/netsoltrademark.php?d=ivermectin.auction buy ivermectin for humans uk
[url=http://intimatelandscape.com/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin over the counter[/url] stromectol online pharmacy and [url=http://talk.dofun.cc/home.php?mod=space&uid=4412]ivermectin 50 mg[/url] ivermectin lice
neurontin price uk neurontin 2018 or can you buy neurontin over the counter
http://finediningdiscounts.com/__media__/js/netsoltrademark.php?d=gabapentin.tech buy neurontin
[url=http://tristantaormino.net/__media__/js/netsoltrademark.php?d=gabapentin.tech]where can i buy neurontin from canada[/url] neurontin tablets 100mg and [url=http://wnt1688.cn/home.php?mod=space&uid=6499622]neurontin 100mg caps[/url] canada neurontin 100mg lowest price
best online pharmacy india: Online medication home delivery – pharmacy website india
buying prescription drugs in mexico online medicine in mexico pharmacies or medication from mexico pharmacy
http://bunkerindustries.com/__media__/js/netsoltrademark.php?d=mexicoph.life best online pharmacies in mexico
[url=http://eurojobboard.com/__media__/js/netsoltrademark.php?d=mexicoph.life]purple pharmacy mexico price list[/url] mexican border pharmacies shipping to usa and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=2371839]mexican online pharmacies prescription drugs[/url] purple pharmacy mexico price list
canada drugs online legitimate canadian pharmacies or best online canadian pharmacy
http://nittanyventures.com/__media__/js/netsoltrademark.php?d=canadaph.life canadian pharmacy tampa
[url=http://fgwmexico.com/__media__/js/netsoltrademark.php?d=canadaph.life]certified canadian international pharmacy[/url] canada pharmacy online and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=655352]canada cloud pharmacy[/url] ed meds online canada
indianpharmacy com: Online medication home delivery – reputable indian online pharmacy
top online pharmacy india mail order pharmacy india or indian pharmacy
http://ubaalliance.com/__media__/js/netsoltrademark.php?d=indiaph.life Online medicine home delivery
[url=http://pawnbiz.com/__media__/js/netsoltrademark.php?d=indiaph.life]pharmacy website india[/url] reputable indian pharmacies and [url=http://lsdsng.com/user/486668]buy prescription drugs from india[/url] cheapest online pharmacy india
best canadian online pharmacy best rated canadian pharmacy or canadian pharmacy sarasota
http://www.nuevaprensa.com/__media__/js/netsoltrademark.php?d=canadaph.life reputable canadian online pharmacy
[url=http://skinnytrunk.net/__media__/js/netsoltrademark.php?d=canadaph.life]canadian online drugstore[/url] onlinecanadianpharmacy 24 and [url=http://wnt1688.cn/home.php?mod=space&uid=6522913]best canadian pharmacy online[/url] canadian mail order pharmacy
mexican drugstore online: mexico pharmacies prescription drugs – mexican mail order pharmacies
pharmacies in mexico that ship to usa п»їbest mexican online pharmacies or mexican online pharmacies prescription drugs
http://awsfaq.com/__media__/js/netsoltrademark.php?d=mexicoph.life mexican drugstore online
[url=http://tamprc.com/__media__/js/netsoltrademark.php?d=mexicoph.life]buying from online mexican pharmacy[/url] mexican rx online and [url=http://forum.meogames.com/home.php?mod=space&uid=8865022]mexican rx online[/url] buying from online mexican pharmacy
ivermectin 9 mg ivermectin cost uk or stromectol buy uk
http://www.grupoabadia.com/__media__/js/netsoltrademark.php?d=ivermectin.today stromectol australia
[url=http://drumsey.org/__media__/js/netsoltrademark.php?d=ivermectin.today]ivermectin 10 mg[/url] ivermectin iv and [url=http://plixsite.net/forum/member.php?action=profile&uid=2440137]ivermectin 4000 mcg[/url] ivermectin 6mg dosage
ivermectin oral stromectol 3mg or ivermectin australia
http://bestapplicationdevelopment.com/__media__/js/netsoltrademark.php?d=ivermectin.auction buy ivermectin uk
[url=http://instrumart.nl/__media__/js/netsoltrademark.php?d=ivermectin.auction]ivermectin price usa[/url] stromectol how much it cost and [url=http://www.ziyuangroup.com/space-uid-77673.html]stromectol cost[/url] stromectol buy
ivermectin pills ivermectin gel or can you buy stromectol over the counter
http://julianlennon.gallery/__media__/js/netsoltrademark.php?d=ivermectin.today ivermectin eye drops
[url=http://biker-injury-lawyers.com/__media__/js/netsoltrademark.php?d=ivermectin.today]ivermectin 4 tablets price[/url] ivermectin 10 mg and [url=http://www.emsxl.com/home.php?mod=space&uid=204030]ivermectin 1% cream generic[/url] ivermectin lotion cost
where to buy stromectol buy ivermectin canada or stromectol tablets buy online
http://kidderpeabody.net/__media__/js/netsoltrademark.php?d=ivermectin.today ivermectin australia
[url=http://towelmanagement.com/__media__/js/netsoltrademark.php?d=ivermectin.today]stromectol 3 mg price[/url] stromectol ivermectin tablets and [url=http://www.ziyuangroup.com/space-uid-77895.html]cost of ivermectin cream[/url] buy ivermectin cream
ivermectin 5 ivermectin where to buy for humans or ivermectin syrup
http://kthsystems.com/__media__/js/netsoltrademark.php?d=ivermectinpharmacy.best stromectol covid 19
[url=http://weldingacademy.net/__media__/js/netsoltrademark.php?d=ivermectinpharmacy.best]ivermectin australia[/url] ivermectin online and [url=http://www.88995511.com/home.php?mod=space&uid=601787]ivermectin tablets order[/url] ivermectin coronavirus
stromectol canada ivermectin over the counter or ivermectin oral solution
http://pandoraweb.info/__media__/js/netsoltrademark.php?d=ivermectinpharmacy.best cost of ivermectin pill
[url=http://liveoneastmain.com/__media__/js/netsoltrademark.php?d=ivermectinpharmacy.best]stromectol tablets[/url] stromectol 3mg tablets and [url=http://bbs1.857moli.com/home.php?mod=space&uid=461095]ivermectin brand[/url] ivermectin ebay
canada where to buy neurontin neurontin 300 mg tablet or neurontin 100mg tablets
http://itransfer-esp.com/__media__/js/netsoltrademark.php?d=gabamed.store neurontin 600 mg coupon
[url=http://citizen2gov.us/__media__/js/netsoltrademark.php?d=gabamed.store]neurontin 204[/url] neurontin 3 and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=662778]buy neurontin uk[/url] generic neurontin
lasix uses furosemida or furosemide 40 mg
http://madisonadv.co/__media__/js/netsoltrademark.php?d=lasixfurosemide.store lasix 100 mg
[url=http://softwarelicensingcenter.com/__media__/js/netsoltrademark.php?d=lasixfurosemide.store]lasix furosemide 40 mg[/url] furosemida and [url=http://forum.meogames.com/home.php?mod=space&uid=8974522]furosemide 40 mg[/url] lasix for sale
best canadian pharmacy: canadian pharmacy online – canadian world pharmacy
canadianpharmacy com cross border pharmacy canada or canadian pharmacy 365
http://loleit.com/__media__/js/netsoltrademark.php?d=canadaph.pro safe canadian pharmacy
[url=http://midwestfoldingflstatecontract.com/__media__/js/netsoltrademark.php?d=canadaph.pro]canadian pharmacy store[/url] safe canadian pharmacies and [url=http://www.ziyuangroup.com/space-uid-80246.html]pharmacy rx world canada[/url] canadian pharmacies that deliver to the us
best rated canadian pharmacy canadian pharmacy ratings or canadian online pharmacy reviews
http://dorzagliatin.com/__media__/js/netsoltrademark.php?d=canadaph.pro legit canadian pharmacy
[url=http://aldoaccessories.org/__media__/js/netsoltrademark.php?d=canadaph.pro]drugs from canada[/url] canada pharmacy 24h and [url=https://cracked.sx/member.php?action=profile&uid=174192]canadian compounding pharmacy[/url] canada discount pharmacy
medication from mexico pharmacy: best online pharmacies in mexico – best online pharmacies in mexico
п»їlegitimate online pharmacies india indian pharmacy or Online medicine order
http://companyadviser.com/__media__/js/netsoltrademark.php?d=indiaph.ink online pharmacy india
[url=http://scoregrooming.com/__media__/js/netsoltrademark.php?d=indiaph.ink]mail order pharmacy india[/url] buy medicines online in india and [url=http://qihuo.org.cn/space-uid-215416.html]top 10 pharmacies in india[/url] india pharmacy
no perscription pharmacy [url=https://internationalpharmacy.icu/#]canada pharmacy without prescription[/url] prescription canada
buying canadian drugs online pharmacy online canada or canadian viagra pharmacies
http://obagiprofessionalonline.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu cnadian pharmacy
[url=http://unofficialtrailguide.info/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu]top rated canadian pharmacy online[/url] canadian pharmacy cheap and [url=http://83783.net/home.php?mod=space&uid=7207259]canadian mail order pharmacy[/url] canada drug center promo code
how to get a prescription in canada canandian pharmacy or canadian pharmacies that ship to us
http://rodcrafter.org/__media__/js/netsoltrademark.php?d=interpharm.pro canadianrx
[url=http://tellmyplayer.com/__media__/js/netsoltrademark.php?d=interpharm.pro]order meds from canada[/url] canadian pharmacy en espaГ±ol and [url=http://m.414500.cc/home.php?mod=space&uid=2346147]online pharmacies without prescription[/url] safest online pharmacy
canadiam pharmacy best online canadian pharmacy or us based online pharmacy
http://surplussmartpaper.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu prescription drugs canada
[url=http://academicphysicianandscientist.biz/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu]best online pharmacy canada[/url] canadian rx and [url=http://xunshang.cc/home.php?mod=space&uid=4155184]canadian rx[/url] canada rx drugs online
what is the best online pharmacy what is the best pharmacy in canada or canada drug pharmacy review
http://washingtonexpresslinestanding.info/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu no.rx
[url=http://737studio.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu]buy drugs online from canada[/url] legitimate online pharmacy usa and [url=http://www.118btc.com/home.php?mod=space&uid=656036]buy without perscription[/url] canadian mail order prescriptions
best online pharmacy without prescriptions canada pharmacy store or canadian prescription drugstore review
http://oregonccc.net/__media__/js/netsoltrademark.php?d=interpharm.pro canadian drug co
[url=http://treatfibriods.com/__media__/js/netsoltrademark.php?d=interpharm.pro]online drugstore no prescription[/url] canadianrx and [url=https://kwik.adriensosa.fr/forums/users/fxnmzeameq/]canadian mail order medications[/url] canadian farmacy
best rated canadian pharmacy no presciption needed or mexican rx online
http://braking-sunstar.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu canadian pharmacy online store
[url=http://roundskylight.us/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu]canada pharmacy without prescription[/url] online pharmacies no prescription usa and [url=https://forexzloty.pl/members/314838-dvcojfurkx]no script pharmacy[/url] online pharmacy no prescriptions
https://interpharm.pro/# cheap drugs no prescription
mexican drug stores online – interpharm.pro They provide access to global brands that are hard to find locally.
canadian pharmacy no prescription canafian pharmacy or canadian pharmacy service
http://oakislandcompany.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu non prescription pharmacy
[url=http://fnbot.mobi/__media__/js/netsoltrademark.php?d=internationalpharmacy.icu]medications online without prescription[/url] foreign pharmacies com and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2960627]canada drug pharmacy promo code[/url] canada meds online
farmacia online madrid [url=https://farmaciabarata.pro/#]farmacia barata[/url] farmacia 24h
farmacias baratas online envГo gratis farmacia online barata or п»їfarmacia online
http://losangalex.net/__media__/js/netsoltrademark.php?d=farmaciabarata.pro farmacias baratas online envГo gratis
[url=http://upd8.org/__media__/js/netsoltrademark.php?d=farmaciabarata.pro]farmacia online barata[/url] farmacias baratas online envГo gratis and [url=https://quantrinet.com/forum/member.php?u=514286]п»їfarmacia online[/url] farmacia online barata
farmacie online autorizzate elenco farmacie on line spedizione gratuita or acquistare farmaci senza ricetta
http://www.google.ki/url?q=https://farmaciaonline.men farmacie online sicure
[url=http://tenovai2s.com/__media__/js/netsoltrademark.php?d=farmaciaonline.men]farmacia online piГ№ conveniente[/url] comprare farmaci online con ricetta and [url=http://80tt1.com/home.php?mod=space&uid=85221]farmacia online piГ№ conveniente[/url] farmacia online miglior prezzo
http://pharmacieenligne.icu/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne France Pharmacie en ligne livraison gratuite or Pharmacie en ligne fiable
http://planetreuse.org/__media__/js/netsoltrademark.php?d=pharmacieenligne.icu Pharmacie en ligne livraison gratuite
[url=http://thriftyautosales.org/__media__/js/netsoltrademark.php?d=pharmacieenligne.icu]Pharmacie en ligne sans ordonnance[/url] Pharmacie en ligne pas cher and [url=https://forexzloty.pl/members/316351-pqailsoihl]Pharmacie en ligne pas cher[/url] Pharmacie en ligne pas cher
online apotheke preisvergleich online apotheke gГјnstig or online apotheke versandkostenfrei
http://necusa.biz/__media__/js/netsoltrademark.php?d=onlineapotheke.tech online apotheke versandkostenfrei
[url=http://hairdirectsucks.net/__media__/js/netsoltrademark.php?d=onlineapotheke.tech]online-apotheken[/url] online apotheke deutschland and [url=https://www.ixbren.net/home.php?mod=space&uid=615920]versandapotheke[/url] online apotheke deutschland
http://farmaciaonline.men/# farmacie on line spedizione gratuita
farmacias online seguras en espaГ±a farmacia 24h or farmacia barata
http://rcivacationexchange.net/__media__/js/netsoltrademark.php?d=farmaciabarata.pro farmacia online envГo gratis
[url=http://wawamania.com/__media__/js/netsoltrademark.php?d=farmaciabarata.pro]farmacia 24h[/url] farmacias online seguras en espaГ±a and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1399887]farmacia envГos internacionales[/url] farmacia barata
https://esfarmacia.men/# farmacias online seguras
farmacia online miglior prezzo farmacia online migliore or farmacie online autorizzate elenco
http://nataliedancewear.org/__media__/js/netsoltrademark.php?d=itfarmacia.pro farmacia online piГ№ conveniente
[url=http://www.wittybanter.com/__media__/js/netsoltrademark.php?d=itfarmacia.pro]farmacie on line spedizione gratuita[/url] farmacia online migliore and [url=http://wuyuebanzou.com/home.php?mod=space&uid=370412]acquistare farmaci senza ricetta[/url] farmacia online piГ№ conveniente
farmaci senza ricetta elenco: viagra prezzo generico – farmacia online migliore
п»їpharmacie en ligne acheter mГ©dicaments Г l’Г©tranger or Pharmacie en ligne France
http://intelliprepaid.info/__media__/js/netsoltrademark.php?d=edpharmacie.pro pharmacie ouverte
[url=http://sellatire.com/__media__/js/netsoltrademark.php?d=edpharmacie.pro]Pharmacies en ligne certifiГ©es[/url] Pharmacies en ligne certifiГ©es and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=8613377]п»їpharmacie en ligne[/url] pharmacie ouverte
https://esfarmacia.men/# farmacias baratas online envГo gratis
farmaci senza ricetta elenco farmacia online piГ№ conveniente or farmaci senza ricetta elenco
http://wondr.us/__media__/js/netsoltrademark.php?d=itfarmacia.pro farmacie online affidabili
[url=http://active8tion.com/__media__/js/netsoltrademark.php?d=itfarmacia.pro]farmacie online autorizzate elenco[/url] farmaci senza ricetta elenco and [url=http://www.aiwujie.wang/home.php?mod=space&uid=1565202]comprare farmaci online all’estero[/url] migliori farmacie online 2023
http://esfarmacia.men/# farmacia online madrid
farmacia online barata farmacia online 24 horas or farmacia online 24 horas
http://jfinkelstein.com/__media__/js/netsoltrademark.php?d=esfarmacia.men farmacia 24h
[url=http://votedbestslots.net/__media__/js/netsoltrademark.php?d=esfarmacia.men]farmacia online internacional[/url] farmacia online barata and [url=https://quantrinet.com/forum/member.php?u=515969]farmacia online 24 horas[/url] farmacia envГos internacionales
mexican border pharmacies shipping to usa mexican drugstore online or mexican online pharmacies prescription drugs
http://vietnamantique.org/__media__/js/netsoltrademark.php?d=mexicopharm.store buying from online mexican pharmacy
[url=http://mastercardcorporatecard.info/__media__/js/netsoltrademark.php?d=mexicopharm.store]pharmacies in mexico that ship to usa[/url] purple pharmacy mexico price list and [url=https://tc.yuedotech.com/home.php?mod=space&uid=268253]mexican online pharmacies prescription drugs[/url] mexican mail order pharmacies
pharmacy rx world canada pharmacies in canada that ship to the us or online canadian pharmacy review
http://monsterauctions.com/__media__/js/netsoltrademark.php?d=canadapharm.store canadian pharmacies comparison
[url=http://www.tipodecambio.com/__media__/js/netsoltrademark.php?d=canadapharm.store]best canadian online pharmacy reviews[/url] canadian pharmacy 365 and [url=http://517nn.com/home.php?mod=space&uid=399949]legal canadian pharmacy online[/url] canada ed drugs
п»їlegitimate online pharmacies india indian pharmacy paypal or top 10 online pharmacy in india
http://aqua-tech.motornet.com/__media__/js/netsoltrademark.php?d=indiapharm.cheap india online pharmacy
[url=http://kiyagere.com/__media__/js/netsoltrademark.php?d=indiapharm.cheap]indian pharmacy[/url] world pharmacy india and [url=https://tc.yuedotech.com/home.php?mod=space&uid=268785]top online pharmacy india[/url] reputable indian online pharmacy
indian pharmacies safe: top 10 pharmacies in india – cheapest online pharmacy india
reliable canadian pharmacy reviews drugs from canada or www canadianonlinepharmacy
http://gardnerscandies.us/__media__/js/netsoltrademark.php?d=canadapharm.store canadian discount pharmacy
[url=http://slotchips.com/__media__/js/netsoltrademark.php?d=canadapharm.store]canadian king pharmacy[/url] safe reliable canadian pharmacy and [url=http://plixsite.net/forum/member.php?action=profile&uid=2449564]canadian pharmacy online[/url] canadian online pharmacy reviews
Their medication therapy management is top-notch. trustworthy canadian pharmacy: safe canadian pharmacy – safe online pharmacies in canada
canadian pharmacy price checker: canadadrugpharmacy com – canadian online pharmacy
real canadian pharmacy: canadian discount pharmacy – reliable canadian pharmacy
buying from canadian pharmacies is canadian pharmacy legit or canadian pharmacy com
http://user-manual.org/__media__/js/netsoltrademark.php?d=canadapharm.store real canadian pharmacy
[url=http://www.preservationcarpentry.com/__media__/js/netsoltrademark.php?d=canadapharm.store/]canada rx pharmacy world[/url] canadian pharmacy mall and [url=http://521boy.com/home.php?mod=space&uid=14580]global pharmacy canada[/url] pharmacy canadian superstore
Stellar service in every department. buying prescription drugs in mexico online: medication from mexico pharmacy – mexican mail order pharmacies
online pharmacy india online pharmacy india or top online pharmacy india
http://putasanta.org/__media__/js/netsoltrademark.php?d=indiapharm.cheap online pharmacy india
[url=http://mbkgroup.net/__media__/js/netsoltrademark.php?d=indiapharm.cheap]buy prescription drugs from india[/url] indian pharmacy paypal and [url=https://kwik.adriensosa.fr/forums/users/jqtnfyvgds/]Online medicine order[/url] top 10 online pharmacy in india
buying prescription drugs in mexico online: pharmacies in mexico that ship to usa – medicine in mexico pharmacies
Their global perspective enriches local patient care. buying prescription drugs in mexico online: mexican mail order pharmacies – mexican drugstore online
mexican online pharmacies prescription drugs: mexican drugstore online – mexican online pharmacies prescription drugs
canadian online drugs reputable canadian online pharmacies or canadian online drugstore
http://originatorsnotimitators.net/__media__/js/netsoltrademark.php?d=canadapharm.store thecanadianpharmacy
[url=http://julianlennonphotography.net/__media__/js/netsoltrademark.php?d=canadapharm.store]canadian pharmacy king[/url] best online canadian pharmacy and [url=http://www.9yuanmoli.com/bbs/home.php?mod=space&uid=413585]reputable canadian online pharmacy[/url] canadianpharmacyworld
canadian drug pharmacy best online canadian pharmacy or legitimate canadian pharmacies
http://livehappyfoundation.net/__media__/js/netsoltrademark.php?d=canadapharm.store cheap canadian pharmacy online
[url=http://www.20century.com/__media__/js/netsoltrademark.php?d=canadapharm.store]best canadian pharmacy online[/url] northwest pharmacy canada and [url=http://www.wjyjh.cn/home.php?mod=space&uid=7789]canadian pharmacy checker[/url] canada drugs online reviews
canadian pharmacy meds: canadian pharmacy phone number – reputable canadian pharmacy
Always professional, whether dealing domestically or internationally. indian pharmacies safe: india pharmacy mail order – cheapest online pharmacy india
mexico pharmacies prescription drugs mexico drug stores pharmacies or п»їbest mexican online pharmacies
http://pinderella.com/__media__/js/netsoltrademark.php?d=mexicopharm.store purple pharmacy mexico price list
[url=http://ihatebarryherstein.com/__media__/js/netsoltrademark.php?d=mexicopharm.store]mexico drug stores pharmacies[/url] mexican online pharmacies prescription drugs and [url=http://chunboshi.cn/home.php?mod=space&uid=1652640]mexican mail order pharmacies[/url] mexican rx online
india pharmacy mail order india pharmacy mail order or best online pharmacy india
http://barbadostridents.com/__media__/js/netsoltrademark.php?d=indiapharm.cheap best india pharmacy
[url=http://joesinterweb.com/main.php?g2_view=core.UserAdmin&g2_subView=core.UserLogin&g2_return=https://indiapharm.cheap]Online medicine order[/url] indian pharmacy and [url=http://cos258.com/home.php?mod=space&uid=934974]online shopping pharmacy india[/url] best india pharmacy
Online medicine order: india online pharmacy – indian pharmacy
Pharmacists who are passionate about what they do. buying prescription drugs in mexico online: buying prescription drugs in mexico online – mexican rx online
canadian pharmacy victoza canadian pharmacy meds or canadian pharmacy world reviews
http://www.greensboroswolf.com/__media__/js/netsoltrademark.php?d=canadapharm.store canada drugs online reviews
[url=http://westernstatesec.com/__media__/js/netsoltrademark.php?d=canadapharm.store]canadian online pharmacy[/url] canadian online drugs and [url=http://www.ziyuangroup.com/space-uid-85667.html]buying drugs from canada[/url] canadian pharmacy scam
www canadianonlinepharmacy canada ed drugs or canadian drugs
http://gregrussellmusic.com/__media__/js/netsoltrademark.php?d=canadapharm.store canadian pharmacy
[url=http://allaccessmusic.com/__media__/js/netsoltrademark.php?d=canadapharm.store]safe online pharmacies in canada[/url] canadian valley pharmacy and [url=https://quantrinet.com/forum/member.php?u=519769]canadian pharmacy ltd[/url] canadian online drugs
vipps approved canadian online pharmacy: reputable canadian pharmacy – canadianpharmacymeds
Their worldwide delivery system is impeccable. https://edpillsotc.store/# top ed drugs
Their global perspective enriches local patient care. top erection pills: best male enhancement pills – natural ed medications
doxycycline 75 mg price [url=http://doxycyclineotc.store/#]buy doxycycline online[/url] doxycycline singapore pharmacy
They offer international health solutions without borders. http://edpillsotc.store/# pills for erection
ed medication ed pills cheap or compare ed drugs
http://www.southernrealtor.net/__media__/js/netsoltrademark.php?d=edpillsotc.store ed treatment pills
[url=http://localmobilenotary.com/__media__/js/netsoltrademark.php?d=edpillsotc.store]buy ed pills online[/url] erectile dysfunction medicines and [url=http://www.pcwhsn.com/home.php?mod=space&uid=500150]ed treatment review[/url] best male enhancement pills
ed medications list ed pills that work or best ed pills at gnc
http://pigfestkeywest.com/__media__/js/netsoltrademark.php?d=edpillsotc.store ed pills cheap
[url=http://popscosmetics.biz/__media__/js/netsoltrademark.php?d=edpillsotc.store]cures for ed[/url] cures for ed and [url=http://www.so0912.com/home.php?mod=space&uid=1866094]drugs for ed[/url] best erectile dysfunction pills
http://azithromycinotc.store/# where can i buy zithromax capsules
They have an extensive range of skincare products. http://doxycyclineotc.store/# doxycycline 25mg tablets
zithromax 500 mg for sale generic zithromax 500mg or where can i get zithromax over the counter
http://ww17.visionaryconcepts.com/__media__/js/netsoltrademark.php?d=azithromycinotc.store buy generic zithromax online
[url=http://deltacentrifugal.info/__media__/js/netsoltrademark.php?d=azithromycinotc.store]buy zithromax online cheap[/url] buy zithromax and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=5973863]zithromax 600 mg tablets[/url] generic zithromax medicine
best ed drugs [url=https://edpillsotc.store/#]buy ed pills[/url] non prescription ed pills
Their global outlook is evident in their expansive services. https://edpillsotc.store/# erection pills
doxycycline 20 mg cost doxycycline capsules 40 mg or online doxycycline prescription
http://mynextraq.org/__media__/js/netsoltrademark.php?d=doxycyclineotc.store doxycycline 100mg cost uk
[url=http://julian-lennon.photography/__media__/js/netsoltrademark.php?d=doxycyclineotc.store]doxycycline 100mg price 1mg[/url] doxycycline 40 mg capsules and [url=http://www.9kuan9.com/home.php?mod=space&uid=134562]doxycycline australia[/url] doxycycline price usa
Read here. http://azithromycinotc.store/# zithromax z-pak price without insurance
Leading the charge in international pharmacy standards. http://indianpharmacy.life/# best online pharmacy india
india online pharmacy [url=http://indianpharmacy.life/#]india pharmacy[/url] world pharmacy india
Their medication synchronization service is fantastic. https://mexicanpharmacy.site/# reputable mexican pharmacies online
purple pharmacy mexico price list buying prescription drugs in mexico or mexico drug stores pharmacies
http://www.lifeflourgroup.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.site pharmacies in mexico that ship to usa
[url=http://recycle-west.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.site]mexican pharmaceuticals online[/url] best online pharmacies in mexico and [url=http://www.pcwhsn.com/home.php?mod=space&uid=500710]purple pharmacy mexico price list[/url] п»їbest mexican online pharmacies
reliable rx pharmacy pharmacy websites or what’s the best online pharmacy
http://salinasventures.com/__media__/js/netsoltrademark.php?d=drugsotc.pro canadian online pharmacy viagra
[url=http://hospitalitysupplymanagement.com/__media__/js/netsoltrademark.php?d=drugsotc.pro]online shopping pharmacy india[/url] viagra canadian pharmacy vipps approved and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=681983]escrow pharmacy canada[/url] canadian pharmacy world coupon
The best choice for personalized care. http://drugsotc.pro/# canadian pharmacy
india online pharmacy cheapest online pharmacy india or india online pharmacy
http://newlion.org/__media__/js/netsoltrademark.php?d=indianpharmacy.life reputable indian pharmacies
[url=http://lookingforhim.com/__media__/js/netsoltrademark.php?d=indianpharmacy.life]indian pharmacies safe[/url] mail order pharmacy india and [url=http://www.9yuanmoli.com/bbs/home.php?mod=space&uid=418958]mail order pharmacy india[/url] top online pharmacy india
They always keep my medication history well-organized. https://indianpharmacy.life/# reputable indian pharmacies
best european online pharmacy [url=https://drugsotc.pro/#]canadian pharmacy without prescription[/url] legit canadian online pharmacy
safe canadian pharmacy worldwide pharmacy online or canadien pharmacies
http://7riversregionvisitor.com/__media__/js/netsoltrademark.php?d=drugsotc.pro discount pharmacy online
[url=http://buttonwoodventures.com/__media__/js/netsoltrademark.php?d=drugsotc.pro]buying prescription drugs from canada[/url] trustworthy online pharmacy and [url=http://www.whatsapap.com/home.php?mod=space&uid=485336]affordable pharmacy[/url] canada pharmacy online
best online pharmacy online canadian pharmacy coupon or online pharmacy worldwide shipping
http://www.modelpro.com/__media__/js/netsoltrademark.php?d=drugsotc.pro canadian pharmacy world coupons
[url=http://rapid-facts.net/__media__/js/netsoltrademark.php?d=drugsotc.pro]77 canadian pharmacy[/url] canadianpharmacymeds com and [url=http://xunshang.cc/home.php?mod=space&uid=4230036]canada drug pharmacy[/url] canadian online pharmacy no prescription
indian pharmacy online shopping pharmacy india or top 10 online pharmacy in india
http://franciscanvocations.org/__media__/js/netsoltrademark.php?d=indianpharmacy.life mail order pharmacy india
[url=http://routingmetal.com/__media__/js/netsoltrademark.php?d=indianpharmacy.life]top 10 pharmacies in india[/url] indian pharmacy online and [url=http://plixsite.net/forum/member.php?action=profile&uid=2453832]online shopping pharmacy india[/url] indian pharmacy
mexican rx online purple pharmacy mexico price list or purple pharmacy mexico price list
http://voyerrooms.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.site pharmacies in mexico that ship to usa
[url=http://halfacar.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.site]buying prescription drugs in mexico[/url] medication from mexico pharmacy and [url=http://wnt1688.cn/home.php?mod=space&uid=6747027]medication from mexico pharmacy[/url] mexican border pharmacies shipping to usa
The one-stop solution for all international medication requirements. http://mexicanpharmacy.site/# mexican border pharmacies shipping to usa
“One of the major obstacles in the world of crypto is the complex process of paying for transactions or operations on blockchains. Each operation, whether it’s a simple token transfer or a more intricate interaction with a smart contract, incurs a cost known as a ‘gas’ fee. In the case of Ethereum, this gas fee must be paid in the blockchain’s native token, ETH,” Visa said. A connection to the Ethereum network (a Provider) Holds your private key and can sign things (a Signer) For explanations of our data calculations, check docs.oneland.world . For metaverse market and project data, check oneland.world. However, how does Visa streamline transaction fee payments on the blockchain? According to the diagram provided by Visa, a user seeking to buy $200 worth of Ether (ETH) on a crypto trading platform with only $1000 USD Coin (USDC) and no ETH can initiate the transaction in a self-custodial wallet that supports ERC-4437. They can then opt for a Visa Card to cover the gas fees.
http://www.moaprint.com/bbs/board.php?bo_table=free&wr_id=27767
On the flip side, a rejection from the $30,476 level could see Bitcoin price move back below the 50-day EMA and lower to break below the $28,806 support level before tagging the 100-day EMA at $28,690. If this support level fails to hold, BTC could continue south to tag the 200-day EMA at $27,265 or, in the dire case, extend to the June 19 low at around $26,344. The largest cryptocurrency has climbed more than 20% since March 1, when it was trading slightly above $23,000. Given the bullish month for BTC, investors already have their eyes set on the near-term price for the end of April, hoping the asset can experience similar growth. Bitcoin Price Analysis: Orbiting 30491 Technicals – 3 July 2023 2023 07 02 – 11:00BTC USD Orbiting 30491 Technicals: Sally Ho’s Technical Analysis – 3 July 2023 Bitcoin (BTC USD) sought fresh technical guidance early in the Asian session as the pair continued to orbit the 30491.62 area, representing the 50% retracement of the appreciating range from 29539.57 to 31443.67. The pair’s recent depreciation to the 29417.14 area represented a test of the 38.2% retracement of the appreciating range from 26165.98 to 31443.67. The decline occurred after BTC USD spiked higher to t info
mexico drug stores pharmacies [url=https://mexicanpharmacy.site/#]buy drugs at mexican pharmacy[/url] mexican border pharmacies shipping to usa
what’s the best online pharmacy canadian pharmacy coupon or brazilian pharmacy online
http://puntosportodo.biz/__media__/js/netsoltrademark.php?d=drugsotc.pro canadian pharmacy discount coupon
[url=http://trumpinternationalhotelandtowerchicago.com/__media__/js/netsoltrademark.php?d=drugsotc.pro]canadian pharmacy reviews[/url] canadian family pharmacy and [url=http://www.mmecaw.com/home.php?mod=space&uid=432941]reputable canadian pharmacy[/url] online pharmacy same day delivery
on line pharmacy pharmacy rx world canada or online pharmacy without prescription
http://imecheregions.org/__media__/js/netsoltrademark.php?d=drugsotc.pro online pharmacy group
[url=http://vegetariancapsules.com/__media__/js/netsoltrademark.php?d=drugsotc.pro]reputable online pharmacy no prescription[/url] online pharmacy europe and [url=http://cos258.com/home.php?mod=space&uid=962860]canadian pharmacy viagra[/url] pharmacy rx
The best choice for personalized care. http://mexicanpharmacy.site/# medication from mexico pharmacy
Their global presence ensures prompt medication deliveries. https://drugsotc.pro/# canadian pharmacy mall
buy meds online no prescription top rated online pharmacy or online pharmacy mexico
http://anesthesialibrary.org/__media__/js/netsoltrademark.php?d=internationalpharmacy.pro top online pharmacies
[url=http://quantumdigitol.com/__media__/js/netsoltrademark.php?d=internationalpharmacy.pro]online meds no prescription[/url] best mexican pharmacies and [url=https://www.ixbren.net/home.php?mod=space&uid=627673]no perscription required[/url] global pharmacy canada order form
best online canadian pharmacy canadian pharmacy cheap or canadian drug
http://omnireservations.com/__media__/js/netsoltrademark.php?d=canadapharmacy.cheap best online canadian pharmacy
[url=http://appliance-part.com/__media__/js/netsoltrademark.php?d=canadapharmacy.cheap]canadian pharmacy 24 com[/url] canadian pharmacies that deliver to the us and [url=https://slovakia-forex.com/members/222700-wrtmmugkud]safe canadian pharmacies[/url] legal canadian pharmacy online
Their home delivery service is top-notch. https://canadapharmacy.cheap/# legal canadian pharmacy online
neurontin price india: order neurontin – neurontin canada
canadian pharmacy mall best canadian pharmacy online or canadian pharmacy com
http://dinnerthere.com/__media__/js/netsoltrademark.php?d=canadapharmacy.cheap canadian pharmacy no scripts
[url=http://arabvision.us/__media__/js/netsoltrademark.php?d=canadapharmacy.cheap]canadian family pharmacy[/url] canadian pharmacy in canada and [url=http://43.143.201.219/home.php?mod=space&uid=92124]canadian 24 hour pharmacy[/url] canadian 24 hour pharmacy
canadian pharmacies online: canadian international pharmacy – www canadian pharmacy
A beacon of reliability and trust. http://mexicanpharmonline.shop/# mexico drug stores pharmacies
mexican mail order pharmacies [url=http://mexicanpharmonline.com/#]mexico online pharmacy[/url] medicine in mexico pharmacies
mexico pharmacies prescription drugs mexican pharmaceuticals online or medication from mexico pharmacy
http://sightsoundmotion.com/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop purple pharmacy mexico price list
[url=http://xactprice.org/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop]buying from online mexican pharmacy[/url] mexico pharmacies prescription drugs and [url=http://www.9kuan9.com/home.php?mod=space&uid=139607]best online pharmacies in mexico[/url] п»їbest mexican online pharmacies
mexico pharmacies prescription drugs buying prescription drugs in mexico online or pharmacies in mexico that ship to usa
http://orderfundinfo.us/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop buying from online mexican pharmacy
[url=http://okvet.com/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop]mexican border pharmacies shipping to usa[/url] mexico drug stores pharmacies and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1413295]best online pharmacies in mexico[/url] mexican online pharmacies prescription drugs
mexican mail order pharmacies : mexican pharmacies – п»їbest mexican online pharmacies
buying prescription drugs in mexico mexican mail order pharmacies or mexico drug stores pharmacies
http://www.gerberacapital.net/__media__/js/netsoltrademark.php?d=mexicanpharmonline.com mexican rx online
[url=http://mygt-advisor.biz/__media__/js/netsoltrademark.php?d=mexicanpharmonline.com]medicine in mexico pharmacies[/url] mexican drugstore online and [url=https://www.ixbren.net/home.php?mod=space&uid=629790]mexico pharmacies prescription drugs[/url] mexican rx online
Always greeted with warmth and professionalism. http://mexicanpharmonline.com/# mexican border pharmacies shipping to usa
mexican border pharmacies shipping to usa [url=http://mexicanpharmonline.shop/#]mexico pharmacy online[/url] medication from mexico pharmacy
buying prescription drugs in mexico online – mexican pharmacy – mexico pharmacy
buying from online mexican pharmacy and mexico pharmacy online – mexican drugstore online
The go-to place for all my healthcare needs. http://mexicanpharmonline.shop/# mexico drug stores pharmacies
reputable mexican pharmacies online [url=http://mexicanpharmonline.com/#]reputable mexican pharmacies online[/url] medicine in mexico pharmacies
mexican border pharmacies shipping to usa п»їbest mexican online pharmacies or mexican online pharmacies prescription drugs
http://technovirus.com/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop pharmacies in mexico that ship to usa
[url=http://statmethods.com/__media__/js/netsoltrademark.php?d=mexicanpharmonline.shop]buying from online mexican pharmacy[/url] medication from mexico pharmacy and [url=http://101.34.208.228/home.php?mod=space&uid=376631]best online pharmacies in mexico[/url] buying prescription drugs in mexico online
medicine in mexico pharmacies and mexico pharmacy online – best online pharmacies in mexico
https://canadapharmacy24.pro/# reputable canadian online pharmacies
top 10 online pharmacy in india: india pharmacy – world pharmacy india
ivermectin topical: stromectol order online – minocycline 50
online shopping pharmacy india indian pharmacies safe or online shopping pharmacy india
http://dallasrugbyfoundation.org/__media__/js/netsoltrademark.php?d=indiapharmacy24.pro india pharmacy
[url=http://modabee.net/__media__/js/netsoltrademark.php?d=indiapharmacy24.pro]cheapest online pharmacy india[/url] online pharmacy india and [url=https://hdkaraokesong.com/space-uid-250935.html]top online pharmacy india[/url] india pharmacy mail order
https://indiapharmacy24.pro/# india online pharmacy
northwest canadian pharmacy canada drugs online reviews or canadian pharmacy king reviews
http://www.metees.com/__media__/js/netsoltrademark.php?d=canadapharmacy24.pro ordering drugs from canada
[url=http://coachedondemand.com/__media__/js/netsoltrademark.php?d=canadapharmacy24.pro]certified canadian international pharmacy[/url] canadianpharmacymeds and [url=http://lsdsng.com/user/497969]canadian pharmacy world reviews[/url] canadian world pharmacy
onlinecanadianpharmacy 24: best pharmacy online – canada pharmacy online legit
https://indiapharmacy24.pro/# indian pharmacies safe
ivermectin pills human ivermectin tablets order or ivermectin ireland
http://chrisbrubeck.biz/__media__/js/netsoltrademark.php?d=stromectol24.pro minocycline capsules 100mg
[url=http://ishopaa.com/__media__/js/netsoltrademark.php?d=stromectol24.pro]ivermectin 3 mg tabs[/url] ivermectin price and [url=http://www.so0912.com/home.php?mod=space&uid=1889938]acne minocycline[/url] ivermectin 1
safe canadian pharmacy: Pharmacies in Canada that ship to the US – global pharmacy canada
cheapest online pharmacy india indian pharmacy online or india pharmacy
http://swingingballs.com/__media__/js/netsoltrademark.php?d=indiapharmacy24.pro online pharmacy india
[url=http://lasalledesign.com/__media__/js/netsoltrademark.php?d=indiapharmacy24.pro]reputable indian online pharmacy[/url] best india pharmacy and [url=http://forum.meogames.com/home.php?mod=space&uid=9121457]cheapest online pharmacy india[/url] reputable indian pharmacies
http://indiapharmacy24.pro/# indianpharmacy com
canadian neighbor pharmacy canada pharmacy or northwest canadian pharmacy
http://f1rstpay.org/__media__/js/netsoltrademark.php?d=canadapharmacy24.pro canadian pharmacy drugs online
[url=http://southwestsmart.com/__media__/js/netsoltrademark.php?d=canadapharmacy24.pro]canadian valley pharmacy[/url] reputable canadian pharmacy and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=2602165]the canadian drugstore[/url] canadian pharmacy online
where can i buy cheap mobic without a prescription: cost of mobic for sale – can you buy mobic no prescription
https://plavix.guru/# plavix best price
ivermectin 5 [url=https://stromectol.icu/#]stromectol 3 mg price[/url] ivermectin 24 mg
http://valtrex.auction/# valtrex australia buy
ivermectin cost australia ivermectin lotion cost or ivermectin generic cream
http://kenfisherinvestmentloss.com/__media__/js/netsoltrademark.php?d=stromectol.icu stromectol how much it cost
[url=http://huntingtonlearnctr.com/__media__/js/netsoltrademark.php?d=stromectol.icu]ivermectin 4[/url] stromectol 6 mg dosage and [url=https://www.warshipsfaq.ru/user/cnswvceqqa]stromectol drug[/url] ivermectin rx
paxlovid generic paxlovid buy or paxlovid price
http://mychurchfundraisers.com/__media__/js/netsoltrademark.php?d=paxlovid.bid paxlovid pill
[url=http://oilequalsdeath.net/__media__/js/netsoltrademark.php?d=paxlovid.bid]Paxlovid buy online[/url] paxlovid india and [url=http://forum.meogames.com/home.php?mod=space&uid=9123080]paxlovid pill[/url] paxlovid cost without insurance
how to get mobic tablets: buy anti-inflammatory drug – where can i get generic mobic without a prescription
https://paxlovid.bid/# paxlovid price
where buy generic mobic without rx [url=https://mobic.icu/#]cheap meloxicam[/url] how to get mobic prices
http://stromectol.icu/# ivermectin 2mg
generic plavix: generic plavix – clopidogrel bisulfate 75 mg
can you buy cheap mobic pills: Mobic meloxicam best price – how to buy mobic
valtrex over counter buy valtrex singapore or order valtrex generic
http://vancouverumbrellashop.com/__media__/js/netsoltrademark.php?d=valtrex.auction can you buy valtrex over the counter in canada
[url=http://lpacks.com/__media__/js/netsoltrademark.php?d=valtrex.auction]canadian pharmacy valtrex[/url] buy generic valtrex on line and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6068428]buy valtrex online in usa[/url] valtrex cost india
http://valtrex.auction/# valtrex generic price canada
minocycline 50 mg tablet: ivermectin generic cream – buy minocycline 100 mg online
http://paxlovid.bid/# paxlovid cost without insurance
generic plavix [url=http://plavix.guru/#]Plavix 75 mg price[/url] plavix medication
Paxlovid buy online Paxlovid over the counter or paxlovid pharmacy
http://artbaselasia.com/__media__/js/netsoltrademark.php?d=paxlovid.bid paxlovid cost without insurance
[url=http://worldwidepackagingllc.com/__media__/js/netsoltrademark.php?d=paxlovid.bid]paxlovid pill[/url] paxlovid for sale and [url=http://www.empyrethegame.com/forum/memberlist.php?mode=viewprofile&u=268095]paxlovid buy[/url] paxlovid india
п»їplavix generic: Cost of Plavix without insurance – Cost of Plavix on Medicare
minocycline hydrochloride: ivermectin 50ml – п»їwhere to buy stromectol online
paxlovid pill: nirmatrelvir and ritonavir online – buy paxlovid online
http://stromectol.icu/# order minocycline 100mg
can you get mobic pill [url=https://mobic.icu/#]cheap meloxicam[/url] where can i buy cheap mobic tablets
https://levitra.eus/# Levitra tablet price
Generic Levitra 20mg [url=http://levitra.eus/#]Generic Levitra 20mg[/url] Levitra generic best price
Viagra Tablet price Cheap Sildenafil 100mg or sildenafil 50 mg price
http://obgynassociates.us/__media__/js/netsoltrademark.php?d=viagra.eus Generic Viagra online
[url=http://north-american-watergardens.com/__media__/js/netsoltrademark.php?d=viagra.eus]Generic Viagra online[/url] Order Viagra 50 mg online and [url=https://forexzloty.pl/members/327604-vrbghlujkq]Generic Viagra for sale[/url] buy Viagra online
Generic Cialis price Buy Cialis online or buy cialis pill
http://healthcooperative.co/__media__/js/netsoltrademark.php?d=cialis.foundation Cialis 20mg price in USA
[url=http://mirabelgolf.net/__media__/js/netsoltrademark.php?d=cialis.foundation]Buy Tadalafil 20mg[/url] Buy Tadalafil 5mg and [url=http://wnt1688.cn/home.php?mod=space&uid=6754120]Tadalafil Tablet[/url] п»їcialis generic
http://cialis.foundation/# Tadalafil Tablet
http://kamagra.icu/# Kamagra 100mg price
order viagra [url=https://viagra.eus/#]Sildenafil 100mg price[/url] cheap viagra
super kamagra super kamagra or Kamagra Oral Jelly
http://historyofpharmacy.com/__media__/js/netsoltrademark.php?d=kamagra.icu buy kamagra online usa
[url=http://larucorporation.us/__media__/js/netsoltrademark.php?d=kamagra.icu]sildenafil oral jelly 100mg kamagra[/url] buy Kamagra and [url=http://www.9yuanmoli.com/bbs/home.php?mod=space&uid=430342]super kamagra[/url] Kamagra tablets
http://levitra.eus/# Buy Vardenafil online
https://kamagra.icu/# Kamagra tablets
Kamagra 100mg price [url=http://kamagra.icu/#]buy kamagra online usa[/url] buy Kamagra
Generic Cialis without a doctor prescription Cialis 20mg price in USA or Generic Cialis price
http://sacajaweaplaza.com/__media__/js/netsoltrademark.php?d=cialis.foundation Cialis without a doctor prescription
[url=http://scadsucks.info/__media__/js/netsoltrademark.php?d=cialis.foundation]Generic Cialis without a doctor prescription[/url] Buy Tadalafil 5mg and [url=http://qihuo.org.cn/space-uid-257165.html]Generic Cialis price[/url] Cialis without a doctor prescription
Buy Viagra online cheap sildenafil over the counter or cheapest viagra
http://jeffreygrillo.org/__media__/js/netsoltrademark.php?d=viagra.eus Generic Viagra for sale
[url=http://oceancity.pro/__media__/js/netsoltrademark.php?d=viagra.eus]Viagra without a doctor prescription Canada[/url] buy Viagra over the counter and [url=http://www.xiaolanmb.com/space-uid-17767.html]generic sildenafil[/url] Buy Viagra online cheap
100 percent free online dating sites worth the basic functions of dating in toronto each year. Like a date can be. Has several tools; you need for a match will be honest it is also not easy for singles 247 is the name. Which dating or personals site for singles don’t cost any closer to make new options and. The new people they might not get what you pay for those. Do you imagine that 24-hour countdown worries you are actually free dating sites have to change without payment. The collection and processing of information about your use of this service to subsequently personalise advertising and or content for you in other contexts, such as on other websites or apps, over time. Typically, the content of the site or app is used to make inferences about your interests, which inform future selection of advertising and or content.
https://www.mapleprimes.com/users/g1xlldp176
Trust is the key element of long-term relationships. You only need attraction and trust if you want a long-lasting emotional connection with women. In order to get into a more intimate environment with you, she needs to trust you. They want to feel safe with a man who understands them. Downloading a dating app can seem like a big commitment and feel a little bit overwhelming if you’re not sure which to try first since they all have extremely different vibes. Hinge is the best option if you’re looking to get a little bit more serious about app dating. It gives you more information about potential dates and encourages more meaningful conversations. Raya is ideal if you’re hoping to spot a celebrity or want to network with other like-minded creatives, but it can be difficult to get an invite to it.
http://kamagra.icu/# п»їkamagra
https://kamagra.icu/# Kamagra 100mg price
Cheap Sildenafil 100mg [url=https://viagra.eus/#]Viagra generic over the counter[/url] Viagra online price
https://kamagra.icu/# п»їkamagra
http://kamagra.icu/# Kamagra 100mg
http://kamagra.icu/# super kamagra
super kamagra cheap kamagra or buy Kamagra
http://next123.com/__media__/js/netsoltrademark.php?d=kamagra.icu buy Kamagra
[url=http://bounceclick.net/__media__/js/netsoltrademark.php?d=kamagra.icu]Kamagra 100mg price[/url] cheap kamagra and [url=http://bbs1.857moli.com/home.php?mod=space&uid=491984]Kamagra 100mg price[/url] buy kamagra online usa
Generic Cialis price Cheap Cialis or Cialis without a doctor prescription
http://bassplayerforhire.com/__media__/js/netsoltrademark.php?d=cialis.foundation cheapest cialis
[url=http://merjantgroup.com/__media__/js/netsoltrademark.php?d=cialis.foundation]Buy Tadalafil 10mg[/url] Generic Cialis price and [url=http://lsdsng.com/user/499943]buy cialis pill[/url] cialis for sale
Buy Tadalafil 20mg [url=https://cialis.foundation/#]Cialis over the counter[/url] Cheap Cialis
Viagra online price order viagra or generic sildenafil
http://wmar.net/__media__/js/netsoltrademark.php?d=viagra.eus sildenafil online
[url=https://kentei.cc/jump.php?url=http://viagra.eus]Viagra Tablet price[/url] Viagra tablet online and [url=http://80tt1.com/home.php?mod=space&uid=96656]viagra canada[/url] Generic Viagra for sale
http://viagra.eus/# cheap viagra
buy cialis pill [url=http://cialis.foundation/#]Buy Tadalafil 5mg[/url] Cialis 20mg price
https://kamagra.icu/# Kamagra Oral Jelly
https://viagra.eus/# Sildenafil 100mg price
Buy Tadalafil 20mg Cheap Cialis or Cialis over the counter
http://altectruck.com/__media__/js/netsoltrademark.php?d=cialis.foundation Tadalafil price
[url=http://55heart.com/__media__/js/netsoltrademark.php?d=cialis.foundation]Generic Cialis price[/url] Generic Cialis without a doctor prescription and [url=http://517nn.com/home.php?mod=space&uid=416288]Cialis 20mg price[/url] Buy Tadalafil 20mg
Cialis over the counter [url=http://cialis.foundation/#]buy cialis pill[/url] Cheap Cialis
https://kamagra.icu/# Kamagra 100mg price
https://indiapharmacy.pro/# top 10 online pharmacy in india indiapharmacy.pro
cheap canadian pharmacy online: the canadian pharmacy – online canadian pharmacy canadapharmacy.guru
indian pharmacies safe [url=https://indiapharmacy.pro/#]reputable indian pharmacies[/url] п»їlegitimate online pharmacies india indiapharmacy.pro
purple pharmacy mexico price list: п»їbest mexican online pharmacies – mexican rx online mexicanpharmacy.company
my canadian pharmacy: best canadian pharmacy – canada pharmacy 24h canadapharmacy.guru
buying prescription drugs in mexico online: mexico drug stores pharmacies – п»їbest mexican online pharmacies mexicanpharmacy.company
canadian pharmacy drugs online [url=https://canadapharmacy.guru/#]canada pharmacy[/url] online canadian pharmacy reviews canadapharmacy.guru
mexican mail order pharmacies: buying prescription drugs in mexico online – best online pharmacies in mexico mexicanpharmacy.company
http://mexicanpharmacy.company/# reputable mexican pharmacies online mexicanpharmacy.company
reputable indian pharmacies indian pharmacy paypal or indian pharmacies safe
http://www.redridetaxi.net/__media__/js/netsoltrademark.php?d=indiapharmacy.pro indian pharmacy online
[url=http://roblock.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]india online pharmacy[/url] indian pharmacies safe and [url=http://www.xiaolanmb.com/space-uid-18284.html]indian pharmacy paypal[/url] india pharmacy mail order
mexican rx online mexican pharmaceuticals online or mexico drug stores pharmacies
http://fiberdoor.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company medicine in mexico pharmacies
[url=http://internshipsmexico.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company]buying from online mexican pharmacy[/url] best online pharmacies in mexico and [url=http://m.414500.cc/home.php?mod=space&uid=2610866]mexican drugstore online[/url] medicine in mexico pharmacies
medicine in mexico pharmacies: buying from online mexican pharmacy – mexican mail order pharmacies mexicanpharmacy.company
п»їbest mexican online pharmacies [url=http://mexicanpharmacy.company/#]mexico pharmacies prescription drugs[/url] mexico pharmacies prescription drugs mexicanpharmacy.company
http://mexicanpharmacy.company/# mexican drugstore online mexicanpharmacy.company
best online pharmacies in mexico: buying from online mexican pharmacy – medicine in mexico pharmacies mexicanpharmacy.company
reputable indian online pharmacy: online pharmacy india – indian pharmacies safe indiapharmacy.pro
best india pharmacy: pharmacy website india – reputable indian online pharmacy indiapharmacy.pro
best online pharmacies in mexico [url=http://mexicanpharmacy.company/#]best online pharmacies in mexico[/url] mexico pharmacies prescription drugs mexicanpharmacy.company
http://mexicanpharmacy.company/# mexican mail order pharmacies mexicanpharmacy.company
canadian pharmacy ltd canadian medications or best online canadian pharmacy
http://dbaland.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru canada pharmacy online
[url=http://academysportsandoutdoor.biz/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]best canadian pharmacy[/url] canadianpharmacyworld com and [url=https://cracked.sx/member.php?action=profile&uid=183674]adderall canadian pharmacy[/url] certified canadian international pharmacy
buy prescription drugs from india top online pharmacy india or india pharmacy
http://ashleyleasure.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro indianpharmacy com
[url=http://stephen-lin.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]indianpharmacy com[/url] reputable indian online pharmacy and [url=http://www.sanclick.com/member.php?754435-sedittjnfe]canadian pharmacy india[/url] cheapest online pharmacy india
https://indiapharmacy.pro/# п»їlegitimate online pharmacies india indiapharmacy.pro
buy medicines online in india: Online medicine home delivery – pharmacy website india indiapharmacy.pro
pharmacies in mexico that ship to usa: pharmacies in mexico that ship to usa – buying from online mexican pharmacy mexicanpharmacy.company
purple pharmacy mexico price list [url=https://mexicanpharmacy.company/#]buying prescription drugs in mexico online[/url] п»їbest mexican online pharmacies mexicanpharmacy.company
northern pharmacy canada cheap canadian pharmacy online or best canadian pharmacy
http://perspectivesontheworldchristianmovement.org/__media__/js/netsoltrademark.php?d=canadapharmacy.guru safe reliable canadian pharmacy
[url=http://www.kaustus.biz/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]canadian compounding pharmacy[/url] reliable canadian pharmacy reviews and [url=http://www.yizefangxi.com/home.php?mod=space&uid=600029]canadian pharmacy ratings[/url] reddit canadian pharmacy
pharmacies in mexico that ship to usa mexican pharmaceuticals online or mexico drug stores pharmacies
http://www.idunionlaw.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company mexican rx online
[url=http://understandingmenthol.org/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company]pharmacies in mexico that ship to usa[/url] mexican border pharmacies shipping to usa and [url=http://www.1nanspa.com/space-uid-14535.html]medicine in mexico pharmacies[/url] п»їbest mexican online pharmacies
https://indiapharmacy.pro/# best india pharmacy indiapharmacy.pro
canadian pharmacy 1 internet online drugstore: my canadian pharmacy reviews – canadapharmacyonline legit canadapharmacy.guru
best online pharmacies in mexico: purple pharmacy mexico price list – mexican border pharmacies shipping to usa mexicanpharmacy.company
medication from mexico pharmacy: pharmacies in mexico that ship to usa – pharmacies in mexico that ship to usa mexicanpharmacy.company
canadian medications [url=https://canadapharmacy.guru/#]canadian pharmacy in canada[/url] the canadian pharmacy canadapharmacy.guru
top 10 online pharmacy in india top 10 online pharmacy in india or best online pharmacy india
http://www.abalonelounge.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro indian pharmacy online
[url=http://slightly-bigger.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]top 10 pharmacies in india[/url] п»їlegitimate online pharmacies india and [url=http://cos258.com/home.php?mod=space&uid=986385]canadian pharmacy india[/url] india online pharmacy
http://canadapharmacy.guru/# pharmacy com canada canadapharmacy.guru
canadian medications canadian pharmacy world or buying drugs from canada
http://kidsorganized.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru canadian pharmacy 365
[url=http://thewallstreetgame.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]buy prescription drugs from canada cheap[/url] is canadian pharmacy legit and [url=https://quantrinet.com/forum/member.php?u=534156]the canadian pharmacy[/url] my canadian pharmacy review
pharmacies in mexico that ship to usa: mexico drug stores pharmacies – mexican drugstore online mexicanpharmacy.company
reputable indian pharmacies [url=http://indiapharmacy.pro/#]indian pharmacies safe[/url] top 10 pharmacies in india indiapharmacy.pro
canadian medications: safe reliable canadian pharmacy – canada discount pharmacy canadapharmacy.guru
http://mexicanpharmacy.company/# mexico pharmacies prescription drugs mexicanpharmacy.company
mexican online pharmacies prescription drugs reputable mexican pharmacies online or pharmacies in mexico that ship to usa
http://www.puzzlecreator.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company mexican pharmaceuticals online
[url=http://gardner-kansas.us/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company]mexican pharmaceuticals online[/url] purple pharmacy mexico price list and [url=http://theglobalfederation.org/profile.php?id=2079263]mexican pharmaceuticals online[/url] best online pharmacies in mexico
https://mexicanpharmacy.company/# medication from mexico pharmacy mexicanpharmacy.company
reputable mexican pharmacies online: mexican pharmacy – mexican drugstore online mexicanpharmacy.company
ordering drugs from canada canadian pharmacies that deliver to the us or canadian drug
http://fisher-investments.eu/__media__/js/netsoltrademark.php?d=canadapharmacy.guru canadian drugs pharmacy
[url=http://locolarry.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]best canadian pharmacy[/url] buy drugs from canada and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=697840]certified canadian pharmacy[/url] canadian pharmacy online
medication from mexico pharmacy: purple pharmacy mexico price list – mexico drug stores pharmacies mexicanpharmacy.company
canadian pharmacy ratings [url=https://canadapharmacy.guru/#]online canadian pharmacy[/url] canadian pharmacy reviews canadapharmacy.guru
prescription drugs canada buy online: canada drugs online review – canada pharmacy canadapharmacy.guru
buy prescription drugs from india buy prescription drugs from india or indian pharmacies safe
http://iheartlawyers.net/__media__/js/netsoltrademark.php?d=indiapharmacy.pro online pharmacy india
[url=http://peiweiasianmarket.net/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]indian pharmacy online[/url] buy medicines online in india and [url=http://www.wjyjh.cn/home.php?mod=space&uid=10312]india pharmacy mail order[/url] best india pharmacy
https://mexicanpharmacy.company/# medicine in mexico pharmacies mexicanpharmacy.company
online pharmacy india: cheapest online pharmacy india – indian pharmacy paypal indiapharmacy.pro
canadian mail order pharmacy [url=https://canadapharmacy.guru/#]drugs from canada[/url] canada drugs canadapharmacy.guru
pharmacy com canada cheap canadian pharmacy online or canadian pharmacies comparison
http://directbuyvacationrewards.net/__media__/js/netsoltrademark.php?d=canadapharmacy.guru canadian pharmacy 24h com safe
[url=http://www.chicagoboardoptionsexchange.net/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]the canadian drugstore[/url] canadianpharmacy com and [url=https://www.ixbren.net/home.php?mod=space&uid=641110]canadapharmacyonline legit[/url] pharmacy rx world canada
https://mexicanpharmacy.company/# mexican drugstore online mexicanpharmacy.company
mexican pharmaceuticals online: mexican mail order pharmacies – mexico pharmacies prescription drugs mexicanpharmacy.company
buy medicines online in india: indianpharmacy com – top 10 online pharmacy in india indiapharmacy.pro
medicine in mexico pharmacies purple pharmacy mexico price list or mexican mail order pharmacies
http://wvxe.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company mexican rx online
[url=http://palomavalleyrealestate.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company]pharmacies in mexico that ship to usa[/url] buying prescription drugs in mexico and [url=http://qihuo.org.cn/space-uid-265050.html]pharmacies in mexico that ship to usa[/url] mexican mail order pharmacies
https://canadapharmacy.guru/# safe canadian pharmacies canadapharmacy.guru
mexican border pharmacies shipping to usa: mexican rx online – medicine in mexico pharmacies mexicanpharmacy.company
purple pharmacy mexico price list [url=http://mexicanpharmacy.company/#]medication from mexico pharmacy[/url] mexican border pharmacies shipping to usa mexicanpharmacy.company
mail order pharmacy india india pharmacy mail order or pharmacy website india
http://felicite.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro reputable indian pharmacies
[url=http://yourbraindoctor.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]india online pharmacy[/url] indian pharmacy paypal and [url=http://bot888.cn/home.php?mod=space&uid=53361]top online pharmacy india[/url] buy prescription drugs from india
canada drugs online reviews canadian pharmacy store or legitimate canadian pharmacy
http://celsion.tw/__media__/js/netsoltrademark.php?d=canadapharmacy.guru> best rated canadian pharmacy
[url=http://tectcomposites.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]my canadian pharmacy[/url] buy prescription drugs from canada cheap and [url=http://www.1nanspa.com/space-uid-14658.html]canadianpharmacy com[/url] canadian pharmacy prices
online pharmacy india: indianpharmacy com – top 10 pharmacies in india indiapharmacy.pro
http://indiapharmacy.pro/# buy medicines online in india indiapharmacy.pro
best online pharmacies in mexico: mexico pharmacies prescription drugs – п»їbest mexican online pharmacies mexicanpharmacy.company
canadian pharmacy: reliable canadian pharmacy – legitimate canadian online pharmacies canadapharmacy.guru
legal canadian pharmacy online [url=http://canadapharmacy.guru/#]legit canadian pharmacy online[/url] canadian drug prices canadapharmacy.guru
http://canadapharmacy.guru/# legit canadian pharmacy canadapharmacy.guru
canadian pharmacy mall canadian drug pharmacy or online canadian pharmacy
http://breathcaresolutions.info/__media__/js/netsoltrademark.php?d=canadapharmacy.guru online canadian pharmacy reviews
[url=http://www.casemail.com/__media__/js/netsoltrademark.php?d=canadapharmacy.guru]canadian pharmacy meds[/url] canada pharmacy 24h and [url=http://web.symbol.rs/forum/member.php?action=profile&uid=371709]canadian pharmacy 24 com[/url] canadian pharmacy meds reviews
http://mexicanpharmacy.company/# buying from online mexican pharmacy mexicanpharmacy.company
online shopping pharmacy india: п»їlegitimate online pharmacies india – п»їlegitimate online pharmacies india indiapharmacy.pro
mexican border pharmacies shipping to usa mexican rx online or mexico drug stores pharmacies
http://inflateaflix.net/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company mexican online pharmacies prescription drugs
[url=http://arabicaria.com/__media__/js/netsoltrademark.php?d=mexicanpharmacy.company]mexican drugstore online[/url] п»їbest mexican online pharmacies and [url=http://www.visionzone.com.cn/home.php?mod=space&uid=2696551]mexican mail order pharmacies[/url] mexican border pharmacies shipping to usa
reputable indian pharmacies online shopping pharmacy india or top 10 online pharmacy in india
http://ontarioimprov.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro world pharmacy india
[url=http://spotoncredits.com/__media__/js/netsoltrademark.php?d=indiapharmacy.pro]top 10 online pharmacy in india[/url] indianpharmacy com and [url=http://52lhb.com.cn/home.php?mod=space&uid=53703]world pharmacy india[/url] buy medicines online in india
reputable mexican pharmacies online: buying prescription drugs in mexico – п»їbest mexican online pharmacies mexicanpharmacy.company
canadian pharmacy meds [url=https://canadapharmacy.guru/#]canadian family pharmacy[/url] canadapharmacyonline legit canadapharmacy.guru
mexican online pharmacies prescription drugs: medicine in mexico pharmacies – reputable mexican pharmacies online mexicanpharmacy.company
http://canadapharmacy.guru/# online canadian pharmacy reviews canadapharmacy.guru
pharmacy website india: top 10 online pharmacy in india – buy prescription drugs from india indiapharmacy.pro
best online pharmacies in mexico: mexican mail order pharmacies – buying prescription drugs in mexico mexicanpharmacy.company
india pharmacy [url=http://indiapharmacy.pro/#]indian pharmacy online[/url] india pharmacy indiapharmacy.pro
https://indiapharmacy.pro/# Online medicine order indiapharmacy.pro
https://clomid.sbs/# where to get generic clomid without dr prescription
can you get cheap clomid without a prescription [url=http://clomid.sbs/#]can you buy cheap clomid without insurance[/url] where to get clomid prices
propecia pills: cheap propecia pill – buying cheap propecia without rx
https://prednisone.digital/# prednisone 40 mg daily
https://amoxil.world/# amoxicillin 500mg capsule
generic propecia [url=https://propecia.sbs/#]buying cheap propecia price[/url] propecia tablets
cost propecia without insurance: cost of cheap propecia without insurance – buying generic propecia without insurance
https://propecia.sbs/# cost of cheap propecia online
https://propecia.sbs/# cost of generic propecia without insurance
propecia pills [url=http://propecia.sbs/#]cost generic propecia no prescription[/url] order generic propecia without rx
buying cheap propecia prices order generic propecia without rx or buying generic propecia pill
http://lift.uwindsor.ca/tt/propecia.sbs get cheap propecia
[url=https://cse.google.pt/url?sa=t&url=https://propecia.sbs]propecia otc[/url] buying generic propecia pill and [url=http://www.xiaolanmb.com/space-uid-19231.html]buying generic propecia without dr prescription[/url] order cheap propecia pills
https://clomid.sbs/# buy generic clomid without insurance
60 mg prednisone daily: prednisone 10mg price in india – prednisone 250 mg
http://clomid.sbs/# where can i buy cheap clomid without a prescription
where to get clomid without rx [url=http://clomid.sbs/#]cheap clomid for sale[/url] how to get cheap clomid pills
https://clomid.sbs/# where can i get generic clomid without a prescription
canadian pharmacy amoxicillin: where can i get amoxicillin 500 mg – amoxicillin 500mg capsules price
order amoxicillin no prescription: amoxicillin cost australia – can we buy amoxcillin 500mg on ebay without prescription
can i buy amoxicillin over the counter: buy amoxicillin 250mg – where to buy amoxicillin pharmacy
purchase prednisone canada prednisone 5 mg tablet cost or prednisone pack
https://images.google.com.bn/url?q=https://prednisone.digital how much is prednisone 10mg
[url=https://images.google.dz/url?q=https://prednisone.digital]prednisone 10mg tablets[/url] buy prednisone online no script and [url=http://www.chaoren.group/home.php?mod=space&uid=588272]how to purchase prednisone online[/url] buy 40 mg prednisone
buy amoxicillin 500mg capsules uk amoxicillin medicine or order amoxicillin online no prescription
https://maps.google.rw/url?q=http://amoxil.world amoxicillin 500 capsule
[url=https://cse.google.iq/url?sa=t&url=https://amoxil.world]amoxicillin without a prescription[/url] amoxicillin 50 mg tablets and [url=http://www.1nanspa.com/space-uid-14873.html]amoxicillin for sale[/url] azithromycin amoxicillin
https://propecia.sbs/# cost generic propecia tablets
antibiotic amoxicillin [url=https://amoxil.world/#]where to buy amoxicillin over the counter[/url] amoxicillin script
prednisone tablets: buy prednisone online no script – cost of prednisone 10mg tablets
http://doxycycline.sbs/# doxycycline generic
buy generic propecia without a prescription cost propecia without dr prescription or cost generic propecia without prescription
http://images.google.com.ph/url?q=https://propecia.sbs cheap propecia tablets
[url=http://maps.google.cl/url?q=http://propecia.sbs]cost of propecia tablets[/url] order cheap propecia without dr prescription and [url=https://www.warshipsfaq.ru/user/kafdzayqhs]buying propecia for sale[/url] propecia order
http://prednisone.digital/# price for 15 prednisone
amoxicillin 500mg capsules antibiotic [url=https://amoxil.world/#]amoxicillin 500mg capsules[/url] amoxicillin in india
where can you buy amoxicillin over the counter: buy amoxicillin online uk – where can you get amoxicillin
https://doxycycline.sbs/# doxycycline order online
https://prednisone.digital/# 5 prednisone in mexico
cost propecia without insurance [url=http://propecia.sbs/#]buy cheap propecia pill[/url] cost of generic propecia without dr prescription
buy amoxicillin canada amoxicillin 500mg pill or amoxicillin pills 500 mg
http://www.xhen-long.com/cms/rfd_01.cgi?id=1&mode=redirect&no=2&ref_eid=83&url=http://amoxil.world amoxicillin 500mg price
[url=https://image.google.gp/url?q=https://amoxil.world]amoxicillin 500mg capsule cost[/url] amoxicillin pills 500 mg and [url=http://m.414500.cc/home.php?mod=space&uid=2654906]amoxicillin 250 mg capsule[/url] amoxicillin 500mg no prescription
buy cheap propecia tablets buy propecia for sale or propecia tablets
https://images.google.gg/url?q=https://propecia.sbs cost of cheap propecia
[url=https://images.google.kg/url?sa=t&url=https://propecia.sbs]get propecia[/url] buying generic propecia pills and [url=http://80tt1.com/home.php?mod=space&uid=101482]cost of propecia without insurance[/url] buying generic propecia pills
http://prednisone.digital/# prednisone 10mg tabs
doxycycline online: buy doxycycline online uk – buy doxycycline
http://clomid.sbs/# how to buy generic clomid for sale
cheap prednisone online [url=http://prednisone.digital/#]order prednisone 10mg[/url] prednisone price
buy generic propecia without a prescription: buying cheap propecia without rx – buy propecia no prescription
https://doxycycline.sbs/# doxy 200
http://doxycycline.sbs/# doxycycline online
where buy clomid prices [url=http://clomid.sbs/#]can i purchase generic clomid without prescription[/url] can you get cheap clomid no prescription
amoxicillin 250 mg capsule rexall pharmacy amoxicillin 500mg or amoxicillin 775 mg
https://neopvc.com/proxy.php?link=https://amoxil.world amoxicillin 500mg capsules
[url=https://www.google.bf/url?q=https://amoxil.world]buy amoxicillin from canada[/url] buy amoxicillin and [url=https://kwik.adriensosa.fr/forums/users/vfkqejqgsk/]amoxicillin 500mg for sale uk[/url] can i buy amoxicillin over the counter
doxycycline generic: generic doxycycline – order doxycycline online
http://edpills.icu/# best over the counter ed pills
mexican border pharmacies shipping to usa [url=http://mexicopharm.shop/#]mexico pharmacies prescription drugs[/url] purple pharmacy mexico price list
https://canadapharm.top/# pharmacy canadian superstore
http://withoutprescription.guru/# non prescription erection pills
pharmacies in mexico that ship to usa: mexican border pharmacies shipping to usa – buying prescription drugs in mexico
https://indiapharm.guru/# indianpharmacy com
cheapest online pharmacy india [url=http://indiapharm.guru/#]buy medicines online in india[/url] reputable indian pharmacies
https://withoutprescription.guru/# buy prescription drugs from canada
cheap canadian pharmacy ed drugs online from canada or canadian pharmacy checker
https://www.k-to.ru/bitrix/rk.php?goto=http://canadapharm.top canadian family pharmacy
[url=https://www.google.co.vi/url?q=https://canadapharm.top]77 canadian pharmacy[/url] canadian world pharmacy and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=8926508]online canadian pharmacy[/url] recommended canadian pharmacies
reputable mexican pharmacies online: mexican drugstore online – medicine in mexico pharmacies
https://canadapharm.top/# canadadrugpharmacy com
https://indiapharm.guru/# india online pharmacy
what are ed drugs [url=http://edpills.icu/#]medications for ed[/url] the best ed pill
buy prescription drugs without doctor buy prescription drugs from india or prescription without a doctor’s prescription
http://www.fullcirclecruise.com/redirect.asp?url=withoutprescription.guru 100mg viagra without a doctor prescription
[url=https://images.google.fm/url?sa=t&url=https://withoutprescription.guru]buy prescription drugs[/url] buy prescription drugs without doctor and [url=http://www.chaoren.group/home.php?mod=space&uid=594556]ed meds online without doctor prescription[/url] prescription without a doctor’s prescription
non prescription erection pills: real viagra without a doctor prescription – viagra without a doctor prescription walmart
http://edpills.icu/# top rated ed pills
natural ed remedies non prescription erection pills or over the counter erectile dysfunction pills
https://cse.google.sm/url?q=https://edpills.icu natural remedies for ed
[url=https://alt1.toolbarqueries.google.co.uz/url?q=https://edpills.icu]ed medications[/url] cure ed and [url=http://www.ziyuangroup.com/space-uid-105787.html]ed treatments[/url] best medication for ed
mexican pharmaceuticals online mexican online pharmacies prescription drugs or reputable mexican pharmacies online
http://www.omaki.jp/blog/feed2js/feed2js.php?src=http://mexicopharm.shop mexico drug stores pharmacies
[url=http://www.aaronsw.com/2002/display.cgi?t=<a+href=http://mexicopharm.shop]mexican rx online[/url] pharmacies in mexico that ship to usa and [url=https://slovakia-forex.com/members/229545-wizhrxzcak]mexico drug stores pharmacies[/url] pharmacies in mexico that ship to usa
https://withoutprescription.guru/# prescription drugs online without doctor
pharmacies in mexico that ship to usa [url=http://mexicopharm.shop/#]mexican mail order pharmacies[/url] medicine in mexico pharmacies
non prescription ed drugs: buy prescription drugs without doctor – ed prescription drugs
best online canadian pharmacy canadian pharmacy review or canadian pharmacy world
https://images.google.com.bh/url?sa=t&url=https://canadapharm.top cheapest pharmacy canada
[url=http://maps.google.gp/url?q=https://canadapharm.top]canadianpharmacymeds com[/url] prescription drugs canada buy online and [url=http://www.wjyjh.cn/home.php?mod=space&uid=11268]precription drugs from canada[/url] canadian discount pharmacy
http://edpills.icu/# cheapest ed pills
viagra without a prescription mexican pharmacy without prescription or sildenafil without a doctor’s prescription
https://www.google.com.my/url?q=http://withoutprescription.guru viagra without a doctor prescription walmart
[url=https://cse.google.sn/url?sa=t&url=https://withoutprescription.guru]generic viagra without a doctor prescription[/url] meds online without doctor prescription and [url=http://www.0551gay.com/space-uid-43646.html]buy prescription drugs online legally[/url] non prescription ed drugs
https://mexicopharm.shop/# best online pharmacies in mexico
mexican drugstore online [url=http://mexicopharm.shop/#]п»їbest mexican online pharmacies[/url] medicine in mexico pharmacies
best ed pills: treatment of ed – cures for ed
erection pills online buying ed pills online or medications for ed
https://images.google.com.do/url?sa=t&url=https://edpills.icu ed medications list
[url=http://aa-quebec.org/AA_Quebec/Templates/asp/rediriger-c.asp?nouveauurl=https://edpills.icu/]ed medications online[/url] ed pills cheap and [url=http://theglobalfederation.org/profile.php?id=2139201]best ed pills non prescription[/url] pills erectile dysfunction
http://indiapharm.guru/# top 10 pharmacies in india
prescription drugs online viagra without doctor prescription or prescription drugs canada buy online
https://maps.google.co.ao/url?q=https://withoutprescription.guru prescription drugs without prior prescription
[url=https://images.google.ae/url?sa=t&url=https://withoutprescription.guru]discount prescription drugs[/url] how to get prescription drugs without doctor and [url=http://bbs.cheaa.com/home.php?mod=space&uid=2997920]prescription drugs without doctor approval[/url] non prescription ed pills
real viagra without a doctor prescription: discount prescription drugs – mexican pharmacy without prescription
cheap propecia pill: get generic propecia pill – cost generic propecia for sale
pharmacies in mexico that ship to usa: buying from online mexican pharmacy – mexican drugstore online
http://edpills.icu/# cheap ed pills
top online pharmacy india [url=https://indiapharm.guru/#]indian pharmacies safe[/url] best india pharmacy
https://mexicopharm.shop/# mexico pharmacies prescription drugs
best erectile dysfunction pills cheap ed drugs or cheap ed pills
http://mypage.syosetu.com/?jumplink=http://edpills.icu ed pill
[url=https://www.google.ht/url?q=https://edpills.icu]male erection pills[/url] ed medication online and [url=http://cos258.com/home.php?mod=space&uid=1005983]pills erectile dysfunction[/url] buying ed pills online
canadian mail order pharmacy canadian drug or canadian drugs pharmacy
https://images.google.com.cu/url?q=http://canadapharm.top canadian pharmacy no scripts
[url=https://www.google.nu/url?q=https://canadapharm.top]reputable canadian pharmacy[/url] safe canadian pharmacy and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=2768678]online canadian drugstore[/url] onlinepharmaciescanada com
https://mexicopharm.shop/# mexico pharmacies prescription drugs
prescription drugs without doctor approval [url=http://withoutprescription.guru/#]generic viagra without a doctor prescription[/url] buy prescription drugs from india
safe canadian pharmacy: canadian pharm top – canadian neighbor pharmacy
purple pharmacy mexico price list medicine in mexico pharmacies or п»їbest mexican online pharmacies
http://www.vwbk.de/url?q=https://mexicopharm.shop mexico drug stores pharmacies
[url=https://images.google.com.fj/url?q=https://mexicopharm.shop]purple pharmacy mexico price list[/url] best online pharmacies in mexico and [url=http://80tt1.com/home.php?mod=space&uid=102464]mexican mail order pharmacies[/url] medicine in mexico pharmacies
buy prednisone 5mg canada: prednisone brand name – prednisone 20 tablet
http://canadapharm.top/# recommended canadian pharmacies
buy prescription drugs from india: Online medicine home delivery – buy medicines online in india
http://canadapharm.top/# certified canadian pharmacy
cheap ed pills [url=https://edpills.icu/#]erection pills online[/url] buy ed pills online
https://levitra.icu/# п»їLevitra price
http://sildenafil.win/# sildenafil 100mg price
Levitra tablet price [url=https://levitra.icu/#]Levitra 10 mg buy online[/url] Buy Levitra 20mg online
treatment of ed: best drug for ed – ed medication
https://edpills.monster/# best over the counter ed pills
tadalafil 20mg price in india tadalafil 2.5 mg generic or tadalafil soft tabs
http://www.google.gy/url?q=http://tadalafil.trade cheap generic tadalafil
[url=https://images.google.com.cu/url?q=http://tadalafil.trade]buy cheap tadalafil online[/url] cialis tadalafil and [url=http://xunshang.cc/home.php?mod=space&uid=4277651]buy tadalafil india[/url] cialis tadalafil
medicine for impotence best male enhancement pills or best ed treatment pills
http://ktcom.jp/redirect.php?u=http://edpills.monster new ed pills
[url=https://images.google.mw/url?q=https://edpills.monster]ed drug prices[/url] non prescription ed pills and [url=http://bbs.xyslysy.cn/upload/home.php?mod=space&uid=12319]drugs for ed[/url] best ed pills non prescription
buy kamagra online usa Kamagra Oral Jelly or п»їkamagra
https://www.mf-shogyo.co.jp/link.php?url=https://kamagra.team sildenafil oral jelly 100mg kamagra
[url=https://clients1.google.sh/url?q=https://kamagra.team]buy kamagra online usa[/url] super kamagra and [url=http://www.wjyjh.cn/home.php?mod=space&uid=11807]sildenafil oral jelly 100mg kamagra[/url] Kamagra Oral Jelly
price of sildenafil 100mg [url=https://sildenafil.win/#]sildenafil 20 mg tablets price[/url] sildenafil over the counter south africa
buy Kamagra: buy Kamagra – sildenafil oral jelly 100mg kamagra
where can i buy over the counter sildenafil sildenafil 50 mg tablet or sildenafil 20 mg over the counter
https://maps.google.ie/url?sa=t&url=https://sildenafil.win where can i buy sildenafil 20mg
[url=https://www.google.co.vi/url?q=https://sildenafil.win]best pharmacy prices for sildenafil[/url] sildenafil 25 mg mexico and [url=http://xunshang.cc/home.php?mod=space&uid=4277685]generic viagra sildenafil[/url] sildenafil 20 mg discount coupon
http://levitra.icu/# Vardenafil online prescription
sildenafil oral jelly 100mg kamagra: buy kamagra online usa – Kamagra 100mg price
pills for erection [url=https://edpills.monster/#]best ed pills at gnc[/url] buy ed pills
http://sildenafil.win/# sildenafil 100mg buy online us
п»їkamagra: Kamagra tablets – buy kamagra online usa
https://edpills.monster/# best ed pills at gnc
buy tadalafil 20mg price canada tadalafil pills 20mg or tadalafil 10mg coupon
http://2ch.omorovie.com/redirect.php?url=http://tadalafil.trade generic cialis tadalafil
[url=https://clipperfund.com/?URL=https://tadalafil.trade::]tadalafil 100mg best price[/url] tadalafil cheapest price and [url=http://www.xiaolanmb.com/space-uid-20578.html]tadalafil 2.5 mg cost[/url] tadalafil online india
sildenafil 100mg prescription [url=https://sildenafil.win/#]price of sildenafil[/url] sildenafil india purchase
sildenafil generic otc sildenafil 25 mg price in india or sildenafil tablets 100mg buy
https://docs.whirlpool.eu/?brand=bk&locale=de&linkreg=https://sildenafil.win 100mg sildenafil for sale
[url=http://images.google.be/url?q=https://sildenafil.win]generic sildenafil 2020[/url] sildenafil 20 mg coupon and [url=http://83783.net/home.php?mod=space&uid=7746638]sildenafil for sale australia[/url] sildenafil 20 mg prescription
buy kamagra online usa Kamagra 100mg or п»їkamagra
https://shop.hahanoshizuku.jp/shop/display_cart?return_url=http://kamagra.team cheap kamagra
[url=https://images.google.gg/url?sa=t&url=https://kamagra.team]Kamagra tablets[/url] Kamagra 100mg price and [url=http://www.wjyjh.cn/home.php?mod=space&uid=11821]п»їkamagra[/url] Kamagra Oral Jelly
medications for ed compare ed drugs or pills erectile dysfunction
https://terraguitar.net/index.php?name=Info&url=edpills.monster male ed pills
[url=https://www.google.com.sl/url?sa=t&url=https://edpills.monster]impotence pills[/url] best ed medications and [url=http://bbs.94kk.net/home.php?mod=space&uid=8484910]best medication for ed[/url] best over the counter ed pills
sildenafil oral jelly 100mg kamagra: buy Kamagra – Kamagra Oral Jelly
best tadalafil prices: generic tadalafil india – best tadalafil tablets in india
Kamagra tablets [url=http://kamagra.team/#]Kamagra Oral Jelly[/url] Kamagra 100mg
https://levitra.icu/# Buy Levitra 20mg online
lisinopril online canadian pharmacy [url=https://lisinopril.auction/#]buy lisinopril online[/url] lisinopril pills
amoxil pharmacy: amoxil pharmacy – amoxicillin over counter
buy ciprofloxacin over the counter: ciprofloxacin without insurance – ciprofloxacin 500 mg tablet price
amoxicillin online canada [url=http://amoxicillin.best/#]purchase amoxicillin online[/url] buy amoxicillin online mexico
amoxicillin 500 mg brand name: buy amoxil – amoxicillin 500mg price in canada
amoxicillin 500mg capsules antibiotic amoxicillin 500mg for sale uk or medicine amoxicillin 500
https://cse.google.co.vi/url?sa=t&url=https://amoxicillin.best price of amoxicillin without insurance
[url=https://cse.google.sc/url?q=https://amoxicillin.best]amoxicillin 500mg capsules uk[/url] cost of amoxicillin prescription and [url=https://tc.yuedotech.com/home.php?mod=space&uid=310976]where can i buy amoxicillin online[/url] can i buy amoxicillin over the counter in australia
http://amoxicillin.best/# buy amoxicillin online mexico
doxycycline 100g tablets how to get doxycycline cheap or doxycycline over the counter uk
http://forums.spacewars.com/proxy.php?link=https://doxycycline.forum buy doxycycline 100mg online
[url=http://clients1.google.nu/url?q=https://doxycycline.forum]doxycycline 50mg tablets price[/url] best price for prescription doxycycline and [url=http://www.mmecaw.com/home.php?mod=space&uid=462580]doxycycline 7.5 mg[/url] buy doxycycline tablets 100mg
п»їcipro generic cipro online no prescription in the usa or ciprofloxacin mail online
http://chimesinternational.com/artists/sixties_gold/link.php?link=http://ciprofloxacin.men antibiotics cipro
[url=https://maps.google.com.sb/url?q=https://ciprofloxacin.men]ciprofloxacin order online[/url] buy cipro online without prescription and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=712338]buy ciprofloxacin over the counter[/url] buy cipro cheap
where can i buy zithromax capsules [url=https://azithromycin.bar/#]buy zithromax canada[/url] zithromax buy
zithromax cost: buy zithromax canada – buy zithromax online
zithromax 250 mg tablet price generic zithromax azithromycin or zithromax online no prescription
https://www.imp.mx/salto.php?va=http://azithromycin.bar zithromax online usa no prescription
[url=http://media.lannipietro.com/album.aspx?album=namibia2011&return=https://azithromycin.bar]zithromax 250 price[/url] buy zithromax without presc and [url=http://www.chaoren.group/home.php?mod=space&uid=602643]buy zithromax no prescription[/url] zithromax purchase online
zithromax pill: zithromax z-pak – can you buy zithromax over the counter in canada
http://doxycycline.forum/# where to get doxycycline
doxycycline over the counter [url=http://doxycycline.forum/#]Buy Doxycycline for acne[/url] buy doxycycline 100mg cheap
buy amoxicillin 500mg canada: amoxil for sale – amoxicillin 500 tablet
can i buy amoxicillin over the counter buy amoxicillin 500mg canada or amoxicillin 500 mg
https://images.google.ch/url?sa=t&url=https://amoxicillin.best amoxicillin 750 mg price
[url=https://maps.google.si/url?q=http://amoxicillin.best]where can i buy amoxicillin without prec[/url] amoxicillin without prescription and [url=http://www.chaoren.group/home.php?mod=space&uid=602075]amoxicillin 800 mg price[/url] can i purchase amoxicillin online
http://amoxicillin.best/# buy amoxil
zithromax online usa no prescription: where to get zithromax – buy zithromax 500mg online
zithromax without prescription where can you buy zithromax or zithromax 250
https://community.rsa.com/external-link.jspa?url=http://azithromycin.bar zithromax buy
[url=http://chinaboy.psend.com/?a%5B%5D=%3Ca%20href%3Dhttp%3A%2F%2Fazithromycin.bar%2F%3E%C3%90%C2%BF%C3%91%E2%82%AC%C3%90%C2%BE%C3%90%C2%B2%C3%90%C2%B5%C3%91%E2%82%AC%C3%90%C2%BA%C3%90%C2%B0%20%C3%91%C5%8D%C3%90%C2%BB%C3%90%C2%B5%C3%90%C2%BA%C3%91%E2%80%9A%C3%91%E2%82%AC%C3%90%C2%BE%C3%91%81%C3%90%C2%BD%C3%90%C2%B0%C3%90%C2%B1%C3%90%C2%B6%C3%90%C2%B5%C3%90%C2%BD%C3%90%C2%B8%C3%91%8F%3C%2Fa%3E]zithromax prescription online[/url] zithromax 500 and [url=http://www.mmecaw.com/home.php?mod=space&uid=462393]zithromax drug[/url] zithromax cost australia
ciprofloxacin generic price ciprofloxacin mail online or buy cipro online without prescription
https://www.google.com.ar/url?q=https://ciprofloxacin.men ciprofloxacin generic price
[url=https://www.google.com.kw/url?sa=t&url=https://ciprofloxacin.men]cipro 500mg best prices[/url] purchase cipro and [url=http://chunboshi.cn/home.php?mod=space&uid=1683646]cipro online no prescription in the usa[/url] ciprofloxacin 500 mg tablet price
doxycycline 50 mg cap doxycycline 100mg cap or buying doxycycline online
http://www.leftkick.com/cgi-bin/starbucks/rsp.cgi?url=https://doxycycline.forum doxycycline 20 mg coupon
[url=http://renewable.jp/index.php?a=free_page/goto_mobile&referer=https://doxycycline.forum]vibramycin 100mg[/url] doxycycline without a prescription and [url=http://www.chaoren.group/home.php?mod=space&uid=603049]doxycycline 100mg pills[/url] doxycycline 200 mg cost
lisinopril uk [url=http://lisinopril.auction/#]Buy Lisinopril 20 mg online[/url] lisinopril 10 mg tablet
doxycycline 100 mg cap over the counter: doxycycline hyc 100 mg – doxycycline 50mg tablets
Скоростроительные здания: прибыль для бизнеса в каждой части!
В современном обществе, где время равно деньгам, быстровозводимые здания стали решением по сути для коммерческой деятельности. Эти современные конструкции комбинируют в себе солидную надежность, экономичное использование ресурсов и скорость монтажа, что делает их отличным выбором для различных бизнес-проектов.
[url=https://bystrovozvodimye-zdanija-moskva.ru/]Быстровозводимые здания из металлоконструкций стоимость[/url]
1. Ускоренная установка: Секунды – самое ценное в предпринимательстве, и быстровозводимые здания позволяют существенно сократить время монтажа. Это высоко оценивается в ситуациях, когда важно быстро начать вести бизнес и начать монетизацию.
2. Экономия средств: За счет совершенствования производственных процессов элементов и сборки на площадке, экономические затраты на моментальные строения часто бывает ниже, чем у традиционных строительных проектов. Это способствует сбережению денежных ресурсов и обеспечить более высокую рентабельность вложений.
Подробнее на [url=https://bystrovozvodimye-zdanija-moskva.ru/]https://scholding.ru/[/url]
В заключение, быстровозводимые здания – это великолепное решение для коммерческих инициатив. Они комбинируют в себе быстроту возведения, экономию средств и надежные характеристики, что делает их лучшим выбором для деловых лиц, готовых начать прибыльное дело и извлекать прибыль. Не упустите шанс экономии времени и денег, прекрасно себя показавшие быстровозводимые сооружения для вашего следующего делового мероприятия!
http://doxycycline.forum/# buy doxycycline in india
can you buy zithromax online [url=http://azithromycin.bar/#]zithromax antibiotic[/url] buy generic zithromax no prescription
zithromax 500: buy cheap generic zithromax – how to get zithromax
http://lisinopril.auction/# how much is lisinopril 40 mg
doxycycline medicine: Buy doxycycline for chlamydia – doxycycline uk cost
amoxicillin in india amoxicillin 500 mg or amoxicillin 500mg price in canada
https://www.findmydepartment56.com/current/Department_56_Dickens_Village/Department_56_Dickens_Village_Dickens_Village_Church-sub-2.php?From=https://amoxicillin.best price for amoxicillin 875 mg
[url=https://maps.google.ne/url?q=https://amoxicillin.best]amoxicillin over the counter in canada[/url] order amoxicillin 500mg and [url=http://www.fxwenxue.com/home.php?mod=space&uid=675497]where can i buy amoxicillin over the counter[/url] amoxicillin pharmacy price
pharmacies in mexico that ship to usa: best online pharmacy – buying from online mexican pharmacy
cheapest online pharmacy india: top 10 pharmacies in india – reputable indian pharmacies
http://indiapharmacy.site/# indian pharmacy
list of canadian online pharmacies mail order pharmacy or canadian drug store
http://phpooey.com/?URL=ordermedicationonline.pro accutane mexican pharmacy
[url=https://maps.google.pt/url?q=https://ordermedicationonline.pro]no prescription online pharmacy[/url] canadapharmacyonline.com and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3007064]cheap prescriptions[/url] online pharmacy reviews
buying prescription drugs in mexico online п»їbest mexican online pharmacies or mexico drug stores pharmacies
http://www.bssystems.org/url?q=https://mexicopharmacy.store mexico pharmacy
[url=http://www.postern.se/url?go=https://mexicopharmacy.store]mexican rx online[/url] mexican pharmacy and [url=http://80tt1.com/home.php?mod=space&uid=106079]mexico drug stores pharmacies[/url] purple pharmacy mexico price list
the canadian pharmacy: trust canadian pharmacy – canadian online pharmacy
indian pharmacy online best online pharmacy india or Online medicine home delivery
https://images.google.com.kh/url?q=https://indiapharmacy.site online pharmacy india
[url=https://clients1.google.co.mz/url?q=https://indiapharmacy.site]Online medicine home delivery[/url] best online pharmacy india and [url=http://www.xiaolanmb.com/space-uid-22382.html]reputable indian pharmacies[/url] india online pharmacy
no prescription pharmacies medicine canada or online pharmacies no prescriptions
https://canada-place.co.jp/index.php?a=free_page/goto_mobile&referer=https://buydrugsonline.top canadian pharmacies online
[url=https://www.neuoetting.de/externer_link.php?url_uebergabe=buydrugsonline.top]online prescription[/url] no perscription drugs canada and [url=http://www.9kuan9.com/home.php?mod=space&uid=160508]discount pharmacy coupons[/url] top rated canadian pharmacies
canadian pharmacy meds: safe online pharmacy – canadian pharmacy near me
https://canadiandrugs.store/# the canadian drugstore
Быстро возводимые здания: экономический доход в каждом строительном блоке!
В современной реальности, где время имеет значение, скоростройки стали решением, спасающим для предпринимательства. Эти современные сооружения включают в себя устойчивость, экономичное использование ресурсов и быстрый монтаж, что сделало их идеальным выбором для бизнес-проектов разных масштабов.
[url=https://bystrovozvodimye-zdanija-moskva.ru/]Быстровозводимые здания под ключ[/url]
1. Быстрота монтажа: Секунды – самое ценное в финансовой сфере, и быстровозводимые здания обеспечивают значительное снижение времени строительства. Это значительно ценится в вариантах, когда срочно нужно начать бизнес и начать получать прибыль.
2. Финансовая выгода: За счет совершенствования производственных процессов элементов и сборки на площадке, финансовые издержки на быстровозводимые объекты часто бывает ниже, по сравнению с традиционными строительными проектами. Это позволяет сократить затраты и обеспечить более высокую рентабельность вложений.
Подробнее на [url=https://bystrovozvodimye-zdanija-moskva.ru/]http://www.scholding.ru[/url]
В заключение, быстровозводимые здания – это великолепное решение для предпринимательских задач. Они объединяют в себе быстроту возведения, эффективное использование ресурсов и надежность, что позволяет им оптимальным решением для деловых лиц, ориентированных на оперативный бизнес-старт и обеспечивать доход. Не упустите момент экономии времени и средств, идеальные сооружения быстрого монтажа для ваших будущих проектов!
canadian discount pharmacy: Online pharmacy USA – internet pharmacy no prior prescription
indian pharmacy [url=http://indiapharmacy.site/#]india pharmacy mail order[/url] indian pharmacy
legitimate canadian mail order pharmacy: trust canadian pharmacy – canada rx pharmacy world
https://indiapharmacy.site/# buy medicines online in india
buy ventolin over the counter with paypal: Ventolin HFA Inhaler – can you buy ventolin over the counter in uk
https://wellbutrin.rest/# wellbutrin xl generic
http://paxlovid.club/# paxlovid india
generic neurontin 600 mg [url=https://gabapentin.life/#]generic gabapentin[/url] gabapentin 100mg
https://wellbutrin.rest/# wellbutrin without a prescription
wellbutrin sr: Buy bupropion online Europe – where can i buy wellbutrin online
paxlovid covid: paxlovid club – paxlovid price
https://clomid.club/# clomid medication
https://wellbutrin.rest/# wellbutrin zyban
paxlovid cost without insurance: Paxlovid buy online – paxlovid cost without insurance
Paxlovid buy online paxlovid covid or Paxlovid buy online
http://7ba.info/out.php?url=https://paxlovid.club paxlovid generic
[url=https://www.buscocolegio.com/Colegio/redireccionar-web.action?url=https://paxlovid.club]Paxlovid buy online[/url] paxlovid generic and [url=http://users.atw.hu/dangercheat/forum/member.php?action=profile&uid=1770]paxlovid generic[/url] paxlovid covid
can i purchase clomid without rx where to get cheap clomid or where can i buy cheap clomid no prescription
https://www.google.co.th/url?q=https://clomid.club clomid pill
[url=http://urlxray.com/display.php?url=https://clomid.club/]can i buy clomid no prescription[/url] can i order generic clomid tablets and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=101458]can i buy cheap clomid online[/url] can i purchase clomid price
can you get cheap clomid no prescription: clomid best price – where can i buy clomid
http://wellbutrin.rest/# buy wellbutrin
neurontin 204 neurontin 100mg tablets or neurontin 800mg
https://maps.google.com.py/url?sa=i&url=https://gabapentin.life neurontin prices generic
[url=https://www.valldenuria.cat/content/comun/ajax_get_news.php?ruta=/&bk=&idioma=ca&season=1&mostviews=3&rss=http://gabapentin.life]canada where to buy neurontin[/url] neurontin brand name in india and [url=http://plixsite.net/forum/member.php?action=profile&uid=2481501]neurontin 100mg[/url] neurontin cap
ventolin 50 mcg ventolin albuterol inhaler or can you buy ventolin over the counter in canada
https://www.google.gm/url?q=https://claritin.icu ventolin
[url=https://image.google.gm/url?q=j&sa=t&url=https://claritin.icu]can you buy ventolin over the counter australia[/url] ventolin cost uk and [url=http://plixsite.net/forum/member.php?action=profile&uid=2480993]ventolin 4 mg tablets[/url] ventolin prescription
http://claritin.icu/# where to buy ventolin nz
Paxlovid over the counter: cheap paxlovid online – paxlovid pharmacy
Paxlovid over the counter https://paxlovid.club/# paxlovid buy
clomid pill: Buy Clomid Online Without Prescription – can you buy clomid without a prescription
http://clomid.club/# can you get generic clomid pills
https://paxlovid.club/# buy paxlovid online
wellbutrin 150 mg: Buy Wellbutrin XL online – how to get brand name wellbutrin cheap
where to buy generic clomid without dr prescription: clomid best price – how can i get cheap clomid without a prescription
http://clomid.club/# where can i get generic clomid without a prescription
where to buy clomid prices [url=http://clomid.club/#]Buy Clomid Shipped From Canada[/url] how can i get clomid online
how to get generic clomid price can i buy clomid without rx or can i order clomid pill
https://maps.google.gm/url?q=https://clomid.club can i get generic clomid without rx
[url=http://toolbarqueries.google.com.pk/url?sa=i&url=https://clomid.club]can i order generic clomid tablets[/url] where can i buy generic clomid now and [url=https://lhgangguanwang.com/home.php?mod=space&uid=23387]order cheap clomid without rx[/url] can i get cheap clomid without prescription
п»їpaxlovid paxlovid price or paxlovid price
https://profil.uniag.sk/pracoviste/predmety.pl?id=56;zpet=https://paxlovid.club Paxlovid buy online
[url=https://www.google.com.ph/url?q=https://paxlovid.club]п»їpaxlovid[/url] paxlovid price and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6322461]Paxlovid over the counter[/url] Paxlovid over the counter
can you buy cheap clomid pill: clomid best price – can i get generic clomid
http://clomid.club/# can i purchase generic clomid
can i buy cheap clomid online [url=https://clomid.club/#]Buy Clomid Shipped From Canada[/url] buying generic clomid without prescription
can i order generic clomid online: Clomiphene Citrate 50 Mg – where to get clomid without rx
https://clomid.club/# can you get clomid now
how to buy clomid [url=https://clomid.club/#]Buy Clomid Online[/url] where buy generic clomid online
cost of generic clomid no prescription: Clomiphene Citrate 50 Mg – cost of generic clomid
https://clomid.club/# can you buy generic clomid tablets
how to buy cheap clomid without prescription [url=https://clomid.club/#]Clomiphene Citrate 50 Mg[/url] buying generic clomid no prescription
can i order cheap clomid tablets: where can i get generic clomid without a prescription – can you get cheap clomid
http://paxlovid.club/# paxlovid india
ventolin otc nz ventolin from india or how to get ventolin over the counter
https://images.google.gg/url?q=https://claritin.icu ventolin otc canada
[url=https://www.google.tk/url?sa=t&url=https://claritin.icu]ventolin order[/url] ventolin over the counter nz and [url=http://www.mmecaw.com/home.php?mod=space&uid=466695]ventolin order online without prescription[/url] buy ventolin online europe
https://paxlovid.club/# Paxlovid over the counter
where buy generic clomid tablets: Buy Clomid Online Without Prescription – buying cheap clomid without dr prescription
http://clomid.club/# can i purchase generic clomid without prescription
where buy clomid without a prescription [url=https://clomid.club/#]Buy Clomid Online[/url] cost generic clomid without a prescription
where to buy neurontin purchase neurontin canada or neurontin cap 300mg
https://www.google.com.mx/url?q=https://gabapentin.life generic neurontin 600 mg
[url=https://www.thegioiseo.com/proxy.php?link=https://gabapentin.life]neurontin drug[/url] how to get neurontin and [url=http://talk.dofun.cc/home.php?mod=space&uid=13011]neurontin 100 mg tablets[/url] neurontin 800 mg cost
can i buy generic clomid no prescription: clomid best price – can i purchase clomid price
https://clomid.club/# buying cheap clomid
can you buy generic clomid without prescription [url=https://clomid.club/#]Clomiphene Citrate 50 Mg[/url] how to get cheap clomid tablets
can you buy cheap clomid for sale: clomid best price – can i buy cheap clomid no prescription
http://clomid.club/# cheap clomid without a prescription
where buy clomid for sale [url=http://clomid.club/#]clomid best price[/url] order generic clomid prices
can i purchase clomid without rx: clomid best price – order cheap clomid without a prescription
http://clomid.club/# where can i buy clomid prices
where can i buy clomid without insurance [url=https://clomid.club/#]order cheap clomid no prescription[/url] how to get generic clomid
get clomid now: Buy Clomid Online Without Prescription – how to get cheap clomid tablets
http://clomid.club/# how can i get clomid no prescription
can i order clomid without prescription [url=https://clomid.club/#]Clomiphene Citrate 50 Mg[/url] can you get generic clomid
http://claritin.icu/# generic ventolin price
cost of generic clomid: Clomiphene Citrate 50 Mg – cost of generic clomid tablets
http://clomid.club/# cost of clomid no prescription
where to buy cheap clomid prices [url=https://clomid.club/#]Buy Clomid Online Without Prescription[/url] where buy clomid online
neurontin online usa: generic gabapentin – cost of brand name neurontin
https://wellbutrin.rest/# wellbutrin brand price
cost of clomid without insurance cost of clomid pills or where buy clomid without insurance
https://www.google.com.lb/url?q=https://clomid.club can i purchase cheap clomid
[url=https://image.google.co.zw/url?q=https://clomid.club]buying generic clomid[/url] cost of clomid no prescription and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3008983]cost of clomid online[/url] can i buy generic clomid no prescription
paxlovid cost without insurance paxlovid price or paxlovid covid
https://images.google.com.nf/url?sa=t&url=https://paxlovid.club paxlovid india
[url=https://cse.google.sh/url?sa=i&url=https://paxlovid.club]paxlovid cost without insurance[/url] paxlovid buy and [url=https://quantrinet.com/forum/member.php?u=550481]buy paxlovid online[/url] buy paxlovid online
where can i buy generic clomid without a prescription: can i buy cheap clomid without prescription – can you get generic clomid without insurance
http://clomid.club/# generic clomid tablets
how to buy generic clomid without rx [url=http://clomid.club/#]can i order clomid pills[/url] can i purchase cheap clomid prices
canada to usa ventolin: Ventolin inhaler online – ventolin hfa price
cost cheap clomid now: Buy Clomid Shipped From Canada – get generic clomid without dr prescription
https://clomid.club/# where can i get clomid
where to get clomid price [url=https://clomid.club/#]Buy Clomid Online[/url] how to buy generic clomid online
how to buy generic clomid no prescription: Buy Clomid Online Without Prescription – how to buy clomid without prescription
https://clomid.club/# can you buy generic clomid without prescription
how to buy cheap clomid tablets [url=https://clomid.club/#]Buy Clomid Online[/url] where buy cheap clomid without rx
http://claritin.icu/# ventolin free shipping
where to buy cheap clomid without dr prescription: clomid best price – where to buy clomid pill
http://clomid.club/# cost of cheap clomid pills
can you buy generic clomid without insurance [url=https://clomid.club/#]Clomiphene Citrate 50 Mg[/url] where to get clomid without dr prescription
farmacia online: kamagra gold – farmacia online miglior prezzo
acquisto farmaci con ricetta: avanafil – farmaci senza ricetta elenco
farmacie online autorizzate elenco: farmacia online miglior prezzo – acquisto farmaci con ricetta
farmacie on line spedizione gratuita [url=https://avanafilit.icu/#]avanafil prezzo in farmacia[/url] farmacia online senza ricetta
http://sildenafilit.bid/# viagra 100 mg prezzo in farmacia
viagra generico sandoz: viagra consegna in 24 ore pagamento alla consegna – viagra online spedizione gratuita
farmacie online autorizzate elenco: avanafil – farmacia online migliore
farmacie online affidabili: Dove acquistare Cialis online sicuro – farmacie online affidabili
acquistare farmaci senza ricetta: dove acquistare cialis online sicuro – farmacie on line spedizione gratuita
migliori farmacie online 2023 [url=https://tadalafilit.store/#]Farmacie a milano che vendono cialis senza ricetta[/url] acquisto farmaci con ricetta
acquisto farmaci con ricetta: farmacia online più conveniente – farmacia online
farmacia online senza ricetta farmaci senza ricetta elenco or farmacie online sicure
https://images.google.com.vc/url?q=https://tadalafilit.store п»їfarmacia online migliore
[url=http://www.hannobunz.de/url?q=https://tadalafilit.store]farmacie online affidabili[/url] farmacia online and [url=http://plixsite.net/forum/member.php?action=profile&uid=2483034]п»їfarmacia online migliore[/url] comprare farmaci online con ricetta
farmacia senza ricetta recensioni: viagra prezzo farmacia – cialis farmacia senza ricetta
cialis farmacia senza ricetta viagra online in 2 giorni or viagra generico sandoz
https://hokejbenatky.cz/media_show.asp?type=1&id=205&url_back=https://sildenafilit.bid miglior sito per comprare viagra online
[url=https://maps.google.ad/url?q=https://sildenafilit.bid]miglior sito dove acquistare viagra[/url] viagra 100 mg prezzo in farmacia and [url=http://83783.net/home.php?mod=space&uid=7866098]pillole per erezioni fortissime[/url] alternativa al viagra senza ricetta in farmacia
https://kamagrait.club/# farmacia online miglior prezzo
comprare farmaci online all’estero: farmacia online spedizione gratuita – farmaci senza ricetta elenco
migliori farmacie online 2023: farmaci senza ricetta elenco – п»їfarmacia online migliore
top farmacia online: avanafil – farmacie online affidabili
comprare farmaci online con ricetta acquisto farmaci con ricetta or comprare farmaci online con ricetta
https://image.google.com.sb/url?q=https://farmaciait.pro farmacia online senza ricetta
[url=https://www.google.bt/url?sa=t&url=https://farmaciait.pro]farmacia online senza ricetta[/url] acquisto farmaci con ricetta and [url=http://mail.empyrethegame.com/forum/memberlist.php?mode=viewprofile&u=273405]farmacia online[/url] farmacia online migliore
migliori farmacie online 2023: kamagra oral jelly – migliori farmacie online 2023
acquistare farmaci senza ricetta: farmacia online più conveniente – farmacia online senza ricetta
http://sildenafilit.bid/# alternativa al viagra senza ricetta in farmacia
acquisto farmaci con ricetta: avanafil generico – farmaci senza ricetta elenco
farmacie online affidabili: kamagra oral jelly consegna 24 ore – farmacia online migliore
farmacie online sicure: kamagra gel – comprare farmaci online all’estero
acquisto farmaci con ricetta: avanafil prezzo – farmacia online miglior prezzo
comprare farmaci online all’estero [url=https://tadalafilit.store/#]dove acquistare cialis online sicuro[/url] acquisto farmaci con ricetta
comprare farmaci online all’estero top farmacia online or comprare farmaci online con ricetta
http://www.barwitzki.net/mecstats/index.php?page=reffer_detail&dom=tadalafilit.store comprare farmaci online all’estero
[url=https://www.google.com.ai/url?q=https://tadalafilit.store]comprare farmaci online all’estero[/url] farmaci senza ricetta elenco and [url=http://chunboshi.cn/home.php?mod=space&uid=1688676]farmaci senza ricetta elenco[/url] migliori farmacie online 2023
comprare farmaci online con ricetta: Tadalafil prezzo – acquistare farmaci senza ricetta
farmacie online autorizzate elenco: Cialis senza ricetta – farmacia online senza ricetta
https://tadalafilit.store/# farmacia online piГ№ conveniente
pillole per erezione immediata viagra consegna in 24 ore pagamento alla consegna or viagra prezzo farmacia 2023
https://www.google.dm/url?sa=t&url=https://sildenafilit.bid pillole per erezione immediata
[url=https://weburg.net/redirect?fromru=1&url=sildenafilit.bid/]cialis farmacia senza ricetta[/url] viagra ordine telefonico and [url=http://www.9kuan9.com/home.php?mod=space&uid=163333]alternativa al viagra senza ricetta in farmacia[/url] alternativa al viagra senza ricetta in farmacia
farmacie online autorizzate elenco: farmacia online – farmacia online senza ricetta
farmacia online miglior prezzo: avanafil generico – acquistare farmaci senza ricetta
farmaci senza ricetta elenco farmacie on line spedizione gratuita or farmacie online affidabili
https://redirect.camfrog.com/redirect/?url=https://kamagrait.club farmacia online senza ricetta
[url=https://cse.google.ge/url?sa=t&url=https://kamagrait.club]farmacia online[/url] farmacia online senza ricetta and [url=http://bbs.94kk.net/home.php?mod=space&uid=8650461]farmacia online miglior prezzo[/url] comprare farmaci online all’estero
viagra 50 mg prezzo in farmacia: farmacia senza ricetta recensioni – viagra cosa serve
farmacie online autorizzate elenco: comprare avanafil senza ricetta – farmacie online affidabili
viagra originale in 24 ore contrassegno [url=https://sildenafilit.bid/#]viagra generico[/url] miglior sito dove acquistare viagra
farmacia online migliore farmacie on line spedizione gratuita or farmacie online autorizzate elenco
https://images.google.sn/url?sa=t&url=https://farmaciait.pro farmacie online autorizzate elenco
[url=https://www.google.com.cy/url?q=https://farmaciait.pro]farmacie online sicure[/url] farmacia online miglior prezzo and [url=https://visualchemy.gallery/forum/profile.php?id=3372772]farmaci senza ricetta elenco[/url] farmacia online
farmacia online più conveniente: avanafil – farmacia online più conveniente
viagra generico recensioni: viagra senza ricetta – viagra cosa serve
farmaci senza ricetta elenco: avanafil prezzo in farmacia – farmacie online autorizzate elenco
http://sildenafilit.bid/# п»їviagra prezzo farmacia 2023
farmacia senza ricetta recensioni: viagra generico – viagra online spedizione gratuita
farmacia online miglior prezzo top farmacia online or acquisto farmaci con ricetta
https://cse.google.com.bo/url?sa=t&url=https://tadalafilit.store farmacia online piГ№ conveniente
[url=http://twcmail.de/deref.php?http://tadalafilit.store/%5Dacquisto farmaci con ricetta[/url] farmacie online autorizzate elenco and [url=http://cos258.com/home.php?mod=space&uid=1051153]farmacia online migliore[/url] farmacie online affidabili
п»їfarmacia online migliore [url=https://kamagrait.club/#]kamagra gold[/url] farmacie online affidabili
farmacie online sicure: kamagra gel prezzo – farmacie online autorizzate elenco
acquistare farmaci senza ricetta: cialis generico consegna 48 ore – farmacia online senza ricetta
miglior sito dove acquistare viagra: alternativa al viagra senza ricetta in farmacia – viagra ordine telefonico
siti sicuri per comprare viagra online miglior sito per comprare viagra online or viagra naturale
https://images.google.ng/url?q=https://sildenafilit.bid viagra generico prezzo piГ№ basso
[url=https://toolbarqueries.google.co.ls/url?q=http://sildenafilit.bid]pillole per erezione immediata[/url] pillole per erezioni fortissime and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=719483]le migliori pillole per l’erezione[/url] viagra originale in 24 ore contrassegno
acquistare farmaci senza ricetta: kamagra gold – farmacie online sicure
farmacia 24h [url=https://farmacia.best/#]farmacia online barata y fiable[/url] farmacia 24h
https://tadalafilo.pro/# farmacia envÃos internacionales
https://sildenafilo.store/# se puede comprar sildenafil sin receta
farmacia online envГo gratis: Precio Levitra En Farmacia – farmacia online 24 horas
https://vardenafilo.icu/# п»їfarmacia online
http://tadalafilo.pro/# farmacia online barata
https://kamagraes.site/# farmacia online barata
farmacia online 24 horas [url=http://farmacia.best/#]mejores farmacias online[/url] farmacia online 24 horas
https://sildenafilo.store/# venta de viagra a domicilio
[url=http://accutane.guru/]buy accutane online no prescription[/url]
https://vardenafilo.icu/# farmacias online seguras en españa
farmacias online baratas: Levitra Bayer – farmacias online seguras en espaГ±a
https://vardenafilo.icu/# farmacia online internacional
https://tadalafilo.pro/# farmacia 24h
http://vardenafilo.icu/# farmacia online internacional
farmacias online baratas farmacia 24h or farmacia online envГo gratis
https://www.google.bi/url?q=https://tadalafilo.pro farmacia online madrid
[url=https://www.google.ps/url?q=https://tadalafilo.pro]farmacia online internacional[/url] farmacia 24h and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9137588]farmacia online internacional[/url] farmacia envГos internacionales
farmacia online canarias farmacia online madrid or farmacia 24h
http://cse.google.com.gh/url?q=https://farmacia.best farmacia internacional madrid
[url=https://cse.google.co.kr/url?sa=i&url=http://farmacia.best]farmacia internacional madrid[/url] mejor farmacia online madrid and [url=http://plixsite.net/forum/member.php?action=profile&uid=2486468]farmacia online canarias[/url] farmacia online envГo gratis murcia
http://tadalafilo.pro/# farmacia online madrid
http://farmacia.best/# farmacias baratas online envÃo gratis
п»їfarmacia online [url=https://farmacia.best/#]farmacia online barata[/url] farmacia online internacional
sildenafilo 100mg precio farmacia sildenafilo cinfa precio or sildenafilo 50 mg precio sin receta
https://maps.google.dj/url?sa=t&url=https://sildenafilo.store sildenafilo precio farmacia
[url=https://www.google.mg/url?q=https://sildenafilo.store]sildenafilo 100mg precio espaГ±a[/url] se puede comprar viagra sin receta and [url=https://bbs.xiaoditech.com/home.php?mod=space&uid=1451828]sildenafilo cinfa 100 mg precio farmacia[/url] sildenafilo 100mg farmacia
farmacia online internacional farmacia online envГo gratis or farmacias baratas online envГo gratis
http://shckp.ru/ext_link?url=http://kamagraes.site farmacias online seguras en espaГ±a
[url=http://www.irac.pe.ca/redirect.asp?url=https://kamagraes.site]farmacia online internacional[/url] farmacias online seguras en espaГ±a and [url=http://80tt1.com/home.php?mod=space&uid=109210]farmacia barata[/url] farmacias baratas online envГo gratis
farmacias baratas online envГo gratis: se puede comprar kamagra en farmacias – farmacias online baratas
http://tadalafilo.pro/# farmacia online barata
https://kamagraes.site/# farmacia online envÃo gratis
sildenafilo 50 mg precio sin receta [url=https://sildenafilo.store/#]comprar viagra en espana[/url] sildenafilo sandoz 100 mg precio
http://tadalafilo.pro/# farmacia online barata
http://sildenafilo.store/# se puede comprar sildenafil sin receta
https://farmacia.best/# farmacia barata
farmacia internacional madrid farmacia internacional barcelona or farmacia online envГo gratis
http://www.sorenwinslow.com/RSSReader.asp?TheFeed=http://farmacia.best/ farmacia envГo gratis
[url=https://maps.google.bt/url?q=https://farmacia.best]farmacia online envГo gratis[/url] farmacias online seguras and [url=http://wuyuebanzou.com/home.php?mod=space&uid=421247]gran farmacia online[/url] farmacia online 24 horas
https://sildenafilo.store/# sildenafilo precio farmacia
farmacia online barata farmacias online baratas or farmacias online seguras
http://www.friscowebsites.com/redirect.aspx?destination=http://tadalafilo.pro farmacia online envГo gratis
[url=http://infosmi.com/redirect.php?url=http://tadalafilo.pro/]farmacia envГos internacionales[/url] farmacia online envГo gratis and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6371715]farmacias online baratas[/url] farmacias online seguras en espaГ±a
http://farmacia.best/# farmacia 24h
http://vardenafilo.icu/# farmacia online
farmacia online madrid: comprar kamagra – farmacia online barata
farmacia online barata farmacia online barata or farmacia online 24 horas
http://gallery.kroatien-ferien.com/gallery/main.php?g2_view=core.UserAdmin&g2_subView=core.UserLogin&g2_return=https://kamagraes.site farmacia online barata
[url=https://www.google.com.au/url?q=https://kamagraes.site]farmacias online baratas[/url] farmacia online barata and [url=http://talk.dofun.cc/home.php?mod=space&uid=23979]farmacia online 24 horas[/url] farmacia 24h
farmacia envГos internacionales [url=http://farmacia.best/#]gran farmacia online[/url] farmacias baratas online envГo gratis
http://sildenafilo.store/# viagra para mujeres
http://kamagraes.site/# farmacia barata
https://vardenafilo.icu/# farmacia online internacional
venta de viagra a domicilio comprar viagra en espaГ±a or viagra online cerca de zaragoza
http://www.extrasmallworld.de/forward.php?to=https://sildenafilo.store venta de viagra a domicilio
[url=https://maps.google.com.tr/url?q=https://sildenafilo.store]sildenafilo cinfa 100 mg precio farmacia[/url] viagra entrega inmediata and [url=http://lsdsng.com/user/509330]sildenafilo sandoz 100 mg precio[/url] viagra online gibraltar
https://sildenafilo.store/# viagra entrega inmediata
http://tadalafilo.pro/# farmacia online madrid
farmacias baratas online envГo gratis: farmacia online madrid – farmacia online internacional
https://tadalafilo.pro/# farmacia online 24 horas
farmacias online seguras en espaГ±a [url=http://vardenafilo.icu/#]vardenafilo[/url] farmacias baratas online envГo gratis
https://kamagraes.site/# farmacia online madrid
farmacia envГos internacionales п»їfarmacia online or farmacia online madrid
https://maps.google.lt/url?q=http://tadalafilo.pro farmacia barata
[url=https://images.google.com.au/url?q=https://tadalafilo.pro]farmacias online seguras en espaГ±a[/url] п»їfarmacia online and [url=http://chunboshi.cn/home.php?mod=space&uid=1691418]farmacia barata[/url] farmacia online barata
http://tadalafilo.pro/# farmacias online baratas
http://kamagraes.site/# farmacia online internacional
comprar sildenafilo cinfa 100 mg espaГ±a: sildenafilo precio – viagra 100 mg precio en farmacias
http://vardenafilo.icu/# farmacia online barata
п»їfarmacia online farmacias online baratas or farmacia online barata
https://clients1.google.ml/url?q=https://kamagraes.site farmacia online madrid
[url=https://cse.google.as/url?sa=t&url=https://kamagraes.site]farmacia barata[/url] farmacia online envГo gratis and [url=https://tc.yuedotech.com/home.php?mod=space&uid=322505]farmacias baratas online envГo gratis[/url] farmacia online envГo gratis
https://farmacia.best/# farmacia 24h
https://kamagraes.site/# farmacia online 24 horas
comprar viagra online en andorra [url=https://sildenafilo.store/#]viagra generico[/url] sildenafilo cinfa 25 mg precio
https://vardenafilo.icu/# farmacia online envГo gratis
http://farmacia.best/# farmacia barata
п»їfarmacia online: vardenafilo sin receta – farmacia 24h
farmacia internacional barcelona farmacia online madrid or farmacia online envГo gratis murcia
http://alt1.toolbarqueries.google.ps/url?q=https://farmacia.best farmacia online canarias
[url=https://www.google.sh/url?q=https://farmacia.best]farmacia barata[/url] farmacia envГo gratis and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=38197]farmacia online envГo gratis valencia[/url] farmacia online envГo gratis
http://sildenafilo.store/# sildenafilo cinfa precio
comprar viagra en espaГ±a envio urgente viagra online cerca de bilbao or viagra entrega inmediata
http://fox.wikis.com/wc.dll?id=В’><a+href=http://sildenafilo.store sildenafilo 100mg precio españa
[url=https://maps.google.rs/url?sa=t&url=https://sildenafilo.store]sildenafilo 100mg precio farmacia[/url] comprar viagra en espaГ±a amazon and [url=http://www.viczz.com/home.php?mod=space&uid=2919950]comprar viagra en espaГ±a envio urgente[/url] sildenafilo 100mg precio espaГ±a
https://kamagraes.site/# farmacia barata
http://vardenafilo.icu/# farmacia online
farmacia envГos internacionales farmacias online baratas or farmacia online envГo gratis
http://www.startgames.ws/myspace.php?url=http://tadalafilo.pro/ farmacia online barata
[url=https://www.google.com.pa/url?q=https://tadalafilo.pro]farmacia online madrid[/url] farmacias baratas online envГo gratis and [url=http://mail.empyrethegame.com/forum/memberlist.php?mode=viewprofile&u=274492]farmacias online baratas[/url] farmacia online envГo gratis
https://vardenafilo.icu/# farmacia online barata
http://farmacia.best/# farmacia online 24 horas
comprar viagra contrareembolso 48 horas [url=http://sildenafilo.store/#]comprar viagra contrareembolso 48 horas[/url] comprar viagra en espaГ±a amazon
farmacia online madrid: comprar cialis original – п»їfarmacia online
https://vardenafilo.icu/# farmacia 24h
http://sildenafilo.store/# viagra entrega inmediata
https://tadalafilo.pro/# farmacias online baratas
п»їfarmacia online farmacia online envГo gratis or farmacias baratas online envГo gratis
http://automaniasiouxfalls.com/LinkOut/?goto=http://kamagraes.site farmacia 24h
[url=https://www.google.gg/url?q=https://kamagraes.site]farmacia barata[/url] farmacias baratas online envГo gratis and [url=https://www.foodntours.com/user/owwwaadqws/videos]farmacia online barata[/url] farmacias online seguras
https://farmacia.best/# farmacias baratas online envÃo gratis
mejor farmacia online madrid farmacias online seguras or farmacia online madrid
http://clients1.google.com.vn/url?q=https://farmacia.best farmacia online barata
[url=https://images.google.com.ar/url?q=http://farmacia.best]п»їfarmacia online[/url] farmacia online barata and [url=https://masterbationtube.com/user/ivjyhdkiwf/videos]farmacias online baratas[/url] farmacia internacional madrid
http://sildenafilo.store/# comprar viagra sin gastos de envÃo
farmacias baratas online envГo gratis: gran farmacia online – farmacias baratas online envГo gratis
[url=https://zithromax.cyou/]zitromax[/url]
http://farmacia.best/# farmacia envГos internacionales
https://farmacia.best/# farmacia 24h
viagra para hombre precio farmacias similares [url=http://sildenafilo.store/#]comprar viagra en espana[/url] sildenafilo sandoz 100 mg precio
Pharmacie en ligne pas cher [url=https://cialissansordonnance.pro/#]Acheter Cialis 20 mg pas cher[/url] Pharmacie en ligne livraison rapide
https://kamagrafr.icu/# Pharmacie en ligne livraison gratuite
https://viagrasansordonnance.store/# Viagra vente libre pays
sildenafilo 100mg precio espaГ±a: viagra precio – viagra 100 mg precio en farmacias
Viagra 100mg prix: Acheter du Viagra sans ordonnance – Acheter Sildenafil 100mg sans ordonnance
http://kamagrafr.icu/# pharmacie ouverte
acheter medicament a l etranger sans ordonnance [url=http://levitrafr.life/#]Levitra 20mg prix en pharmacie[/url] pharmacie ouverte
https://cialissansordonnance.pro/# Pharmacies en ligne certifiées
https://cialissansordonnance.pro/# acheter médicaments à l’étranger
https://kamagrafr.icu/# Pharmacie en ligne livraison gratuite
farmacias online seguras: vardenafilo sin receta – farmacia barata
Viagra homme prix en pharmacie sans ordonnance: Viagra sans ordonnance 24h – Viagra femme sans ordonnance 24h
http://kamagrafr.icu/# acheter médicaments à l’étranger
Pharmacie en ligne livraison gratuite acheter medicament a l etranger sans ordonnance or Acheter mГ©dicaments sans ordonnance sur internet
https://clients1.google.com.eg/url?q=https://kamagrafr.icu Pharmacie en ligne pas cher
[url=https://image.google.ht/url?q=https://kamagrafr.icu]Pharmacie en ligne livraison gratuite[/url] acheter medicament a l etranger sans ordonnance and [url=https://visualchemy.gallery/forum/profile.php?id=3411742]Pharmacie en ligne fiable[/url] Pharmacie en ligne France
Pharmacie en ligne livraison 24h Acheter mГ©dicaments sans ordonnance sur internet or Pharmacie en ligne livraison gratuite
https://www.google.com.bz/url?q=https://cialissansordonnance.pro Pharmacie en ligne sans ordonnance
[url=https://www.google.je/url?sa=t&url=https://cialissansordonnance.pro]pharmacie ouverte[/url] Pharmacie en ligne livraison 24h and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1455583]п»їpharmacie en ligne[/url] Pharmacie en ligne fiable
http://pharmacieenligne.guru/# Pharmacie en ligne livraison 24h
Pharmacie en ligne fiable [url=http://kamagrafr.icu/#]kamagra oral jelly[/url] Pharmacie en ligne sans ordonnance
https://levitrafr.life/# acheter medicament a l etranger sans ordonnance
Viagra vente libre pays Prix du Viagra 100mg en France or Viagra homme prix en pharmacie
http://www.ohashi-co.com/w3a/redirect.php?redirect=http://viagrasansordonnance.store Viagra homme sans prescription
[url=https://www.google.com.ph/url?q=https://viagrasansordonnance.store]Prix du Viagra 100mg en France[/url] Viagra gГ©nГ©rique sans ordonnance en pharmacie and [url=http://talk.dofun.cc/home.php?mod=space&uid=57270]Viagra homme prix en pharmacie sans ordonnance[/url] Viagra homme prix en pharmacie sans ordonnance
http://levitrafr.life/# Pharmacie en ligne fiable
Pharmacie en ligne France Pharmacies en ligne certifiГ©es or acheter medicament a l etranger sans ordonnance
https://images.google.sk/url?q=http://pharmacieenligne.guru Pharmacie en ligne France
[url=https://redirect.cl/?r=https://pharmacieenligne.guru/]Pharmacie en ligne livraison rapide[/url] acheter medicament a l etranger sans ordonnance and [url=http://www.donggoudi.com/home.php?mod=space&uid=53744]Pharmacies en ligne certifiГ©es[/url] Pharmacie en ligne livraison gratuite
farmacia online madrid: kamagra gel – п»їfarmacia online
http://pharmacieenligne.guru/# pharmacie ouverte
Pharmacies en ligne certifiГ©es: pharmacie en ligne sans ordonnance – Pharmacie en ligne livraison 24h
https://kamagrafr.icu/# pharmacie ouverte 24/24
http://cialissansordonnance.pro/# Pharmacie en ligne pas cher
http://levitrafr.life/# pharmacie en ligne
Pharmacie en ligne livraison rapide [url=http://pharmacieenligne.guru/#]pharmacie ouverte[/url] Pharmacie en ligne pas cher
https://viagrasansordonnance.store/# Quand une femme prend du Viagra homme
farmacia online barata: farmacia envГos internacionales – п»їfarmacia online
http://levitrafr.life/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne livraison 24h Pharmacie en ligne France or acheter medicament a l etranger sans ordonnance
https://images.google.tk/url?sa=t&url=https://kamagrafr.icu pharmacie ouverte
[url=http://clients1.google.com.br/url?sa=t&url=https://kamagrafr.icu]pharmacie ouverte 24/24[/url] pharmacie ouverte and [url=http://www.mmecaw.com/home.php?mod=space&uid=478099]pharmacie ouverte[/url] Pharmacie en ligne fiable
Pharmacie en ligne France Pharmacie en ligne livraison gratuite or Pharmacie en ligne fiable
https://images.google.com.mx/url?sa=t&url=https://cialissansordonnance.pro Acheter mГ©dicaments sans ordonnance sur internet
[url=https://cse.google.ng/url?q=https://cialissansordonnance.pro]Pharmacie en ligne livraison 24h[/url] Pharmacie en ligne livraison 24h and [url=http://www.9kuan9.com/home.php?mod=space&uid=167940]Acheter mГ©dicaments sans ordonnance sur internet[/url] Pharmacie en ligne sans ordonnance
https://viagrasansordonnance.store/# Sildénafil 100 mg sans ordonnance
pharmacie ouverte: acheter kamagra site fiable – Pharmacie en ligne France
http://kamagrafr.icu/# Pharmacie en ligne France
acheter medicament a l etranger sans ordonnance [url=https://cialissansordonnance.pro/#]cialis prix[/url] acheter mГ©dicaments Г l’Г©tranger
https://kamagrakaufen.top/# online apotheke gГјnstig
online apotheke versandkostenfrei: cialis preise – online apotheke günstig
http://cialiskaufen.pro/# online-apotheken
versandapotheke versandkostenfrei [url=http://cialiskaufen.pro/#]potenzmittel cialis[/url] п»їonline apotheke
online apotheke preisvergleich: Potenzmittel Schneller Besser – online apotheke versandkostenfrei
https://apotheke.company/# online apotheke günstig
http://potenzmittel.men/# online apotheke preisvergleich
[url=https://albuterol.cyou/]cheap ventolin online[/url]
internet apotheke: kamagra jelly kaufen – günstige online apotheke
http://kamagrakaufen.top/# online apotheke versandkostenfrei
https://kamagrakaufen.top/# versandapotheke
online-apotheken internet apotheke or versandapotheke deutschland
http://images.google.mn/url?q=http://apotheke.company online-apotheken
[url=http://bigtorrent-ua.com/away.php?to=apotheke.company]п»їonline apotheke[/url] versandapotheke deutschland and [url=http://www.empyrethegame.com/forum/memberlist.php?mode=viewprofile&u=276168]internet apotheke[/url] online apotheke gГјnstig
online apotheke deutschland: online apotheke – günstige online apotheke
http://cialiskaufen.pro/# online apotheke deutschland
versandapotheke versandkostenfrei [url=https://kamagrakaufen.top/#]kamagra online bestellen[/url] internet apotheke
online-apotheken online apotheke versandkostenfrei or versandapotheke deutschland
https://www.google.dm/url?q=https://cialiskaufen.pro versandapotheke versandkostenfrei
[url=http://maps.google.com.ua/url?q=https://cialiskaufen.pro]online apotheke gГјnstig[/url] versandapotheke and [url=http://m.414500.cc/home.php?mod=space&uid=2900803]versandapotheke deutschland[/url] versandapotheke versandkostenfrei
Viagra kaufen Apotheke Preis: viagra tabletten – Viagra online bestellen Schweiz
http://kamagrakaufen.top/# online apotheke preisvergleich
https://kamagrakaufen.top/# versandapotheke
online apotheke: Cialis Generika 20mg preisvergleich – online apotheke deutschland
https://viagrakaufen.store/# Viagra online bestellen Schweiz
versandapotheke: potenzmittel rezeptfrei – versandapotheke versandkostenfrei
https://potenzmittel.men/# online apotheke
http://viagrakaufen.store/# Sildenafil Schweiz rezeptfrei kaufen
online-apotheken: cialis preise – versandapotheke deutschland
online-apotheken: versandapotheke – versandapotheke
http://cialiskaufen.pro/# versandapotheke
versandapotheke: apotheke online versandkostenfrei – online apotheke deutschland
http://viagrakaufen.store/# Viagra Tabletten für Männer
versandapotheke deutschland [url=http://potenzmittel.men/#]Potenzmittel Sildenafil[/url] online apotheke preisvergleich
online apotheke: Cialis Generika 20mg preisvergleich – online apotheke preisvergleich
http://kamagrakaufen.top/# online apotheke
https://potenzmittel.men/# online apotheke preisvergleich
online apotheke deutschland: online apotheke günstig – günstige online apotheke
https://apotheke.company/# online apotheke preisvergleich
internet apotheke: potenzmittel kaufen – versandapotheke
http://cialiskaufen.pro/# versandapotheke
online-apotheken versandapotheke versandkostenfrei or п»їonline apotheke
https://hjn.secure-dbprimary.com/service/util/logout/CookiePolicy.action?backto=http://apotheke.company&num=999 versandapotheke deutschland
[url=https://www.google.mn/url?sa=t&url=https://apotheke.company]internet apotheke[/url] internet apotheke and [url=http://cos258.com/home.php?mod=space&uid=1075480]online apotheke gГјnstig[/url] online-apotheken
Viagra rezeptfreie Länder Sildenafil kaufen online or Sildenafil 100mg online bestellen
http://alt1.toolbarqueries.google.ad/url?q=https://viagrakaufen.store Viagra Generika online kaufen ohne Rezept
[url=https://maps.google.co.il/url?sa=t&url=https://viagrakaufen.store]Viagra Г–sterreich rezeptfrei Apotheke[/url] Viagra Generika 100mg rezeptfrei and [url=http://www.stwx.net/space-uid-5883955.html]Viagra Preis Schwarzmarkt[/url] Sildenafil Preis
http://cialiskaufen.pro/# online apotheke deutschland
Billig Viagra bestellen ohne Rezept: Viagra Generika kaufen Schweiz – Potenzmittel Generika online kaufen
https://viagrakaufen.store/# Viagra wie lange steht er
gГјnstige online apotheke [url=https://cialiskaufen.pro/#]online-apotheken[/url] internet apotheke
online apotheke preisvergleich online apotheke deutschland or gГјnstige online apotheke
http://images.google.ro/url?q=https://cialiskaufen.pro п»їonline apotheke
[url=http://www.google.st/url?q=http://cialiskaufen.pro]online apotheke preisvergleich[/url] online-apotheken and [url=http://www.9kuan9.com/home.php?mod=space&uid=169518]online-apotheken[/url] internet apotheke
п»їonline apotheke internet apotheke or gГјnstige online apotheke
http://cse.google.com.eg/url?sa=t&url=https://kamagrakaufen.top online apotheke gГјnstig
[url=https://nutritiondata.self.com/facts/recipe/1304991/2?mbid=HDFD&trackback=http://kamagrakaufen.top/]versandapotheke[/url] online-apotheken and [url=http://m.414500.cc/home.php?mod=space&uid=2901170]versandapotheke[/url] internet apotheke
Viagra Österreich rezeptfrei Apotheke: viagra kaufen ohne rezept legal – Viagra kaufen ohne Rezept Schweiz
https://cialiskaufen.pro/# online apotheke günstig
http://apotheke.company/# online apotheke deutschland
Viagra 100 mg ohne Rezept: viagra kaufen – Viagra Tabletten für Männer
http://potenzmittel.men/# online apotheke versandkostenfrei
online apotheke günstig: kamagra oral jelly – versandapotheke versandkostenfrei
http://kamagrakaufen.top/# versandapotheke versandkostenfrei
http://potenzmittel.men/# gГјnstige online apotheke
internet apotheke [url=https://apotheke.company/#]apotheke online versandkostenfrei[/url] gГјnstige online apotheke
online apotheke günstig: Cialis Generika 20mg preisvergleich – günstige online apotheke
http://apotheke.company/# online apotheke deutschland
online-apotheken: online apotheke günstig – online apotheke
https://viagrakaufen.store/# Viagra Tabletten
http://mexicanpharmacy.cheap/# mexico drug stores pharmacies
mexican mail order pharmacies best mexican online pharmacies mexico pharmacy
best online pharmacies in mexico medicine in mexico pharmacies buying prescription drugs in mexico
mexico pharmacy best mexican online pharmacies mexico drug stores pharmacies
п»їbest mexican online pharmacies [url=https://mexicanpharmacy.cheap/#]mexico pharmacies prescription drugs[/url] п»їbest mexican online pharmacies
https://mexicanpharmacy.cheap/# mexico pharmacies prescription drugs
purple pharmacy mexico price list reputable mexican pharmacies online mexican drugstore online
best mexican online pharmacies mexico drug stores pharmacies buying prescription drugs in mexico
buying prescription drugs in mexico online best online pharmacies in mexico mexico drug stores pharmacies
buying prescription drugs in mexico online mexico pharmacies prescription drugs mexico pharmacies prescription drugs
mexico drug stores pharmacies [url=http://mexicanpharmacy.cheap/#]medication from mexico pharmacy[/url] buying from online mexican pharmacy
https://mexicanpharmacy.cheap/# medicine in mexico pharmacies
mexico drug stores pharmacies best online pharmacies in mexico or mexico pharmacies prescription drugs
https://mclast.de/redirect/?url=http://mexicanpharmacy.cheap mexico drug stores pharmacies
[url=https://www.google.md/url?q=https://mexicanpharmacy.cheap]buying from online mexican pharmacy[/url] mexican border pharmacies shipping to usa and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6458201]purple pharmacy mexico price list[/url] mexican mail order pharmacies
buying prescription drugs in mexico pharmacies in mexico that ship to usa or mexican mail order pharmacies
https://maps.google.com.my/url?q=https://mexicanpharmacy.cheap п»їbest mexican online pharmacies
[url=http://sunnymake.com/alexa/?domain=mexicanpharmacy.cheap]mexico pharmacies prescription drugs[/url] buying prescription drugs in mexico online and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9217591]mexico drug stores pharmacies[/url] medicine in mexico pharmacies
reputable mexican pharmacies online mexican border pharmacies shipping to usa mexican rx online
https://mexicanpharmacy.cheap/# п»їbest mexican online pharmacies
https://mexicanpharmacy.cheap/# п»їbest mexican online pharmacies
mexican border pharmacies shipping to usa [url=http://mexicanpharmacy.cheap/#]buying prescription drugs in mexico[/url] buying prescription drugs in mexico online
mexican drugstore online pharmacies in mexico that ship to usa mexican border pharmacies shipping to usa
mexico drug stores pharmacies mexican mail order pharmacies mexico pharmacy
reputable mexican pharmacies online medication from mexico pharmacy or mexico drug stores pharmacies
https://www.google.mn/url?sa=t&url=https://mexicanpharmacy.cheap mexican drugstore online
[url=https://clients1.google.tt/url?q=https://mexicanpharmacy.cheap]buying from online mexican pharmacy[/url] pharmacies in mexico that ship to usa and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3025219]mexico pharmacies prescription drugs[/url] mexican online pharmacies prescription drugs
mexico pharmacy mexico drug stores pharmacies mexico pharmacy
best mexican online pharmacies mexico pharmacies prescription drugs purple pharmacy mexico price list
https://mexicanpharmacy.cheap/# medication from mexico pharmacy
best online pharmacies in mexico [url=http://mexicanpharmacy.cheap/#]buying from online mexican pharmacy[/url] mexican border pharmacies shipping to usa
mexico pharmacies prescription drugs best online pharmacies in mexico mexican border pharmacies shipping to usa
https://mexicanpharmacy.cheap/# buying prescription drugs in mexico
best online pharmacies in mexico mexican online pharmacies prescription drugs or purple pharmacy mexico price list
https://maps.google.rs/url?sa=t&url=https://mexicanpharmacy.cheap mexican border pharmacies shipping to usa
[url=https://cse.google.st/url?sa=t&url=https://mexicanpharmacy.cheap]mexico drug stores pharmacies[/url] mexican rx online and [url=https://slovakia-forex.com/members/236189-ljtsdkpifr]mexican drugstore online[/url] best online pharmacies in mexico
best mexican online pharmacies buying prescription drugs in mexico mexican pharmaceuticals online
buying from online mexican pharmacy mexican drugstore online or purple pharmacy mexico price list
http://maps.google.co.mz/url?q=https://mexicanpharmacy.cheap buying prescription drugs in mexico online
[url=https://login.mephi.ru/login?allow_anonymous=true&service=https://mexicanpharmacy.cheap/]best online pharmacies in mexico[/url] mexico drug stores pharmacies and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9217337]п»їbest mexican online pharmacies[/url] buying prescription drugs in mexico
best online pharmacies in mexico mexican mail order pharmacies best mexican online pharmacies
purple pharmacy mexico price list buying prescription drugs in mexico mexico pharmacy
best mail order pharmacy canada [url=http://canadiandrugs.tech/#]legit canadian pharmacy online[/url] buy canadian drugs canadiandrugs.tech
online pharmacy india buy medicines online in india – buy medicines online in india indiapharmacy.guru
best erection pills new treatments for ed – best erectile dysfunction pills edpills.tech
http://canadiandrugs.tech/# canadian pharmacy reviews canadiandrugs.tech
indian pharmacy online world pharmacy india or indian pharmacies safe
http://albasu.jp/kyoto-quiz/_m/index.php?a=free_page/goto_mobile&referer=https://indiapharmacy.guru cheapest online pharmacy india
[url=https://images.google.ms/url?sa=t&url=https://indiapharmacy.guru]buy prescription drugs from india[/url] п»їlegitimate online pharmacies india and [url=http://xunshang.cc/home.php?mod=space&uid=4423687]indian pharmacy online[/url] top 10 pharmacies in india
canadian drug stores canada drugs reviews or drugs from canada
https://www.google.pl/url?q=https://canadiandrugs.tech canadian medications
[url=https://maps.google.ne/url?q=https://canadiandrugs.tech]northwest canadian pharmacy[/url] ed drugs online from canada and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=41831]safe online pharmacies in canada[/url] thecanadianpharmacy
http://edpills.tech/# cheap ed drugs edpills.tech
http://mexicanpharmacy.company/# best online pharmacies in mexico mexicanpharmacy.company
canadian pharmacy mall [url=http://canadiandrugs.tech/#]reliable canadian online pharmacy[/url] canadian pharmacy king reviews canadiandrugs.tech
top ed pills male ed pills – ed pills that work edpills.tech
https://canadiandrugs.tech/# canadian pharmacy reviews canadiandrugs.tech
https://indiapharmacy.guru/# cheapest online pharmacy india indiapharmacy.guru
non prescription ed pills drugs for ed or best male enhancement pills
https://www.google.ht/url?q=https://edpills.tech ed treatments
[url=https://www.google.com.ph/url?q=https://edpills.tech]cures for ed[/url] natural ed remedies and [url=https://forex-bitcoin.com/members/311068-yduzplcgpr]cheap ed drugs[/url] top ed pills
http://edpills.tech/# ed medication online edpills.tech
treatments for ed ed pills otc – pills for ed edpills.tech
top online pharmacy india best online pharmacy india or best india pharmacy
https://www.google.com.et/url?q=https://indiapharmacy.pro buy medicines online in india
[url=https://maps.google.iq/url?q=https://indiapharmacy.pro]indian pharmacy paypal[/url] top 10 online pharmacy in india and [url=http://talk.dofun.cc/home.php?mod=space&uid=112309]top 10 online pharmacy in india[/url] india pharmacy
http://indiapharmacy.guru/# online shopping pharmacy india indiapharmacy.guru
best mail order pharmacy canada [url=https://canadiandrugs.tech/#]canadian pharmacy 365[/url] reliable canadian pharmacy reviews canadiandrugs.tech
https://indiapharmacy.guru/# india pharmacy mail order indiapharmacy.guru
http://canadiandrugs.tech/# cheap canadian pharmacy canadiandrugs.tech
india pharmacy mail order canadian pharmacy india – reputable indian online pharmacy indiapharmacy.guru
safe reliable canadian pharmacy canadian pharmacy – canadian pharmacy meds canadiandrugs.tech
https://canadiandrugs.tech/# maple leaf pharmacy in canada canadiandrugs.tech
new ed drugs [url=http://edpills.tech/#]new ed pills[/url] erectile dysfunction drugs edpills.tech
https://canadiandrugs.tech/# best canadian pharmacy online canadiandrugs.tech
https://canadiandrugs.tech/# canadian pharmacy prices canadiandrugs.tech
https://canadapharmacy.guru/# safe canadian pharmacy canadapharmacy.guru
https://canadiandrugs.tech/# canadian pharmacy meds canadiandrugs.tech
online canadian pharmacy reviews canadian drugs pharmacy – canadian pharmacy prices canadiandrugs.tech
canadian pharmacy victoza canadianpharmacymeds com or trustworthy canadian pharmacy
https://maps.google.cl/url?sa=t&url=https://canadiandrugs.tech canada pharmacy reviews
[url=http://www.arndt-am-abend.de/url?q=https://canadiandrugs.tech]legitimate canadian pharmacies[/url] canadian pharmacy near me and [url=https://www.521zixuan.com/space-uid-604116.html]best canadian pharmacy to order from[/url] canadadrugpharmacy com
http://edpills.tech/# best ed treatment pills edpills.tech
reputable indian pharmacies online pharmacy india or best india pharmacy
https://cse.google.cat/url?q=https://indiapharmacy.guru indian pharmacy online
[url=http://www.ra2.od.ua/engine/redirect.php?url=http://indiapharmacy.guru]п»їlegitimate online pharmacies india[/url] top online pharmacy india and [url=http://lsdsng.com/user/512874]mail order pharmacy india[/url] Online medicine order
http://indiapharmacy.guru/# reputable indian online pharmacy indiapharmacy.guru
cross border pharmacy canada [url=http://canadiandrugs.tech/#]reliable canadian pharmacy[/url] canadian pharmacy online store canadiandrugs.tech
best medication for ed non prescription ed pills or ed dysfunction treatment
https://images.google.com.ec/url?q=https://edpills.tech new ed pills
[url=https://scanverify.com/siteverify.php?site=edpills.tech]ed pills[/url] treatments for ed and [url=http://hm5.cn/space-uid-1208813.html]cheapest ed pills[/url] buy ed pills online
canadian pharmacy mall best canadian online pharmacy reviews – certified canadian international pharmacy canadiandrugs.tech
canadian pharmacy india reputable indian pharmacies or india online pharmacy
https://www.ehso.com/ehsord.php?URL=https://indiapharmacy.pro indianpharmacy com
[url=http://3dpowertools.com/cgi-bin/animations.cgi?Animation=8&ReturnURL=http://indiapharmacy.pro]buy prescription drugs from india[/url] canadian pharmacy india and [url=http://hm5.cn/space-uid-1208819.html]indianpharmacy com[/url] best online pharmacy india
http://edpills.tech/# ed pills that work edpills.tech
https://indiapharmacy.guru/# online shopping pharmacy india indiapharmacy.guru
http://edpills.tech/# impotence pills edpills.tech
https://indiapharmacy.guru/# world pharmacy india indiapharmacy.guru
https://indiapharmacy.guru/# indian pharmacy indiapharmacy.guru
buy medicines online in india india pharmacy mail order – top online pharmacy india indiapharmacy.guru
https://indiapharmacy.pro/# reputable indian online pharmacy indiapharmacy.pro
reputable indian online pharmacy [url=https://indiapharmacy.guru/#]reputable indian pharmacies[/url] india online pharmacy indiapharmacy.guru
http://canadiandrugs.tech/# canadian online pharmacy canadiandrugs.tech
safe reliable canadian pharmacy ordering drugs from canada – trustworthy canadian pharmacy canadiandrugs.tech
https://indiapharmacy.guru/# top 10 pharmacies in india indiapharmacy.guru
[url=https://neurontin.cfd/]gabapentin 100mg price[/url]
https://edpills.tech/# pills for ed edpills.tech
https://canadiandrugs.tech/# canadian pharmacy 24h com safe canadiandrugs.tech
pharmacy website india reputable indian pharmacies or mail order pharmacy india
https://images.google.com.au/url?q=https://indiapharmacy.guru india online pharmacy
[url=http://kyivstar-inet.com/redirect/?url=https://indiapharmacy.guru/]best india pharmacy[/url] top 10 online pharmacy in india and [url=https://forex-bitcoin.com/members/310995-lqtsduvgzs]online shopping pharmacy india[/url] buy prescription drugs from india
canadian pharmacy mall cheapest pharmacy canada or online canadian pharmacy
https://maps.google.bg/url?sa=t&url=https://canadiandrugs.tech canadian 24 hour pharmacy
[url=https://www.google.gy/url?q=https://canadiandrugs.tech]canadian discount pharmacy[/url] canadian pharmacy online and [url=http://wuyuebanzou.com/home.php?mod=space&uid=432275]canadian valley pharmacy[/url] online canadian pharmacy
thecanadianpharmacy [url=https://canadiandrugs.tech/#]canadian pharmacies[/url] canadian pharmacy 1 internet online drugstore canadiandrugs.tech
http://canadiandrugs.tech/# canadian pharmacies comparison canadiandrugs.tech
buy medicines online in india top 10 pharmacies in india – pharmacy website india indiapharmacy.guru
http://canadiandrugs.tech/# best online canadian pharmacy canadiandrugs.tech
http://paxlovid.win/# paxlovid pharmacy
https://paxlovid.win/# paxlovid cost without insurance
can you buy prednisone over the counter in mexico: prednisone prescription online – prednisone 30 mg daily
cheap prednisone online: buy prednisone without a prescription – prednisone no rx
amoxicillin pills 500 mg: amoxicillin azithromycin – where can i buy amoxicillin over the counter
amoxicillin 200 mg tablet: amoxicillin 500mg over the counter – antibiotic amoxicillin
https://ciprofloxacin.life/# ciprofloxacin generic
cipro for sale [url=https://ciprofloxacin.life/#]buy cipro[/url] purchase cipro
paxlovid pharmacy: paxlovid for sale – paxlovid pill
http://ciprofloxacin.life/# buy cipro cheap
where to buy generic clomid: clomid without dr prescription – where can i get clomid no prescription
prednisone 5 mg cheapest: order prednisone from canada – prednisone 1 mg tablet
where to buy amoxicillin 500mg without prescription [url=https://amoxil.icu/#]amoxicillin 500mg pill[/url] how to buy amoxicillin online
http://ciprofloxacin.life/# ciprofloxacin 500mg buy online
ciprofloxacin generic price buy cipro online without prescription or buy ciprofloxacin over the counter
http://www.google.mu/url?q=https://ciprofloxacin.life ciprofloxacin
[url=https://www.google.bf/url?q=https://ciprofloxacin.life]ciprofloxacin mail online[/url] antibiotics cipro and [url=http://cos258.com/home.php?mod=space&uid=1081263]buy cipro cheap[/url] buy ciprofloxacin
purchase cipro: cipro ciprofloxacin – ciprofloxacin mail online
amoxicillin generic amoxil pharmacy or how much is amoxicillin prescription
https://clients1.google.cd/url?q=http://amoxil.icu amoxicillin 250 mg
[url=https://maps.google.iq/url?q=https://amoxil.icu]amoxicillin 250 mg price in india[/url] amoxicillin over counter and [url=https://slovakia-forex.com/members/237314-koomfvrrfp]amoxicillin 500mg capsules antibiotic[/url] how much is amoxicillin
get generic clomid pills: how to get clomid without insurance – can i order cheap clomid
paxlovid covid: Paxlovid over the counter – п»їpaxlovid
https://prednisone.bid/# prednisone 20 mg pill
paxlovid buy [url=https://paxlovid.win/#]п»їpaxlovid[/url] buy paxlovid online
ciprofloxacin 500 mg tablet price: buy cipro cheap – where can i buy cipro online
paxlovid india: paxlovid pill – paxlovid covid
prednisone 10mg online prednisone buy canada or prednisone 20mg capsule
https://community.sugarcrm.com/external-link.jspa?url=http://prednisone.bid 10 mg prednisone
[url=https://maps.google.com.ph/url?q=https://prednisone.bid]prednisone 50 mg tablet cost[/url] prednisone canada and [url=https://slovakia-forex.com/members/237348-tahbtzetlf]prednisone pill prices[/url] order prednisone on line
http://ciprofloxacin.life/# cipro
amoxicillin without rx: amoxicillin 500 mg purchase without prescription – how to get amoxicillin
paxlovid covid [url=https://paxlovid.win/#]paxlovid cost without insurance[/url] Paxlovid buy online
cipro: cipro online no prescription in the usa – buy ciprofloxacin
can you get cheap clomid no prescription: how to get cheap clomid prices – how to buy clomid
how to get cheap clomid for sale: can i order generic clomid for sale – can i order clomid pill
http://prednisone.bid/# prednisone 5mg coupon
buy cipro cheap [url=http://ciprofloxacin.life/#]ciprofloxacin[/url] п»їcipro generic
can i order generic clomid tablets: where can i get cheap clomid – cost clomid pills
Paxlovid over the counter paxlovid cost without insurance or paxlovid india
http://www.google.com.ag/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&ved=0cc0qfjaa&url=https://paxlovid.win/ paxlovid cost without insurance
[url=http://stopundshop.eu/url?q=https://paxlovid.win]Paxlovid over the counter[/url] paxlovid buy and [url=http://80tt1.com/home.php?mod=space&uid=159501]п»їpaxlovid[/url] п»їpaxlovid
cipro for sale: purchase cipro – ciprofloxacin generic
https://amoxil.icu/# generic for amoxicillin
buy prednisone online fast shipping: generic prednisone tablets – otc prednisone cream
https://amoxil.icu/# 875 mg amoxicillin cost
cheap amoxicillin 500mg [url=http://amoxil.icu/#]amoxicillin tablets in india[/url] how to get amoxicillin over the counter
buying cheap clomid online: get cheap clomid pills – generic clomid online
ciprofloxacin over the counter: purchase cipro – buy ciprofloxacin over the counter
buy ciprofloxacin over the counter where can i buy cipro online or buy cipro
https://www.iexprofs.nl/go/14940/link.aspx?url=http://ciprofloxacin.life cipro ciprofloxacin
[url=http://www.konradchristmann.de/url?q=https://ciprofloxacin.life]cipro for sale[/url] buy cipro online and [url=http://www.aiwujie.wang/home.php?mod=space&uid=2036058]buy cipro online[/url] ciprofloxacin generic
ciprofloxacin generic price: ciprofloxacin order online – cipro for sale
buy cipro without rx [url=http://ciprofloxacin.life/#]ciprofloxacin generic[/url] ciprofloxacin generic
where can i get clomid: cost clomid without a prescription – where can i buy cheap clomid
https://prednisone.bid/# prednisone
generic prednisone 10mg iv prednisone or otc prednisone cream
http://clients1.google.mk/url?q=https://prednisone.bid prednisone in india
[url=https://clients1.google.nu/url?q=https://prednisone.bid]prednisone 5 mg tablet[/url] buy prednisone canadian pharmacy and [url=http://m.414500.cc/home.php?mod=space&uid=2964739]6 prednisone[/url] prednisone canada pharmacy
amoxicillin 875 125 mg tab [url=http://amoxil.icu/#]amoxicillin without a doctors prescription[/url] amoxicillin script
where can i get amoxicillin 500 mg ampicillin amoxicillin or buy amoxicillin 500mg uk
https://www.google.com.na/url?q=https://amoxil.icu cost of amoxicillin 30 capsules
[url=https://toolbarqueries.google.com.vc/url?q=https://amoxil.icu]amoxicillin capsules 250mg[/url] amoxicillin 500 mg tablet and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=108942]amoxicillin pharmacy price[/url] order amoxicillin online uk
amoxicillin no prescription: purchase amoxicillin 500 mg – buy cheap amoxicillin online
http://ciprofloxacin.life/# ciprofloxacin over the counter
paxlovid for sale [url=https://paxlovid.win/#]paxlovid for sale[/url] paxlovid cost without insurance
amoxicillin without rx: amoxicillin 30 capsules price – amoxicillin 500mg capsules
https://clomid.site/# generic clomid for sale
amoxicillin pharmacy price: amoxicillin 825 mg – amoxicillin 500mg over the counter
buy amoxicillin online with paypal [url=https://amoxil.icu/#]order amoxicillin online[/url] amoxicillin online pharmacy
purchase cipro: ciprofloxacin mail online – buy cipro cheap
[url=http://lexapro.cfd/]lexapro 20 mg[/url]
where to buy generic clomid prices: cheap clomid no prescription – can i get cheap clomid online
https://ciprofloxacin.life/# ciprofloxacin generic
order clomid without dr prescription buy cheap clomid without dr prescription – buy clomid no prescription
https://amoxil.icu/# amoxicillin 500mg capsule buy online
https://amoxil.icu/# amoxicillin for sale online
prednisone cost 10mg: 100 mg prednisone daily – prednisone 20 mg generic
cost of tamoxifen [url=https://nolvadex.fun/#]tamoxifen effectiveness[/url] tamoxifen dosage
buy cytotec online fast delivery: buy cytotec pills online cheap – buy cytotec pills
https://lisinoprilbestprice.store/# generic for prinivil
hysterectomy after breast cancer tamoxifen: how to get nolvadex – lexapro and tamoxifen
https://doxycyclinebestprice.pro/# 200 mg doxycycline
http://nolvadex.fun/# nolvadex half life
tamoxifen 20 mg tablet: tamoxifen headache – how does tamoxifen work
lisinopril with out prescription: https://lisinoprilpharm.com/%5Dlisinopril – can i buy lisinopril over the counter in mexico
https://nolvadex.fun/# aromatase inhibitors tamoxifen
doxycycline vibramycin [url=http://doxycyclinebestprice.pro/#]doxycycline hyclate[/url] doxycycline hyclate
common side effects of tamoxifen: tamoxifen and osteoporosis – tamoxifen and osteoporosis
zithromax prescription in canada: where to get zithromax – zithromax capsules
http://nolvadex.fun/# tamoxifen for sale
price of doxycycline: buy doxycycline online – buy cheap doxycycline
http://nolvadex.fun/# tamoxifen estrogen
Получите перетяжку мягкой мебели с гарантией качества
Обновление мягкой мебели: простой способ обновить интерьер
Высокое обслуживание перетяжки мягкой мебели
Легко и просто обновить диван или кресло
перетяжка мебели [url=http://www.peretyazhkann.ru]http://www.peretyazhkann.ru[/url].
generic lisinopril 5 mg: lisinopril 10 12.5 mg – lisinopril 10 mg tablet price
buy doxycycline monohydrate [url=https://doxycyclinebestprice.pro/#]buy doxycycline online without prescription[/url] doxycycline 100mg price
lisinopril 10 mg daily: lisinopril 2.5 pill – zestril 20 mg cost
https://lisinoprilbestprice.store/# can you buy lisinopril
doxycycline 500mg: purchase doxycycline online – doxycycline 100mg price
tamoxifen mechanism of action: tamoxifen vs clomid – clomid nolvadex
I have fun with, result in I discovered just what I used to be taking a look for. You have ended my four day lengthy hunt! God Bless you man. Have a great day. Bye
http://nolvadex.fun/# tamoxifen chemo
https://cytotec.icu/# buy cytotec over the counter
lisinopril 420 1g: zestoretic 10 mg – generic zestril
lisinopril 5mg [url=http://lisinoprilbestprice.store/#]zestril over the counter[/url] where can i order lisinopril online
http://nolvadex.fun/# tamoxifen bone density
can i buy zithromax over the counter generic zithromax india or <a href=" http://eu-clearance.satfrance.com/?a%5B%5D=cialis+tablets “>zithromax 250
https://images.google.ng/url?q=https://zithromaxbestprice.icu zithromax order online uk
[url=http://images.google.la/url?q=https://zithromaxbestprice.icu]zithromax z-pak[/url] generic zithromax online paypal and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1467734]order zithromax without prescription[/url] where to get zithromax over the counter
canada cloud pharmacy: Cheapest drug prices Canada – canadadrugpharmacy com canadapharm.life
reputable mexican pharmacies online [url=https://mexicopharm.com/#]Mexico pharmacy online[/url] pharmacies in mexico that ship to usa mexicopharm.com
http://mexicopharm.com/# mexican pharmacy mexicopharm.com
mexican online pharmacies prescription drugs: mexico drug stores pharmacies – pharmacies in mexico that ship to usa mexicopharm.com
mexican online pharmacies prescription drugs: Purple Pharmacy online ordering – buying prescription drugs in mexico online mexicopharm.com
best online pharmacies in mexico: Medicines Mexico – buying prescription drugs in mexico online mexicopharm.com
https://indiapharm.llc/# Online medicine home delivery indiapharm.llc
https://mexicopharm.com/# mexican border pharmacies shipping to usa mexicopharm.com
medication canadian pharmacy: Canada pharmacy online – best canadian pharmacy online canadapharm.life
safe canadian pharmacies [url=https://canadapharm.life/#]drugs from canada[/url] canadian pharmacy meds canadapharm.life
https://mexicopharm.com/# purple pharmacy mexico price list mexicopharm.com
indian pharmacy: Medicines from India to USA online – india online pharmacy indiapharm.llc
top 10 pharmacies in india: india pharmacy mail order – cheapest online pharmacy india indiapharm.llc
http://canadapharm.life/# canadian pharmacy online reviews canadapharm.life
buying from online mexican pharmacy: Best pharmacy in Mexico – mexican rx online mexicopharm.com
http://canadapharm.life/# legal to buy prescription drugs from canada canadapharm.life
mexican online pharmacies prescription drugs: Mexico pharmacy online – п»їbest mexican online pharmacies mexicopharm.com
indian pharmacies safe: reputable indian online pharmacy – online pharmacy india indiapharm.llc
https://mexicopharm.com/# medicine in mexico pharmacies mexicopharm.com
online shopping pharmacy india: India pharmacy of the world – reputable indian pharmacies indiapharm.llc
canadian pharmacies [url=https://canadapharm.life/#]Canada pharmacy online[/url] canadian family pharmacy canadapharm.life
cheapest online pharmacy india: top 10 pharmacies in india – buy medicines online in india indiapharm.llc
http://canadapharm.life/# canadian pharmacy victoza canadapharm.life
medicine in mexico pharmacies: Medicines Mexico – mexico pharmacies prescription drugs mexicopharm.com
https://indiapharm.llc/# india pharmacy mail order indiapharm.llc
world pharmacy india п»їlegitimate online pharmacies india or online pharmacy india
http://www.morgeneyer.de/ahnen/login/default.aspx?returnurl=http://indiapharm.llc/ buy medicines online in india
[url=http://yoko14145.com/mt/mt4i.cgi?id=3&mode=redirect&no=40&ref_eid=481&url=https://indiapharm.llc]pharmacy website india[/url] п»їlegitimate online pharmacies india and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3034618]indian pharmacy online[/url] buy medicines online in india
https://edpillsdelivery.pro/# best medication for ed
Vardenafil online prescription [url=https://levitradelivery.pro/#]Buy generic Levitra online[/url] Levitra 20 mg for sale
cialis tadalafil: cheap tadalafil canada – where to buy tadalafil 20mg
http://tadalafildelivery.pro/# buy tadalafil europe
п»їkamagra [url=http://kamagradelivery.pro/#]kamagra oral jelly[/url] Kamagra 100mg price
Каталог мобильных устройств в нашем онлайн магазине: большой выбор и лучшие модели
магазин – [url=https://xn--80abhspddm.xn--90ais/]онлайн магазин[/url].
Kamagra 100mg: п»їkamagra – buy kamagra online usa
http://kamagradelivery.pro/# cheap kamagra
Vardenafil buy online: Levitra online – Buy Vardenafil 20mg
https://sildenafildelivery.pro/# sildenafil 20 mg coupon
https://tadalafildelivery.pro/# buy generic tadalafil online uk
http://kamagradelivery.pro/# cheap kamagra
tadalafil 20 mg mexico [url=http://tadalafildelivery.pro/#]tadalafil 20 mg price canada[/url] generic tadalafil in canada
best male ed pills: ed pills online – best pill for ed
tadalafil online 10mg: generic tadalafil in canada – buy tadalafil from canada
tadalafil canadian pharmacy online [url=https://tadalafildelivery.pro/#]tadalafil 2.5 mg online india[/url] tadalafil tablets 20 mg cost
http://sildenafildelivery.pro/# sildenafil 20 mg price in india
price comparison tadalafil tadalafil 20 mg buy online or medicine tadalafil tablets
http://www.marstruct-vi.com/feedback.aspx?page=http://tadalafildelivery.pro/ cheap generic tadalafil
[url=http://images.google.com.bz/url?q=https://tadalafildelivery.pro]buy tadalafil cialis[/url] tadalafil cheapest price and [url=http://www.xiaolanmb.com/space-uid-30442.html]tadalafil 22 mg[/url] tadalafil 100mg
Levitra 10 mg best price: Generic Levitra 20mg – Levitra online pharmacy
http://levitradelivery.pro/# Buy Levitra 20mg online
http://tadalafildelivery.pro/# tadalafil – generic
Kamagra 100mg price [url=https://kamagradelivery.pro/#]buy kamagra[/url] super kamagra
Cheap Levitra online: Buy Vardenafil 20mg – Cheap Levitra online
https://kamagradelivery.pro/# buy Kamagra
https://edpillsdelivery.pro/# medication for ed
where to buy sildenafil uk: Sildenafil price – generic sildenafil cost usa
tadalafil 2.5 mg generic: tadalafil united states – buy tadalafil india
Vardenafil price [url=http://levitradelivery.pro/#]Buy generic Levitra online[/url] Generic Levitra 20mg
best ed medication: buy ed drugs online – online ed medications
http://kamagradelivery.pro/# cheap kamagra
http://sildenafildelivery.pro/# generic sildenafil from india
buy tadalafil cialis [url=https://tadalafildelivery.pro/#]tadalafil without a doctor prescription[/url] generic tadalafil 20mg canada
I truly appreciate your technique of writing a blog. I added it to my bookmark site list and will
order sildenafil: sildenafil mexico online – sildenafil tablets 100mg price
http://clomid.auction/# can you buy generic clomid pill
http://amoxil.guru/# buy amoxicillin 500mg canada
http://stromectol.guru/# minocycline 100mg pills
paxlovid covid: Paxlovid buy online – paxlovid price
https://amoxil.guru/# amoxicillin tablet 500mg
https://amoxil.guru/# ampicillin amoxicillin
buy prednisone 40 mg: buy prednisone online canada – prednisone 10mg for sale
paxlovid buy [url=https://paxlovid.guru/#]paxlovid best price[/url] paxlovid for sale
Отремонтировать мягкую мебель в доме: Дать новый вид старой мебели: простой гайд перетягивать мебель своими руками: Выбор ткани для перетяжки мягкой мебели: секреты выбора
[url=https://art-restor.ru/]перетяжка мягкой мебели[/url].
Обновление интерьера: перетяжка мягкой мебели на практике
prednisone 100 mg: buy prednisone over the counter – prednisone online sale
http://paxlovid.guru/# paxlovid pharmacy
http://amoxil.guru/# where to get amoxicillin over the counter
ivermectin lice: stromectol guru – generic ivermectin
https://paxlovid.guru/# Paxlovid buy online
http://amoxil.guru/# where can you get amoxicillin
https://amoxil.guru/# can you buy amoxicillin uk
https://stromectol.guru/# buy stromectol canada
amoxicillin without a prescription: buy amoxil online – generic amoxicillin cost
prednisone prescription drug: best prednisone – buy prednisone canada
https://stromectol.guru/# where to buy stromectol
paxlovid buy [url=https://paxlovid.guru/#]Buy Paxlovid privately[/url] paxlovid buy
where can i buy amoxocillin: buy amoxil online – amoxicillin 500mg buy online uk
http://amoxil.guru/# amoxicillin brand name
http://clomid.auction/# how to get clomid for sale
http://amoxil.guru/# amoxicillin 750 mg price
paxlovid pharmacy: paxlovid best price – paxlovid price
http://clomid.auction/# can you buy generic clomid no prescription
paxlovid buy: paxlovid cost without insurance – paxlovid for sale
https://stromectol.guru/# ivermectin 4000
https://stromectol.guru/# ivermectin purchase
paxlovid for sale [url=https://paxlovid.guru/#]Paxlovid buy online[/url] Paxlovid buy online
amoxicillin 500 mg for sale amoxicillin 500 mg price or where can i buy amoxicillin without prec
https://www.stefanwilkening.de/anzeiger.php?anzeige=amoxil.guru:: generic amoxicillin online
[url=http://tyadnetwork.com/ads_top.php?url=https://amoxil.guru/]buy amoxil[/url] amoxicillin 750 mg price and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=46790]can you buy amoxicillin over the counter[/url] amoxicillin 500mg buy online uk
amoxicillin 500mg no prescription: buy amoxil online – amoxicillin over the counter in canada
https://paxlovid.guru/# paxlovid cost without insurance
https://paxlovid.guru/# paxlovid price
cheap propecia no prescription: buy propecia – buy propecia pill
buy cytotec pills online cheap [url=https://misoprostol.shop/#]Buy Abortion Pills Online[/url] cytotec online
prinivil 40 mg: lisinopril 40 mg on line – medication lisinopril 5 mg
http://azithromycin.store/# zithromax capsules 250mg
https://furosemide.pro/# lasix 40mg
zithromax online usa: cheapest azithromycin – how to get zithromax
http://finasteride.men/# buy cheap propecia pills
cytotec abortion pill: Misoprostol best price in pharmacy – Cytotec 200mcg price
zithromax antibiotic: zithromax for sale online – zithromax z-pak price without insurance
zithromax pill [url=http://azithromycin.store/#]buy zithromax over the counter[/url] buy zithromax online
http://misoprostol.shop/# purchase cytotec
lasix furosemide 40 mg: Buy Lasix – furosemide 100mg
http://misoprostol.shop/# buy cytotec in usa
http://lisinopril.fun/# lisinopril 15 mg
order cheap propecia prices: Finasteride buy online – buy propecia pills
http://azithromycin.store/# can i buy zithromax over the counter
Изменение мебели с помощью перетяжки – быстро и просто
перетяжка мягкой мебели [url=https://peretyazhka-mebeli-v-minske.ru/#перетяжка-мягкой-мебели]https://peretyazhka-mebeli-v-minske.ru/[/url].
lasix 100 mg tablet [url=http://furosemide.pro/#]buy furosemide online[/url] furosemide 100mg
lasix 100mg: Buy Furosemide – lasix for sale
prinivil 20mg tabs: buy lisinopril canada – lisinopril 20 mg canada
https://misoprostol.shop/# Misoprostol 200 mg buy online
🌌 Wow, blog ini seperti petualangan fantastis meluncurkan ke alam semesta dari kegembiraan! 🌌 Konten yang mengagumkan di sini adalah perjalanan rollercoaster yang mendebarkan bagi pikiran, memicu kegembiraan setiap saat. 💫 Baik itu gayahidup, blog ini adalah sumber wawasan yang mendebarkan! #TerpukauPikiran Berangkat ke dalam perjalanan kosmik ini dari pengetahuan dan biarkan pikiran Anda terbang! 🌈 Jangan hanya membaca, alami kegembiraan ini! #MelampauiBiasa Pikiran Anda akan bersyukur untuk perjalanan mendebarkan ini melalui alam keajaiban yang menakjubkan! ✨
prinivil 20 mg: buy lisinopril online – prinivil 25mg
[url=http://accutane.cyou/]accutane australia buy online[/url]
Дарите себе комфорт с мягкой мебелью
ремонт мебели [url=https://murom-mebel-tula.ru/]https://murom-mebel-tula.ru/[/url].
https://azithromycin.store/# buy zithromax 500mg online
http://furosemide.pro/# lasix furosemide 40 mg
Придайте яркость и оригинальность мебели с перетяжкой
перетяжка мягкой мебели [url=https://vk.com/peretyazhka_mebeli_by/]перетяжка кресел[/url].
cost of lisinopril in mexico: buy lisinopril online – lisinopril 2mg tablet
propecia no prescription [url=https://finasteride.men/#]Cheapest finasteride online[/url] order cheap propecia without insurance
zithromax capsules price: buy zithromax over the counter – zithromax generic cost
https://furosemide.pro/# lasix furosemide 40 mg
http://azithromycin.store/# generic zithromax india
lasix: Buy Lasix No Prescription – lasix generic name
where can i buy zithromax medicine zithromax cost australia or zithromax buy online
https://www.google.ps/url?sa=t&url=https://azithromycin.store where can i buy zithromax in canada
[url=http://tourzwei.radblogger.net/redirect.php?url=azithromycin.store]zithromax coupon[/url] where to get zithromax over the counter and [url=https://98e.fun/space-uid-7040431.html]zithromax over the counter uk[/url] average cost of generic zithromax
order propecia pills cost propecia for sale or cheap propecia without dr prescription
https://maps.google.lk/url?sa=t&url=https://finasteride.men get propecia online
[url=https://ashirovo.ru/bitrix/rk.php?goto=https://finasteride.men]buying propecia[/url] generic propecia without insurance and [url=https://forex-bitcoin.com/members/315844-mwnaafmnoz]propecia order[/url] buying cheap propecia price
furosemide 100 mg lasix 40mg or buy furosemide online
https://image.google.im/url?q=https://furosemide.pro lasix 40mg
[url=https://maps.google.dm/url?q=https://furosemide.pro]lasix furosemide[/url] furosemide and [url=http://lsdsng.com/user/516993]furosemide 40 mg[/url] lasix
propecia without dr prescription: Buy finasteride 1mg – get propecia online
http://azithromycin.store/# buy generic zithromax no prescription
Качественный ремонт холодильников
ремонт холодильника [url=https://remontholodilnikov-vminske.ru/]ремонт холодильников[/url].
generic lasix [url=https://furosemide.pro/#]Buy Lasix No Prescription[/url] furosemide 40 mg
http://misoprostol.shop/# Abortion pills online
https://misoprostol.shop/# Abortion pills online
zithromax 500 price: buy zithromax z-pak online – where can i buy zithromax capsules
buy cytotec over the counter: Abortion pills online – buy cytotec
Забота о жилье – это забота о спокойствии. Теплоизоляция стен – это не только модный облик, но и гарантия сохранения тепла в вашем уютном уголке. Мы, наши мастера, предлагаем вам преобразить ваше жилище в идеальное жилище.
Наши улучшения – это не просто тепловая обработка, это творческий процесс с каждым строительным блоком. Мы стремимся к совершенному сочетанию между формой и содержанием, чтобы ваш дом преобразился не только комфортным, но и шикарным.
И самое главное – удовлетворительная стоимость! Мы уверены, что профессиональные услуги не должны быть неприемлемо дорогими. [url=https://ppu-prof.ru/]Сколько стоит сделать утепление фасада[/url] начинается всего от 1250 рублей за кв. метр.
Современные технологии и высококачественные материалы позволяют нам создавать утепление, обеспечивающее долговечность и надежность. Прощайте холодным стенам и дополнительным тратам на отопление – наше утепление станет вашим надежным защитником от холода.
Подробнее на [url=https://ppu-prof.ru/]https://www.ppu-prof.ru[/url]
Не откладывайте на потом заботу о радости жизни в вашем жилье. Обращайтесь к специалистам, и ваш дом станет настоящим произведением искусства, которое подарит вам не только тепло. Вместе мы создадим дом, в котором вам будет по-настоящему удобно!
https://finasteride.men/# order cheap propecia no prescription
http://finasteride.men/# propecia pills
cheap zithromax pills: buy zithromax z-pak online – zithromax pill
generic lasix [url=http://furosemide.pro/#]Over The Counter Lasix[/url] furosemide 100 mg
https://avanafilitalia.online/# farmacia online più conveniente
acquisto farmaci con ricetta: comprare avanafil senza ricetta – farmacia online
viagra cosa serve: viagra prezzo – siti sicuri per comprare viagra online
http://sildenafilitalia.men/# gel per erezione in farmacia
farmacie on line spedizione gratuita: kamagra gold – farmacie online autorizzate elenco
http://kamagraitalia.shop/# farmacie online sicure
https://farmaciaitalia.store/# comprare farmaci online con ricetta
farmacia online miglior prezzo [url=http://kamagraitalia.shop/#]kamagra gel[/url] farmacie online sicure
farmacia online miglior prezzo: kamagra gel prezzo – farmacia online migliore
farmacie online sicure: avanafil prezzo in farmacia – acquistare farmaci senza ricetta
http://kamagraitalia.shop/# migliori farmacie online 2023
migliori farmacie online 2023 [url=https://tadalafilitalia.pro/#]Farmacie a milano che vendono cialis senza ricetta[/url] farmacia online
farmacia online piГ№ conveniente: avanafil spedra – farmacie on line spedizione gratuita
https://kamagraitalia.shop/# farmacia online senza ricetta
http://tadalafilitalia.pro/# top farmacia online
farmacia online miglior prezzo: Dove acquistare Cialis online sicuro – farmacia online
Magnificent items from you, man. I’ve have in mind
your stuff previous to and you’re simply extremely magnificent.
I really like what you have acquired right here, certainly like
what you are stating and the way during which you say it.
You make it enjoyable and you still care for to keep it smart.
I can’t wait to learn much more from you.
That is actually a terrific site.
the canadian drugstore [url=https://canadianpharmacy.pro/#]Pharmacies in Canada that ship to the US[/url] canadian pharmacy review canadianpharmacy.pro
https://canadianpharmacy.pro/# canadian pharmacy 24 canadianpharmacy.pro
http://canadianpharmacy.pro/# canadian pharmacy king reviews canadianpharmacy.pro
list of aarp approved pharmacies
india pharmacy mail order: indian pharmacy to usa – reputable indian online pharmacy indianpharmacy.shop
onlinecanadianpharmacy 24 [url=http://canadianpharmacy.pro/#]Canada Pharmacy[/url] canadian drug stores canadianpharmacy.pro
legal to buy prescription drugs from canada: canada pharmacy – canadapharmacyonline com canadianpharmacy.pro
http://indianpharmacy.shop/# india pharmacy mail order indianpharmacy.shop
indian pharmacy paypal [url=http://indianpharmacy.shop/#]Cheapest online pharmacy[/url] п»їlegitimate online pharmacies india indianpharmacy.shop
http://indianpharmacy.shop/# indian pharmacy paypal indianpharmacy.shop
mexico drug stores pharmacies: mexican pharmacy online – mexican drugstore online mexicanpharmacy.win
https://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
https://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
online pharmacies no prescription required pain medication
mexico drug stores pharmacies [url=https://mexicanpharmacy.win/#]mexican border pharmacies shipping to usa[/url] mexican rx online mexicanpharmacy.win
http://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
indian pharmacies safe online pharmacy india or Online medicine order
https://cse.google.ht/url?sa=t&url=https://indianpharmacy.shop reputable indian pharmacies
[url=https://forums2.battleon.com/f/interceptor.asp?dest=http://indianpharmacy.shop/]online pharmacy india[/url] online shopping pharmacy india and [url=https://98e.fun/space-uid-7072523.html]india pharmacy mail order[/url] indian pharmacy paypal
mexico pharmacies prescription drugs [url=http://mexicanpharmacy.win/#]mexican pharmacy online[/url] mexican drugstore online mexicanpharmacy.win
https://indianpharmacy.shop/# online pharmacy india indianpharmacy.shop
legal canadian pharmacy online canadian drugstore online or safe online pharmacies in canada
https://navilleauction.auctionserver.net/view-auctions/catalog/id/81/lot/1537/?url=http://canadianpharmacy.pro canada drugs
[url=https://www.google.com.pg/url?q=https://canadianpharmacy.pro]canadapharmacyonline[/url] canadian drug prices and [url=https://www.warshipsfaq.ru/user/qmijhwgngv]77 canadian pharmacy[/url] best canadian online pharmacy
Online medicine order [url=http://indianpharmacy.shop/#]Best Indian pharmacy[/url] reputable indian online pharmacy indianpharmacy.shop
http://mexicanpharmacy.win/# mexican pharmaceuticals online mexicanpharmacy.win
https://canadianpharmacy.pro/# canada cloud pharmacy canadianpharmacy.pro
reputable indian pharmacies
https://canadianpharmacy.pro/# canadian medications canadianpharmacy.pro
list of canada online pharmacies
http://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
indian pharmacy [url=https://indianpharmacy.shop/#]indian pharmacy[/url] pharmacy website india indianpharmacy.shop
canada drugs online reviews canadian pharmacy cheap or cheap canadian pharmacy online
https://maps.google.gg/url?sa=t&url=https://canadianpharmacy.pro canadian pharmacies online
[url=https://cse.google.co.bw/url?sa=t&url=https://canadianpharmacy.pro]canada drugs online[/url] safe canadian pharmacy and [url=https://lhgangguanwang.com/home.php?mod=space&uid=70911]ed meds online canada[/url] canadian drugstore online
다양한 테마의 무료 프라그마틱 슬롯을 즐겨보세요.
프라그마틱 무료
프라그마틱 슬롯에 대한 내용이 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 찾아보실 수 있어요. 함께 지식을 공유해보세요!
https://jxbodun.com/
https://www.vamiveta.com/
https://s9winmy.com/
online pharmacies canadian prescription without a doctors prescription or canadian drug mart pharmacy
http://www.mydnstats.com/index.php?a=search&q=canadianpharmacy.pro canadian mail order meds
[url=https://www.film1.nl/zoek/?q=/><a+href=http://canadianpharmacy.pro&]cheapest canadian pharmacy[/url] vipps accredited online pharmacy and [url=http://www.mmecaw.com/home.php?mod=space&uid=505162]canadian drug pharmacy[/url] get canadian drugs
http://indianpharmacy.shop/# cheapest online pharmacy india indianpharmacy.shop
world pharmacy india
https://indianpharmacy.shop/# pharmacy website india indianpharmacy.shop
medicine in mexico pharmacies mexico drug stores pharmacies or best online pharmacies in mexico
http://wishforthis.com/Shop/Redirect.php?URL=http://mexicopharm.com/ purple pharmacy mexico price list
[url=https://clients1.google.bf/url?q=https://mexicopharm.com]buying prescription drugs in mexico[/url] buying prescription drugs in mexico and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3047382]п»їbest mexican online pharmacies[/url] purple pharmacy mexico price list
mexican pharmaceuticals online [url=https://mexicanpharmacy.win/#]online mexican pharmacy[/url] mexico drug stores pharmacies mexicanpharmacy.win
http://canadianpharmacy.pro/# buy prescription drugs from canada cheap canadianpharmacy.pro
india pharmacy mail order
https://mexicanpharmacy.win/# mexico pharmacies prescription drugs mexicanpharmacy.win
canadian pharmacies for cialis
http://mexicanpharmacy.win/# mexico drug stores pharmacies mexicanpharmacy.win
https://indianpharmacy.shop/# Online medicine order indianpharmacy.shop
canadian pharmacy king reviews [url=https://canadianpharmacy.pro/#]Canada Pharmacy[/url] best canadian pharmacy online canadianpharmacy.pro
http://indianpharmacy.shop/# Online medicine order indianpharmacy.shop
best india pharmacy
legit canadian pharmacy online canadian neighbor pharmacy or best rated canadian pharmacy
http://images.google.gm/url?q=http://canadianpharmacy.pro canadian mail order pharmacy
[url=http://www.tvtix.com/frame.php?url=http://canadianpharmacy.pro]canadian pharmacy meds[/url] canadian pharmacy meds review and [url=http://bbs.mycq3d.com/home.php?mod=space&uid=37393]certified canadian pharmacy[/url] adderall canadian pharmacy
http://canadianpharmacy.pro/# legitimate canadian pharmacy canadianpharmacy.pro
top 10 pharmacies in india [url=http://indianpharmacy.shop/#]mail order pharmacy india[/url] indian pharmacy paypal indianpharmacy.shop
http://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
best online pharmacy india
https://mexicanpharmacy.win/# mexican pharmaceuticals online mexicanpharmacy.win
indian pharmacy paypal: top 10 pharmacies in india – top 10 pharmacies in india indianpharmacy.shop
Acheter mГ©dicaments sans ordonnance sur internet: Cialis sans ordonnance 24h – Pharmacie en ligne fiable
Pharmacies en ligne certifiГ©es: Pharmacie en ligne pas cher – Pharmacie en ligne livraison gratuite
https://pharmadoc.pro/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne livraison rapide: pharmacie en ligne pas cher – Acheter mГ©dicaments sans ordonnance sur internet
http://viagrasansordonnance.pro/# Viagra en france livraison rapide
Viagra femme ou trouver [url=https://viagrasansordonnance.pro/#]Viagra gГ©nГ©rique pas cher livraison rapide[/url] Viagra vente libre allemagne
Viagra homme sans ordonnance belgique [url=https://viagrasansordonnance.pro/#]viagra sans ordonnance[/url] Le gГ©nГ©rique de Viagra
pharmacie ouverte: PharmaDoc.pro – Pharmacie en ligne fiable
http://viagrasansordonnance.pro/# Acheter viagra en ligne livraison 24h
Pharmacie en ligne fiable
https://cialissansordonnance.shop/# Acheter médicaments sans ordonnance sur internet
Pharmacie en ligne sans ordonnance [url=https://pharmadoc.pro/#]pharmacie en ligne[/url] acheter mГ©dicaments Г l’Г©tranger
Acheter mГ©dicaments sans ordonnance sur internet: PharmaDoc – pharmacie ouverte 24/24
Viagra Pfizer sans ordonnance: Acheter du Viagra sans ordonnance – Acheter Sildenafil 100mg sans ordonnance
https://viagrasansordonnance.pro/# Viagra gГ©nГ©rique sans ordonnance en pharmacie
Pharmacie en ligne sans ordonnance [url=https://cialissansordonnance.shop/#]cialis prix[/url] acheter medicament a l etranger sans ordonnance
http://levitrasansordonnance.pro/# Pharmacie en ligne fiable
Pharmacie en ligne livraison rapide [url=http://acheterkamagra.pro/#]kamagra gel[/url] Pharmacies en ligne certifiГ©es
Viagra femme ou trouver Le gГ©nГ©rique de Viagra or <a href=" http://weinlexikon.net/info.php?a%5B%5D=cheap+cialis “>Viagra sans ordonnance livraison 48h
https://edesk.jp/atp/Redirect.do?url=https://viagrasansordonnance.pro/ Viagra sans ordonnance 24h suisse
[url=https://maps.google.co.il/url?sa=t&url=https://viagrasansordonnance.pro]Le gГ©nГ©rique de Viagra[/url] Viagra femme sans ordonnance 24h and [url=http://80tt1.com/home.php?mod=space&uid=342169]Viagra sans ordonnance pharmacie France[/url] SildГ©nafil 100 mg prix en pharmacie en France
Pharmacie en ligne livraison gratuite: Acheter mГ©dicaments sans ordonnance sur internet – Pharmacie en ligne pas cher
https://pharmadoc.pro/# Pharmacie en ligne sans ordonnance
Pharmacie en ligne livraison 24h: kamagra oral jelly – acheter mГ©dicaments Г l’Г©tranger
https://levitrasansordonnance.pro/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne sans ordonnance
http://cialissansordonnance.shop/# pharmacie ouverte
acheter medicament a l etranger sans ordonnance: Acheter Cialis – Pharmacie en ligne fiable
modokicase.com
강력한 팀은 수많은 사람들의 추측 속에서 천천히 움직였습니다.
http://blog.assortedgarbage.com/?redirect=http%3A%2F%2Fanomaxx.com%2F&wptouch_switch=mobile
Pharmacie en ligne pas cher: Pharmacies en ligne certifiees – Pharmacie en ligne livraison gratuite
https://acheterkamagra.pro/# Pharmacie en ligne livraison rapide
Pharmacies en ligne certifiГ©es [url=http://pharmadoc.pro/#]PharmaDoc[/url] Pharmacie en ligne fiable
Acheter mГ©dicaments sans ordonnance sur internet [url=http://cialissansordonnance.shop/#]cialis prix[/url] Pharmacie en ligne livraison gratuite
http://levitrasansordonnance.pro/# Pharmacie en ligne fiable
Pharmacie en ligne sans ordonnance: cialis sans ordonnance – Pharmacie en ligne fiable
Viagra femme ou trouver: Viagra sans ordonnance 24h – Viagra homme prix en pharmacie sans ordonnance
http://cialissansordonnance.shop/# Pharmacie en ligne livraison rapide
acheter medicament a l etranger sans ordonnance [url=http://levitrasansordonnance.pro/#]Levitra acheter[/url] acheter medicament a l etranger sans ordonnance
세계 시장에 다양한 테마의 슬롯을 제공하는 250개 이상의 게임으로 구성된 프라그마틱 플레이의 슬롯 포트폴리오를 즐겨보세요.
프라그마틱 슬롯
프라그마틱 콘텐츠 항상 기대돼요! 또한 제 사이트에서도 유용한 정보를 제공하고 있어요. 상호 교류하며 더 많은 지식을 얻어가요!
https://okgasda.weebly.com/
https://spinner44.com/
https://plus-toto.com/
socialmediatric.com
Fang Jifan은 이빨을 드러 냈습니다. 이 세상은 정말 이상합니다.
https://azithromycin.bid/# can you buy zithromax over the counter in canada
buy zithromax 1000mg online: zithromax order online uk – zithromax capsules australia
buy generic clomid without rx: how to buy clomid price – can you buy generic clomid without prescription
https://amoxicillin.bid/# amoxicillin cost australia
amruthaborewells.com
“즉시…즉시 왕세자에게 넘어가라…팡지판…”
prednisone without rx [url=https://prednisonetablets.shop/#]buy prednisone 40 mg[/url] prednisone 40 mg daily
prednisone best prices: prednisone for sale – prednisone 20mg online
https://amoxicillin.bid/# amoxicillin 800 mg price
zithromax 500 mg lowest price pharmacy online: buy azithromycin zithromax – zithromax online
https://clomiphene.icu/# clomid for sale
amoxicillin 500mg tablets price in india [url=https://amoxicillin.bid/#]amoxicillin 500mg capsules uk[/url] amoxicillin 500mg capsules antibiotic
stromectol online canada: ivermectin stromectol – ivermectin 6mg tablet for lice
prednisone 60 mg prednisone 10 mg brand name or 40 mg prednisone pill
http://mychatik.ru/go.php?url=http://prednisonetablets.shop buy prednisone nz
[url=http://charitiesbuyinggroup.com/membersearch.aspx?returnurl=http://prednisonetablets.shop]canine prednisone 5mg no prescription[/url] prednisone 20mg capsule and [url=http://xunshang.cc/home.php?mod=space&uid=4497569]prednisone 20 mg pill[/url] prednisone 20mg nz
prednisone cost 10mg: prednisone 2 5 mg – prednisone 30 mg daily
https://clomiphene.icu/# can you get generic clomid online
http://clomiphene.icu/# get cheap clomid without a prescription
buy amoxicillin online cheap [url=http://amoxicillin.bid/#]buy amoxicillin online uk[/url] can i buy amoxicillin over the counter in australia
zithromax buy online no prescription: zithromax generic price – zithromax buy online
https://ivermectin.store/# stromectol online pharmacy
can i purchase generic clomid: can i buy clomid without rx – cheap clomid without insurance
https://amoxicillin.bid/# generic for amoxicillin
ivermectin usa price ivermectin price or ivermectin generic cream
https://clients1.google.tt/url?q=https://ivermectin.store ivermectin 3mg tab
[url=https://wiki.ood.ch/api.php?action=https://ivermectin.store]ivermectin 200 mcg[/url] ivermectin 6 mg tablets and [url=http://ckxken.synology.me/discuz/home.php?mod=space&uid=6016]stromectol brand[/url] stromectol tablets buy online
zithromax buy: zithromax prescription online – cheap zithromax pills
buy zithromax 1000mg online [url=http://azithromycin.bid/#]zithromax 250 mg pill[/url] buy cheap zithromax online
http://prednisonetablets.shop/# 30mg prednisone
prednisone 5093: prednisone 10mg cost – prednisone 20 mg tablet
amoxicillin medicine: generic amoxicillin over the counter – buy amoxicillin without prescription
prednisone 12 mg [url=http://prednisonetablets.shop/#]prednisone 20 mg tablets coupon[/url] order prednisone with mastercard debit
https://clomiphene.icu/# cost generic clomid no prescription
how much is amoxicillin: amoxicillin azithromycin – amoxicillin 500 mg without a prescription
http://amoxicillin.bid/# amoxicillin 500mg prescription
http://azithromycin.bid/# zithromax 1000 mg online
can i get generic clomid without prescription [url=http://clomiphene.icu/#]cheap clomid without rx[/url] cost of clomid without insurance
amoxicillin for sale amoxicillin 500mg capsules antibiotic or buy amoxicillin online no prescription
https://images.google.sh/url?q=https://azithromycin.bid amoxicillin cost australia
[url=https://cse.google.com.cu/url?sa=t&url=https://azithromycin.bid]how to get amoxicillin[/url] amoxicillin 200 mg tablet and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3050956]buy amoxicillin 500mg[/url] amoxil generic
cost generic clomid without a prescription: how to get clomid without rx – generic clomid pills
ivermectin online ivermectin 1 or ivermectin 3
https://www.google.com.tj/url?q=https://ivermectin.store ivermectin 3 mg
[url=https://images.google.com.pr/url?q=https://ivermectin.store]purchase oral ivermectin[/url] stromectol buy uk and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=117834]stromectol ivermectin 3 mg[/url] ivermectin 8000 mcg
prednisone 2.5 tablet: how can i get prednisone online without a prescription – fast shipping prednisone
amoxicillin 500 amoxicillin order online or medicine amoxicillin 500
https://maps.google.co.za/url?q=https://amoxicillin.bid buy amoxicillin 500mg usa
[url=https://cse.google.dj/url?q=https://amoxicillin.bid]generic amoxil 500 mg[/url] purchase amoxicillin 500 mg and [url=http://www.donggoudi.com/home.php?mod=space&uid=67239]buy amoxicillin online with paypal[/url] amoxicillin 500 mg tablet
where to get zithromax: buy zithromax without prescription online – zithromax over the counter uk
https://amoxicillin.bid/# amoxicillin 500mg capsule
drug prices prednisone prednisone 5mg capsules or prednisone online paypal
http://prime50plus.co.uk/site-redirect.php?bannerid=137&redirectlink=https://prednisonetablets.shop prednisone buy no prescription
[url=http://www.webclap.com/php/jump.php?url=http://prednisonetablets.shop]generic prednisone 10mg[/url] how can i order prednisone and [url=http://bbs.94kk.net/home.php?mod=space&uid=8812236]prednisone 50 mg buy[/url] prednisone purchase canada
https://clomiphene.icu/# how can i get clomid without a prescription
stromectol without prescription: ivermectin oral 0 8 – stromectol in canada
can i buy cheap clomid price [url=http://clomiphene.icu/#]order generic clomid prices[/url] where to buy generic clomid pills
Your blog is a goldmine of information. So glad I found it!
ремонт стульев [url=https://peretyazhka-mebeli-minsk.ru/]https://peretyazhka-mebeli-minsk.ru/[/url].
saungsantoso.com
Wang Shouren은 천천히 활을 당기며 “모두 나를 따르십시오. “라고 말했습니다.
Your passion for the subject shines through in every post. It’s contagious!
online shopping pharmacy india: Online medicine home delivery – online pharmacy india indianpharm.store
https://mexicanpharm.shop/# buying prescription drugs in mexico online mexicanpharm.shop
top online pharmacy india: order medicine from india to usa – top 10 online pharmacy in india indianpharm.store
https://indianpharm.store/# buy prescription drugs from india indianpharm.store
canada drug pharmacy [url=http://canadianpharm.store/#]Canada Pharmacy online[/url] canadian pharmacy ltd canadianpharm.store
canadian pharmacies online: Licensed Online Pharmacy – canadian pharmacy ratings canadianpharm.store
canadian pharmacy 24: Pharmacies in Canada that ship to the US – reputable canadian online pharmacy canadianpharm.store
http://mexicanpharm.shop/# best mexican online pharmacies mexicanpharm.shop
mexico drug stores pharmacies [url=http://mexicanpharm.shop/#]Online Mexican pharmacy[/url] medication from mexico pharmacy mexicanpharm.shop
mexican mail order pharmacies medication from mexico pharmacy or mexico drug stores pharmacies
https://www.google.fi/url?q=https://mexicanpharm.shop mexican drugstore online
[url=https://www.google.com.om/url?sa=t&url=https://mexicanpharm.shop]best online pharmacies in mexico[/url] mexican online pharmacies prescription drugs and [url=https://forexzloty.pl/members/352687-lbixvbtzuq]medication from mexico pharmacy[/url] п»їbest mexican online pharmacies
Your insights on this are really ahead of the curve.
Online medicine home delivery: reputable indian pharmacies – world pharmacy india indianpharm.store
https://indianpharm.store/# best online pharmacy india indianpharm.store
[url=https://rybelsus.party/]wegovy canada[/url]
doeaccforum.com
Fang Jifan은 어색하게 말했습니다. “노파가 어느 고등학교에서 왔는지 모르겠어요?”
mexico pharmacies prescription drugs [url=https://mexicanpharm.shop/#]Online Mexican pharmacy[/url] mexico pharmacy mexicanpharm.shop
india online pharmacy: Indian pharmacy to USA – cheapest online pharmacy india indianpharm.store
iGaming 업계에서 리딩되는 프라그마틱 게임은 모바일 중심의 혁신적이고 표준화된 콘텐츠를 제공합니다.
프라그마틱 무료
프라그마틱의 게임은 높은 퀄리티와 흥미진진한 스토리로 항상 눈길을 끌어요. 이번에 어떤 게임을 즐겼나요?
http://www.iavstudios.com/
https://www.dinotri.com
https://www.citizendentalclinic.com
legitimate canadian pharmacy online: canadian world pharmacy – reputable canadian online pharmacy canadianpharm.store
https://canadianpharm.store/# pharmacy in canada canadianpharm.store
Обратившись к нашей компании, вы гарантируете себе доступ к профессиональных юридических консультаций от квалифицированных юристов. Узнайте больше на нашем сайте по ссылке
[url=https://kioski.by/blog/pomoshh-yurista/zakonodatelnye-trebovaniya-i-sroki-zameny-schetchikov-elektroenergii.html]счетчик это прибор[/url].
canadian pharmacy best canadian pharmacy to order from or best canadian online pharmacy
https://www.google.is/url?sa=t&url=https://canadianpharm.store canadian neighbor pharmacy
[url=https://www.iexprofs.nl/go/14940/link.aspx?url=http://canadianpharm.store]reliable canadian pharmacy reviews[/url] canadianpharmacy com and [url=https://masterbationtube.com/user/rhthlfkswr/videos]legitimate canadian pharmacy online[/url] best canadian online pharmacy reviews
canadian pharmacy prices: Canada Pharmacy online – canadian pharmacy scam canadianpharm.store
http://mexicanpharm.shop/# mexican border pharmacies shipping to usa mexicanpharm.shop
mexican rx online: mexican mail order pharmacies – medication from mexico pharmacy mexicanpharm.shop
indian pharmacy paypal [url=http://indianpharm.store/#]international medicine delivery from india[/url] top online pharmacy india indianpharm.store
http://indianpharm.store/# online shopping pharmacy india indianpharm.store
mexico pharmacies prescription drugs: best online pharmacies in mexico – mexican online pharmacies prescription drugs mexicanpharm.shop
http://mexicanpharm.shop/# mexico pharmacies prescription drugs mexicanpharm.shop
best canadian online pharmacy [url=https://canadianpharm.store/#]Best Canadian online pharmacy[/url] canadian pharmacy ltd canadianpharm.store
cheapest online pharmacy india: Indian pharmacy to USA – india online pharmacy indianpharm.store
buying prescription drugs in mexico online: Certified Pharmacy from Mexico – best online pharmacies in mexico mexicanpharm.shop
http://mexicanpharm.shop/# reputable mexican pharmacies online mexicanpharm.shop
cheapest pharmacy canada: Pharmacies in Canada that ship to the US – canadian drugstore online canadianpharm.store
canadian pharmacy king: Licensed Online Pharmacy – canadapharmacyonline canadianpharm.store
canadian pharmacy ratings canadian online pharmacy or adderall canadian pharmacy
https://maps.google.lu/url?q=https://canadianpharm.store canadian pharmacy 24h com safe
[url=https://maps.google.vu/url?sa=t&url=https://canadianpharm.store]certified canadian international pharmacy[/url] legit canadian pharmacy and [url=https://www.foodntours.com/user/uopirmpcmz/videos]canadian pharmacies compare[/url] canadapharmacyonline legit
indian pharmacy paypal [url=http://indianpharm.store/#]Indian pharmacy to USA[/url] buy prescription drugs from india indianpharm.store
https://indianpharm.store/# indian pharmacy indianpharm.store
https://indianpharm.store/# top 10 online pharmacy in india indianpharm.store
medication from mexico pharmacy: Certified Pharmacy from Mexico – mexican pharmacy mexicanpharm.shop
canada pharmacy 24h buy drugs from canada or buy prescription drugs from canada cheap
https://www.agu-web.jp/~pharmacy1/feed2js/feed2js.php?src=http://canadianpharm.store canada drugs online
[url=http://www.hogwarts.be/frame.php?url=https://canadianpharm.store]legitimate canadian pharmacies[/url] canada pharmacy 24h and [url=http://www.dbgjjs.com/home.php?mod=space&uid=445583]ed drugs online from canada[/url] canadian online pharmacy reviews
Online medicine home delivery [url=https://indianpharm.store/#]order medicine from india to usa[/url] best india pharmacy indianpharm.store
mexico drug stores pharmacies best online pharmacies in mexico or <a href=" http://www.gnu-darwin.org/www001/src/ports/www/b2evolution/work/b2evolution/blogs/install/phpinfo.php?a%5B%5D=buy+generic+viagra “>best online pharmacies in mexico
https://cse.google.com.ph/url?sa=t&url=https://mexicanpharm.shop mexico pharmacies prescription drugs
[url=https://www.adminer.org/redirect/?url=https://mexicanpharm.shop]reputable mexican pharmacies online[/url] best online pharmacies in mexico and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9484834]mexican online pharmacies prescription drugs[/url] mexican pharmaceuticals online
https://mexicanpharm.shop/# buying from online mexican pharmacy mexicanpharm.shop
my canadian pharmacy: Canadian Pharmacy – canadian pharmacies compare canadianpharm.store
indian pharmacy online: indian pharmacy – best online pharmacy india indianpharm.store
canadian discount pharmacy [url=https://canadianpharm.store/#]Pharmacies in Canada that ship to the US[/url] best canadian pharmacy to buy from canadianpharm.store
canadian drug prices: Canadian International Pharmacy – canadian drug canadianpharm.store
indian pharmacy online: international medicine delivery from india – Online medicine home delivery indianpharm.store
canadian discount pharmacy best rated canadian pharmacy or pharmacy com canada
https://maps.google.gg/url?q=https://canadianpharm.store safe online pharmacies in canada
[url=https://www.google.com.sv/url?q=https://canadianpharm.store]canadian pharmacy cheap[/url] online canadian pharmacy and [url=http://web.symbol.rs/forum/member.php?action=profile&uid=491915]pharmacy rx world canada[/url] cheap canadian pharmacy
Обратившись к нашей компании, вы обеспечите себе получение профессиональных юридических консультаций от опытных специалистов. Подробнее читайте в статье по ссылке
[url=https://kioski.by/blog/pomoshh-yurista/lgoty-dlya-uchastnikov-boevyh-dejstvij-obzor-i-protsedura-polucheniya.html]оформление льгот ветеранам боевых действий[/url].
homefronttoheartland.com
젠장… 무슨 일이야, 젊은 스승님을 화나게 했어, 드디어 쫓겨날 거지?
https://canadianpharm.store/# the canadian drugstore canadianpharm.store
http://mexicanpharm.shop/# mexico drug stores pharmacies mexicanpharm.shop
mexican drugstore online: Certified Pharmacy from Mexico – mexican mail order pharmacies mexicanpharm.shop
pharmacy canadian superstore [url=https://canadianpharm.store/#]Canadian Pharmacy[/url] best canadian pharmacy to buy from canadianpharm.store
indian pharmacy online: Online medicine home delivery – india pharmacy indianpharm.store
http://mexicanpharm.shop/# best online pharmacies in mexico mexicanpharm.shop
reputable indian online pharmacy: international medicine delivery from india – cheapest online pharmacy india indianpharm.store
my canadian pharmacy reviews [url=https://canadianpharm.store/#]Canadian Pharmacy[/url] canadian pharmacy victoza canadianpharm.store
mail order pharmacy india indian pharmacy online or online pharmacy india
https://maps.google.bj/url?q=https://indianpharm.store best online pharmacy india
[url=https://maps.google.nu/url?q=https://indianpharm.store]indian pharmacies safe[/url] pharmacy website india and [url=https://lhgangguanwang.com/home.php?mod=space&uid=78628]indian pharmacy online[/url] india online pharmacy
프라그마틱 슬롯을 무료로 즐겨보며 행운을 시험해보세요.
프라그마틱 게임
프라그마틱 관련 정보 감사합니다! 제 사이트에서도 유용한 정보를 공유하고 있어요. 함께 소통하면서 발전하는 모습 기대합니다!
https://www.hotelsoftwarepro.com
https://www.ix9up70gi0.site
https://www.rubiconfc.com
online pharmacy without a prescription: perscription drugs without prescription – my canadian pharmacy viagra
http://canadadrugs.pro/# canada pharmacy not requiring prescription
legitimate canadian pharmacies [url=http://canadadrugs.pro/#]prescriptions canada[/url] global pharmacy plus canada
http://canadadrugs.pro/# pharmacy drugstore online
canadian pharmacies mail order: reliable mexican pharmacy – viagra 100mg canadian pharmacy
prescription price comparison [url=https://canadadrugs.pro/#]best canadian drug prices[/url] overseas no rx drugs online
legitimate canadian pharmacies online: drug canada – canada meds
canadian pharmacies list: canada pharmacy world – cheap canadian pharmacy
https://canadadrugs.pro/# canadian pharmacies list
canadian pharmacy usa [url=http://canadadrugs.pro/#]canada pharmacy[/url] canada drugs without prescription
online drugstore service canada: canadian pharmacy prices – list of mexican pharmacies
http://canadadrugs.pro/# mexican pharmacy online
safe canadian pharmacy prescription without a doctors prescription or internet pharmacy list
https://maps.google.li/url?q=https://canadadrugs.pro trust online pharmacy
[url=http://images.google.sr/url?q=https://canadadrugs.pro]recommended canadian pharmacies[/url] buy medicine canada and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1527075]giant discount pharmacy[/url] canadian drugstore reviews
Its such as you read my thoughts! You seem to understand a lot approximately this, such
as you wrote the guide in it or something. I think that you can do with a few p.c.
to force the message home a little bit, however instead of that,
that is excellent blog. A fantastic read. I will definitely be back.
drugs canada: no perscription drugs canada – most reliable canadian pharmacies
cheap rx drugs [url=http://canadadrugs.pro/#]perscription drugs without perscription[/url] online medications
canada drug online: foreign online pharmacy – canada pharmacies online prescriptions
online pharmacy mail order: no prescription canadian drugs – canadian pharmaceuticals online reviews
https://canadadrugs.pro/# overseas pharmacies online
katsluxury.com
날씨가 화창하니 아이들이 마당에서 야외에서 놀게 하세요.
https://maps.google.kz/url?q=https://www.pozitivit.com/
netovideo.com
그러나 사람의 마음속에 있는 탐욕은 여전히 제거할 수 없습니다.
mexican online pharmacies: family discount pharmacy – overseas pharmacies
canadian pharmacies without an rx [url=http://canadadrugs.pro/#]top rated canadian pharmacies online[/url] canadian medications
legal canadian prescription drugs online safe online pharmacies in canada or certified canadian online pharmacies
http://huber.ru/bitrix/rk.php?goto=http://canadadrugs.pro/ list of canada online pharmacies
[url=http://www.google.co.zm/url?q=https://canadadrugs.pro]highest discount on medicines online[/url] canadian drug companies and [url=http://wuyuebanzou.com/home.php?mod=space&uid=461980]online drugstore[/url] online canadian pharcharmy
https://canadadrugs.pro/# canada pharmacy online no prescription
licensed canadian pharmacies [url=https://canadadrugs.pro/#]canadian rx[/url] online pharmacy store
http://canadadrugs.pro/# most reputable canadian pharmacies
Инструкция по перетяжке дивана
перетяжка мебели тканью [url=https://peretyazhka-mebeli-vminske.ru/]https://peretyazhka-mebeli-vminske.ru/[/url] .
mexican pharmacy drugs: canada pharmacy online – cheap prescription drugs online
https://canadadrugs.pro/# recommended canadian online pharmacies
online pharmacy with no prescription: safe canadian online pharmacies – pharmacy online canada
modernkarachi.com
Zhu Houzhao는 즉시 “내 아들은 부끄럽고 내가 말한 것은 좋지 않습니다. “라고 말했습니다.
world pharmacy: prescription drug price check – pharmacy drug store
http://canadadrugs.pro/# online pharmacies without an rx
canada prescriptions [url=https://canadadrugs.pro/#]mexican pharmacy list[/url] mexican online pharmacies
canadian online pharmacy reviews: prescription without a doctor’s prescription – us online pharmacy
http://canadadrugs.pro/# no perscription drugs canada
[url=http://semaglutiderybelsus.online/]rybelsus weight loss[/url]
no 1 canadian pharcharmy online: online pharmacies – most trusted canadian online pharmacy
Как сэкономить на покупке новой мебели: перетяжка старой
перетяжка мебели в гродно [url=https://peretyazhka-mebeli-vminske.ru/]https://peretyazhka-mebeli-vminske.ru/[/url] .
pharmacy my canadian family pharmacy or drugs from canada with prescription
https://images.google.ms/url?sa=t&url=https://canadadrugs.pro mail order pharmacy canada
[url=https://www.google.me/url?q=https://canadadrugs.pro]certified canadian drug stores[/url] online pharmacy no peescription and [url=http://talk.dofun.cc/home.php?mod=space&uid=350686]bestpharmacyonline.com[/url] no prescription drugs canada
https://canadadrugs.pro/# best online pharmacy no prescription
list of trusted canadian pharmacies: discount drug store online shopping – prescription drug pricing
prescription drugs prices prescriptions from canada without or best online pharmacies without a script
https://maps.google.co.ls/url?q=https://canadadrugs.pro prescription drugs prices
[url=https://maps.google.bs/url?q=http://canadadrugs.pro]cheap prescription drugs[/url] drugs without a prescription and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=120584]mexican mail order pharmacy[/url] legitimate canadian mail order pharmacies
Новый внешний вид за один день: перетяжка мягкой мебели
ремонт мягкой мебели в минске [url=https://peretyazhka-mebeli-vminske.ru/]https://peretyazhka-mebeli-vminske.ru/[/url] .
mail order drug store: best canadian online pharmacy reviews – canadian mail order pharmacy reviews
https://canadadrugs.pro/# online pharmacy no prescription necessary
https://canadadrugs.pro/# best online pharmacy without prescription
canadian prescriptions [url=http://canadadrugs.pro/#]canada prescription drugs[/url] pharmacy drugstore online
online pharmacy without precriptions: buy mexican drugs online – canadian pharmaceuticals online safe
http://canadadrugs.pro/# discount prescription drugs online
internet pharmacy list: online pharmacy reviews – canada pharmacy no prescription
혁신적이고 표준화된 콘텐츠를 제공하는 최신 프라그마틱 게임은 슬롯, 라이브 카지노, 빙고 등 다양한 제품을 지원합니다.
프라그마틱 슬롯 무료
프라그마틱에 대한 글 읽는 것이 정말 재미있었어요! 또한, 제 사이트에서도 프라그마틱과 관련된 정보를 공유하고 있어요. 함께 발전하며 더 많은 지식을 쌓아가요!
https://www.ahmethasimoglu.com
https://www.buytamoxifen.site
https://www.academygohari.com
I’m amazed by the depth and breadth of your knowledge. Thanks for sharing!
best rated canadian pharmacies: cheap medications – internet pharmacy list
canadian pharmacy online ship to usa canadian drug store prices or safe online pharmacy
in**@ap**********.com&from=bovecnet&status=0" rel="nofollow ugc">http://www.bovec.net/redirect.php?link=canadadrugs.pro&un=in**@ap**********.com&from=bovecnet&status=0 no prescription online pharmacy
[url=https://www.google.com.bn/url?q=https://canadadrugs.pro]online drugstore without prescription[/url] canadian pharmacy direct and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3056969]canadian drugs online pharmacy[/url] drug canada
http://canadadrugs.pro/# discount prescription drugs online
Get cash rewards with these games in Kenya today
online casino games that pay real money [url=https://realmoneygameskenya.com/]games that pay real money in kenya[/url] .
https://canadianinternationalpharmacy.pro/# best canadian pharmacy online
A masterpiece of writing! You’ve covered all bases with elegance.
best pill for ed: best ed treatment pills – best pill for ed
http://canadianinternationalpharmacy.pro/# canadian pharmacy meds
buy prescription drugs from india: best online pharmacy india – indian pharmacies safe
http://certifiedpharmacymexico.pro/# purple pharmacy mexico price list
canadian online drugs [url=http://canadianinternationalpharmacy.pro/#]canadapharmacyonline com[/url] canadian pharmacy 24 com
canadian pharmacy ed medications: canadian pharmacy reviews – pharmacy canadian superstore
http://canadianinternationalpharmacy.pro/# safe reliable canadian pharmacy
natural ed medications: pills for erection – best pills for ed
prescription drugs online without [url=http://edwithoutdoctorprescription.pro/#]ed pills without doctor prescription[/url] buy prescription drugs without doctor
http://medicinefromindia.store/# legitimate online pharmacies india
online canadian pharmacy reviews ed drugs online from canada or best canadian online pharmacy
https://www.google.com.bn/url?q=https://canadianinternationalpharmacy.pro canadian pharmacies that deliver to the us
[url=https://maps.google.com.lb/url?q=https://canadianinternationalpharmacy.pro]canadian neighbor pharmacy[/url] canadianpharmacymeds and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3060716]legitimate canadian pharmacy online[/url] best online canadian pharmacy
reputable canadian pharmacy: canadian pharmacy 24h com safe – canadian valley pharmacy
You have a unique perspective that I find incredibly valuable. Thank you for sharing.
best medication for ed [url=https://edpill.cheap/#]treatment for ed[/url] male ed pills
india pharmacy mail order Online medicine home delivery or online pharmacy india
http://nwspprs.com/?format=simple&action=shorturl&url=https://medicinefromindia.store indian pharmacies safe
[url=http://pachl.de/url?q=https://medicinefromindia.store::]indian pharmacy[/url] online shopping pharmacy india and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6758650]india pharmacy mail order[/url] cheapest online pharmacy india
male erection pills: top ed pills – medication for ed dysfunction
https://certifiedpharmacymexico.pro/# mexican online pharmacies prescription drugs
https://medicinefromindia.store/# indian pharmacy online
http://edpill.cheap/# natural ed medications
mexican rx online [url=http://certifiedpharmacymexico.pro/#]medication from mexico pharmacy[/url] buying prescription drugs in mexico online
현재 프라그마틱 게임은 iGaming에서 선도적이며 독창적이고 표준화된 콘텐츠를 제공하는 주요 제공 업체 중 하나입니다.
프라그마틱슬롯
프라그마틱 슬롯에 대한 설명 정말 감사합니다! 더불어, 제 사이트에서도 프라그마틱과 관련된 내용을 찾아보세요. 함께 발전하며 더 많은 지식을 얻어가요!
http://albuterolsulfate.site
https://www.sujanews.com
http://buydiclofenac.site
This post is a testament to your expertise and hard work. Thank you!
medications for ed: erectile dysfunction medications – ed medication
http://edpill.cheap/# best erectile dysfunction pills
mail order pharmacy india [url=http://medicinefromindia.store/#]indianpharmacy com[/url] top 10 online pharmacy in india
http://canadianinternationalpharmacy.pro/# canadian pharmacy in canada
pharmacy website india india pharmacy mail order or online shopping pharmacy india
https://images.google.com.au/url?q=https://medicinefromindia.store indian pharmacy paypal
[url=https://www.google.co.in/url?sa=t&url=https://medicinefromindia.store]п»їlegitimate online pharmacies india[/url] buy medicines online in india and [url=http://talk.dofun.cc/home.php?mod=space&uid=362261]Online medicine order[/url] india pharmacy mail order
viagra without doctor prescription: generic cialis without a doctor prescription – meds online without doctor prescription
canada pharmacy best canadian pharmacy to order from or canadian online pharmacy reviews
https://toolbarqueries.google.is/url?sa=i&url=https://canadianinternationalpharmacy.pro canada drugs online review
[url=http://www.yabuno.net/w3a/redirect.php?redirect=http://canadianinternationalpharmacy.pro]best rated canadian pharmacy[/url] online canadian pharmacy review and [url=http://talk.dofun.cc/home.php?mod=space&uid=362220]canadian pharmacy store[/url] canadian online pharmacy reviews
http://canadianinternationalpharmacy.pro/# canadian pharmacy world reviews
tadalafil without a doctor’s prescription [url=http://edwithoutdoctorprescription.pro/#]ed pills without doctor prescription[/url] non prescription ed pills
I’m impressed by your ability to convey such nuanced ideas with clarity.
http://canadianinternationalpharmacy.pro/# ed drugs online from canada
cheapest online pharmacy india [url=https://medicinefromindia.store/#]indian pharmacy online[/url] п»їlegitimate online pharmacies india
buy prescription drugs online legally: generic cialis without a doctor prescription – buy prescription drugs online
Online medicine order india pharmacy mail order or india online pharmacy
https://sauvetage-nyon.ch/link.php?client=Winterthur&url=https://medicinefromindia.store online shopping pharmacy india
[url=https://www.clickcritters.com/external_page.php?url=https://medicinefromindia.store]cheapest online pharmacy india[/url] online pharmacy india and [url=https://forex-bitcoin.com/members/326568-mlasnumear]indian pharmacy online[/url] india pharmacy
mexican pharmacy without prescription: ed pills without doctor prescription – ed meds online without doctor prescription
https://edpill.cheap/# online ed medications
http://canadianinternationalpharmacy.pro/# canadian pharmacy sarasota
Putin Interview Video Interview With Putin. Putin Carlson.
mexican rx online mexican mail order pharmacies or reputable mexican pharmacies online
http://kimaarkitektur.no/?URL=http://certifiedpharmacymexico.pro purple pharmacy mexico price list
[url=http://maps.google.to/url?q=http://certifiedpharmacymexico.pro]mexico drug stores pharmacies[/url] purple pharmacy mexico price list and [url=http://80tt1.com/home.php?mod=space&uid=405368]п»їbest mexican online pharmacies[/url] mexico drug stores pharmacies
saungsantoso.com
홍지황제는 기대에 찬 눈으로 그를 바라보았다.
buy prescription drugs from india [url=https://medicinefromindia.store/#]top online pharmacy india[/url] india pharmacy
kinoboomhd.com
결국 Fusi Beizhen도 Jiujiang Mansion의 불만을 진실하게보고했습니다.
http://edwithoutdoctorprescription.pro/# best ed pills non prescription
indian pharmacy top 10 online pharmacy in india or п»їlegitimate online pharmacies india
http://maps.google.com.sl/url?q=https://medicinefromindia.store india online pharmacy
[url=http://maps.google.com.bz/url?q=http://medicinefromindia.store]top 10 pharmacies in india[/url] buy medicines online in india and [url=https://visualchemy.gallery/forum/profile.php?id=3585794]online pharmacy india[/url] indian pharmacies safe
canadian world pharmacy [url=https://canadianinternationalpharmacy.pro/#]canadian pharmacy[/url] safe online pharmacies in canada
http://certifiedpharmacymexico.pro/# purple pharmacy mexico price list
northern pharmacy canada prescription drugs canada buy online or canadianpharmacyworld com
https://cse.google.tg/url?sa=t&url=https://canadianinternationalpharmacy.pro canadian pharmacies online
[url=http://webservices.icodes.co.uk/transfer2.php?location=https://canadianinternationalpharmacy.pro]canadian pharmacies[/url] best mail order pharmacy canada and [url=http://bbs.51pinzhi.cn/home.php?mod=space&uid=6758219]legal to buy prescription drugs from canada[/url] my canadian pharmacy rx
best treatment for ed: ed treatment drugs – ed remedies
http://certifiedpharmacymexico.pro/# buying from online mexican pharmacy
canadian pharmacy: canadian pharmacy price checker – northwest canadian pharmacy
http://edpill.cheap/# medication for ed dysfunction
pharmacies in mexico that ship to usa [url=https://certifiedpharmacymexico.pro/#]mexican mail order pharmacies[/url] buying prescription drugs in mexico online
http://medicinefromindia.store/# reputable indian online pharmacy
indianpharmacy com online pharmacy india or indian pharmacy
https://cse.google.ws/url?sa=t&url=https://medicinefromindia.store indian pharmacy
[url=https://clients1.google.ro/url?q=https://medicinefromindia.store]top online pharmacy india[/url] indian pharmacy paypal and [url=http://ckxken.synology.me/discuz/home.php?mod=space&uid=7200]mail order pharmacy india[/url] top 10 online pharmacy in india
Online medicine order [url=https://medicinefromindia.store/#]best india pharmacy[/url] india pharmacy
http://medicinefromindia.store/# best india pharmacy
trustworthy canadian pharmacy [url=https://canadianinternationalpharmacy.pro/#]northern pharmacy canada[/url] precription drugs from canada
buying drugs from canada: canadian pharmacy in canada – canadian pharmacy cheap
https://certifiedpharmacymexico.pro/# mexican online pharmacies prescription drugs
buying prescription drugs in mexico online: buying prescription drugs in mexico – mexican drugstore online
https://certifiedpharmacymexico.pro/# buying from online mexican pharmacy
world pharmacy india best online pharmacy india or online pharmacy india
https://cse.google.is/url?q=https://medicinefromindia.store india pharmacy
[url=http://ktcom.jp/redirect.php?u=http://medicinefromindia.store]mail order pharmacy india[/url] world pharmacy india and [url=https://masterbationtube.com/user/ycwqlwfiga/videos]indian pharmacy[/url] Online medicine home delivery
buy erection pills [url=http://edpill.cheap/#]best ed pills[/url] best treatment for ed
https://certifiedpharmacymexico.pro/# medication from mexico pharmacy
canadian world pharmacy best rated canadian pharmacy or canadian compounding pharmacy
http://www.google.cm/url?sa=i&rct=j&q=w4&source=images&cd=&cad=rja&uact=8&docid=IFutAwmU3vpbNM&tbnid=OFjjVOSMg9C9UM:://canadianinternationalpharmacy.pro/pages/about-us canadian online drugstore
[url=https://cse.google.com.my/url?sa=t&url=https://canadianinternationalpharmacy.pro]real canadian pharmacy[/url] canadian pharmacies compare and [url=http://www.yizlife.com/space-uid-243177.html]reputable canadian online pharmacies[/url] my canadian pharmacy rx
프라그마틱 슬롯으로 재미와 스릴을 만끽하세요.
http://www.pragmatic-game.com
프라그마틱의 게임은 언제나 풍부한 그래픽과 흥미진진한 플레이로 유명해요. 이번에 새로운 게임이 나왔나요?
https://www.pzdig.com
https://www.bellarel.com
http://buycymbalta.site
New customers claim the best bonuses for casino players in Michigan. We have listed Michigan online casinos offer in collaboration with the Michigan online casino industry. Here is how new customers can get the biggest and best casino offers including Michigan casino no deposit bonuses. Use these tricks and hacks not just as a new customer but also as an existing customer of different sites. This website is using a security service to protect itself from online attacks. The action you just performed triggered the security solution. There are several actions that could trigger this block including submitting a certain word or phrase, a SQL command or malformed data. The games you are able to play using a no deposit bonus depends on two factors: the no deposit casino you’ve signed up for, as well as the type of no deposit bonus you’ve been allocated.
http://paxtonmxmf326.theglensecret.com/caesars-slots-777-to-new-zealand-dollar
Claiming a casino welcome bonus varies from one casino to another, and in most cases you are given the option to accept or decline the bonus when you make your deposit. Some will require that you enter a bonus code, which is a sequence of letters and or numbers, and in most cases the bonus codes are advertised in the promotion. Here at No Deposit Casinos 247 we display the latest casino bonuses in all of our reviews. $30 free upon registration is up for grabs with the Bally Casino promo code INQUIRERMAX, a strong amount when compared with other no-deposit casino offers. Sloto Cash welcomes its new players with a staggering $7,777 worth of welcome bonuses and 300 free spins on 5 of the most popular slot games in its casino library. You only need to make a deposit of $20 to claim this bonus. The wagering requirement is only 25x, which is significantly lower than what other bonuses on our list have to offer.
http://canadianinternationalpharmacy.pro/# canadian drugs pharmacy
indian pharmacy online [url=https://medicinefromindia.store/#]indianpharmacy com[/url] cheapest online pharmacy india
mexico drug stores pharmacies purple pharmacy mexico price list or purple pharmacy mexico price list
http://www.gaxclan.de/url?q=https://certifiedpharmacymexico.pro mexico drug stores pharmacies
[url=http://alfachat.ru/exit.php?linkurl=certifiedpharmacymexico.pro]buying prescription drugs in mexico online[/url] medication from mexico pharmacy and [url=http://bbs.jhqxml.com/home.php?mod=space&uid=5796]buying from online mexican pharmacy[/url] buying prescription drugs in mexico
best online pharmacy india indian pharmacy online or indian pharmacy
http://images.google.mw/url?q=https://medicinefromindia.store india pharmacy
[url=http://www.garrisonexcelsior.com/redirect.php?url=http://medicinefromindia.store]cheapest online pharmacy india[/url] п»їlegitimate online pharmacies india and [url=https://98e.fun/space-uid-7112510.html]top 10 online pharmacy in india[/url] buy prescription drugs from india
mexico pharmacies prescription drugs: mexico pharmacies prescription drugs – mexican drugstore online
https://certifiedpharmacymexico.pro/# purple pharmacy mexico price list
http://edwithoutdoctorprescription.pro/# viagra without doctor prescription
mexico pharmacy [url=https://certifiedpharmacymexico.pro/#]mexico pharmacy[/url] pharmacies in mexico that ship to usa
generic viagra without a doctor prescription: ed pills without doctor prescription – buy prescription drugs online legally
http://medicinefromindia.store/# indian pharmacies safe
naturally like your website however you need to take a look at the spelling on several of your posts. Many of them are rife with spelling problems and I to find it very troublesome to tell the reality on the other hand I will certainly come again again.
http://edwithoutdoctorprescription.pro/# prescription drugs online without doctor
canada drugs reviews [url=https://canadianinternationalpharmacy.pro/#]canadian drug prices[/url] adderall canadian pharmacy
Достигни права управления автомобилем в лучшей автошколе!
Стремись к профессиональной карьере автолюбителя с нашей автошколой!
Пройди обучение в самой автошколе города!
Учись правильного вождения с нашей автошколой!
Стань безупречным навыкам вождения с нашей автошколой!
Научись уверенно водить автомобиль у нас в автошколе!
Стремись к независимости и лицензии, получив права в автошколе!
Прояви мастерство вождения в нашей автошколе!
Открой новые возможности, получив права в автошколе!
Запиши друзей и они получат скидку на обучение в автошколе!
Стремись к профессиональному будущему в автомобильном мире с нашей автошколой!
Учись и научись водить автомобиль вместе с нашей автошколой!
Развивай свои навыки вождения вместе с опытными инструкторами нашей автошколы!
Закажи обучение в автошколе и получи бесплатный консультационный урок от наших инструкторов!
Достигни надежности и безопасности на дороге вместе с нашей автошколой!
Улучши свои навыки вождения вместе с лучшими в нашей автошколе!
Завоевывай дорожные правила и навыки вождения в нашей автошколе!
Стремись к настоящим мастером вождения с нашей автошколой!
Набери опыт вождения и получи права в нашей автошколе!
Пробей дорогу вместе с нами – закажи обучение в автошколе!
авто школи [url=https://www.avtoshkolaznit.kiev.ua/]https://www.avtoshkolaznit.kiev.ua/[/url] .
reputable indian online pharmacy reputable indian pharmacies or india pharmacy
https://www.abc-iwaki.com/jump?url=https://medicinefromindia.store::: top 10 online pharmacy in india
[url=http://chat.4ixa.ru/index.php?url=medicinefromindia.store&ver=html]india online pharmacy[/url] best online pharmacy india and [url=http://talk.dofun.cc/home.php?mod=space&uid=363456]world pharmacy india[/url] online shopping pharmacy india
http://certifiedpharmacymexico.pro/# purple pharmacy mexico price list
buy prescription drugs without doctor [url=https://edwithoutdoctorprescription.pro/#]tadalafil without a doctor’s prescription[/url] viagra without doctor prescription
buying prescription drugs in mexico online: mexican mail order pharmacies – mexican online pharmacies prescription drugs
https://canadianinternationalpharmacy.pro/# buying from canadian pharmacies
homefronttoheartland.com
이미 많은 상인들이 류씨 일가의 안내서에 주목하기 시작했다.
reputable canadian pharmacy canada pharmacy 24h or pet meds without vet prescription canada
https://campus.tdea.edu.co/cas/logout?url=https://canadianinternationalpharmacy.pro pharmacy canadian
[url=http://sharjahcityguide.com/main/advertise.asp?oldurl=http://canadianinternationalpharmacy.pro]canada rx pharmacy[/url] canadian pharmacy ed medications and [url=https://lhgangguanwang.com/home.php?mod=space&uid=86942]canada online pharmacy[/url] canadian pharmacy no scripts
https://medicinefromindia.store/# indian pharmacies safe
프라그마틱플레이의 슬롯으로 도전과 흥미를 느껴보세요.
프라그마틱 플레이
프라그마틱의 게임은 언제나 풍부한 그래픽과 흥미진진한 플레이로 유명해요. 이번에 새로운 게임이 나왔나요?
https://www.jeffklee.com
https://www.tunebreaker.com
https://www.bairpools.com
ed treatment drugs: medications for ed – online ed medications
10yenharwichport.com
Wang Shouren은 한동안 아무 말도하지 않고 신음하며 문제의 어려움을 저울질하는 것처럼 매우 침착했습니다.
baseballoutsider.com
Shen Ao의 마음 속에서 고정관념은 돼지를 먹이고 땅을 경작하는 것과 같습니다.
best online pharmacies in mexico buying from online mexican pharmacy buying prescription drugs in mexico online
reputable mexican pharmacies online mexican pharmacy mexican rx online
https://mexicanph.com/# pharmacies in mexico that ship to usa
mexican online pharmacies prescription drugs [url=https://mexicanph.com/#]mexican online pharmacies prescription drugs[/url] mexican pharmaceuticals online
purple pharmacy mexico price list [url=http://mexicanph.com/#]п»їbest mexican online pharmacies[/url] mexican pharmaceuticals online
mexican pharmaceuticals online mexican rx online mexico drug stores pharmacies
buying from online mexican pharmacy [url=http://mexicanph.shop/#]best online pharmacies in mexico[/url] mexico drug stores pharmacies
buying prescription drugs in mexico mexican rx online mexican pharmacy
mexican online pharmacies prescription drugs [url=http://mexicanph.com/#]mexican rx online[/url] mexican pharmacy
best online pharmacies in mexico buying from online mexican pharmacy п»їbest mexican online pharmacies
mexico drug stores pharmacies [url=http://mexicanph.shop/#]medication from mexico pharmacy[/url] mexican pharmaceuticals online
mexican online pharmacies prescription drugs [url=https://mexicanph.shop/#]mexico pharmacy[/url] п»їbest mexican online pharmacies
Спокусливий пін ап
казіно ігри [url=pinupcasinoqgcvbisd.kiev.ua]pinupcasinoqgcvbisd.kiev.ua[/url] .
https://mexicanph.com/# reputable mexican pharmacies online
mexican mail order pharmacies [url=https://mexicanph.com/#]buying prescription drugs in mexico online[/url] mexican border pharmacies shipping to usa
medication from mexico pharmacy [url=http://mexicanph.com/#]mexican rx online[/url] mexico pharmacies prescription drugs
mexican drugstore online mexican rx online or medication from mexico pharmacy
http://www.elienai.de/url?q=https://mexicanph.shop best online pharmacies in mexico
[url=https://www.google.gy/url?q=https://mexicanph.shop]best online pharmacies in mexico[/url] reputable mexican pharmacies online and [url=http://www.xjkou.com/home.php?mod=space&uid=21962]mexican pharmaceuticals online[/url] reputable mexican pharmacies online
mexico drug stores pharmacies buying from online mexican pharmacy or п»їbest mexican online pharmacies
http://wiki.wlug.org.nz/~matt/m.php?a%5B%5D=%3Ca%20href%3Dhttp%3A%2F%2Fmexicanph.com%2F%3E%C3%91%C5%8D%C3%90%C2%BB%C3%90%C2%B5%C3%90%C2%BA%C3%91%E2%80%9A%C3%91%E2%82%AC%C3%90%C2%BE%C3%91%81%C3%90%C2%BD%C3%90%C2%B0%C3%90%C2%B1%C3%90%C2%B6%C3%90%C2%B5%C3%90%C2%BD%C3%90%C2%B8%C3%90%C2%B5%20%C3%91%83%C3%91%E2%80%A1%C3%90%C2%B0%C3%91%81%C3%91%E2%80%9A%C3%90%C2%BA%C3%90%C2%B0%20%C3%91%E2%80%A0%C3%90%C2%B5%C3%91%E2%80%A6%C3%90%C2%B0%20%C3%90%C2%B4%C3%90%C2%B8%C3%90%C2%BF%C3%90%C2%BB%C3%90%C2%BE%C3%90%C2%BC%3C%2Fa%3E mexico drug stores pharmacies
[url=http://yar-net.ru/go/?url=https://mexicanph.com]mexico drug stores pharmacies[/url] mexican drugstore online and [url=http://www.0551gay.com/space-uid-70455.html]buying prescription drugs in mexico online[/url] mexican pharmaceuticals online
mexico drug stores pharmacies buying prescription drugs in mexico or medication from mexico pharmacy
https://images.google.ch/url?sa=t&url=https://mexicanph.shop mexican drugstore online
[url=https://images.google.com.do/url?sa=t&url=https://mexicanph.shop]mexico drug stores pharmacies[/url] medication from mexico pharmacy and [url=http://seafishzone.com/home.php?mod=space&uid=1210841]purple pharmacy mexico price list[/url] mexico pharmacies prescription drugs
mexican online pharmacies prescription drugs [url=http://mexicanph.com/#]buying prescription drugs in mexico[/url] best online pharmacies in mexico
https://mexicanph.com/# medication from mexico pharmacy
medicine in mexico pharmacies
pharmacies in mexico that ship to usa purple pharmacy mexico price list or mexican border pharmacies shipping to usa
https://images.google.ca/url?q=https://mexicanph.com mexican rx online
[url=http://cse.google.com.my/url?sa=t&url=https://mexicanph.com]mexican rx online[/url] buying prescription drugs in mexico and [url=http://pufa.chemapao.cn/home.php?mod=space&uid=306772]mexico drug stores pharmacies[/url] mexican drugstore online
Идеальная смесь для ремонта
цена кирпичной кладки [url=https://www.remontnaja-smes-dlja-kirpichnoj-kladki.ru]https://www.remontnaja-smes-dlja-kirpichnoj-kladki.ru[/url] .
reputable mexican pharmacies online [url=https://mexicanph.com/#]mexican drugstore online[/url] mexican drugstore online
pharmacies in mexico that ship to usa buying prescription drugs in mexico online buying from online mexican pharmacy
mexican rx online mexican pharmacy mexican drugstore online
Рулонный газон: где купить качественный материал?
рулонный газон москва [url=https://rulonnyj-gazon77.ru/]https://rulonnyj-gazon77.ru/[/url] .
buying prescription drugs in mexico online mexican drugstore online or reputable mexican pharmacies online
https://lehrter.reisen/redirect/index.asp?url=http://mexicanph.shop mexico drug stores pharmacies
[url=http://www.m-bp.jp/bookmark.html?tu_id=yoga-gllow&u=http://mexicanph.shop]best online pharmacies in mexico[/url] mexican pharmacy and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=3324526]medicine in mexico pharmacies[/url] mexico drug stores pharmacies
medication from mexico pharmacy best online pharmacies in mexico or mexican border pharmacies shipping to usa
https://www.seelensturm.net/wcf/acp/dereferrer.php?url=http://mexicanph.com/ mexico pharmacies prescription drugs
[url=https://images.google.com.ai/url?sa=t&url=https://mexicanph.com]mexican drugstore online[/url] medication from mexico pharmacy and [url=http://yslit.com/home.php?mod=space&uid=616922]mexico pharmacy[/url] mexican pharmacy
https://mexicanph.shop/# mexican border pharmacies shipping to usa
mexican rx online [url=https://mexicanph.shop/#]mexico pharmacies prescription drugs[/url] mexican online pharmacies prescription drugs
reputable mexican pharmacies online [url=http://mexicanph.com/#]mexican rx online[/url] mexican border pharmacies shipping to usa
best online pharmacies in mexico mexican pharmacy medication from mexico pharmacy
mexican rx online [url=https://mexicanph.com/#]mexican drugstore online[/url] mexico pharmacies prescription drugs
[url=http://wegovy.best/]rybelsus buy australia[/url]
mexico drug stores pharmacies [url=https://mexicanph.com/#]mexican pharmacy[/url] mexican online pharmacies prescription drugs
mexico pharmacy medication from mexico pharmacy or medication from mexico pharmacy
https://images.google.mu/url?sa=t&url=https://mexicanph.com mexico pharmacy
[url=https://maps.google.com.tr/url?sa=t&url=https://mexicanph.com]reputable mexican pharmacies online[/url] mexico drug stores pharmacies and [url=http://pufa.chemapao.cn/home.php?mod=space&uid=306446]mexico drug stores pharmacies[/url] buying prescription drugs in mexico
mexico pharmacies prescription drugs buying prescription drugs in mexico mexican border pharmacies shipping to usa
mexico drug stores pharmacies mexico pharmacy п»їbest mexican online pharmacies
https://mexicanph.shop/# buying prescription drugs in mexico
medicine in mexico pharmacies [url=https://mexicanph.shop/#]medicine in mexico pharmacies[/url] best online pharmacies in mexico
restaurant-lenvol.net
Fang Jifan은 결국 매우 당황했습니다 … 모두가 자신을 유령으로 여겼습니다.
mexico drug stores pharmacies medicine in mexico pharmacies or buying prescription drugs in mexico
http://mycivil.ir/go/index.php?url=https://mexicanph.shop mexican rx online
[url=https://clients1.google.com.sl/url?q=https://mexicanph.shop]mexico pharmacies prescription drugs[/url] mexican pharmaceuticals online and [url=http://xunshang.cc/home.php?mod=space&uid=4536003]mexican pharmaceuticals online[/url] mexican online pharmacies prescription drugs
Доверь перетяжку мебели квалифицированным специалистам в Минске
перетяжка офисного кресла [url=https://peretyazhka-mebeli-vminske.ru/]https://peretyazhka-mebeli-vminske.ru/[/url] .
п»їbest mexican online pharmacies mexican rx online п»їbest mexican online pharmacies
mexican drugstore online mexican pharmaceuticals online mexican border pharmacies shipping to usa
buying from online mexican pharmacy [url=http://mexicanph.com/#]mexican rx online[/url] medicine in mexico pharmacies
pharmacies in mexico that ship to usa mexican drugstore online or medication from mexico pharmacy
http://feed2js.org/feed2js.php?src=http://mexicanph.com mexican pharmaceuticals online
[url=https://images.google.bf/url?sa=t&url=http://mexicanph.com]п»їbest mexican online pharmacies[/url] mexico pharmacy and [url=http://www.xjkou.com/home.php?mod=space&uid=21611]mexican mail order pharmacies[/url] buying from online mexican pharmacy
medicine in mexico pharmacies mexican online pharmacies prescription drugs mexican drugstore online
pharmacies in mexico that ship to usa mexico drug stores pharmacies medication from mexico pharmacy
best online pharmacies in mexico mexican rx online or medicine in mexico pharmacies
https://clients1.google.li/url?q=http://mexicanph.shop mexican mail order pharmacies
[url=http://www.patrick-bateman.com/url?q=https://mexicanph.shop]buying prescription drugs in mexico online[/url] reputable mexican pharmacies online and [url=https://fl.liaochengquan.cn/home.php?mod=space&uid=1145163]mexico drug stores pharmacies[/url] mexican online pharmacies prescription drugs
п»їbest mexican online pharmacies [url=https://mexicanph.shop/#]mexico drug stores pharmacies[/url] buying from online mexican pharmacy
best mexican online pharmacies mexican drugstore online mexican pharmaceuticals online
purple pharmacy mexico price list mexico pharmacy mexican online pharmacies prescription drugs
best online pharmacies in mexico mexican pharmacy mexican online pharmacies prescription drugs
mexico pharmacy buying prescription drugs in mexico online medicine in mexico pharmacies
buying from online mexican pharmacy [url=http://mexicanph.com/#]mexican pharmaceuticals online[/url] buying prescription drugs in mexico online
buying prescription drugs in mexico online purple pharmacy mexico price list reputable mexican pharmacies online
mexican border pharmacies shipping to usa reputable mexican pharmacies online or mexican mail order pharmacies
https://www.google.jo/url?q=https://mexicanph.com п»їbest mexican online pharmacies
[url=https://images.google.sh/url?q=https://mexicanph.com]mexican drugstore online[/url] medicine in mexico pharmacies and [url=https://103.94.185.62/home.php?mod=space&uid=8220]mexico drug stores pharmacies[/url] mexico pharmacies prescription drugs
mexican drugstore online pharmacies in mexico that ship to usa or reputable mexican pharmacies online
https://www.google.co.vi/url?q=https://mexicanph.com reputable mexican pharmacies online
[url=https://maps.google.bg/url?sa=t&url=https://mexicanph.com]best online pharmacies in mexico[/url] buying prescription drugs in mexico online and [url=http://pufa.chemapao.cn/home.php?mod=space&uid=306470]buying prescription drugs in mexico[/url] medication from mexico pharmacy
mexican pharmaceuticals online buying prescription drugs in mexico online mexico pharmacy
mexican pharmaceuticals online [url=https://mexicanph.com/#]mexico pharmacies prescription drugs[/url] mexican border pharmacies shipping to usa
best mexican online pharmacies buying prescription drugs in mexico online mexican border pharmacies shipping to usa
http://mexicanph.com/# mexican online pharmacies prescription drugs
mexican border pharmacies shipping to usa
mexican drugstore online п»їbest mexican online pharmacies mexican border pharmacies shipping to usa
medicine in mexico pharmacies п»їbest mexican online pharmacies purple pharmacy mexico price list
buying from online mexican pharmacy mexican rx online buying prescription drugs in mexico online
mexican online pharmacies prescription drugs [url=https://mexicanph.shop/#]medication from mexico pharmacy[/url] purple pharmacy mexico price list
mexico drug stores pharmacies medication from mexico pharmacy medication from mexico pharmacy
buying prescription drugs in mexico online mexican pharmaceuticals online or purple pharmacy mexico price list
http://www.elienai.de/url?q=https://mexicanph.com pharmacies in mexico that ship to usa
[url=http://ggeek.ru/bitrix/redirect.php?event1=&event2=&event3=&goto=https://mexicanph.com]mexico drug stores pharmacies[/url] mexican pharmaceuticals online and [url=http://wuyuebanzou.com/home.php?mod=space&uid=466845]pharmacies in mexico that ship to usa[/url] mexican online pharmacies prescription drugs
purple pharmacy mexico price list mexico pharmacy pharmacies in mexico that ship to usa
mexican online pharmacies prescription drugs [url=https://mexicanph.shop/#]buying prescription drugs in mexico online[/url] mexican drugstore online
mexican pharmacy pharmacies in mexico that ship to usa or mexico pharmacy
https://www.google.ie/url?sa=t&rct=j&q=&esrc=s&source=newssearch&cd=1&cad=rja&uact=8&ved=0CB8QqQIoADAA&url=https://mexicanph.shop medication from mexico pharmacy
[url=https://cse.google.lt/url?sa=t&url=https://mexicanph.shop]mexico drug stores pharmacies[/url] mexican online pharmacies prescription drugs and [url=http://talk.dofun.cc/home.php?mod=space&uid=387294]medication from mexico pharmacy[/url] best online pharmacies in mexico
buying prescription drugs in mexico online mexico pharmacies prescription drugs mexican pharmaceuticals online
buying from online mexican pharmacy purple pharmacy mexico price list mexico drug stores pharmacies
mexico drug stores pharmacies buying prescription drugs in mexico online mexico drug stores pharmacies
https://mexicanph.com/# mexican pharmaceuticals online
mexican pharmaceuticals online [url=http://mexicanph.com/#]п»їbest mexican online pharmacies[/url] mexico pharmacies prescription drugs
mexican border pharmacies shipping to usa [url=https://mexicanph.com/#]buying prescription drugs in mexico[/url] medicine in mexico pharmacies
reputable mexican pharmacies online buying prescription drugs in mexico online mexican pharmaceuticals online
mexico pharmacies prescription drugs medication from mexico pharmacy mexico drug stores pharmacies
http://mexicanph.com/# mexico drug stores pharmacies
mexican drugstore online
mexican pharmacy buying prescription drugs in mexico mexico drug stores pharmacies
medication from mexico pharmacy medication from mexico pharmacy or mexican border pharmacies shipping to usa
https://cse.google.co.ug/url?q=https://mexicanph.com medication from mexico pharmacy
[url=https://www.viva.com.bo/google/?n=00-23-f8-7b-6c-ef&host=http://mexicanph.com]medicine in mexico pharmacies[/url] mexican online pharmacies prescription drugs and [url=https://www.xiaoditech.com/bbs/home.php?mod=space&uid=1543879]mexican mail order pharmacies[/url] mexican border pharmacies shipping to usa
mexico drug stores pharmacies [url=https://mexicanph.com/#]medication from mexico pharmacy[/url] mexico drug stores pharmacies
mexican rx online mexican pharmacy mexican online pharmacies prescription drugs
purple pharmacy mexico price list medication from mexico pharmacy mexican border pharmacies shipping to usa
[url=https://ozempic.pics/]buy rybelsus from canada[/url]
mexican rx online mexican border pharmacies shipping to usa or medicine in mexico pharmacies
https://cse.google.rw/url?q=https://mexicanph.shop medicine in mexico pharmacies
[url=https://maps.google.rs/url?sa=t&url=https://mexicanph.shop]mexican mail order pharmacies[/url] mexican drugstore online and [url=https://www.foodntours.com/user/zhwbaljcqa/videos]mexican border pharmacies shipping to usa[/url] buying from online mexican pharmacy
medicine in mexico pharmacies mexico pharmacy mexico pharmacy
medication from mexico pharmacy [url=http://mexicanph.shop/#]mexican rx online[/url] buying prescription drugs in mexico online
buying from online mexican pharmacy [url=https://mexicanph.com/#]mexican border pharmacies shipping to usa[/url] buying prescription drugs in mexico online
https://mexicanph.com/# mexican rx online
buying prescription drugs in mexico
kinoboomhd.com
Shen Wen의 말은 칼처럼 Hongzhi 황제의 마음을 찔렀습니다!
buying from online mexican pharmacy medication from mexico pharmacy mexican pharmaceuticals online
reputable mexican pharmacies online mexican drugstore online or mexican drugstore online
http://vladinfo.ru/away.php?url=http://mexicanph.com mexican drugstore online
[url=http://906090.4-germany.de/tools/klick.php?curl=http://mexicanph.com]п»їbest mexican online pharmacies[/url] mexican rx online and [url=http://www.xjkou.com/home.php?mod=space&uid=21836]mexico drug stores pharmacies[/url] mexico drug stores pharmacies
buying from online mexican pharmacy buying prescription drugs in mexico mexican online pharmacies prescription drugs
medication from mexico pharmacy mexico pharmacy mexico drug stores pharmacies
buying prescription drugs in mexico mexico pharmacy best online pharmacies in mexico
mexican pharmaceuticals online medicine in mexico pharmacies or reputable mexican pharmacies online
http://tanganrss.com/rsstxt/cushion.php?url=mexicanph.com mexican drugstore online
[url=https://maps.google.com.sb/url?sa=t&rct=j&url=https://mexicanph.com]medication from mexico pharmacy[/url] mexico drug stores pharmacies and [url=https://forex-bitcoin.com/members/327713-tguodcizvs]best online pharmacies in mexico[/url] medicine in mexico pharmacies
pharmacies in mexico that ship to usa mexico pharmacies prescription drugs п»їbest mexican online pharmacies
mexican border pharmacies shipping to usa [url=http://mexicanph.com/#]mexican pharmaceuticals online[/url] medicine in mexico pharmacies
best online pharmacies in mexico pharmacies in mexico that ship to usa best mexican online pharmacies
https://resheniezadachmarketing.ru/
buying prescription drugs in mexico online mexico pharmacy pharmacies in mexico that ship to usa
mexican pharmaceuticals online reputable mexican pharmacies online mexico pharmacy
https://hudozhestvenny-perevod.ru/
buying from online mexican pharmacy mexican pharmaceuticals online mexican rx online
canadianpharmacy.com Canadian Pharcharmy Online
cheap viagra online canada pharmacy [url=http://canadianphrmacy23.com/]canadian rx pharmacy[/url]
https://mexicanph.com/# mexico drug stores pharmacies
п»їbest mexican online pharmacies [url=https://mexicanph.com/#]mexico pharmacies prescription drugs[/url] pharmacies in mexico that ship to usa
buying prescription drugs in mexico online mexico pharmacy or reputable mexican pharmacies online
https://www.google.cv/url?q=https://mexicanph.com buying prescription drugs in mexico
[url=https://images.google.ca/url?q=https://mexicanph.com]best online pharmacies in mexico[/url] п»їbest mexican online pharmacies and [url=http://www.coin520.com/home.php?mod=space&uid=14074]buying prescription drugs in mexico[/url] buying from online mexican pharmacy
best online pharmacies in mexico buying from online mexican pharmacy medicine in mexico pharmacies
mexico drug stores pharmacies mexico pharmacy medicine in mexico pharmacies
http://mexicanph.com/# mexico drug stores pharmacies
best online pharmacies in mexico
medication from mexico pharmacy pharmacies in mexico that ship to usa best mexican online pharmacies
buying from online mexican pharmacy best online pharmacies in mexico mexican rx online
saungsantoso.com
중생들은 전하가 침묵하는 것을 보았고 감히 아무 말도 하지 않았습니다.
lisinopril pills 2.5 mg: lisinopril otc – lisinopril 40mg prescription cost
furosemide 100 mg [url=https://furosemide.guru/#]furosemida 40 mg[/url] buy furosemide online
https://referatystatistika.ru/
http://stromectol.fun/# ivermectin uk coronavirus
furosemida 40 mg: Buy Lasix No Prescription – lasix tablet
[url=https://pin-up-casino-official-login.com/]pin-up-casino-official-login.com[/url]
Перепрыгнуть в течение являющийся личной собственностью кабинет. Нажать на кнопочку «Ящик». Определиться один-другой предпочтением подходящей системы, указать сумму депозита и еще оказать нажим «Дополнить». Система автоматически распахнет шлиф, кае что поделаешь уписать обстановка карты, на каковую хорэ изготовляться депозит.
Что можно вытворить с скидками в пин ап?
Чтоб вернуть бонус, игрок повинен совершить суперэкспресс ставки вместе с реального страх, превышающие сумму бонуса в течение 5 раз. В ТЕЧЕНИЕ чума ступают только «экспрессы» от 3-х событий с коэффициентами через 1.40 для любого события. Предусматриваются условия с ответвлений «Лайв» и еще «Линия».
pin-up-casino-official-login.com
http://stromectol.fun/# ivermectin price usa
혁신적이고 표준화된 모바일 중심의 콘텐츠를 제공하는 프라그마틱 게임은 iGaming 업계의 선도적인 제공 업체입니다.
프라그마틱 슬롯
프라그마틱은 항상 최고의 게임을 제공하죠! 여기에서 더 많은 흥미진진한 정보를 얻을 수 있어 기뻐요.
https://www.revelkid.com
https://www.s9winmy.com
https://www.xmcoart.com
https://furosemide.guru/# lasix 40 mg
where to buy ivermectin cream [url=https://stromectol.fun/#]cost of ivermectin pill[/url] stromectol ivermectin 3 mg
lasix for sale: lasix for sale – furosemide 40mg
http://stromectol.fun/# purchase stromectol
topical ivermectin cost: cost of ivermectin cream – price of stromectol
Bet on all your favorite sports at 1xBet
Win Big with 1xBet: The Top Sports Betting Platform
Experience the Excitement of Online Betting with 1xBet
Get in on the Action with 1xBet: The Best Sports Betting Site
Unleash Your Winning Potential with 1xBet
Bet and Win with Confidence at 1xBet
Join the 1xBet Community and Start Winning Today
The Ultimate Sports Betting Experience Awaits at 1xBet
1xBet: Where Champions Are Made
Take Your Betting to the Next Level with 1xBet
Get Ready to Win Big at 1xBet
Multiply Your Winnings with 1xBet’s Exciting Betting Options
Elevate Your Sports Betting Game with 1xBet
Sign Up for 1xBet and Start Winning Instantly
Experience the Thrill of Betting with 1xBet
1xBet: Your Ticket to Winning Big on Sports
Don’t Miss Out on the Action at 1xBet
Join 1xBet Today and Bet on Your Favorite Sports
Winning Has Never Been Easier with 1xBet
Get Started with 1xBet and Discover a World of Betting Opportunities
1xbet download [url=https://1xbet-app-download-ar.com/#1xbet-download]1xbet download[/url] .
Разобрать дом в Московской области
https://vstx.ru/
https://stromectol.fun/# ivermectin cream uk
lisinopril 10mg tablets price [url=http://lisinopril.top/#]generic zestril[/url] 10mg generic 10mg lisinopril
http://lisinopril.top/# lisinopril 2019
can i buy amoxicillin online: buy amoxicillin – generic amoxicillin over the counter
lasix generic name [url=https://furosemide.guru/#]Buy Lasix No Prescription[/url] generic lasix
lisinopril 10 mg 12.5mg: lisinopril cheap brand – rx lisinopril 10mg
https://stromectol.fun/# buy ivermectin for humans uk
20 mg of prednisone: prednisone cost 10mg – prednisone in mexico
lasix furosemide [url=https://furosemide.guru/#]Buy Lasix No Prescription[/url] lasix for sale
https://amoxil.cheap/# amoxicillin without a prescription
https://avidigital-spb.ru/
furosemide 40mg: generic lasix – buy furosemide online
zestril generic: zestril 2.5 mg tablets – 10 mg lisinopril tablets
https://amoxil.cheap/# where to get amoxicillin over the counter
lasix dosage [url=https://furosemide.guru/#]Buy Lasix[/url] lasix dosage
lasix medication lasix uses or furosemida 40 mg
http://www.amagin.jp/cgi-bin/acc/acc.cgi?REDIRECT=https://furosemide.guru lasix uses
[url=http://cse.google.ad/url?sa=t&url=http://furosemide.guru]buy lasix online[/url] furosemida and [url=http://203.195.186.190/space-uid-333577.html]furosemide 40mg[/url] furosemide
stromectol tablets uk [url=https://stromectol.fun/#]ivermectin 50mg/ml[/url] ivermectin 2%
http://amoxil.cheap/# amoxicillin canada price
furosemida 40 mg: generic lasix – lasix for sale
stromectol 3mg tablets: ivermectin uk – stromectol 3mg tablets
https://furosemide.guru/# lasix online
lasix 20 mg: Over The Counter Lasix – buy furosemide online
buy prednisone canadian pharmacy [url=http://buyprednisone.store/#]steroids prednisone for sale[/url] prednisone 20 mg without prescription
https://buyprednisone.store/# prednisone for sale without a prescription
stromectol in canada: where can i buy stromectol – stromectol covid 19
prednisone 1 mg daily 100 mg prednisone daily or prednisone 10mg canada
https://maps.google.sh/url?q=https://buyprednisone.store prednisone uk buy
[url=https://www.google.com.ar/url?sa=i&url=https://buyprednisone.store]order prednisone[/url] price for 15 prednisone and [url=https://forexzloty.pl/members/356050-chvywhaltb]prednisone in uk[/url] price of prednisone 5mg
http://lisinopril.top/# price of lisinopril 30 mg
lisinopril 10 mg over the counter [url=http://lisinopril.top/#]lisinopril in mexico[/url] lisinopril 40 mg no prescription
lisinopril 40 mg cost: lisinopril 10 mg pill – generic zestoretic
https://buyprednisone.store/# order prednisone 100g online without prescription
lasix [url=http://furosemide.guru/#]furosemide 40 mg[/url] lasix 100mg
lasix: Buy Lasix – lasix 40 mg
http://stromectol.fun/# ivermectin 1%
lasix uses lasix for sale or lasix furosemide
https://maps.google.com.do/url?sa=t&url=https://furosemide.guru lasix 40 mg
[url=http://www.wzdq.cc/go.php?url=http://furosemide.guru]lasix 40mg[/url] lasix medication and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3066661]furosemide 40mg[/url] lasix 100 mg tablet
amoxicillin 500mg capsule buy online: buy amoxicillin 500mg capsules uk – buy cheap amoxicillin
http://furosemide.guru/# lasix
lisinopril 10mg prices compare prescription medicine lisinopril or lisinopril 20 mg canadian pharmacy
https://register.transportscotland.gov.uk/subscribe/widgetsignup?url=http://lisinopril.top/ 208 lisinopril
[url=http://www.hyoito-fda.com/out.php?url=http://lisinopril.top]price of lisinopril[/url] buy lisinopril online usa and [url=https://www.ixbren.net/home.php?mod=space&uid=650693]lisinopril 60 mg daily[/url] zestoretic 20 25mg
order amoxicillin uk amoxicillin buy online canada or amoxicillin for sale
http://mensa.mymevis.org/xampp/phpinfo.php?a%5B%5D=sildenafil+coupons</a> amoxicillin generic
[url=https://maps.google.ht/url?q=https://amoxil.cheap]can we buy amoxcillin 500mg on ebay without prescription[/url] amoxicillin without a doctors prescription and [url=http://wnt1688.cn/home.php?mod=space&uid=7568369]amoxicillin 500mg buy online canada[/url] where can i buy amoxicillin online
https://best-santehnika.store/
buy lisinopril 20 mg online united states [url=http://lisinopril.top/#]order cheap lisinopril[/url] п»їbuy lisinopril 10 mg uk
http://amoxil.cheap/# can you buy amoxicillin uk
http://stromectol.fun/# ivermectin 200
where to get amoxicillin over the counter: amoxicillin 500mg capsules antibiotic – ampicillin amoxicillin
prednisone 10mg tabs: prednisone 20 – prednisone in mexico
http://furosemide.guru/# furosemide 40 mg
ivermectin lotion for scabies: buy ivermectin for humans australia – stromectol for head lice
ivermectin 0.08% [url=http://stromectol.fun/#]stromectol medication[/url] ivermectin over the counter uk
lfchungary.com
어떻게 말을 할 수 있는데 결국 일탈 지경에 이르렀습니까?
sm-casino1.com
이 대명궁은 여전히 웅장했지만 비바람이 몰아친 후에도 별반 다르지 않은 것 같았습니다.
https://amoxil.cheap/# amoxicillin 250 mg capsule
prednisone over the counter australia [url=http://buyprednisone.store/#]cost of prednisone in canada[/url] prednisone 7.5 mg
ivermectin buy canada: ivermectin 3 – ivermectin 200 mcg
lisinopril 5mg buy: lisinopril 5 mg tabs – zestril canada
https://buyprednisone.store/# generic prednisone 10mg
https://seo116.ru/
lasix 100mg lasix 100mg or lasix 100mg
https://www.google.tn/url?q=https://furosemide.guru lasix furosemide
[url=https://maps.google.gg/url?q=http://furosemide.guru]lasix furosemide 40 mg[/url] furosemide 100mg and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=126843]furosemide[/url] buy furosemide online
generic amoxicillin 500mg [url=http://amoxil.cheap/#]amoxicillin from canada[/url] buy amoxicillin canada
https://furosemide.guru/# buy furosemide online
lasix 100 mg: Buy Lasix No Prescription – furosemide 40 mg
[url=http://semaglutideozempic.com/]wegovy where to buy[/url]
프라그마틱 플레이의 슬롯 포트폴리오는 250개 이상의 게임으로 구성되어 있으며, 33개 언어와 다양한 화폐를 통해 전 세계 시장에 제공됩니다.
프라그마틱 무료
프라그마틱의 게임은 항상 최고 수준의 퀄리티를 유지하고 있어요. 이번에도 그런 훌륭한 게임을 만났나요?
https://www.buycelebrex.site
https://doggggqwe.weebly.com/
https://www.ashspurr.com
stromectol buy: ivermectin – ivermectin buy uk
http://buyprednisone.store/# prednisone 30
Услуга сноса старых частных домов и вывоза мусора в Москве и Подмосковье под ключ от нашей компании. Работаем в указанном регионе, предлагаем услугу демонтаж фундамента расценки. Наши тарифы ниже рыночных, а выполнение работ гарантируем в течение 24 часов. Бесплатно выезжаем для оценки и консультаций на объект. Звоните нам или оставляйте заявку на сайте для получения подробной информации и расчета стоимости услуг.
generic lisinopril 3973: buy lisinopril 20 mg no prescription – lisinopril 10 mg tablets price
amoxicillin script [url=https://amoxil.cheap/#]can we buy amoxcillin 500mg on ebay without prescription[/url] can you buy amoxicillin uk
https://amoxil.cheap/# amoxil generic
hihouse420.com
Wen Yansheng은 아무렇지도 않게 말했습니다. “Cao Min은 폐하와 함께 두 잔 더 마실까요?”
prinivil brand name: lisinopril online canada – lisinopril mexico
https://amoxil.cheap/# amoxicillin 500mg price canada
lisinopril 5mg tabs [url=http://lisinopril.top/#]lisinopril generic brand[/url] lisinopril generic price comparison
https://furosemide.guru/# furosemide 40 mg
buy amoxicillin over the counter uk: amoxicillin 500mg price – where to buy amoxicillin 500mg
cortisol prednisone buy prednisone 10mg online or buy prednisone online fast shipping
https://www.adventurework.co.uk/extern.aspx?cu=93154&page=1&s=42&t=1&src=https://buyprednisone.store:: prednisone 60 mg price
[url=https://clients1.google.gy/url?q=https://buyprednisone.store]can you buy prednisone online uk[/url] where can you buy prednisone and [url=http://test.viczz.com/home.php?mod=space&uid=3372326]buy prednisone online usa[/url] buy 40 mg prednisone
lasix 40 mg [url=http://furosemide.guru/#]Buy Lasix[/url] furosemide 100 mg
https://lisinopril.top/# lisinopril prescription coupon
lisinopril 20mg online: lisinopril medication otc – prinivil 10 mg tablet
furosemide furosemide 100mg or lasix 40mg
http://dvd24online.de/url?q=https://furosemide.guru lasix for sale
[url=http://winkler-sandrini.it/info/mwst01i.pdf?a[]=places+to+buy+viagra+online]lasix generic name[/url] lasix 100mg and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=3357330]generic lasix[/url] lasix for sale
https://amoxil.cheap/# canadian pharmacy amoxicillin
amoxicillin 775 mg: where can i buy amoxicillin without prec – amoxicillin 200 mg tablet
buy amoxicillin 500mg online: amoxicillin 500mg cost – buy amoxicillin without prescription
prednisone 1mg purchase [url=https://buyprednisone.store/#]prednisone pharmacy[/url] prednisone 20mg prices
http://buyprednisone.store/# buy prednisone 10mg online
lisinopril pill 10mg lisinopril uk or buy lisinopril 2.5 mg
http://mx.taskmanagementsoft.com/bitrix/redirect.php?goto=https://lisinopril.top:: cheapest price for lisinopril
[url=https://maps.google.com.do/url?q=https://lisinopril.top]lisinopril 420[/url] lisinopril cost uk and [url=http://yslit.com/home.php?mod=space&uid=619527]lisinopril tabs 40mg[/url] lisinopril 10mg tablets
buy amoxicillin 500mg online price for amoxicillin 875 mg or where can you buy amoxicillin over the counter
https://www.klickerkids.de/index.php?url=http://amoxil.cheap amoxicillin 500mg capsules price
[url=http://cse.google.com.et/url?sa=t&url=http://amoxil.cheap]amoxicillin 875 mg tablet[/url] amoxicillin script and [url=http://pufa.chemapao.cn/home.php?mod=space&uid=310775]generic amoxicillin 500mg[/url] amoxicillin 250 mg capsule
restaurant-lenvol.net
“맞아요, 하녀도 동창에게서 소식을 듣고 폐하께 보고하려 합니다.”
https://flashsaleprop.com/
https://furosemide.guru/# furosemide 40mg
lasix online: lasix 100mg – generic lasix
https://furosemide.guru/# lasix furosemide 40 mg
minocycline 50mg online [url=https://stromectol.fun/#]stromectol price[/url] minocycline capsule
https://amoxil.cheap/# generic amoxil 500 mg
zestoretic cost [url=https://lisinopril.top/#]order lisinopril online united states[/url] lisinopril online prescription
prednisone 30 mg coupon: prednisone 2.5 mg – prednisone for sale without a prescription
amoxicillin capsules 250mg: buy amoxicillin online uk – amoxicillin capsule 500mg price
https://amoxil.cheap/# generic amoxil 500 mg
buy lasix online furosemide or lasix dosage
https://clients1.google.com.eg/url?q=https://furosemide.guru furosemide 100mg
[url=https://image.google.com.sl/url?q=https://furosemide.guru]furosemide[/url] lasix 40mg and [url=https://98e.fun/space-uid-7137174.html]lasix uses[/url] generic lasix
5mg prednisone: buy prednisone mexico – prescription prednisone cost
https://amoxil.cheap/# amoxicillin 500 mg
https://stromectol.fun/# ivermectin 3mg pill
https://hidehost.net/
amoxicillin 500 mg tablet price [url=https://amoxil.cheap/#]amoxicillin order online[/url] how to buy amoxycillin
prednisone tabs 20 mg: prednisone 20 mg tablets coupon – prednisone tablet 100 mg
http://buyprednisone.store/# prednisone 40 mg tablet
заказать продвижение сайта seo
lasix uses: Buy Lasix No Prescription – lasix side effects
https://lisinopril.top/# lisinopril 60 mg
lasix for sale [url=https://furosemide.guru/#]buy lasix online[/url] lasix for sale
https://hidehost.net/
http://lisinopril.top/# generic drug for lisinopril
lisinopril 40mg [url=http://lisinopril.top/#]purchase lisinopril 10 mg[/url] lisinopril 5 mg pill
stromectol ivermectin tablets: stromectol canada – ivermectin 5 mg
pragmatic-ko.com
Deng Jian은 실제로 Wang Bushi를 매우 존경했습니다.
https://buyprednisone.store/# prednisone without prescription.net
Незабываемые впечатления для всей семьи
– Турция без визы: турция туроператор
подбор тура онлайн [url=https://anex-tour-turkey.ru]https://anex-tour-turkey.ru[/url] .
northwestpharmacy .com one-time offer
canadian pharmacies without a prescription [url=http://canadianphrmacy23.com/]visit the site[/url]
Отпуск мечты: туры в Турцию
подбор тура [url=https://tez-tour-turkey.ru]https://tez-tour-turkey.ru[/url] .
smcasino-game.com
“청나라가 말해도 괜찮습니다.” 홍지황제가 부드럽게 웃었다.
colorful-navi.com
“Ma Butang은 보고서를 먼저 읽어야 합니다. 결국 비즈니스 문제입니다.”
https://clients1.google.ee/url?q=https%3A%2F%2Fwww.colorful-navi.com%2F
продвижение профессиональное сайтов
프라그마틱플레이의 슬롯으로 다양한 게임을 경험하세요.
프라그마틱 슬롯 체험
프라그마틱의 무료 게임 옵션은 정말로 흥미진진한데요. 어떤 무료 게임을 추천하시나요?
https://www.komps.site
https://www.utahppr.com
https://www.vamiveta.com/
reputable indian pharmacies top online pharmacy india indian pharmacy
indian pharmacies safe buy medicines online in india Online medicine home delivery
https://indianph.xyz/# online pharmacy india
buy medicines online in india
https://hidehost.net/
http://indianph.com/# cheapest online pharmacy india
Online medicine order
top 10 online pharmacy in india buy prescription drugs from india or pharmacy website india
http://ewin.biz/jsonp/?url=https://indianph.com:: mail order pharmacy india
[url=https://images.google.li/url?q=https://indianph.com]online pharmacy india[/url] indianpharmacy com and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9712054]world pharmacy india[/url] best india pharmacy
buy prescription drugs from india [url=https://indianph.com/#]indian pharmacy[/url] best india pharmacy
pragmatic-ko.com
그는 Fang Jifan을 응시했습니다. “새로운 학습, 그것을 만지작 거리는 것은 당신이었습니다.”
http://indianph.com/# world pharmacy india
https://indianph.xyz/# top online pharmacy india
india pharmacy mail order
Грузоперевозки для частных лиц
перевозки по харькову [url=http://www.moving-company-kharkov.com.ua/]http://www.moving-company-kharkov.com.ua/[/url] .
https://indianph.com/# mail order pharmacy india
Online medicine home delivery
india pharmacy mail order pharmacy india top online pharmacy india
https://indianph.xyz/# indian pharmacy
п»їlegitimate online pharmacies india [url=http://indianph.xyz/#]indian pharmacy online[/url] top 10 pharmacies in india
indian pharmacy paypal [url=https://indianph.com/#]indian pharmacy online[/url] indianpharmacy com
[url=https://yachtrentalsnirof.com]https://yachtrentalsnirof.com[/url]
A neighbourhood to approach prices to go to renting yachts, sailboats, catamarans around the world and rip your yacht cheaper.
http://www.yachtrentalsnirof.com
http://indianph.com/# top 10 pharmacies in india
india pharmacy mail order
http://indianph.com/# top 10 pharmacies in india
top 10 online pharmacy in india
https://beckom.ru/
buy medicines online in india reputable indian online pharmacy or india pharmacy mail order
https://www.google.com.ar/url?q=https://indianph.xyz indianpharmacy com
[url=http://images.google.mk/url?q=https://indianph.xyz]indian pharmacies safe[/url] buy medicines online in india and [url=https://www.warshipsfaq.ru/user/xpgfzkskvc]best india pharmacy[/url] india online pharmacy
http://indianph.xyz/# top online pharmacy india
indian pharmacy paypal
https://seolinkedin.ru/
india online pharmacy [url=http://indianph.xyz/#]best india pharmacy[/url] india pharmacy mail order
https://indianph.xyz/# mail order pharmacy india
reputable indian pharmacies
Online medicine home delivery india pharmacy mail order mail order pharmacy india
indian pharmacy indian pharmacy or Online medicine order
https://image.google.com.sb/url?q=https://indianph.com cheapest online pharmacy india
[url=http://images.google.com.ai/url?q=https://indianph.com]reputable indian online pharmacy[/url] cheapest online pharmacy india and [url=http://80tt1.com/home.php?mod=space&uid=496442]best india pharmacy[/url] top 10 online pharmacy in india
https://indianph.com/# reputable indian pharmacies
indian pharmacies safe
Забудьте о низких позициях в поиске! Наше SEO продвижение https://seopoiskovye.ru/ под ключ выведет ваш сайт на вершины Google и Yandex. Анализ конкурентов, глубокая оптимизация, качественные ссылки — всё для вашего бизнеса. Получите поток целевых клиентов уже сегодня!
Забудьте о низких позициях в поиске! Наше SEO продвижение и оптимизация на заказ https://seosistemy.ru/ выведут ваш сайт в топ, увеличивая его видимость и привлекая потенциальных клиентов. Индивидуальный подход, глубокий анализ ключевых слов, качественное наполнение контентом — мы сделаем всё, чтобы ваш бизнес процветал.
Нове обладнання для будівництва
купити спецтехніку [url=http://www.spectehnika-sksteh.co.ua/]http://www.spectehnika-sksteh.co.ua/[/url] .
pragmatic-ko.com
이 한 입 가득 돼지 도살 요리는 당신의 식욕에 정말 잘 맞습니다.
Подробное руководство
10. Установка кондиционера: детальное описание процесса
кондиционер mitsubishi [url=https://ustanovit-kondicioner.ru]https://ustanovit-kondicioner.ru[/url] .
Дайте вашему сайту заслуженное место в топе поисковых систем! Наши услуги seo заказать на заказ обеспечат максимальную видимость вашего бизнеса в интернете. Персонализированные стратегии, тщательный подбор ключевых слов, оптимизация контента и технические улучшения — всё это для привлечения целевой аудитории и увеличения продаж. Вместе мы поднимем ваш сайт на новый уровень успеха!
10 способов продвижения строительных услуг
продвижение строительных услуг [url=https://seo-prodvizhenie-sajtov-stroitelnyh-kompanij.ru/]https://seo-prodvizhenie-sajtov-stroitelnyh-kompanij.ru/[/url] .
Дайте вашему сайту заслуженное место в топе поисковых систем! Наши услуги seo продвижение сайта сколько стоит на заказ обеспечат максимальную видимость вашего бизнеса в интернете. Персонализированные стратегии, тщательный подбор ключевых слов, оптимизация контента и технические улучшения — всё это для привлечения целевой аудитории и увеличения продаж. Вместе мы поднимем ваш сайт на новый уровень успеха!
Loving the information on this website , you have done outstanding job on the articles.
Дайте вашему сайту заслуженное место в топе поисковых систем! Наши услуги yandex продвижение сайта на заказ обеспечат максимальную видимость вашего бизнеса в интернете. Персонализированные стратегии, тщательный подбор ключевых слов, оптимизация контента и технические улучшения — всё это для привлечения целевой аудитории и увеличения продаж. Вместе мы поднимем ваш сайт на новый уровень успеха!
http://cytotec24.com/# purchase cytotec
buy cytotec: buy cytotec pills – buy cytotec online fast delivery
purchase cytotec [url=https://cytotec24.com/#]buy cytotec over the counter[/url] buy cytotec over the counter
프라그마틱 게임은 iGaming 분야에서 주목받는 주요 제공 업체로, 독창적이고 표준화된 콘텐츠를 제공합니다.
프라그마틱 게임
프라그마틱 슬롯에 대한 내용이 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 찾아보세요. 함께 서로 이야기하며 더 많은 지식을 쌓아가요!
https://www.komps.site
https://www.salasaredu.com
https://www.buycipro.site
doxycycline without prescription: doxycycline vibramycin – buy doxycycline online uk
http://cipro.guru/# where can i buy cipro online
https://doxycycline.auction/# doxycycline monohydrate
buy ciprofloxacin: buy cipro cheap – ciprofloxacin mail online
ciprofloxacin mail online cipro online no prescription in the usa or buy ciprofloxacin over the counter
https://asia.google.com/url?q=https://cipro.guru buy ciprofloxacin
[url=https://www.google.co.ve/url?q=http://cipro.guru]cipro pharmacy[/url] buy ciprofloxacin over the counter and [url=https://bbs.sanesoft.cn/home.php?mod=space&uid=145344]ciprofloxacin over the counter[/url] where can i buy cipro online
https://doxycycline.auction/# doxycycline 200 mg
smcasino-game.com
손을 등 뒤로 한 채 Zhu Houzhao는 Fang Jifan을 몰래 흘끗 보았습니다.
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara888.wordpress.com/
Good luck!
https://cipro.guru/# purchase cipro
diflucan 150 mg otc [url=http://diflucan.pro/#]diflucan 125mg[/url] diflucan 1 where to buy
yangsfitness.com
검사관이 있기 때문에 모든 공무원이 훨씬 더 정직합니다.
https://cytotec24.com/# cytotec pills online
tamoxifen alternatives premenopausal: what happens when you stop taking tamoxifen – nolvadex for pct
Распродажа кондиционеров в вашем городе
split система [url=https://prodazha-kondicionera.ru]https://prodazha-kondicionera.ru[/url] .
https://lechenie-bolezney.ru/
buy misoprostol over the counter cytotec online or Abortion pills online
http://nimbus.c9w.net/wifi_dest.html?dest_url=https://cytotec24.shop buy cytotec online fast delivery
[url=http://wx.lt/redirect.php?url=http://cytotec24.shop]Misoprostol 200 mg buy online[/url] buy cytotec in usa and [url=https://fl.liaochengquan.cn/home.php?mod=space&uid=1228633]Abortion pills online[/url] buy cytotec pills online cheap
diflucan 150 otc: diflucan over the counter nz – diflucan 100 mg tablet
https://diflucan.pro/# how to buy diflucan
Stomatologurmonsk Полезные советы для будущих мам
Почему важно регулярно посещать стоматолога?
[url=https://rekforum.ru/viewtopic.php?p=121992#p121992]https://rekforum.ru/viewtopic.php?p=121992#p121992[/url] .
https://diflucan.pro/# buy diflucan 1
order cytotec online [url=http://cytotec24.shop/#]buy cytotec online[/url] Abortion pills online
diflucan where to buy uk: how to buy diflucan – diflucan otc canada
https://nolvadex.guru/# tamoxifen and ovarian cancer
lfchungary.com
사실 처음에 팡지판의 사업은 모두 궁궐에 관련되어 있었다.
is nolvadex legal: tamoxifen hormone therapy – where to buy nolvadex
tamoxifen citrate [url=https://nolvadex.guru/#]nolvadex generic[/url] tamoxifen for men
http://doxycycline.auction/# doxylin
ciprofloxacin generic price: buy cipro online without prescription – ciprofloxacin mail online
http://cipro.guru/# cipro
cytotec pills buy online: buy cytotec – Cytotec 200mcg price
http://cytotec24.com/# buy cytotec in usa
order doxycycline 100mg without prescription [url=https://doxycycline.auction/#]doxycycline without prescription[/url] doxycycline 50 mg
doxycycline 150 mg doxycycline 100 mg or buy doxycycline online without prescription
https://cse.google.lv/url?q=https://doxycycline.auction doxylin
[url=https://maps.google.com.mx/url?q=https://doxycycline.auction]doxycycline[/url] doxy 200 and [url=http://wuyuebanzou.com/home.php?mod=space&uid=475361]buy doxycycline online 270 tabs[/url] buy doxycycline 100mg
http://diflucan.pro/# diflucan pill price
https://cytotec24.shop/# cytotec abortion pill
http://doxycycline.auction/# doxycycline pills
buy diflucan canada [url=http://diflucan.pro/#]diflucan buy online[/url] where can you buy diflucan over the counter
tamoxifen endometriosis: tamoxifen for breast cancer prevention – alternative to tamoxifen
http://cipro.guru/# purchase cipro
cipro online no prescription in the usa buy ciprofloxacin or buy generic ciprofloxacin
https://images.google.tk/url?sa=t&url=https://cipro.guru ciprofloxacin mail online
[url=https://www.google.com.ng/url?sa=t&url=https://cipro.guru]ciprofloxacin order online[/url] buy cipro online without prescription and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=85183]ciprofloxacin 500mg buy online[/url] buy cipro online without prescription
http://diflucan.pro/# diflucan daily
http://nolvadex.guru/# how to prevent hair loss while on tamoxifen
tamoxifen alternatives premenopausal [url=https://nolvadex.guru/#]where can i buy nolvadex[/url] tamoxifen for breast cancer prevention
lfchungary.com
Fang Jifan은 스스로 일을 할 수 있기 때문에 당연히 신경 쓰지 않습니다.
http://doxycycline.auction/# doxycycline 100mg dogs
cipro ciprofloxacin: cipro – ciprofloxacin
http://cytotec24.shop/# buy misoprostol over the counter
http://nolvadex.guru/# tamoxifen chemo
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara0006.wordpress.com/
Good luck!
ciprofloxacin mail online [url=http://cipro.guru/#]buy cipro online[/url] cipro
1. Где купить кондиционер: лучшие магазины и выбор
2. Как выбрать кондиционер: советы по покупке
3. Кондиционеры в наличии: где купить прямо сейчас
4. Купить кондиционер онлайн: удобство и выгодные цены
5. Кондиционеры для дома: какой выбрать и где купить
6. Лучшие предложения на кондиционеры: акции и распродажи
7. Кондиционер купить: сравнение цен и моделей
8. Кондиционеры с установкой: где купить и как установить
9. Где купить кондиционер с доставкой: быстро и надежно
10. Кондиционеры: где купить качественный товар по выгодной цене
11. Кондиционер купить: как выбрать оптимальную мощность
12. Кондиционеры для офиса: какой выбрать и где купить
13. Кондиционер купить: самый выгодный вариант
14. Кондиционеры в рассрочку: где купить и как оформить
15. Кондиционеры: лучшие магазины и предложения
16. Кондиционеры на распродаже: где купить по выгодной цене
17. Как выбрать кондиционер: советы перед покупкой
18. Кондиционер купить: где найти лучшие цены
19. Лучшие магазины кондиционеров: где купить качественный товар
20. Кондиционер купить: выбор из лучших моделей
ремонт кондиционера [url=http://www.kondicioner-cena.ru]http://www.kondicioner-cena.ru[/url] .
http://sweetiefox.online/# Sweetie Fox
eva elfie filmleri: eva elfie izle – eva elfie modeli
http://abelladanger.online/# abella danger video
sweety fox [url=http://sweetiefox.online/#]Sweetie Fox[/url] Sweetie Fox izle
tamoxifen [url=http://nolvadex.guru/#]does tamoxifen make you tired[/url] nolvadex during cycle
http://lanarhoades.fun/# lana rhoades video
Советы
19. Как купить хостинг с SSL-сертификатом для безопасности
бесплатный домен и хостинг [url=https://www.kish-host.ru]https://www.kish-host.ru[/url] .
eva elfie video: eva elfie izle – eva elfie izle
http://angelawhite.pro/# Angela White
https://abelladanger.online/# Abella Danger
lana rhodes [url=https://lanarhoades.fun/#]lana rhodes[/url] lana rhoades izle
https://lanarhoades.fun/# lana rhoades
https://angelawhite.pro/# Angela White filmleri
Angela White filmleri: ?????? ???? – Angela White video
http://sweetiefox.online/# Sweetie Fox modeli
Sweetie Fox izle: swetie fox – sweeti fox
https://abelladanger.online/# Abella Danger
http://angelawhite.pro/# Angela White
Angela White filmleri [url=https://angelawhite.pro/#]?????? ????[/url] Angela White
http://sweetiefox.online/# Sweetie Fox izle
http://abelladanger.online/# Abella Danger
프라그마틱의 게임은 항상 최고 수준의 퀄리티를 유지하고 있어요. 이번에도 그런 훌륭한 게임을 만났나요?
http://www.pragmatic-game.net
프라그마틱 슬롯에 대한 내용이 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 찾아보세요. 함께 서로 이야기하며 더 많은 지식을 쌓아가요!
https://www.rmchorseshoeranch.com
http://keoghsflex.com/
https://www.ccgwarehouse.com
?????? ????: abella danger video – abella danger filmleri
pragmatic-ko.com
아시다시피 천연두는 한 번 감염되면 면역력이 생깁니다.
https://lanarhoades.fun/# lana rhoades video
http://abelladanger.online/# abella danger izle
http://lanarhoades.fun/# lana rhoades video
eva elfie video [url=https://evaelfie.pro/#]eva elfie filmleri[/url] eva elfie modeli
dota2answers.com
이 말을 듣고 Li Zheng은 재빨리 “나의 황제 만세! “라고 고함을 질렀습니다.
lana rhoades video: lana rhodes – lana rhoades modeli
https://abelladanger.online/# abella danger izle
Перетяжка мягкой мебели
[url=https://fabnews.ru/forum/showthread.php?p=53490]https://fabnews.ru/forum/showthread.php?p=53490[/url] .
?????? ????: Angela Beyaz modeli – ?????? ????
http://abelladanger.online/# abella danger filmleri
http://lanarhoades.fun/# lana rhoades filmleri
https://evaelfie.pro/# eva elfie
Sweetie Fox izle [url=https://sweetiefox.online/#]Sweetie Fox izle[/url] sweeti fox
http://abelladanger.online/# abella danger filmleri
Angela Beyaz modeli: Angela Beyaz modeli – Angela White filmleri
https://angelawhite.pro/# Angela White izle
https://o-tendencii.com/
https://sweetiefox.online/# sweeti fox
http://abelladanger.online/# Abella Danger
https://hitech24.pro/
eva elfie modeli: eva elfie izle – eva elfie video
https://angelawhite.pro/# Angela White video
Abella Danger [url=http://abelladanger.online/#]abella danger video[/url] abella danger filmleri
http://abelladanger.online/# abella danger izle
http://abelladanger.online/# Abella Danger
eva elfie video: eva elfie – eva elfie video
eva elfie modeli: eva elfie izle – eva elfie izle
https://evaelfie.pro/# eva elfie
Sweetie Fox video Sweetie Fox filmleri or sweety fox
https://www.google.ms/url?sa=t&url=https://sweetiefox.online Sweetie Fox filmleri
[url=https://images.google.cl/url?q=https://sweetiefox.online]swetie fox[/url] Sweetie Fox video and [url=http://skiindustry.org:/forum/member.php?action=profile&uid=1153516]Sweetie Fox filmleri[/url] sweety fox
http://abelladanger.online/# abella danger izle
https://evaelfie.pro/# eva elfie
http://abelladanger.online/# abella danger video
Angela White: abella danger izle – abella danger filmleri
https://sweetiefox.online/# Sweetie Fox
lfchungary.com
이때 성벽을 수리하기에는 너무 늦었습니다.
Ремонт холодильников Атлант на дому: удобно и быстро!
цена ремонта холодильника атлант на дому [url=https://remont-holodilnikov-atlant.ru/]ремонт холодильников атлант[/url] .
https://gruzchikivesy.ru/
https://abelladanger.online/# abella danger izle
Angela White izle: Abella Danger – Abella Danger
Бонусы и акции в онлайн казино Беларусь: как получить выгоду
онлайн казино беларусь [url=https://onlinecasinobelarus.by/]онлайн казино беларусь[/url] .
https://evaelfie.pro/# eva elfie
laanabasis.com
Zhu Zaimo는 이유를 모르고 서둘러 “내 아들이 죽을 것입니다. “라고 절했습니다.
eva elfie modeli: eva elfie izle – eva elfie izle
http://evaelfie.pro/# eva elfie video
http://lanarhoades.fun/# lana rhoades modeli
Sweetie Fox [url=https://sweetiefox.online/#]Sweetie Fox video[/url] Sweetie Fox filmleri
https://sweetiefox.online/# sweeti fox
Sweetie Fox modeli: Sweetie Fox filmleri – swetie fox
https://evaelfie.pro/# eva elfie
Sweetie Fox modeli swetie fox or sweety fox
https://www.dead-donkey.com/scripts/index.php?https://sweetiefox.online/ Sweetie Fox modeli
[url=https://maps.google.la/url?rct=j&sa=t&url=https://sweetiefox.online]Sweetie Fox modeli[/url] swetie fox and [url=http://xilubbs.xclub.tw/space.php?uid=520447]Sweetie Fox filmleri[/url] Sweetie Fox izle
https://evaelfie.pro/# eva elfie modeli
http://evaelfie.pro/# eva elfie
lana rhodes lana rhoades filmleri or lana rhoades izle
https://www.google.co.zw/url?q=https://lanarhoades.fun lana rhoades izle
[url=https://clients1.google.com.kw/url?q=https://lanarhoades.fun]lana rhoades izle[/url] lana rhodes and [url=https://forexzloty.pl/members/358530-svrtkrnmou]lana rhoades modeli[/url] lana rhoades
[url=http://one-xbet-apk-fr.com]http://one-xbet-apk-fr.com[/url]
To log in, click the “Login” button on the official website of the bookmaker and put down your narcotic addict materials – enrol your email give a speech to and password.
http://one-xbet-apk-fr.com
http://lanarhoades.fun/# lana rhoades izle
lana rhoades [url=https://lanarhoades.fun/#]lana rhoades modeli[/url] lana rhoades modeli
https://o-tendencii.com/
http://angelawhite.pro/# Angela White filmleri
lana rhoades filmleri: lana rhoades filmleri – lana rhoades izle
http://lanarhoades.fun/# lana rhoades modeli
http://lanarhoades.fun/# lana rhoades filmleri
Angela White ?????? ???? or ?????? ????
https://www.chuchle.cz/?p=sendPageLink&value=https://angelawhite.pro:: Angela White video
[url=https://images.google.com.nf/url?q=http://angelawhite.pro]Angela Beyaz modeli[/url] Angela Beyaz modeli and [url=http://bbs.mycq3d.com/home.php?mod=space&uid=52664]Angela White izle[/url] Angela White
?????? ????: ?????? ???? – Angela White
Жены получат право вносить мужей-игроманов в черный список онлайн-казино Беларуси
https://gruzchikimeshki.ru/
https://gruzchikinochnoj.ru/
https://abelladanger.online/# abella danger izle
https://gruzchikiklub.ru/
https://gruzchikiperevozchik.ru/
eva elfie izle: eva elfie video – eva elfie
http://abelladanger.online/# abella danger izle
abella danger izle [url=http://abelladanger.online/#]abella danger izle[/url] abella danger video
http://evaelfie.pro/# eva elfie video
Sweetie Fox izle swetie fox or Sweetie Fox izle
http://rosieanimaladoption.ca/?URL=http://sweetiefox.online:: swetie fox
[url=https://maps.google.pn/url?q=https://sweetiefox.online]sweety fox[/url] sweeti fox and [url=http://seafishzone.com/home.php?mod=space&uid=1216250]Sweetie Fox filmleri[/url] sweeti fox
https://abelladanger.online/# Abella Danger
Angela Beyaz modeli: Angela White – Angela White filmleri
https://angelawhite.pro/# Angela White
https://gruzchikikar.ru/
sweetie fox new: sweetie fox new – fox sweetie
http://evaelfie.site/# eva elfie new video
https://evaelfie.site/# eva elfie full video
shopanho.com
사방에서 긴 칼을 휘두르는 사람들이 계속해서 명령을 반복했다.
eva elfie hot: eva elfie full videos – eva elfie new videos
http://lanarhoades.pro/# lana rhoades hot
lana rhoades solo [url=https://lanarhoades.pro/#]lana rhoades boyfriend[/url] lana rhoades boyfriend
https://gruzchikigastarbajter.ru/
eva elfie full videos: eva elfie full videos – eva elfie full video
smcasino7.com
양쪽에는 등이 튼튼하고 허리가 튼튼한 큰 한 장군이 있습니다.
https://gruzchikiperenosit.ru/
https://gruzchikiestakada.ru/
http://evaelfie.site/# eva elfie full videos
https://gruzchikimore.ru/
lana rhoades videos: lana rhoades hot – lana rhoades hot
https://miamalkova.life/# mia malkova photos
eva elfie full video [url=http://evaelfie.site/#]eva elfie[/url] eva elfie full video
https://gruzchikiustalost.ru/
[url=https://azithromycinmds.com/]order zithromax online[/url]
https://gruzchikikuzov.ru/
http://lanarhoades.pro/# lana rhoades unleashed
eva elfie hot: eva elfie new videos – eva elfie videos
https://gruzchikiperevozka.ru/
It’s a game. Five dollars is free. Try it It’s not an easy game
->-> 온라인카지노 .COM
mia malkova only fans: mia malkova new video – mia malkova full video
https://lanarhoades.pro/# lana rhoades solo
lana rhoades unleashed [url=http://lanarhoades.pro/#]lana rhoades unleashed[/url] lana rhoades videos
best dating apps: https://miamalkova.life/# mia malkova new video
crazy-slot1.com
이놈의 일은… 안심이 되지만 그의 말은 조금…
https://cse.google.com.ua/url?sa=i&url=https%3A%2F%2Fwww.colorful-navi.com%2F
Онлайн казино с быстрыми выплатами в Беларуси: безопасные транзакции
лучшие онлайн казино беларуси [url=https://onlinecasinobelarus.by/]лучшие онлайн казино беларуси[/url] .
mia malkova: mia malkova new video – mia malkova new video
https://sweetiefox.pro/# sweetie fox
https://miamalkova.life/# mia malkova new video
eva elfie: eva elfie new video – eva elfie hot
https://evaelfie.site/# eva elfie full videos
sweetie fox [url=https://sweetiefox.pro/#]ph sweetie fox[/url] sweetie fox full video
mia malkova only fans: mia malkova latest – mia malkova movie
mia malkova hd: mia malkova new video – mia malkova new video
https://miamalkova.life/# mia malkova girl
lana rhoades full video: lana rhoades – lana rhoades solo
dating sites for mature singles adults: http://evaelfie.site/# eva elfie hot
https://lanarhoades.pro/# lana rhoades boyfriend
lana rhoades full video: lana rhoades boyfriend – lana rhoades pics
Наша группа опытных специалистов подготовлена предлагать вам актуальные системы утепления, которые не только обеспечивают устойчивую оборону от зимы, но и преподнесут вашему коттеджу элегантный вид.
Мы функционируем с новыми компонентами, заверяя долгий период работы и блестящие результаты. Изолирование внешнего слоя – это не только экономия тепла на обогреве, но и заботливость о природной среде. Энергоспасающие технические средства, какие мы претворяем в жизнь, способствуют не только жилищу, но и сохранению природных ресурсов.
Самое важное: [url=https://ppu-prof.ru/]Отделка фасада с утеплением цена[/url] у нас начинается всего от 1250 рублей за квадратный метр! Это доступное решение, которое превратит ваш домашний уголок в фактический душевный уголок с минимальными затратами.
Наши достижения – это не просто теплоизоляция, это составление пространства, в где каждый компонент отражает ваш собственный образ. Мы примем все все твои просьбы, чтобы переделать ваш дом еще еще больше приятным и привлекательным.
Подробнее на [url=https://ppu-prof.ru/]http://ppu-prof.ru[/url]
Не откладывайте заботу о своем обители на потом! Обращайтесь к спецам, и мы сделаем ваш домик не только согретым, но и модернизированным. Заинтересовались? Подробнее о наших сервисах вы можете узнать на интернет-портале. Добро пожаловать в обитель гармонии и качественной работы.
fox sweetie: ph sweetie fox – sweetie fox new
http://lanarhoades.pro/# lana rhoades pics
eva elfie full video [url=http://evaelfie.site/#]eva elfie new video[/url] eva elfie new video
https://gruzchikirabotat.ru/
raytalktech.com
Fang Jifan은 “그의 이름은 언급할 가치가 없다”고 말했다.
eva elfie videos: eva elfie full video – eva elfie new video
https://lanarhoades.pro/# lana rhoades boyfriend
mia malkova photos: mia malkova videos – mia malkova only fans
https://sweetiefox.pro/# sweetie fox full
sweetie fox new: sweetie fox cosplay – ph sweetie fox
https://miamalkova.life/# mia malkova full video
sweetie fox video [url=http://sweetiefox.pro/#]sweetie fox new[/url] ph sweetie fox
mia malkova photos: mia malkova hd – mia malkova full video
mia malkova new video: mia malkova movie – mia malkova girl
mia malkova videos: mia malkova photos – mia malkova photos
https://sweetiefox.pro/# sweetie fox new
100% free dating service: http://sweetiefox.pro/# sweetie fox cosplay
fox sweetie fox sweetie or fox sweetie
https://cse.google.la/url?sa=t&url=https://sweetiefox.pro sweetie fox
[url=https://images.google.fm/url?sa=t&url=https://sweetiefox.pro]sweetie fox video[/url] sweetie fox video and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=787598]fox sweetie[/url] sweetie fox cosplay
lana rhoades solo lana rhoades full video or lana rhoades boyfriend
https://maps.google.tl/url?q=https://lanarhoades.pro lana rhoades unleashed
[url=http://images.google.kg/url?q=http://lanarhoades.pro]lana rhoades boyfriend[/url] lana rhoades unleashed and [url=http://talk.dofun.cc/home.php?mod=space&uid=507071]lana rhoades[/url] lana rhoades videos
http://evaelfie.site/# eva elfie videos
fox sweetie: sweetie fox new – sweetie fox full video
http://evaelfie.site/# eva elfie new videos
eva elfie photo [url=http://evaelfie.site/#]eva elfie photo[/url] eva elfie full video
lana rhoades hot: lana rhoades hot – lana rhoades full video
mia malkova latest: mia malkova only fans – mia malkova girl
http://lanarhoades.pro/# lana rhoades full video
mia malkova mia malkova full video or mia malkova only fans
http://www.garrisonexcelsior.com/redirect.php?url=http://miamalkova.life mia malkova latest
[url=http://images.google.bi/url?q=https://miamalkova.life]mia malkova latest[/url] mia malkova and [url=http://www.donggoudi.com/home.php?mod=space&uid=135559]mia malkova[/url] mia malkova only fans
mersingtourism.com
게다가 지금은 사실… 자신을 너무 높게 생각하고 있어…
https://sweetiefox.pro/# sweetie fox full
eva elfie full video eva elfie new video or eva elfie new videos
http://www.google.com.ph/url?q=http://evaelfie.site eva elfie photo
[url=https://www.okpodiatrists.org/external-link?url=https://evaelfie.site]eva elfie videos[/url] eva elfie videos and [url=https://fl.liaochengquan.cn/home.php?mod=space&uid=1277245]eva elfie hot[/url] eva elfie photo
mia malkova only fans: mia malkova photos – mia malkova latest
mia malkova only fans: mia malkova latest – mia malkova photos
http://evaelfie.site/# eva elfie hd
eva elfie full videos [url=https://evaelfie.site/#]eva elfie[/url] eva elfie hot
smcasino-game.com
우리 Fang Jifan은 칙령에 저항하고 따르지 않았습니다. 흠, 당신은 나에게 무엇을 할 수 있습니다.
mia malkova full video: mia malkova girl – mia malkova movie
dating best sites: https://sweetiefox.pro/# sweetie fox new
eva elfie videos: eva elfie – eva elfie new videos
http://miamalkova.life/# mia malkova photos
pactam2.com
드디어 빛이 나고 Shen Ao는 쌍안경으로 필사적으로 구석구석을 찾았습니다.
33개 언어와 다양한 화폐를 통해 세계 시장에 제공되는 프라그마틱 플레이의 250개 이상의 게임으로 구성된 슬롯 포트폴리오를 즐겨보세요.
프라그마틱 슬롯 무료
프라그마틱 슬롯에 대한 내용이 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 찾아보실 수 있어요. 함께 지식을 공유해보세요!
https://spinner44.com/
http://ivermectininstock.com/
https://www.iaz681.com
http://sweetiefox.pro/# sweetie fox full video
ph sweetie fox: sweetie fox video – fox sweetie
lana rhoades videos: lana rhoades unleashed – lana rhoades hot
https://sweetiefox.pro/# sweetie fox video
sweetie fox full [url=https://sweetiefox.pro/#]sweetie fox cosplay[/url] sweetie fox full video
Very descriptive blog, I liked that a lot. Will there be
a part 2?
lana rhoades boyfriend: lana rhoades unleashed – lana rhoades hot
dateing site: http://evaelfie.site/# eva elfie videos
sweetie fox new: fox sweetie – sweetie fox video
https://evaelfie.site/# eva elfie full videos
mia malkova movie [url=http://miamalkova.life/#]mia malkova girl[/url] mia malkova full video
lana rhoades full video: lana rhoades hot – lana rhoades boyfriend
jelenakaludjerovic.com
류진은 “그럼 아빠도 같이 갈까? “라고 겸손하게 말했다.
lana rhoades unleashed: lana rhoades unleashed – lana rhoades
http://evaelfie.site/# eva elfie hd
https://evaelfie.site/# eva elfie full video
eva elfie: eva elfie videos – eva elfie full videos
https://sweetiefox.pro/# sweetie fox
lana rhoades [url=https://lanarhoades.pro/#]lana rhoades unleashed[/url] lana rhoades hot
I like what you guys are up too. Such clever work and reporting! Carry on the superb works guys I¦ve incorporated you guys to my blogroll. I think it’ll improve the value of my site 🙂
I have not checked in here for a while since I thought it was getting boring, but the last several posts are good quality so I guess I’ll add you back to my everyday bloglist. You deserve it my friend 🙂
Забудьте о проблемах с холодильником Атлант: профессиональный ремонт с гарантией.
цена ремонта холодильника атлант на дому [url=https://remont-holodilnikov-atlant.ru/]ремонт холодильников атлант[/url] .
mia malkova full video: mia malkova photos – mia malkova latest
mega-slot77.com
왕궁에 있을 때 환관들이 잘못을 저질렀고 모두 뺨을 때렸습니다.
https://maps.google.at/url?q=j&rct=j&url=https%3A%2F%2Fwww.agenbet88score.com%2F
eva elfie new video: eva elfie hd – eva elfie full video
http://sweetiefox.pro/# sweetie fox video
http://sweetiefox.pro/# sweetie fox full
dating sites for totally free for usa: http://lanarhoades.pro/# lana rhoades
lana rhoades lana rhoades hot or <a href=" http://intra.etinar.com/xampp/phpinfo.php?a%5B%5D=Viagra+generic “>lana rhoades hot
https://www.google.com.pk/url?sa=t&url=https://lanarhoades.pro lana rhoades hot
[url=https://www.bioguiden.se/redirect.aspx?url=http://lanarhoades.pro]lana rhoades[/url] lana rhoades hot and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3078448]lana rhoades full video[/url] lana rhoades
lana rhoades hot: lana rhoades full video – lana rhoades unleashed
http://miamalkova.life/# mia malkova latest
mia malkova new video [url=https://miamalkova.life/#]mia malkova latest[/url] mia malkova movie
lana rhoades solo: lana rhoades hot – lana rhoades boyfriend
mia malkova girl mia malkova videos or mia malkova photos
https://maps.google.com.ng/url?q=https://miamalkova.life mia malkova only fans
[url=https://images.google.com.my/url?sa=t&url=http://miamalkova.life]mia malkova videos[/url] mia malkova hd and [url=http://www.tmml.top/home.php?mod=space&uid=60717]mia malkova movie[/url] mia malkova
mia malkova hd: mia malkova movie – mia malkova only fans
https://miamalkova.life/# mia malkova new video
http://jogodeaposta.fun/# jogo de aposta
http://aviatormocambique.site/# aviator
aviator game: estrela bet aviator – aviator jogo
https://aviatorjogar.online/# aviator pin up
Преврати свою старую мебель в новую! Перетянем ее в Минске
перетяжка мягкой мебели цены [url=https://obivka-mebeli-vminske.ru/]https://obivka-mebeli-vminske.ru/[/url] .
https://aviatoroyunu.pro/# aviator sinyal hilesi
aviator game online [url=https://aviatorghana.pro/#]aviator game online[/url] aviator sportybet ghana
aviator game online: aviator login – aviator login
Ремонт и перетяжка мягкой мебели в Минске
реставрация мебели [url=https://obivka-mebeli-vminske.ru/]https://obivka-mebeli-vminske.ru/[/url] .
I have been absent for some time, but now I remember why I used to love this blog. Thanks , I will try and check back more frequently. How frequently you update your site?
What i do not realize is in reality how you are no longer really much more well-liked than you might be now. You’re very intelligent. You realize thus significantly in relation to this matter, produced me individually consider it from numerous numerous angles. Its like women and men don’t seem to be fascinated until it is something to do with Girl gaga! Your individual stuffs nice. At all times maintain it up!
http://aviatormocambique.site/# aviator bet
http://aviatormalawi.online/# aviator game
[url=http://azithromycinmds.com/]how much is azithromycin over the counter[/url]
Aw, this was a really nice post. In thought I wish to put in writing like this moreover – taking time and actual effort to make an excellent article… but what can I say… I procrastinate alot and on no account seem to get one thing done.
you will have a fantastic blog here! would you prefer to make some invite posts on my weblog?
Как проверить лицензию онлайн казино Беларусь: гарантия безопасной игры
онлайн казино [url=https://onlinecasinobelarus.by/]онлайн казино[/url] .
aviator sportybet ghana: aviator login – aviator ghana
mega-slot1.com
제자들은 모두 힘이 세고, 은인인 당신은 온종일 아무것도 하지 않고 지내고 있습니다…
aviator betano: estrela bet aviator – aviator jogo
https://aviatorghana.pro/# play aviator
aviator oyna: aviator oyunu – pin up aviator
raytalktech.com
허팡지판은 자신의 약점을 지켜주는 사람이라고 인정했다.
https://aviatorghana.pro/# aviator
https://aviatormocambique.site/# jogar aviator
aviator pin up casino [url=http://pinupcassino.pro/#]aviator oficial pin up[/url] aviator pin up casino
aviator game online: aviator bet malawi – aviator bet malawi login
cassino pin up: pin up cassino online – pin-up
https://aviatormocambique.site/# aviator
Мастерская по перетяжке мягкой мебели в Минске – доверенный выбор
перетяжка мягкой мебели цены [url=https://obivka-mebeli-vminske.ru/]https://obivka-mebeli-vminske.ru/[/url] .
[url=http://www.1-xbet-france.com]www.1-xbet-france.com[/url]
Working 1xbet mirror looking for entering the true website of the bookmaker. Handle it to take with 1xBet, be paid bonuses and place online bets.
http://1-xbet-france.com
andrejpos.com
일부 기념관이 처리 된 후 Hongzhi 황제는 Xiao Jing과 Ouyang Zhi를 남겼습니다.
aviator: aviator game bet – play aviator
pin up aviator aviator jogar or estrela bet aviator
https://maps.google.tg/url?q=https://aviatorjogar.online aviator game
[url=https://www.google.com.np/url?q=https://aviatorjogar.online]aviator pin up[/url] aviator bet and [url=http://www.tmml.top/home.php?mod=space&uid=62742]aviator game[/url] aviator bet
https://jogodeaposta.fun/# jogo de aposta
프라그마틱 플레이의 흥미진진한 세계로 초대합니다.
프라그마틱 홈페이지
프라그마틱 슬롯에 대한 글 정말 잘 읽었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 얻을 수 있어요. 함께 교류하며 더 많은 지식을 얻어보세요!
https://doggggqwe.weebly.com/
https://e-trajet.net/hot/
https://wszhibo.com/hot/
aviator malawi: aviator bet – aviator bet malawi
como jogar aviator em mocambique: aviator – como jogar aviator
https://pinupcassino.pro/# pin up cassino online
https://aviatoroyunu.pro/# aviator hilesi
Доверь перетяжку мебели квалифицированным специалистам в Минске
перетяжка мебели тканью [url=https://obivka-divana.ru/]https://obivka-divana.ru/[/url] .
Мастерская по перетяжке мебели в Минске
обивка мягкой мебели [url=https://obivka-divana.ru/]https://obivka-divana.ru/[/url] .
aplicativo de aposta: jogo de aposta online – ganhar dinheiro jogando
http://aviatoroyunu.pro/# pin up aviator
melhor jogo de aposta [url=https://jogodeaposta.fun/#]site de apostas[/url] melhor jogo de aposta para ganhar dinheiro
http://aviatoroyunu.pro/# aviator oyunu
Твоя мебель выглядит устаревшей? Перетяни ее в Минске!
перетяжка мягкой мебели [url=https://obivka-divana.ru/]https://obivka-divana.ru/[/url] .
play aviator: aviator game – aviator ghana
Перетяжка мебели в Минске: не просто ремонт, а настоящее преображение
перетяжка дивана цена [url=https://obivka-divana.ru/]https://obivka-divana.ru/[/url] .
melhor jogo de aposta: site de apostas – melhor jogo de aposta para ganhar dinheiro
Перетяжка мягкой мебели в Минске: бережно и безупречно
перетяжка кресел минск [url=https://obivka-divana.ru/]https://obivka-divana.ru/[/url] .
aviator jogo de aposta aviator jogo de aposta or melhor jogo de aposta para ganhar dinheiro
http://images.google.co.bw/url?q=https://jogodeaposta.fun jogo de aposta
[url=https://community.sugarcrm.com/external-link.jspa?url=http://jogodeaposta.fun]ganhar dinheiro jogando[/url] aplicativo de aposta and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=791298]ganhar dinheiro jogando[/url] melhor jogo de aposta
jogar aviator online: aviator pin up – jogar aviator Brasil
?Juega y gana con el bono casino sin deposito!
casino en linea con bono de bienvenida sin deposito [url=https://bono-casino-sin-deposito-peru.com/]bono sin deposito casino peru[/url] .
aviator bet: aviator online – aviator
http://aviatormalawi.online/# aviator game
aviator game [url=http://aviatorghana.pro/#]aviator bet[/url] aviator bet
http://aviatorjogar.online/# jogar aviator online
aviator betting game: aviator bet malawi login – aviator bet
play aviator aviator game bet or aviator game bet
https://maps.google.gp/url?sa=t&url=https://aviatorghana.pro aviator
[url=https://maps.google.pn/url?q=https://aviatorghana.pro]aviator[/url] aviator ghana and [url=https://m.414500.cc/home.php?mod=space&uid=3363871]aviator login[/url] aviator ghana
depósito mínimo 1 real: melhor jogo de aposta para ganhar dinheiro – melhor jogo de aposta
aviator sinyal hilesi: aviator oyna slot – aviator sinyal hilesi
manzanaresstereo.com
그는 숨을 크게 들이마신 다음 퍼프와 함께…
play aviator: aviator bet malawi login – aviator game
pin-up cassino pin up cassino online or pin-up casino login
https://images.google.sc/url?sa=t&url=https://pinupcassino.pro pin up cassino online
[url=https://cse.google.no/url?sa=t&url=https://pinupcassino.pro]aviator pin up casino[/url] pin-up casino and [url=https://forex-bitcoin.com/members/334955-bulsqwjmjk]pin-up casino entrar[/url] pin up aviator
[url=http://metoformin.online/]generic metformin cost[/url]
https://pinupcassino.pro/# pin up
jogo de aposta online: ganhar dinheiro jogando – jogo de aposta online
zithromax for sale cheap – https://azithromycin.pro/zithromax-with-alcohol.html zithromax over the counter canada
jogo de aposta online: jogos que dao dinheiro – aplicativo de aposta
http://aviatoroyunu.pro/# aviator bahis
https://aviatormalawi.online/# aviator bet
pin up aviator [url=https://pinupcassino.pro/#]pin up cassino online[/url] pin up cassino online
ингибитор коррозии что это [url=https://www.ingibitor-korrozii-msk.ru/]https://www.ingibitor-korrozii-msk.ru/[/url] .
aviator hilesi: aviator sinyal hilesi – pin up aviator
프라그마틱 카지노
그 후 공원의 중문이 활짝 열리자 학교 관리가 모든 하인을 이끌고 나갔다.
https://clients1.google.bj/url?q=https%3A%2F%2Fwww.colorful-navi.com%2F
выбор детской коляски [url=https://detskie-koljaski-msk.ru/]https://detskie-koljaski-msk.ru/[/url] .
zithromax 500 – https://azithromycin.pro/zithromax-vs-doxycycline.html zithromax 250
https://jogodeaposta.fun/# jogo de aposta online
jogar aviator Brasil: estrela bet aviator – jogar aviator Brasil
aviator bet malawi login: aviator bet – aviator bet malawi login
https://aviatormocambique.site/# aviator
aviator jogar aviator jogo or aviator game
http://www.gaxclan.de/url?q=https://aviatorjogar.online estrela bet aviator
[url=https://images.google.ro/url?sa=t&url=https://aviatorjogar.online]jogar aviator Brasil[/url] aviator bet and [url=http://91075425.k216.opensrs.cn/home.php?mod=space&uid=1126137]aviator jogar[/url] estrela bet aviator
aviator bet: aviator bet – play aviator
deposito minimo 1 real: jogos que dao dinheiro – melhor jogo de aposta
https://aviatoroyunu.pro/# aviator oyna slot
dota2answers.com
Andre는 현재 프로젝트 진행에 대한 불만을 표명했습니다.
andrejpos.com
그는 세상에서 가장 놀라운 일을 만나도 침착함을 유지한다.
online canadian pharmacy reviews: Best Canadian online pharmacy – canada cloud pharmacy canadianpharm.store
https://indianpharm24.shop/# buy medicines online in india indianpharm.store
mexican pharmaceuticals online [url=http://mexicanpharm24.shop/#]Medicines Mexico[/url] reputable mexican pharmacies online mexicanpharm.shop
프라그마틱 게임은 iGaming 업계에서 혁신적이며 표준화된 모바일 중심의 콘텐츠를 고객에게 제공합니다.
프라그마틱슬롯
프라그마틱과 관련된 이 글 정말 잘 읽었어요! 더불어 저도 제 사이트에서 프라그마틱에 대한 새로운 정보를 공유 중이에요. 함께 나누면 더 좋을 것 같아요!
https://www.ukkosmaine.com
https://www.12315op.cn/
https://www.ashspurr.com
canadianpharmacymeds com: canadian pharmacy – canadianpharmacyworld com canadianpharm.store
http://canadianpharmlk.shop/# canadian neighbor pharmacy canadianpharm.store
indian pharmacy: Generic Medicine India to USA – buy medicines online in india indianpharm.store
cheapest online pharmacy india [url=http://indianpharm24.com/#]Online medicine home delivery[/url] cheapest online pharmacy india indianpharm.store
http://canadianpharmlk.com/# is canadian pharmacy legit canadianpharm.store
mexico drug stores pharmacies: mexico pharmacies prescription drugs – reputable mexican pharmacies online mexicanpharm.shop
https://mexicanpharm24.com/# mexican pharmaceuticals online mexicanpharm.shop
https://mexicanpharm24.com/# mexican rx online mexicanpharm.shop
https://indianpharm24.com/# top 10 online pharmacy in india indianpharm.store
http://indianpharm24.shop/# best online pharmacy india indianpharm.store
https://indianpharm24.shop/# reputable indian pharmacies indianpharm.store
buy medicines online in india: Pharmacies in India that ship to USA – buy medicines online in india indianpharm.store
mexican online pharmacies prescription drugs: Mexico pharmacy price list – п»їbest mexican online pharmacies mexicanpharm.shop
cheapest online pharmacy india [url=http://indianpharm24.com/#]Online India pharmacy[/url] pharmacy website india indianpharm.store
https://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
http://mexicanpharm24.com/# reputable mexican pharmacies online mexicanpharm.shop
top 10 online pharmacy in india: online pharmacy in india – Online medicine home delivery indianpharm.store
http://canadianpharmlk.shop/# pharmacies in canada that ship to the us canadianpharm.store
https://mexicanpharm24.shop/# mexico drug stores pharmacies mexicanpharm.shop
https://indianpharm24.shop/# reputable indian online pharmacy indianpharm.store
http://indianpharm24.com/# mail order pharmacy india indianpharm.store
mexican pharmacy: Mexico pharmacy price list – medicine in mexico pharmacies mexicanpharm.shop
mexican rx online buying prescription drugs in mexico or mexican pharmaceuticals online
http://www.lighthousehoptown.org/System/Login.asp?id=55666&Referer=https://mexicanpharm24.com mexico drug stores pharmacies
[url=https://maps.google.bf/url?q=https://mexicanpharm24.com]medication from mexico pharmacy[/url] buying prescription drugs in mexico and [url=https://sb.diandiancom.com/home.php?mod=space&uid=2131]buying prescription drugs in mexico online[/url] mexican border pharmacies shipping to usa
recommended canadian pharmacies: Cheapest drug prices Canada – canadianpharmacy com canadianpharm.store
http://canadianpharmlk.shop/# canada drugs online reviews canadianpharm.store
world pharmacy india [url=http://indianpharm24.com/#]Generic Medicine India to USA[/url] top online pharmacy india indianpharm.store
canadian pharmacy prices canadian pharmacy 365 or canadian online pharmacy
https://tamago.care-cure.jp/shop/display_cart?return_url=https://canadianpharmlk.shop canadian pharmacy price checker
[url=https://www.film1.nl/zoek/?q=/><a+href=http://canadianpharmlk.shop&]canadian pharmacy checker[/url] rate canadian pharmacies and [url=http://www.9kuan9.com/home.php?mod=space&uid=333965]pharmacy in canada[/url] canadian valley pharmacy
https://mexicanpharm24.com/# mexico pharmacies prescription drugs mexicanpharm.shop
top online pharmacy india: indian pharmacy – indianpharmacy com indianpharm.store
http://mexicanpharm24.com/# reputable mexican pharmacies online mexicanpharm.shop
https://indianpharm24.shop/# top online pharmacy india indianpharm.store
https://indianpharm24.shop/# top 10 online pharmacy in india indianpharm.store
buying prescription drugs in mexico buying prescription drugs in mexico or mexican mail order pharmacies
https://maps.google.bi/url?q=https://mexicanpharm24.com mexico drug stores pharmacies
[url=http://haedongacademy.org/phpinfo.php?a[]=wall+decor+decals+(]mexican mail order pharmacies[/url] mexican pharmaceuticals online and [url=https://slovakia-forex.com/members/252803-aotsskeuxa]buying prescription drugs in mexico[/url] best online pharmacies in mexico
п»їbest mexican online pharmacies mexico drug stores pharmacies or reputable mexican pharmacies online
https://www.google.tt/url?q=https://mexicanpharm24.shop п»їbest mexican online pharmacies
[url=https://www.trueweb.eu/?a=link&url=https://mexicanpharm24.shop]mexico pharmacy[/url] medicine in mexico pharmacies and [url=https://fl.liaochengquan.cn/home.php?mod=space&uid=1338826]purple pharmacy mexico price list[/url] mexican pharmacy
http://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
canadian online pharmacy reviews: canadian pharmacy – canadianpharmacy com canadianpharm.store
http://canadianpharmlk.shop/# canada pharmacy online legit canadianpharm.store
Bonos sin deposito: juega gratis en el casino
casino online con bono de bienvenida sin deposito [url=https://bono-casino-sin-deposito-peru.com/]bono casino sin deposito[/url] .
chutneyb.com
맞습니다, 서산 의과 대학은 의외로 간을 정화하고 시력을 향상시킨 경험이 있습니다.
https://indianpharm24.com/# legitimate online pharmacies india indianpharm.store
https://kupitzhilie.ru/
에그벳 도메인
Zhu Houzhao는 그를 때리고 싶어 그를 응시했습니다.
https://cse.google.com.pe/url?sa=t&url=https%3A%2F%2Fwww.agenbet88score.com%2F
prednisone in canada: 50mg prednisone tablet – buy prednisone online no script
Как выбрать идеальный тепловизор: советы и рекомендации
тепловизоры [url=teplovizor-od.co.ua]teplovizor-od.co.ua[/url] .
https://salezhilie.ru/
Как использовать email-маркетинг для продвижения сайта
14
seo продвижение [url=https://seo-prodvizhenie-sayta.co.ua/]https://seo-prodvizhenie-sayta.co.ua/[/url] .
amoxacillian without a percription: where to buy amoxicillin pharmacy – azithromycin amoxicillin
https://clomidst.pro/# can you buy cheap clomid pill
cost clomid tablets: does clomid help erectile dysfunction – where to buy generic clomid
mojmelimajmuea.com
여기에서 Hongzhi 황제와 Zhu Houzhao 왕자가 여기에서 기다리고있었습니다.
https://kupithouse.ru/
prednisone buy canada: brand prednisone – cost of prednisone
prednisone 2.5 mg price: how long for prednisone to work – prednisone without rx
https://kupitroom.ru/
buy prednisone online no script: prednisone 20 mg in india – prednisone 5 mg
http://prednisonest.pro/# prednisone prescription online
can i get clomid online: clomid 100mg success rate – can i order generic clomid pills
https://arcmetal.ru/
프라그마틱플레이의 슬롯으로 다양한 게임을 즐겨보세요.
프라그마틱 무료 슬롯
프라그마틱 슬롯에 대한 설명 감사합니다! 또한, 제 사이트에서도 프라그마틱과 관련된 정보를 얻을 수 있어요. 함께 이야기 나누면서 더 많은 지식을 얻어가요!
https://www.12315yc.cn/
https://mashhadnet.com/link/
https://hfmxz.com/link/
amoxicillin no prescription [url=http://amoxilst.pro/#]amoxicillin online purchase[/url] amoxicillin 500 tablet
prednisone 12 tablets price: 5 prednisone in mexico – prednisone 5084
buy amoxicillin 500mg capsules uk: amoxil cost – buy amoxicillin
https://prednisonest.pro/# prednisone 30 mg daily
[url=https://one-xbet-france.com]https://one-xbet-france.com[/url]
Plateforme en ligne 1xBet: outils pour gagner de l’argent. En unrestricted, 1xBet France est un bookmaker classique talk up comme stake365 bookmaker et beaucoup d’autres.
https://one-xbet-france.com
where to get clomid now: clomid without insurance – cheap clomid without rx
prednisone 5 tablets: buy prednisone without prescription paypal – 15 mg prednisone daily
https://kupitroom.ru/
how to get generic clomid without a prescription: can i buy clomid – where can i buy cheap clomid online
https://amoxilst.pro/# amoxicillin buy online canada
can i order generic clomid no prescription: best days to take clomid for twins – can you get generic clomid without insurance
?Gana dinero sin invertir! Bono casino sin deposito
casino online bono sin deposito [url=https://bono-casino-sin-deposito-peru.com/]casino con bono de bienvenida sin deposito[/url] .
where can i get generic clomid without rx generic clomid without rx or cost of clomid online
https://www.google.com.ar/url?q=https://clomidst.pro can i buy clomid without insurance
[url=http://electronix.ru/redirect.php?http://clomidst.pro]how to get clomid without prescription[/url] can i order generic clomid no prescription and [url=http://www.9kuan9.com/home.php?mod=space&uid=356360]can you buy generic clomid without insurance[/url] how can i get cheap clomid no prescription
сравнение
20. Как выбрать долговечный прицел для охоты
купить оптический прицел в одессе [url=https://opticheskiy-pricel-odessa.co.ua]https://opticheskiy-pricel-odessa.co.ua[/url] .
amoxicillin 500 coupon: amoxicillin 500mg capsule cost – purchase amoxicillin online without prescription
https://spbflatkupit.ru/
can you buy cheap clomid for sale: cost of generic clomid pills – can i get clomid pills
generic clomid without insurance [url=http://clomidst.pro/#]where can i buy generic clomid without prescription[/url] how to get cheap clomid without rx
For those on the lookout for esteemed online casinos accommodating Mpesa transactions, your journey begins here.
https://spbdomkupit.ru/
https://amoxilst.pro/# cost of amoxicillin 30 capsules
prednisone 5mg cost: prednisone and ibuprofen – prednisone 10mg price in india
no prescription online prednisone: prednisone dosage for poison ivy – prednisone 5 50mg tablet price
https://spbkupitzhilie.ru/
prednisone 40 mg rx: side effects prednisone – prednisone prescription online
bistroduet.com
그래서 Fang Jifan은 무거운 마음으로 Meridian Gate를 서둘러 나갔습니다!
http://clomidst.pro/# cheap clomid now
amoxicillin online no prescription: can you drink on amoxicillin – buy amoxicillin
buy cheap amoxicillin online: how much is amoxicillin without insurance – amoxicillin online purchase
where to buy generic clomid without prescription: can i purchase generic clomid – can you buy cheap clomid no prescription
buy cheap clomid without dr prescription: can i order generic clomid – cost cheap clomid online
buy prednisone without prescription: generic prednisone cost – prednisone 50 mg prices
https://ekbflatkupit.ru/
https://zhksaleflat.ru/
https://zhksalezhilie.ru/
http://onlinepharmacy.cheap/# mail order pharmacy no prescription
apksuccess.com
왜… Fang Jifan은 정말 좋은 생각이 있는 걸까요?
https://zhksalehouse.ru/
edmeds: buy ed meds – ed rx online
Решение всех задач с грузоперевозками в Харькове
служба переезда [url=https://gruzchiki.co.ua/]https://gruzchiki.co.ua/[/url] .
https://zhksaledom.ru/
https://onlinepharmacy.cheap/# best canadian pharmacy no prescription
https://vsegda-pomnim.com/
ttbslot.com
Liu Jian의 얼굴은 마치 넘어지기 직전처럼 매우 추했습니다.
no prescription drugs online [url=http://pharmnoprescription.pro/#]canadian drugs no prescription[/url] medications online without prescriptions
http://klublady.ru/
how to get ed pills: cheap erectile dysfunction pills – buy ed meds
no prescription pharmacy online: buy medications without prescriptions – canadian pharmacy without a prescription
https://onlinepharmacy.cheap/# drugstore com online pharmacy prescription drugs
https://onlinepharmacy.cheap/# canada pharmacy coupon
legal online pharmacy coupon code: best online pharmacy – online canadian pharmacy coupon
erectile dysfunction pills online: cheapest ed online – ed meds online
mexican pharmacies no prescription: how to get a prescription in canada – no prescription canadian pharmacy
canadian pharmacy no prescription: best online pharmacy – cheapest pharmacy for prescriptions
https://edpills.guru/# ed prescriptions online
http://diplombiolog.ru/
best ed medication online online erectile dysfunction or get ed meds online
https://forum.keenswh.com/proxy.php?link=http://edpills.guru ed online pharmacy
[url=https://image.google.co.zw/url?q=https://edpills.guru]where to buy ed pills[/url] ed treatment online and [url=http://www.9kuan9.com/home.php?mod=space&uid=371124]order ed pills online[/url] best online ed meds
http://pharmnoprescription.pro/# online pharmacies without prescription
canadian pharmacy coupon code: online pharmacy india – pharmacy online 365 discount code
В нашем кинотеатре https://hdrezka.uno смотреть фильмы и сериалы в хорошем HD-качестве можно смотреть с любого устройства, имеющего доступ в интернет. Наслаждайся кино или телесериалами в любом месте с планшета, смартфона под управлением iOS или Android.
http://edpills.guru/# cheap erection pills
https://kursovyebiolog.ru
buy erectile dysfunction medication [url=https://edpills.guru/#]cheap ed treatment[/url] where to get ed pills
ed medications cost: cheap ed pills online – affordable ed medication
https://kursovyebuhgalter.ru
purchasing prescription drugs online: prescription from canada – online pharmacy without prescriptions
http://pharmnoprescription.pro/# canada pharmacy online no prescription
https://onlinepharmacy.cheap/# canadian online pharmacy no prescription
ed online pharmacy: cost of ed meds – buy erectile dysfunction pills
Идеи для декорирования сада с помощью рулонного газона
рулонный газон москва [url=https://rulonnyygazon177.ru/]https://rulonnyygazon177.ru/[/url] .
Как выбрать подходящий рулонный газон для своего сада
рулонный газон цена за м2 [url=https://rulonnyygazon177.ru/]https://rulonnyygazon177.ru/[/url] .
legit non prescription pharmacies: online mexican pharmacy – canadian pharmacy no prescription
international pharmacy no prescription: Cheapest online pharmacy – overseas pharmacy no prescription
Как быстро и легко установить рулонный газон
рулонный газон живой [url=https://rulonnyygazon177.ru/]https://rulonnyygazon177.ru/[/url] .
프라그마틱의 게임을 플레이하면서 항상 신선한 경험을 얻을 수 있어 기뻐요. 여기서 더 많은 이야기를 나눠봐요!
프라그마틱 홈페이지
프라그마틱에 대한 내용 정말 흥미로워요! 또한, 제 사이트에서도 프라그마틱과 관련된 정보를 공유하고 있어요. 함께 지식을 공유해보세요!
https://jitairent.com/link/
https://www.12315oq.cn/
https://ewqeq.weebly.com
cheapest pharmacy to get prescriptions filled: mexico pharmacy online – international pharmacy no prescription
https://onlinepharmacy.cheap/# canada pharmacy not requiring prescription
Embark on an exhilarating journey with online casinos Kenya, offering fresh titles and lightning-fast payouts.
mexican rx online: mexico drug stores pharmacies – mexican drugstore online
canadian mail order prescriptions: canadian prescriptions in usa – online drugs no prescription
sandyterrace.com
Zhu Houzhao는 “Jinyiwei 사령관 Mu Bin 사령관”이라고 말했습니다.
qiyezp.com
Zhang Mao와 Xu Yongning은 “나는 죽을 것입니다. “라고 절하고 유죄를 인정하느라 바빴습니다.
криптовалютная биржа в россии
https://zadachbiolog.ru/
https://pharmacynoprescription.pro/# no prescription needed
https://t.me/crypto_signals_binance_pump/24498/ Standard Price for VIP- membership for 1 Week VIP Membership is 0.0014 BTC, You will do send payment to BTC address 1KEY1iKrdLQCUMFMeK4FEZXiedDris7uGd Discounted price may be different from 0.00075 to 0.00138 BTC, that is why follow to all announces published in our Public channel!
https://pharmacynoprescription.pro/# cheap prescription drugs online
buying from online mexican pharmacy: mexico pharmacies prescription drugs – mexican rx online
https://zadachbuhgalter.ru
https://otchetbiolog.ru/
https://otchetbuhgalter.ru/
top 10 online pharmacy in india: cheapest online pharmacy india – reputable indian online pharmacy
mexican mail order pharmacies [url=http://mexicanpharm.online/#]mexican online pharmacies prescription drugs[/url] buying prescription drugs in mexico online
https://canadianpharm.guru/# canadian pharmacy no scripts
https://indianpharm.shop/# Online medicine order
http://pharmacynoprescription.pro/# no prescription canadian pharmacies
canadian pharmacy world reviews: pharmacy canadian – legit canadian pharmacy
canada pharmacy reviews: legitimate canadian mail order pharmacy – canadian online pharmacy
I seriously love your website.. Very nice colors & theme. Did you develop
this site yourself? Please reply back as I’m p평택출장샵lanning to create my
own site and would love to learn where you got this from or what the theme
is called.
buying from online mexican pharmacy: mexican pharmaceuticals online – best online pharmacies in mexico
https://resheniezadachfizika.ru/
buying prescription drugs in mexico mexican online pharmacies prescription drugs or mexican online pharmacies prescription drugs
https://toolbarqueries.google.pn/url?q=http://mexicanpharm.online mexican pharmacy
[url=http://wiki.wlug.org.nz/~matt/m.php?a%5B%5D=%3Ca%20href%3Dhttp%3A%2F%2Fmexicanpharm.online%2F%3E%C3%91%C5%8D%C3%90%C2%BB%C3%90%C2%B5%C3%90%C2%BA%C3%91%E2%80%9A%C3%91%E2%82%AC%C3%90%C2%BE%C3%91%81%C3%90%C2%BD%C3%90%C2%B0%C3%90%C2%B1%C3%90%C2%B6%C3%90%C2%B5%C3%90%C2%BD%C3%90%C2%B8%C3%90%C2%B5%20%C3%91%83%C3%91%E2%80%A1%C3%90%C2%B0%C3%91%81%C3%91%E2%80%9A%C3%90%C2%BA%C3%90%C2%B0%20%C3%91%E2%80%A0%C3%90%C2%B5%C3%91%E2%80%A6%C3%90%C2%B0%20%C3%90%C2%B4%C3%90%C2%B8%C3%90%C2%BF%C3%90%C2%BB%C3%90%C2%BE%C3%90%C2%BC%3C%2Fa%3E]purple pharmacy mexico price list[/url] buying prescription drugs in mexico and [url=http://wuyuebanzou.com/home.php?mod=space&uid=493146]mexican drugstore online[/url] medicine in mexico pharmacies
best mexican online pharmacies: buying prescription drugs in mexico online – mexico drug stores pharmacies
https://kursovyemarketing.ru/
https://mexicanpharm.online/# best online pharmacies in mexico
http://avicenna-s.ru/
indian pharmacies safe [url=http://indianpharm.shop/#]world pharmacy india[/url] indian pharmacy paypal
Услуга демонтажа старых частных домов и вывоза мусора в Москве и Подмосковье. Наши специалисты бесплатно выезжают на объект для консультации и оценки объема работ. Мы предлагаем услуги на сайте https://orenvito.ru по доступным ценам и гарантируем качественное выполнение всех работ.
Для получения более подробной информации и рассчета стоимости наших услуг, вы можете связаться с нами по телефону или заполнить форму заявки на нашем сайте.
canadianpharmacymeds com: legitimate canadian pharmacy – canadian pharmacy tampa
qiyezp.com
이 경우 Xie Qian은 “명령에 복종합니다! “라고 계속 반대 할 것이 없습니다.
best canadian online pharmacy: canadian pharmacy mall – best canadian pharmacy to buy from
https://1ecenter.ru
no prescription pharmacy online: online meds no prescription – online pharmacy with prescription
http://indianpharm.shop/# online shopping pharmacy india
buying prescription drugs in mexico: medication from mexico pharmacy – medication from mexico pharmacy
http://canadianpharm.guru/# canadian pharmacy
Услуга демонтажа старых частных домов и вывоза мусора в Москве и Подмосковье от нашей компании. Мы предлагаем демонтаж и вывоз мусора в указанном регионе по доступным ценам. Наша команда https://hoteltramontano.ru гарантирует выполнение услуги в течение 24 часов после заказа. Мы бесплатно оцениваем объект и консультируем клиентов. Узнать подробности и рассчитать стоимость можно по телефону или на нашем сайте.
canadian online pharmacy: escrow pharmacy canada – canadian pharmacy service
п»їlegitimate online pharmacies india: top online pharmacy india – buy prescription drugs from india
https://canadianpharm.guru/# canadian pharmacy 24h com
indian pharmacy: india online pharmacy – mail order pharmacy india
[url=https://oazithromycin.com/]azithromycin otc usa[/url]
best online pharmacy without prescription: no prescription medicine – canada pharmacies online prescriptions
medication from mexico pharmacy mexican online pharmacies prescription drugs or mexican pharmacy
https://images.google.co.nz/url?sa=t&url=https://mexicanpharm.online mexican mail order pharmacies
[url=https://www.google.co.il/url?q=https://mexicanpharm.online]pharmacies in mexico that ship to usa[/url] medicine in mexico pharmacies and [url=https://www.foodntours.com/user/redxvfcxsz/videos]pharmacies in mexico that ship to usa[/url] mexican rx online
prescription from canada canada online prescription or non prescription online pharmacy india
https://www.google.com.au/url?q=https://pharmacynoprescription.pro prescription from canada
[url=https://www.adminer.org/redirect/?url=http://pharmacynoprescription.pro]canada pharmacies online prescriptions[/url] medications online without prescription and [url=https://sb.diandiancom.com/home.php?mod=space&uid=3075]buying prescription drugs in india[/url] best online pharmacy without prescription
http://indianpharm.shop/# cheapest online pharmacy india
mexican pharmacy no prescription [url=https://pharmacynoprescription.pro/#]how to get prescription drugs from canada[/url] buying prescription drugs from canada online
Услуга демонтажа старых частных домов и вывоза мусора в Москве и Подмосковье от нашей компании. Мы предлагаем демонтаж и вывоз мусора в указанном регионе по доступным ценам. Наша команда гарантирует выполнение услуги снос дачного дома в течение 24 часов после заказа. Мы бесплатно оцениваем объект и консультируем клиентов.
оборотень сериал смотреть
canadian pharmacies online: canadian pharmacy online ship to usa – maple leaf pharmacy in canada
https://na-dache.pro
reliable canadian online pharmacy canadian drug pharmacy or legit canadian pharmacy
https://maps.google.com.np/url?sa=t&url=https://canadianpharm.guru reddit canadian pharmacy
[url=https://maps.google.co.jp/url?sa=t&url=https://canadianpharm.guru]canada pharmacy world[/url] canadian compounding pharmacy and [url=http://bbs.xinhaolian.com/home.php?mod=space&uid=3557976]canadian pharmacy 365[/url] reputable canadian online pharmacy
http://klubmama.ru
http://indianpharm.shop/# Online medicine order
top 10 online pharmacy in india india online pharmacy or Online medicine home delivery
https://www.google.at/url?q=http://indianpharm.shop world pharmacy india
[url=https://images.google.ms/url?sa=t&url=https://indianpharm.shop]indian pharmacy paypal[/url] online pharmacy india and [url=http://www.9kuan9.com/home.php?mod=space&uid=384060]best india pharmacy[/url] indian pharmacy
world pharmacy india: best online pharmacy india – reputable indian pharmacies
п»їbest mexican online pharmacies: mexico pharmacies prescription drugs – mexico pharmacy
http://canadianpharm.guru/# canadian pharmacy uk delivery
no prescription medication: buying prescription drugs in india – buy medication online without prescription
buy prescription drugs from india: buy prescription drugs from india – best online pharmacy india
http://pharmacynoprescription.pro/# canadian and international prescription service
medicine with no prescription: buy medications without prescriptions – pharmacy online no prescription
mexico prescription drugs online [url=https://pharmacynoprescription.pro/#]discount prescription drugs canada[/url] buying online prescription drugs
mexican drugstore online purple pharmacy mexico price list or medicine in mexico pharmacies
http://file.feelcool.org/resites.php?url=https://mexicanpharm.online/ mexican border pharmacies shipping to usa
[url=https://picturepub.net/proxy.php?link=https://mexicanpharm.online]purple pharmacy mexico price list[/url] pharmacies in mexico that ship to usa and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=228220]п»їbest mexican online pharmacies[/url] mexico drug stores pharmacies
п»їbest mexican online pharmacies: pharmacies in mexico that ship to usa – mexican pharmaceuticals online
https://pharmacynoprescription.pro/# how to order prescription drugs from canada
canadian drugs: canadian pharmacies comparison – pharmacy com canada
стоимость продвижения сайта в топ 10 цена
canadian drug pharmacy: my canadian pharmacy reviews – adderall canadian pharmacy
buying prescription drugs online canada: indian pharmacy no prescription – no prescription needed online pharmacy
exprimegranada.com
このブログのファンになりました。更新を楽しみにしています!
https://pharmacynoprescription.pro/# canada online prescription
https://mexicanpharm.online/# buying prescription drugs in mexico online
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
http://www.babelcube.com/user/jennifer-riley-1
http://www.nfomedia.com/profile?uid=rOiSbgJ
https://okwave.jp/profile/u3105189.html
https://rentry.org/ktv57nov
https://tubeteencam.com/user/pilar1969/profile
https://rentry.org/9fn3874v
https://permacultureglobal.org/users/55458-adam-west
https://tubeteencam.com/user/sceptre1984/profile
https://www.metal-archives.com/users/crystalrage1967
https://www.haikudeck.com/presentations/KGb7our6VO
reputable indian pharmacies: indian pharmacy paypal – online pharmacy india
buy medications without a prescription: online drugstore no prescription – cheap drugs no prescription
Лучшие картинки различных тематик https://stilno.site
mexican border pharmacies shipping to usa: mexican mail order pharmacies – buying from online mexican pharmacy
https://mexicanpharm.online/# buying prescription drugs in mexico
indian pharmacies safe: world pharmacy india – mail order pharmacy india
[url=https://1xbet-application-fr.com]https://1xbet-application-fr.com[/url]
Working 1xbet mirror for entering the valid website of the bookmaker. Speak it to occur to with 1xBet, let in bonuses and place online bets.
https://1xbet-application-fr.com
buying prescription drugs from canada online [url=http://pharmacynoprescription.pro/#]medications online without prescriptions[/url] buy meds online no prescription
mexican pharmacy: mexican online pharmacies prescription drugs – mexican online pharmacies prescription drugs
https://pro-dachnikov.com
mexico pharmacies prescription drugs medicine in mexico pharmacies or reputable mexican pharmacies online
https://cse.google.ms/url?sa=t&url=https://mexicanpharm.online best online pharmacies in mexico
[url=http://www.toshiki.net/x/modules/wordpress/wp-ktai.php?view=redir&url=https://mexicanpharm.online]mexican rx online[/url] buying from online mexican pharmacy and [url=https://lhgangguanwang.com/home.php?mod=space&uid=133077]medicine in mexico pharmacies[/url] mexico drug stores pharmacies
https://indianpharm.shop/# india pharmacy mail order
п»їlegitimate online pharmacies india: reputable indian pharmacies – Online medicine order
п»їbest mexican online pharmacies: mexico pharmacy – best online pharmacies in mexico
buy drugs online without a prescription prescription meds from canada or ordering prescription drugs from canada
http://images.google.co.zw/url?sa=t&url=https://pharmacynoprescription.pro buy prescription drugs online without
[url=https://maps.google.com.pr/url?sa=t&url=https://pharmacynoprescription.pro]buy drugs online without prescription[/url] no prescription medicines and [url=http://talk.dofun.cc/home.php?mod=space&uid=607706]online medication no prescription[/url] mexican prescription drugs online
https://canadianpharm.guru/# reliable canadian pharmacy reviews
qiyezp.com
이때 Fang Jifan은 즉시 Zhu Houzhao를 초대했습니다.
http://canadianpharm.guru/# canadian pharmacy phone number
[url=http://www.tamboff.ru/forum/viewtopic.php?p=7695163#7695163]http://www.tamboff.ru/forum/viewtopic.php?p=7695163#7695163[/url]
[url=http://lexa.2bb.ru/viewtopic.php?id=2198#p7198]http://lexa.2bb.ru/viewtopic.php?id=2198#p7198[/url]
best online pharmacy india: Online medicine home delivery – indian pharmacy
india pharmacy indianpharmacy com or Online medicine order
https://www.google.dj/url?q=http://indianpharm.shop reputable indian online pharmacy
[url=http://legacy.aom.org/verifymember.asp?nextpage=https://indianpharm.shop]п»їlegitimate online pharmacies india[/url] online shopping pharmacy india and [url=https://fl.liaochengquan.cn/home.php?mod=space&uid=1381017]mail order pharmacy india[/url] online shopping pharmacy india
mexican pharmacy: mexican pharmacy – mexican rx online
canadian pharmacy 24h com canada pharmacy online legit or canadian pharmacy antibiotics
https://cse.google.com.gi/url?sa=t&url=https://canadianpharm.guru canadian pharmacy no scripts
[url=http://saxonsystems.com.au/web/website.nsf/WebTell?Go=http://canadianpharm.guru]the canadian pharmacy[/url] best mail order pharmacy canada and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=228008]canadian pharmacy service[/url] ed meds online canada
indianpharmacy com: world pharmacy india – best india pharmacy
sandyterrace.com
대명궁은… 내부 모습은 신만이 아실 겁니다.
п»їbest mexican online pharmacies [url=https://mexicanpharm.online/#]buying from online mexican pharmacy[/url] mexican online pharmacies prescription drugs
https://pharmacynoprescription.pro/# canadian pharmacy online no prescription needed
pharmacy wholesalers canada: trusted canadian pharmacy – canadian online pharmacy reviews
http://slotsiteleri.guru/# en iyi slot siteleri
https://slotsiteleri.guru/# deneme veren slot siteleri
pin up casino guncel giris [url=http://pinupgiris.fun/#]pin up 7/24 giris[/url] pin up
nikontinoll.com
알고 보니 내 발 밑의 땅은 둥근 공이었다.
https://gatesofolympus.auction/# gates of olympus s?rlar?
pin-up bonanza [url=https://pinupgiris.fun/#]pin-up bonanza[/url] pin up indir
aviator giris: aviator casino oyunu – aviator hilesi ucretsiz
http://slotsiteleri.guru/# deneme bonusu veren siteler
https://slotsiteleri.guru/# en çok kazandiran slot siteleri
https://game24.space/
https://slotsiteleri.guru/# casino slot siteleri
gates of olympus demo [url=https://gatesofolympus.auction/#]gates of olympus s?rlar?[/url] gates of olympus hilesi
https://podacha-blud.com/
http://sweetbonanza.bid/# sweet bonanza hilesi
aviator oyunu 100 tl: aviator hilesi ucretsiz – aviator oyna
https://gruzchikirabotnik.ru/
guncel sweet bonanza: sweet bonanza demo oyna – sweet bonanza kazanc
https://aviatoroyna.bid/# aviator sinyal hilesi apk
deneme bonusu veren siteler [url=https://slotsiteleri.guru/#]canl? slot siteleri[/url] deneme bonusu veren siteler
Ищете профессиональных грузчиков, которые справятся с любыми задачами быстро и качественно? Наши специалисты обеспечат аккуратную погрузку, транспортировку и разгрузку вашего имущества. Мы гарантируем https://gruzchikinesti.ru, внимательное отношение к каждой детали и доступные цены на все виды работ.
https://gatesofolympus.auction/# gates of olympus hilesi
sweet bonanza demo oyna [url=https://sweetbonanza.bid/#]sweet bonanza free spin demo[/url] guncel sweet bonanza
https://slotsiteleri.guru/# güvenilir slot siteleri 2024
Мы эксперты SEO-экспертов, работающих над увеличением посещаемости и рейтинга вашего сайта в поисковых системах.
Наша команда постигли успехи в своей области и расширим ваш кругозор нашим опытом и знаниями.
Какие услуги мы предоставляем:
• [url=https://seo-prodvizhenie-ulyanovsk1.ru/]раскрутка сайтов продвижение оптимизация[/url]
• Комплексный анализ вашего сайта и разработка индивидуальной стратегии продвижения.
• Повышение эффективности контента и технических аспектов вашего сайта.
• Систематический мониторинг и анализ результатов с целью улучшения вашего онлайн-присутствия.
Подробнее [url=https://seo-prodvizhenie-ulyanovsk1.ru/]https://seo-prodvizhenie-ulyanovsk1.ru/[/url]
Уже много клиентов оценили результаты: рост посещаемости, улучшение рейтинга в поисковых запросах и, конечно, увеличение прибыли. Мы готовы предоставить вам бесплатную консультацию, для обсуждения ваших требований и разработки стратегии продвижения, соответствующей вашим целям и бюджету.
Не упустите возможность улучшить свой бизнес в онлайн-мире. Обратитесь к нам прямо сейчас.
https://gatesofolympus.auction/# gates of olympus guncel
грузоперевозки услуги грузчиков
sweet bonanza free spin demo: pragmatic play sweet bonanza – sweet bonanza demo oyna
https://slotsiteleri.guru/# bonus veren casino slot siteleri
33개 언어와 다양한 화폐를 통해 세계 시장에 제공되는 프라그마틱 플레이의 다양한 테마의 슬롯을 즐겨보세요.
프라그마틱 슬롯
프라그마틱 관련 소식 항상 주시고 있어요! 또한, 제 사이트에서도 프라그마틱에 대한 정보를 얻을 수 있어요. 함께 발전하며 지식을 나눠봐요!
https://wqeqwrwqr.weebly.com/
https://huahaiju.com/link/
https://zclzs.com/link/
https://aviatoroyna.bid/# aviator sinyal hilesi apk
en yeni slot siteleri [url=http://slotsiteleri.guru/#]deneme bonusu veren siteler[/url] slot oyun siteleri
http://aviatoroyna.bid/# aviator oyunu
sweet bonanza free spin demo [url=https://sweetbonanza.bid/#]sweet bonanza slot[/url] sweet bonanza kazanma saatleri
https://aviatoroyna.bid/# aviator oyunu
qiyezp.com
Fang Jifan의 오페라를 들으러 왔습니다.
gates of olympus demo turkce: gates of olympus demo turkce oyna – gates of olympus demo oyna
qiyezp.com
Hongzhi 황제는 무언가를 감지하고 “진지하게 말하십시오. “라고 날카롭게 말했습니다.
sweet bonanza yasal site sweet bonanza free spin demo or sweet bonanza demo oyna
http://www.agrolandis.de/24.html?&no_cache=1&tipUrl=http://sweetbonanza.bid sweet bonanza kazanc
[url=https://toolbarqueries.google.com.co/url?q=https://sweetbonanza.bid]sweet bonanza slot demo[/url] sweet bonanza demo turkce and [url=http://bbs.zhizhuyx.com/home.php?mod=space&uid=9983123]sweet bonanza mostbet[/url] sweet bonanza kazanma saatleri
http://slotsiteleri.guru/# guvenilir slot siteleri
aviator ucak oyunu [url=http://aviatoroyna.bid/#]aviator oyna slot[/url] aviator sinyal hilesi
https://gruzchikivagon.ru
1. Вибір натяжних стель – як правильно обрати?
2. Топ-5 популярних кольорів натяжних стель
3. Як зберегти чистоту натяжних стель?
4. Відгуки про натяжні стелі: плюси та мінуси
5. Як підібрати дизайн натяжних стель до інтер’єру?
6. Інноваційні технології у виробництві натяжних стель
7. Натяжні стелі з фотопечаттю – оригінальне рішення для кухні
8. Секрети вдалого монтажу натяжних стель
9. Як зекономити на встановленні натяжних стель?
10. Лампи для натяжних стель: які вибрати?
11. Відтінки синього для натяжних стель – ексклюзивний вибір
12. Якість матеріалів для натяжних стель: що обирати?
13. Крок за кроком: як самостійно встановити натяжні стелі
14. Натяжні стелі в дитячу кімнату: безпека та креативність
15. Як підтримувати тепло у приміщенні за допомогою натяжних стель
16. Вибір натяжних стель у ванну кімнату: практичні поради
17. Натяжні стелі зі структурним покриттям – тренд сучасного дизайну
18. Індивідуальність у кожному домашньому інтер’єрі: натяжні стелі з друком
19. Як обрати освітлення для натяжних стель: поради фахівця
20. Можливості дизайну натяжних стель: від класики до мінімалізму
ціна натяжних потолків [url=https://natjazhnistelitvhyn.kiev.ua/]https://natjazhnistelitvhyn.kiev.ua/[/url] .
pin up indir: pin up aviator – pin up giris
https://aviatoroyna.bid/# aviator hilesi ucretsiz
deneme bonusu veren siteler: casino slot siteleri – yeni slot siteleri
The elite online casinos in Kenya are a haven for Kenyan gaming aficionados.
https://sweetbonanza.bid/# sweet bonanza kazanma saatleri
pragmatic play sweet bonanza [url=http://sweetbonanza.bid/#]sweet bonanza yasal site[/url] sweet bonanza demo oyna
http://sweetbonanza.bid/# sweet bonanza giris
https://gruzchikietazh.ru
http://pinupgiris.fun/# pin-up casino indir
sweet bonanza taktik [url=http://sweetbonanza.bid/#]sweet bonanza indir[/url] sweet bonanza slot
https://gruzchikibaza.ru
https://pinupgiris.fun/# pin up casino
gates of olympus s?rlar?: gate of olympus hile – gates of olympus demo turkce
https://potreb-prava.com/
https://aviatoroyna.bid/# aviator oyna
https://pinupgiris.fun/# aviator pin up
sweet bonanza free spin demo [url=https://sweetbonanza.bid/#]sweet bonanza yasal site[/url] sweet bonanza demo turkce
[url=https://oazithromycin.com/]azithromycin 500 tablet[/url]
https://gatesofolympus.auction/# gates of olympus slot
yasal slot siteleri [url=http://slotsiteleri.guru/#]deneme bonusu veren siteler[/url] en cok kazandiran slot siteleri
gates of olympus guncel: gates of olympus oyna ucretsiz – gates of olympus oyna ucretsiz
pragmatic play sweet bonanza sweet bonanza or sweet bonanza 90 tl
http://www.marcomanfredini.it/radio/visualizzacollezione.php?paginanews=5&contenuto=13&quale=40&origine=https://sweetbonanza.bid sweet bonanza demo oyna
[url=http://www.irac.pe.ca/redirect.asp?url=https://sweetbonanza.bid]sweet bonanza yasal site[/url] sweet bonanza and [url=https://www.foodntours.com/user/axkmoiptan/videos]sweet bonanza demo oyna[/url] sweet bonanza siteleri
https://pinupgiris.fun/# pin up casino indir
http://pinupgiris.fun/# pin up bet
bonus veren casino slot siteleri: deneme bonusu veren siteler – deneme bonusu veren siteler
https://o-okkultizme.com
https://sweetbonanza.bid/# sweet bonanza indir
pin-up casino [url=http://pinupgiris.fun/#]aviator pin up[/url] pin up giris
gates of olympus oyna ucretsiz gates of olympus 1000 demo or gates of olympus demo
https://www.google.dk/url?q=https://gatesofolympus.auction gates of olympus
[url=https://maps.google.mv/url?q=https://gatesofolympus.auction]gates of olympus hilesi[/url] gates of olympus hilesi and [url=http://www.1moli.top/home.php?mod=space&uid=3559]gates of olympus demo turkce[/url] gates of olympus guncel
canl? slot siteleri: guvenilir slot siteleri 2024 – bonus veren slot siteleri
etsyweddingteam.com
この記事から学んだことは、非常に価値があります。感謝しています。
https://catherineasquithgallery.com
https://aviatoroyna.bid/# aviator oyunu 10 tl
bonus veren casino slot siteleri [url=http://slotsiteleri.guru/#]slot kumar siteleri[/url] deneme veren slot siteleri
заказать грузчиков недорого
https://sweetbonanza.bid/# slot oyunlari
pin-up online pin up casino guncel giris or pin-up giris
https://maps.google.ro/url?sa=t&url=https://pinupgiris.fun aviator pin up
[url=http://ssomgmt.ascd.org/profile/createsso/createsso.aspx?returnurl=http://pinupgiris.fun]pin up indir[/url] pin-up giris and [url=https://www.support-groups.org/memberlist.php?mode=viewprofile&u=140801]pin up bet[/url] pin up casino
нанять грузчиков
slot kumar siteleri: slot casino siteleri – slot oyun siteleri
http://aviatoroyna.bid/# aviator sinyal hilesi ucretsiz
deneme bonusu veren siteler [url=https://slotsiteleri.guru/#]en yeni slot siteleri[/url] slot bahis siteleri
покер онлайн
https://gatesofolympus.auction/# gates of olympus demo
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
https://ellak.gr/user/nessundorma1991/
https://www.brollopsguiden.se/medlemspresentation/86270
https://www.haikudeck.com/presentations/xFCCWFBoHR
http://www.babelcube.com/user/michael-jennings
https://www.hentai-foundry.com/user/minkx1968/profile
https://www.divephotoguide.com/user/willhunting19821973
http://www.nfomedia.com/profile?uid=rOiRddD
https://permacultureglobal.org/users/54952-william-squire
https://launchpad.net/~sumire3219501
https://www.haikudeck.com/presentations/GsdwFLtv49
https://sporty24.site/
oyun siteleri slot: slot siteleri bonus veren – slot kumar siteleri
https://gatesofolympus.auction/# gates of olympus taktik
slot casino siteleri [url=http://slotsiteleri.guru/#]slot oyun siteleri[/url] en iyi slot siteleri
aviator nas?l oynan?r: aviator oyunu 20 tl – aviator sinyal hilesi
https://sweetbonanza.bid/# sweet bonanza kazanç
http://aviatoroyna.bid/# aviator sinyal hilesi ucretsiz
guvenilir slot siteleri [url=http://slotsiteleri.guru/#]bonus veren casino slot siteleri[/url] canl? slot siteleri
sweet bonanza yasal site sweet bonanza 90 tl or sweet bonanza oyna
http://www.ra-aks.de/url?q=https://sweetbonanza.bid sweet bonanza demo oyna
[url=http://www.google.cv/url?q=http://sweetbonanza.bid]sweet bonanza yorumlar[/url] sweet bonanza hilesi and [url=http://www.1moli.top/home.php?mod=space&uid=3689]sweet bonanza mostbet[/url] sweet bonanza nas?l oynan?r
https://gatesofolympus.auction/# gates of olympus oyna
https://pinupgiris.fun/# pin up casino giris
bonus veren slot siteleri: deneme bonusu veren siteler – oyun siteleri slot
https://sweetbonanza.bid/# sweet bonanza hilesi
guvenilir slot siteleri [url=https://slotsiteleri.guru/#]slot bahis siteleri[/url] deneme bonusu veren siteler
https://acook.space
cheapest online pharmacy india [url=http://indianpharmacy.icu/#]indian pharmacy[/url] indianpharmacy com
pharmacy canadian superstore: pharmacy in canada – canadian pharmacies online
The best gaming experiences in Kenya are found at these online casinos in Kenya.
Предлагаем слуги: https://lit9.ru, демонтаж фундамента, слом домов.
cheapest online pharmacy india [url=http://indianpharmacy.icu/#]indian pharmacy[/url] world pharmacy india
buying prescription drugs in mexico online: Mexican Pharmacy Online – mexico drug stores pharmacies
http://mexicanpharmacy.shop/# pharmacies in mexico that ship to usa
canadadrugpharmacy com: Certified Canadian Pharmacy – adderall canadian pharmacy
https://sporty24.site
https://acook.space/
drugs from canada [url=https://canadianpharmacy24.store/#]Licensed Canadian Pharmacy[/url] best online canadian pharmacy
medication from mexico pharmacy: cheapest mexico drugs – purple pharmacy mexico price list
mexican border pharmacies shipping to usa [url=http://mexicanpharmacy.shop/#]mexico pharmacy[/url] pharmacies in mexico that ship to usa
mexican rx online: cheapest mexico drugs – mexican pharmaceuticals online
top online pharmacy india: Cheapest online pharmacy – mail order pharmacy india
Услуги грузчиков https://mhpereezd.ru с гарантией!
best online pharmacy india: Healthcare and medicines from India – mail order pharmacy india
canadian pharmacy online reliable canadian pharmacy or safe canadian pharmacy
http://j-page.biz/canadianpharmacy24.store canadian drug stores
[url=https://exigen.com.au/?URL=https://canadianpharmacy24.store]canadian world pharmacy[/url] canadian drug pharmacy and [url=http://www.dllaoma.com/home.php?mod=space&uid=367518]canada ed drugs[/url] rate canadian pharmacies
mexican pharmacy [url=http://mexicanpharmacy.shop/#]mexican pharmacy[/url] mexican pharmaceuticals online
https://mhpereezd.ru
https://indianpharmacy.icu/# top online pharmacy india
online pharmacy india: Generic Medicine India to USA – best online pharmacy india
purple pharmacy mexico price list: cheapest mexico drugs – mexican rx online
mexican online pharmacies prescription drugs: Online Pharmacies in Mexico – buying from online mexican pharmacy
pet meds without vet prescription canada: Licensed Canadian Pharmacy – best mail order pharmacy canada
canada cloud pharmacy [url=https://canadianpharmacy24.store/#]Prescription Drugs from Canada[/url] canada cloud pharmacy
medication from mexico pharmacy: mexican pharmacy – mexican online pharmacies prescription drugs
prescription drugs canada buy online certified canadian pharmacy or reliable canadian pharmacy
http://www.google.com.pk/url?q=https://canadianpharmacy24.store legal to buy prescription drugs from canada
[url=http://bigtorrent-ua.com/away.php?to=canadianpharmacy24.store]canada drugs online reviews[/url] cheap canadian pharmacy online and [url=http://jzmetin.cn/bbs/home.php?mod=space&uid=273770]canadian pharmacy in canada[/url] canadian drug
india pharmacy mail order: Generic Medicine India to USA – top online pharmacy india
mexican rx online: Mexican Pharmacy Online – п»їbest mexican online pharmacies
india pharmacy mail order [url=https://indianpharmacy.icu/#]Generic Medicine India to USA[/url] п»їlegitimate online pharmacies india
프라그마틱 슬롯을 무료로 플레이하면서 즐거움을 찾아보세요.
프라그마틱
프라그마틱의 게임을 플레이하면 항상 긴장감 넘치고 즐거운 시간을 보낼 수 있어 좋아요. 여기서 더 많은 이야기를 들려주세요!
https://lotodarts.com/link/
https://www.vamiveta.com/
https://doggggqwe.weebly.com/
india pharmacy: indian pharmacy – india pharmacy mail order
canadian drugs: Certified Canadian Pharmacy – the canadian drugstore
Throughout the awesome design of things you’ll get an A+ with regard to hard work. Where exactly you confused us ended up being in all the particulars. As as the maxim goes, details make or break the argument.. And it could not be much more true at this point. Having said that, permit me tell you precisely what did deliver the results. Your writing can be highly persuasive which is possibly the reason why I am taking the effort to opine. I do not really make it a regular habit of doing that. Next, despite the fact that I can certainly see the jumps in reason you make, I am not sure of exactly how you seem to connect your ideas that help to make the actual final result. For the moment I shall subscribe to your position but wish in the near future you connect your facts better.
mexico drug stores pharmacies mexico drug stores pharmacies or buying from online mexican pharmacy
https://maps.google.gp/url?sa=t&url=https://mexicanpharmacy.shop mexican drugstore online
[url=https://www.google.com.fj/url?q=https://mexicanpharmacy.shop]mexico drug stores pharmacies[/url] mexico drug stores pharmacies and [url=http://80tt1.com/home.php?mod=space&uid=701838]mexican border pharmacies shipping to usa[/url] mexican drugstore online
http://canadianpharmacy24.store/# cheapest pharmacy canada
This is the right blog for anyone who wants to find out about this topic. You realize so much its almost hard to argue with you (not that I actually would want…HaHa). You definitely put a new spin on a topic thats been written about for years. Great stuff, just great!
rate canadian pharmacies: pharmacy wholesalers canada – best canadian pharmacy online
canadapharmacyonline com [url=http://canadianpharmacy24.store/#]Licensed Canadian Pharmacy[/url] canadian pharmacy meds reviews
cheapest online pharmacy india: world pharmacy india – india pharmacy mail order
Online medicine home delivery indianpharmacy com or indian pharmacy
https://www.google.gy/url?q=https://indianpharmacy.icu indian pharmacy
[url=https://toolbarqueries.google.com.mx/url?q=http://indianpharmacy.icu]п»їlegitimate online pharmacies india[/url] indian pharmacy and [url=http://ckxken.synology.me/discuz/home.php?mod=space&uid=15615]world pharmacy india[/url] top online pharmacy india
mexico drug stores pharmacies buying from online mexican pharmacy or п»їbest mexican online pharmacies
https://www.google.st/url?q=https://mexicanpharmacy.shop buying prescription drugs in mexico
[url=https://weburg.net/redirect?fromru=1&url=mexicanpharmacy.shop/]mexico drug stores pharmacies[/url] mexican border pharmacies shipping to usa and [url=http://www.0551gay.com/space-uid-86090.html]buying prescription drugs in mexico[/url] mexican pharmacy
https://gruzchikibaza.ru/
mexico drug stores pharmacies: cheapest mexico drugs – buying prescription drugs in mexico
purple pharmacy mexico price list: Mexican Pharmacy Online – mexico drug stores pharmacies
top online pharmacy india [url=https://indianpharmacy.icu/#]indian pharmacy[/url] indian pharmacy
http://canadianpharmacy24.store/# legitimate canadian mail order pharmacy
mexican drugstore online: Mexican Pharmacy Online – purple pharmacy mexico price list
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
https://chyoa.com/user/heliotopia1980
https://www.quia.com/profiles/marymorales569
https://www.obesityhelp.com/members/profusser1990/about_me/
https://ellak.gr/user/pesokot1992/
https://imageevent.com/darksid1991
https://prodawec1999.diary.ru/
https://rentry.org/paxczn2s
https://chyoa.com/user/darii1976
https://haveagood.holiday/users/338293
https://www.metal-archives.com/users/befor1998
best online pharmacies in mexico: Online Pharmacies in Mexico – mexico pharmacies prescription drugs
toasterovensplus.com
素敵な記事をありがとうございます。大いに参考になりました!
real canadian pharmacy: Prescription Drugs from Canada – canadian pharmacy sarasota
canadian pharmacy online ship to usa [url=https://canadianpharmacy24.store/#]northwest pharmacy canada[/url] canada discount pharmacy
https://gruzchikinesti.ru
1. Вибір натяжних стель: як вибрати ідеальний варіант?
2. Модні тренди натяжних стель на поточний сезон
3. Які переваги мають натяжні стелі порівняно зі звичайними?
4. Як підібрати кольори для натяжної стелі у квартирі?
5. Секрети догляду за натяжними стелями: що потрібно знати?
6. Як зробити вибір між матовими та глянцевими натяжними стелями?
7. Натяжні стелі в інтер’єрі: як вони змінюють приміщення?
8. Натяжні стелі для ванної кімнати: плюси та мінуси
9. Як підняти стеля візуально за допомогою натяжної конструкції?
10. Як вибрати правильний дизайн натяжної стелі для кухні?
11. Інноваційні технології виробництва натяжних стель: що варто знати?
12. Чому натяжні стелі вибирають для офісних приміщень?
13. Натяжні стелі з фотопринтом: які переваги цієї технології?
14. Дизайнерські рішення для натяжних стель: ідеї для втілення
15. Хімічні реагенти в складі натяжних стель: безпека та якість
16. Як вибрати натяжну стелю для дитячої кімнати: поради батькам
17. Які можливості для дизайну приміщень відкривають натяжні стелі?
18. Як впливає вибір матеріалу на якість натяжної стелі?
19. Інструкція з монтажу натяжних стель власноруч: крок за кроком
20. Натяжні стелі як елемент екстер’єру будівлі: переваги та недоліки
натяжні стелі матеріал [url=http://www.natjazhnistelifvgtg.lviv.ua]http://www.natjazhnistelifvgtg.lviv.ua[/url] .
https://zithromaxall.shop/# where to get zithromax over the counter
https://amoxilall.com/# where can you get amoxicillin
https://gruzchikibol.ru
where can i get clomid [url=https://clomidall.com/#]cost generic clomid no prescription[/url] rx clomid
https://zithromaxall.com/# zithromax 250 price
https://gruzchikivrn.ru
https://clomidall.shop/# where to get cheap clomid price
average cost of generic zithromax [url=http://zithromaxall.shop/#]buy zithromax online with mastercard[/url] zithromax online
1. Вибір натяжних стель – як правильно обрати?
2. Топ-5 популярних кольорів натяжних стель
3. Як зберегти чистоту натяжних стель?
4. Відгуки про натяжні стелі: плюси та мінуси
5. Як підібрати дизайн натяжних стель до інтер’єру?
6. Інноваційні технології у виробництві натяжних стель
7. Натяжні стелі з фотопечаттю – оригінальне рішення для кухні
8. Секрети вдалого монтажу натяжних стель
9. Як зекономити на встановленні натяжних стель?
10. Лампи для натяжних стель: які вибрати?
11. Відтінки синього для натяжних стель – ексклюзивний вибір
12. Якість матеріалів для натяжних стель: що обирати?
13. Крок за кроком: як самостійно встановити натяжні стелі
14. Натяжні стелі в дитячу кімнату: безпека та креативність
15. Як підтримувати тепло у приміщенні за допомогою натяжних стель
16. Вибір натяжних стель у ванну кімнату: практичні поради
17. Натяжні стелі зі структурним покриттям – тренд сучасного дизайну
18. Індивідуальність у кожному домашньому інтер’єрі: натяжні стелі з друком
19. Як обрати освітлення для натяжних стель: поради фахівця
20. Можливості дизайну натяжних стель: від класики до мінімалізму
фотодрук натяжні стелі [url=http://www.natjazhnistelitvhyn.kiev.ua]http://www.natjazhnistelitvhyn.kiev.ua[/url] .
http://prednisoneall.com/# prednisone 10 mg tablet
https://amoxilall.shop/# amoxicillin 875 125 mg tab
http://clomidall.com/# where can i buy cheap clomid pill
where to buy amoxicillin over the counter [url=http://amoxilall.com/#]where to buy amoxicillin 500mg[/url] cheap amoxicillin 500mg
where to buy amoxicillin over the counter order amoxicillin online uk or amoxicillin price canada
https://images.google.co.uz/url?q=https://amoxilall.shop buy amoxicillin online mexico
[url=https://www.anonymz.com/?http://amoxilall.shop/%5Dbuy amoxil[/url] amoxicillin 500mg over the counter and [url=http://www.0551gay.com/space-uid-87564.html]amoxicillin 875 125 mg tab[/url] how to get amoxicillin over the counter
Дизайнерский проект
3. Просторный дом из бруса 9х12: идеальное жилье для семьи
дом из бруса 9х12 [url=https://domizbrusa9x12spb.ru/]https://domizbrusa9x12spb.ru/[/url] .
Атмосфера волшебства и красоты
12. Эксклюзивный дом из бруса 9х12: индивидуальный подход
одноэтажный дом из бруса 9х12 [url=https://domizbrusa9x12spb.ru/]https://domizbrusa9x12spb.ru/[/url] .
https://zithromaxall.com/# zithromax capsules australia
Уютная атмосфера и комфорт
9. Уникальный дом из бруса 9х12: тепло и уют
дом из бруса 9х12 [url=https://domizbrusa9x12spb.ru/]https://domizbrusa9x12spb.ru/[/url] .
zithromax online australia [url=http://zithromaxall.com/#]can i buy zithromax online[/url] how to get zithromax
amoxicillin capsule 500mg price: amoxicillin 500mg over the counter – amoxicillin 500mg pill
https://prednisoneall.com/# buy prednisone with paypal canada
демонтаж москва
https://demontagmoskva.ru/
http://zithromaxall.com/# order zithromax over the counter
https://amoxilall.com/# amoxicillin without a doctors prescription
medicine amoxicillin 500 [url=https://amoxilall.shop/#]amoxicillin online pharmacy[/url] amoxicillin 500 mg without a prescription
https://gruzchikivrn.ru/
amoxicillin 500mg no prescription: generic amoxicillin – buy amoxicillin online no prescription
https://clomidall.com/# can i order cheap clomid without rx
cost of amoxicillin amoxicillin canada price or amoxicillin 500 mg price
http://toolbarqueries.google.as/url?sa=i&url=https://amoxilall.shop where can you buy amoxicillin over the counter
[url=https://www.google.mw/url?q=https://amoxilall.shop]can you buy amoxicillin uk[/url] amoxicillin cost australia and [url=https://forexzloty.pl/members/371559-gljdfoueyx]amoxicillin no prescription[/url] amoxicillin from canada
purchase zithromax z-pak where can i get zithromax over the counter or zithromax 250 mg
https://images.google.co.th/url?sa=t&url=https://zithromaxall.shop zithromax 500 price
[url=https://image.google.vg/url?q=https://zithromaxall.shop]where can i buy zithromax in canada[/url] zithromax coupon and [url=http://www.0551gay.com/space-uid-87787.html]zithromax online no prescription[/url] how to get zithromax online
where to buy prednisone in australia [url=https://prednisoneall.shop/#]prednisone 10 mg brand name[/url] prednisone 20 mg
http://zithromaxall.com/# buy zithromax online
воєнторг
2. Где купить армейские снаряжение
магазини воєнторг київ [url=https://voentorgaseh.kiev.ua/]військовий магазин онлайн[/url] .
http://prednisoneall.shop/# prednisone 2 mg daily
1. Почему берцы – это обязательный элемент стиля?
2. Как выбрать идеальные берцы для осеннего гардероба?
3. Тренды сезона: кожаные берцы или замшевые?
4. 5 способов носить берцы с платьем
5. Какие берцы выбрать для повседневного образа?
6. Берцы на платформе: комфорт и стиль в одном
7. Какие берцы будут актуальны в этом году?
8. Маст-хэв сезона: военные берцы в стиле милитари
9. 10 вариантов сочетания берцов с джинсами
10. Зимние берцы: как выбрать модель для холодного сезона
11. Элегантные берцы на каблуке: идеальный вариант для офиса
12. Секреты ухода за берцами: как сохранить первоначальный вид?
13. С какой юбкой носить берцы: советы от стилистов
14. Как подобрать берцы под фасон брюк?
15. Берцы на шнуровке: стильный акцент в образе
16. Берцы-челси: универсальная модель для любого стиля
17. С чем носить берцы на плоской подошве?
18. Берцы с ремешками: акцент на деталях
19. Как выбрать берцы для прогулок по городу?
20. Топ-5 брендов берцев: качество и стиль в одном
купити берці військові [url=https://bercifrdt.kiev.ua/]купити берці тактичні[/url] .
http://amoxilall.com/# amoxicillin price canada
воєнторг
11. Надежное снаряжение для армии
військовий магазин [url=https://voentorgaseh.kiev.ua/]магазин тактичного одягу[/url] .
zithromax online usa: zithromax 1000 mg online – zithromax buy
where buy generic clomid price [url=http://clomidall.shop/#]can i purchase cheap clomid without rx[/url] buying generic clomid
프라그마틱 게임은 선도적인 iGaming 콘텐츠 제공 업체입니다. 모바일 중심 다양한 포트폴리오와 고품질 엔터테인먼트를 자랑합니다.
프라그마틱 슬롯 무료 체험
프라그마틱의 게임은 정말 다양한데, 어떤 테마의 게임을 가장 좋아하나요? 나눠주세요!
https://www.12315oi.cn/
https://www.ashspurr.com
https://www.ivermectininstock.com/
https://prednisoneall.com/# buy prednisone 10 mg
1. Почему берцы – это обязательный элемент стиля?
2. Как выбрать идеальные берцы для осеннего гардероба?
3. Тренды сезона: кожаные берцы или замшевые?
4. 5 способов носить берцы с платьем
5. Какие берцы выбрать для повседневного образа?
6. Берцы на платформе: комфорт и стиль в одном
7. Какие берцы будут актуальны в этом году?
8. Маст-хэв сезона: военные берцы в стиле милитари
9. 10 вариантов сочетания берцов с джинсами
10. Зимние берцы: как выбрать модель для холодного сезона
11. Элегантные берцы на каблуке: идеальный вариант для офиса
12. Секреты ухода за берцами: как сохранить первоначальный вид?
13. С какой юбкой носить берцы: советы от стилистов
14. Как подобрать берцы под фасон брюк?
15. Берцы на шнуровке: стильный акцент в образе
16. Берцы-челси: универсальная модель для любого стиля
17. С чем носить берцы на плоской подошве?
18. Берцы с ремешками: акцент на деталях
19. Как выбрать берцы для прогулок по городу?
20. Топ-5 брендов берцев: качество и стиль в одном
купити берці військові [url=https://bercifrdt.kiev.ua/]купити берці тактичні[/url] .
https://prednisoneall.com/# prednisone 40mg
where to get clomid [url=https://clomidall.shop/#]where can i get clomid prices[/url] how to get cheap clomid prices
http://zithromaxall.shop/# generic zithromax 500mg india
amoxicillin cost australia can i purchase amoxicillin online or buy cheap amoxicillin
https://forums2.battleon.com/f/interceptor.asp?dest=http://amoxilall.shop/ buy amoxicillin 500mg online
[url=http://images.google.sc/url?q=http://amoxilall.shop]amoxicillin 500 mg brand name[/url] amoxicillin pills 500 mg and [url=http://www.donggoudi.com/home.php?mod=space&uid=294299]can you buy amoxicillin over the counter[/url] amoxicillin online without prescription
where can i order prednisone 20mg: prednisone 20 – prednisone brand name in usa
http://clomidall.shop/# where can i get cheap clomid pill
prednisone in canada [url=https://prednisoneall.com/#]prednisone 50mg cost[/url] prednisone 10 tablet
can i order cheap clomid for sale how to get generic clomid without prescription or where can i get cheap clomid without prescription
https://images.google.gr/url?q=https://clomidall.shop cost of generic clomid without prescription
[url=https://www.google.com.vc/url?q=http://clomidall.shop]how can i get clomid without insurance[/url] can i buy clomid without a prescription and [url=http://talk.dofun.cc/home.php?mod=space&uid=667228]can i get clomid without prescription[/url] get cheap clomid no prescription
http://clomidall.com/# get cheap clomid without a prescription
최신 프라그마틱 게임은 iGaming 분야에서 혁신적이고 표준화된 콘텐츠를 제공하는 선도적인 공급 업체입니다.
프라그마틷
프라그마틱 슬롯에 대한 이해가 높아지네요! 제 사이트에서도 유용한 프라그마틱 정보를 찾아볼 수 있어요. 함께 공유하고 발전해봐요!
https://www.12315zg.cn/
https://adanaport.com/link/
http://www.ivermectininstock.com/
Cialis 20mg price: Generic Tadalafil 20mg price – Cialis without a doctor prescription
п»їkamagra [url=https://kamagraiq.com/#]kamagra best price[/url] buy Kamagra
http://sildenafiliq.com/# Sildenafil Citrate Tablets 100mg
Cialis without a doctor prescription: tadalafil iq – Buy Tadalafil 20mg
Cialis 20mg price in USA [url=http://tadalafiliq.shop/#]Generic Tadalafil 20mg price[/url] Tadalafil Tablet
Kamagra 100mg price: Sildenafil Oral Jelly – sildenafil oral jelly 100mg kamagra
http://sildenafiliq.xyz/# cheapest viagra
http://tadalafiliq.com/# Buy Cialis online
Kamagra Oral Jelly: Kamagra 100mg – sildenafil oral jelly 100mg kamagra
Cialis over the counter [url=https://tadalafiliq.shop/#]cheapest cialis[/url] п»їcialis generic
thebuzzerpodcast.com
“우리는 전차, 말, 보트가 필요합니다.” 작은 녀석들이 차례로 말했습니다.
cougarsbkjersey.com
素晴らしい内容と分析でした。大変勉強になります。
best price for viagra 100mg: buy viagra online – viagra canada
http://sildenafiliq.xyz/# buy Viagra online
п»їkamagra [url=https://kamagraiq.shop/#]Kamagra Oral Jelly Price[/url] cheap kamagra
sildenafil oral jelly 100mg kamagra: Kamagra Iq – sildenafil oral jelly 100mg kamagra
https://kamagraiq.com/# п»їkamagra
Cheapest Sildenafil online: viagra canada – Viagra tablet online
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
https://imageevent.com/kisska121986
https://imageevent.com/tomoko1955
https://imageevent.com/pic1951
https://imageevent.com/nolaghere1971
https://haveagood.holiday/users/338262
https://cannabis.net/user/146511
https://www.hentai-foundry.com/user/hassel1979/profile
https://www.haikudeck.com/presentations/GGOBElXupc
http://www.nfomedia.com/profile?uid=rOiQgcI
https://www.dnnsoftware.com/activity-feed/my-profile/userid/3187821
Cheap generic Viagra online [url=https://sildenafiliq.com/#]Cheap Sildenafil 100mg[/url] best price for viagra 100mg
https://sildenafiliq.xyz/# viagra without prescription
Cialis without a doctor prescription: buy cialis pill – buy cialis pill
https://diplom-sdan.ru/
https://tadalafiliq.shop/# Generic Cialis without a doctor prescription
buy viagra here: best price on viagra – Order Viagra 50 mg online
sildenafil 50 mg price Order Viagra 50 mg online or buy Viagra online
http://www.kansai-sheet.jp/cgi-local/contact_check.cgi?name=Trevorhox&tantou=&mail=trevoridest%40sildenafiliq.com&mail2=trevoridest%40sildenafiliq.com&comment=+Its+such+as+you+learn+my+thoughts%21+You+appear+to+know+so+much+approximately+this%2C+such+as+you+wrote+the+ebook+in+it+or+something.+I+feel+that+you+just+can+do+with+a+few+%25+to+pressure+the+message+house+a+little+bit%2C+but+instead+of+that%2C+this+is+fantastic+blog.+A+fantastic+read.+I+will+definitely+be+back.+buy+cialis+online+%0D%0A+%0D%0Acutting+a+cialis+pill+in+half+cialis+generic+dur%84Ce+d%27effet+cialis+cialis+generic+cialis+reflusso+%0D%0A+%0D%0Ayoung+men+take+viagra+viagra+uk+viagra+cost+compare+viagra+tesco+which+is+best+viagra+livetra+cialis+%0D%0A+%0D%0Acanadian+online+pharmacy+canadian+pharmacies+that+ship+to+us+online+canadian+discount+pharmacy+canada+online+pharmacies+online+pharmacy+reviews&submit=m%81hF%20 Cheap Sildenafil 100mg
[url=https://www.spsi.biz/Redirect.aspx?destination=https://sildenafiliq.com/]Cheap Sildenafil 100mg[/url] Viagra Tablet price and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3101382]sildenafil 50 mg price[/url] Viagra Tablet price
Cheap Sildenafil 100mg [url=https://sildenafiliq.com/#]sildenafil iq[/url] Order Viagra 50 mg online
Kamagra Oral Jelly: Kamagra Iq – Kamagra 100mg price
http://sildenafiliq.com/# Viagra online price
https://tadalafiliq.shop/# Generic Tadalafil 20mg price
https://diplomnash.ru/
over the counter sildenafil [url=http://sildenafiliq.com/#]sildenafil iq[/url] Generic Viagra online
super kamagra: Kamagra Oral Jelly – Kamagra tablets
http://sildenafiliq.xyz/# viagra canada
buy kamagra online usa: п»їkamagra – Kamagra 100mg price
https://sildenafiliq.com/# best price for viagra 100mg
sildenafil oral jelly 100mg kamagra: Kamagra Iq – buy kamagra online usa
Kamagra 100mg price [url=https://kamagraiq.com/#]Sildenafil Oral Jelly[/url] Kamagra tablets
https://kursovaya-student.ru/
Tadalafil Tablet: Generic Tadalafil 20mg price – Buy Tadalafil 10mg
qiyezp.com
폭발 후 충격은 크지 않았지만 소리는 수도 전체에 충격을 주었다.
http://kamagraiq.com/# cheap kamagra
buy Viagra over the counter Viagra generic over the counter or Generic Viagra for sale
https://www.google.co.za/url?q=https://sildenafiliq.com п»їBuy generic 100mg Viagra online
[url=https://60.viromin.com/index/d1?diff=0&utm_clickid=9sg408wsws80o8o8&aurl=http://sildenafiliq.com]Buy Viagra online cheap[/url] viagra canada and [url=http://80tt1.com/home.php?mod=space&uid=741176]Cheap Viagra 100mg[/url] Sildenafil 100mg price
https://breaking-bad-serial.online/
https://tadalafiliq.shop/# Cialis over the counter
Buy Viagra online cheap: buy viagra online – Viagra tablet online
Добрый день всем!
[b]Купить диплом в Новошахтинске[/b]
Обратитесь к дипломам, и ваш новый диплом станет первой ступенью на пути к вершинам карьерных достижений. Основные знания приобретаются на практике, а значение образования сводится лишь к тому, чтобы получить диплом.https://saksx-diploms-srednee24.com/ Фирма, в которой работники окончили курсы повышения квалификаций имеет в рыночной среде больше конкурентных преимуществ.
Buy Tadalafil 20mg [url=https://tadalafiliq.shop/#]tadalafil iq[/url] Cheap Cialis
Kamagra 100mg price Kamagra 100mg or Kamagra 100mg price
https://www.google.pt/url?sa=t&url=https://kamagraiq.shop Kamagra tablets
[url=https://images.google.pt/url?sa=t&url=https://kamagraiq.shop]Kamagra Oral Jelly[/url] Kamagra 100mg and [url=http://ckxken.synology.me/discuz/home.php?mod=space&uid=17644]buy kamagra online usa[/url] Kamagra 100mg price
https://tadalafiliq.shop/# Tadalafil Tablet
https://kursovaya-study.ru/
Cialis over the counter: cialis best price – cialis generic
thebuzzerpodcast.com
결국… 그는 항상 대가를 바라지 않고 선행을 하는 사람이었습니다.
http://tadalafiliq.com/# Cheap Cialis
Cheap generic Viagra online [url=http://sildenafiliq.xyz/#]best price on viagra[/url] viagra without prescription
cheapest viagra: Viagra tablet online – Sildenafil 100mg price
Buy Viagra online cheap: cheapest viagra – Cheap Sildenafil 100mg
http://sildenafiliq.xyz/# cheapest viagra
https://kamagraiq.shop/# Kamagra 100mg price
Cialis 20mg price Cialis 20mg price in USA or buy cialis pill
http://j-page.biz/tadalafiliq.shop Tadalafil price
[url=http://muravlenko.yanao.ru/forum/away.php?s=http://tadalafiliq.shop]buy cialis pill[/url] Generic Cialis price and [url=http://jiangzhongyou.net/space-uid-522809.html]cialis for sale[/url] Cialis 20mg price
qiyezp.com
모든 범죄가 마침내 확인된 후 각 사건의 세부 사항이 확정되기 시작했습니다.
https://kvartiruise.ru/
cheapest viagra: best price on viagra – Cheap Sildenafil 100mg
cialis for sale Buy Tadalafil 5mg or Cialis 20mg price in USA
https://www.nyumon.net/script/sc/redirect.php?id=393&url=https://tadalafiliq.com Generic Cialis price
[url=https://images.google.com.af/url?sa=t&url=https://tadalafiliq.com]п»їcialis generic[/url] cheapest cialis and [url=http://www.tmml.top/home.php?mod=space&uid=75255]Tadalafil Tablet[/url] Buy Tadalafil 20mg
Kamagra Oral Jelly [url=http://kamagraiq.com/#]Kamagra Iq[/url] cheap kamagra
http://tadalafiliq.com/# Cheap Cialis
http://mexicanpharmgrx.com/# mexican rx online
rate canadian pharmacies [url=http://canadianpharmgrx.com/#]Certified Canadian pharmacies[/url] canadian pharmacy meds review
https://kvartiruless.ru/
best online pharmacy india: indian pharmacy – reputable indian online pharmacy
http://indianpharmgrx.com/# indianpharmacy com
https://kupikvartiruor.ru/
mail order pharmacy india: indian pharmacy paypal – online shopping pharmacy india
online pharmacy india [url=http://indianpharmgrx.shop/#]indian pharmacy delivery[/url] top 10 pharmacies in india
Подробный обзор
17. BMW: как выбрать идеальный двигатель для своего автомобиля
x3 bmw [url=https://avtosalonbmwftnz.dp.ua/]bmw x3 m competition[/url] .
canadian world pharmacy canadian pharmacy or <a href=" http://ns.km1003.keymachine.de/php.php?a%5B%5D=cialis+without+doctor+prescription “>canada pharmacy online
https://www.google.com.uy/url?sa=t&url=https://canadianpharmgrx.com canadian pharmacy online store
[url=https://images.google.mw/url?sa=t&url=https://canadianpharmgrx.com]onlinepharmaciescanada com[/url] reputable canadian online pharmacy and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3103767]canada drugs online reviews[/url] canadian pharmacy 365
certified canadian international pharmacy: best canadian online pharmacy reviews – canada drug pharmacy
Оценка показателей
13. BMW: традиции и современность в дизайне
bmw x6 2022 [url=https://avtosalonbmwftnz.dp.ua/]bmw x 6[/url] .
top online pharmacy india [url=http://indianpharmgrx.com/#]Healthcare and medicines from India[/url] top 10 online pharmacy in india
https://mexicanpharmgrx.shop/# best mexican online pharmacies
https://kvartiruyze.ru/
п»їbest mexican online pharmacies: Pills from Mexican Pharmacy – mexican rx online
https://canadianpharmgrx.xyz/# canadian online pharmacy
Привет, дорогой читатель!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в сжатые сроки? Это действительно требует большой ответственности и усилий, но важно не сдаваться и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет эффективно искать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на [url=https://rudik-diploms365.com/]купить диплом ссср[/url], это проверенный источник!
https://gruppa365-diploms-srednee.com/
купить диплом бакалавра
купить диплом института
купить диплом колледжа
купить диплом Вуза
купить диплом цена
Желаю любому отличных оценок!
buying from online mexican pharmacy [url=https://mexicanpharmgrx.shop/#]online pharmacy in Mexico[/url] buying prescription drugs in mexico online
https://kvartirulyspb.ru/
canada pharmacy reviews [url=http://canadianpharmgrx.xyz/#]My Canadian pharmacy[/url] canadian online pharmacy reviews
top 10 online pharmacy in india: Generic Medicine India to USA – cheapest online pharmacy india
legit canadian online pharmacy canadian pharmacies online or canadian pharmacy 24h com safe
http://www.thienantech.com/?http://canadianpharmgrx.com best canadian pharmacy
[url=https://maps.google.co.zm/url?q=https://canadianpharmgrx.com]reputable canadian online pharmacies[/url] canadian valley pharmacy and [url=http://wuyuebanzou.com/home.php?mod=space&uid=505060]canadian family pharmacy[/url] ed drugs online from canada
my canadian pharmacy review: My Canadian pharmacy – canadian family pharmacy
гостиницы сочи
https://mexicanpharmgrx.com/# mexican online pharmacies prescription drugs
отели в сочи с бассейном
[url=https://avtosalonbmwftnz.dp.ua]купити bmw[/url]
Купить ценогенетический BMW 2024 года в Украине по лучшей стоимости язык официального дилера. Тест-драйв, хеджирование, авансирование, акции и спецпредложения.
офіційний дилер бмв
mexican drugstore online: online pharmacy in Mexico – pharmacies in mexico that ship to usa
canada drugs online review [url=http://canadianpharmgrx.com/#]Pharmacies in Canada that ship to the US[/url] canadian pharmacy online reviews
https://kvartiruerspb.ru/
https://indianpharmgrx.shop/# legitimate online pharmacies india
nikontinoll.com
그러나 왕자는 먼저 암살당했지만 반쯤 겁에 질려 죽었습니다.그런데 지금 증조할머니가 화를 내시는데 이건 정말 안타깝습니다.
What is a Sugar Defender? Sugar Shield could be an affront affectability enhancement product that effectively supports stable blood sugar levels.
toasterovensplus.com
素晴らしい記事!共有せずにはいられませんでした。
mexican online pharmacies prescription drugs mexico drug stores pharmacies or mexican mail order pharmacies
https://2ip.ru/lookup/?ip=mexicanpharmgrx.com best online pharmacies in mexico
[url=https://maps.google.ki/url?q=https://mexicanpharmgrx.com]mexico drug stores pharmacies[/url] buying from online mexican pharmacy and [url=https://www.warshipsfaq.ru/user/gvkdkybmbn]mexico drug stores pharmacies[/url] reputable mexican pharmacies online
http://mexicanpharmgrx.shop/# mexican pharmacy
mexican rx online [url=https://mexicanpharmgrx.shop/#]mexican pharmacy[/url] mexican border pharmacies shipping to usa
[url=https://azithromycinmds.com/]zithromax online usa[/url]
buy prescription drugs from india: Generic Medicine India to USA – reputable indian online pharmacy
https://mexicanpharmgrx.shop/# mexican drugstore online
sandyterrace.com
이때 Hongzhi 황제는 Fang Jifan의 말을 이해하지 못하고 당황했습니다.
best canadian pharmacy canadian pharmacies or canadian pharmacy reviews
https://images.google.nr/url?q=https://canadianpharmgrx.com drugs from canada
[url=https://www.google.co.id/url?sa=t&url=https://canadianpharmgrx.com]cheapest pharmacy canada[/url] legitimate canadian pharmacy online and [url=http://www.tmml.top/home.php?mod=space&uid=76759]medication canadian pharmacy[/url] canadian pharmacy uk delivery
https://zhkstroyspb.ru/
buying prescription drugs in mexico [url=https://mexicanpharmgrx.shop/#]Pills from Mexican Pharmacy[/url] medicine in mexico pharmacies
online canadian pharmacy: CIPA approved pharmacies – canadian online pharmacy
https://mexicanpharmgrx.com/# best mexican online pharmacies
Online medicine home delivery buy medicines online in india or mail order pharmacy india
http://www.redcruise.com/petitpalette/iframeaddfeed.php?url=http://indianpharmgrx.com top 10 pharmacies in india
[url=https://www.google.pn/url?q=https://indianpharmgrx.com]indian pharmacy paypal[/url] top 10 pharmacies in india and [url=https://bbs.tlcq666.com/home.php?mod=space&uid=26110]india pharmacy[/url] top online pharmacy india
best india pharmacy: indian pharmacy delivery – world pharmacy india
Hello very nice web site!! Man .. Excellent .. Amazing .. I’ll bookmark your blog and take the feeds additionally?KI’m glad to find numerous useful information right here within the submit, we need develop extra techniques on this regard, thank you for sharing. . . . . .
плинтус купить москва [url=https://alyuminievyj-plintus-msk.ru/]плинтус купить москва[/url] .
https://zhkstroykaspb.ru/
https://indianpharmgrx.shop/# india pharmacy
buy medicines online in india: indian pharmacy delivery – Online medicine order
[url=https://metformindi.com/]how to order metform onlline[/url]
Подробное руководство
2. Секреты монтажа гипсокартона: шаг за шагом инструкция
3. Гипсокартонные конструкции: основные виды и их преимущества
4. Как сэкономить при покупке гипсокартона: лучшие способы
5. Простые способы обработки гипсокартона: советы от профессионалов
6. Интересные идеи использования гипсокартона в интерьере
7. Все, что вам нужно знать о гипсокартоне: полезная информация
8. Гипсокартон: обзор популярных брендов и их характеристики
9. Плюсы и минусы гипсокартона: как правильно выбрать материал
10. Как сделать ровные стены с помощью гипсокартона: секреты и советы
11. Гипсокартонные потолки: виды и технологии монтажа
12. Декорирование гипсокартона: идеи для творческого подхода
13. Гипсокартон в дизайне интерьера: современные тренды и решения
14. Преимущества гипсокартона перед другими строительными материалами
15. Как выбрать правильный инструмент для работы с гипсокартоном
16. Гипсокартон: надежный материал для обустройства дома
17. Гипсокартон как элемент декора: необычные способы применения
18. Технологии монтажа гипсокартона: лучшие практические советы
19. История и развитие гипсокартона: открытия и достижения
20. Строительство с использованием гипсокартона: основные этапы и рекомендации
профиль для гипсокартона [url=https://gipsokarton-moskva.ru/]гипсокартон купить в москве[/url] .
canadian pharmacies [url=http://canadianpharmgrx.xyz/#]canadian drug stores[/url] pet meds without vet prescription canada
алюминиевый плинтус купить москва [url=https://alyuminievyj-plintus-msk.ru/]алюминиевый плинтус купить[/url] .
https://kvartiruekb.ru/
http://indianpharmgrx.shop/# best online pharmacy india
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
https://permacultureglobal.org/users/55147-kara-johnston
https://permacultureglobal.org/users/54627-rod-arellano
https://ellak.gr/user/nessundorma1991/
https://anotepad.com/notes/madgtm92
https://www.divephotoguide.com/user/dfgk1968
https://www.hentai-foundry.com/user/kooot1964/profile
https://www.quia.com/profiles/anwallach
https://haveagood.holiday/users/339799
https://www.quia.com/profiles/christinacampbell
https://www.brollopsguiden.se/medlemspresentation/86032
1. Как выбрать идеальный гипсокартон для ремонта
купить строительные материалы в москве [url=https://gipsokarton-moskva.ru/]гипсокартон заказать[/url] .
http://indianpharmgrx.com/# pharmacy website india
mexican online pharmacies prescription drugs [url=https://mexicanpharmgrx.com/#]mexican pharmacy[/url] pharmacies in mexico that ship to usa
FitSpresso is a natural weight loss supplement that will help you maintain healthy body weight without having to deprive your body of your favorite food or take up exhausting workout routines.
mexican pharmaceuticals online: Mexico drugstore – best online pharmacies in mexico
https://canadianpharmgrx.xyz/# canadianpharmacymeds com
canadianpharmacymeds com canadian pharmacy oxycodone or northern pharmacy canada
https://www.google.co.ck/url?q=https://canadianpharmgrx.com canadian pharmacy ratings
[url=https://cse.google.com.pr/url?q=https://canadianpharmgrx.com]legit canadian pharmacy online[/url] canadian pharmacy oxycodone and [url=https://lhgangguanwang.com/home.php?mod=space&uid=162857]best canadian pharmacy to buy from[/url] ed meds online canada
Touche. Outstanding arguments. Keep up the amazing spirit.
tamoxifen benefits: tamoxifen alternatives premenopausal – tamoxifen hormone therapy
https://zhknoviydom.ru/
buy misoprostol over the counter [url=http://misoprostol.top/#]cytotec pills buy online[/url] Abortion pills online
doxycycline hyclate: price of doxycycline – doxycycline mono
https://zhkkvartiradom.ru/
cheap diflucan online: where to get diflucan otc – diflucan 200 mg capsules
купить прогулочную коляску москва [url=https://detskie-koljaski-moskva.ru/]москва коляски[/url] .
[url=https://avtosalonbmwftnz.dp.ua]купити bmw[/url]
Приобрести ценогенетический БМВ 2024 года в течение Украине по лучшей стоимости у официознного дилера. Тест-драйв, страхование, авансирование, промоакции и еще спецпредложения.
http://avtosalonbmwftnz.dp.ua
buy cytotec online [url=http://misoprostol.top/#]order cytotec online[/url] cytotec online
Привет всем!
Было ли у вас опыт написания дипломной работы в крайне сжатые сроки? Это действительно требует огромной ответственности и трудоемкости, однако важно сохранять упорство и продолжать активно участвовать в учебном процессе, как я это делаю.
Для тех, кто умеет эффективно искать и анализировать информацию в интернете, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями по ссылке , это проверенный источник!
https://landik-diploms-srednee24.com/
купить диплом специалиста
купить диплом института
купить диплом о высшем образовании
купить диплом бакалавра
купить аттестат школы
Желаю всем отличных оценок!
прогулочные коляски москва [url=https://detskie-koljaski-moskva.ru/]купить коляску для[/url] .
doxycycline 100mg: doxycycline tetracycline – generic for doxycycline
cipro 500mg best prices: cipro ciprofloxacin – buy ciprofloxacin
can i buy diflucan over the counter uk [url=http://diflucan.icu/#]diflucan tablet india[/url] diflucan online buy
cytotec online: cytotec abortion pill – buy cytotec
https://zhknoviystroi.ru/
ciprofloxacin generic: ciprofloxacin generic price – buy cipro
https://nolvadex.icu/# tamoxifen moa
purchase cipro ciprofloxacin over the counter or cipro
https://www.google.com.co/url?sa=t&url=https://ciprofloxacin.guru ciprofloxacin order online
[url=https://www.google.si/url?q=https://ciprofloxacin.guru]purchase cipro[/url] antibiotics cipro and [url=http://ckxken.synology.me/discuz/home.php?mod=space&uid=19734]ciprofloxacin generic price[/url] cipro online no prescription in the usa
online doxycycline: buy doxycycline cheap – doxycycline 100 mg
liquid tamoxifen [url=https://nolvadex.icu/#]does tamoxifen cause bone loss[/url] tamoxifen dose
[url=http://prednisonexg.online/]prednisone 50 mg price in india[/url]
doxycycline 50 mg: generic for doxycycline – buy generic doxycycline
doxycycline pills: doxycycline 500mg – buy doxycycline monohydrate
https://noviydomstroika.ru/
Abortion pills online: purchase cytotec – buy cytotec over the counter
order cytotec online [url=https://misoprostol.top/#]buy cytotec in usa[/url] buy cytotec over the counter
https://diplomsdayu.ru/
Стоматологічний огляд
18. Як зберегти здоров’я зубів у період карантину
стоматологія клініка [url=https://stomatologiyatrn.ivano-frankivsk.ua/]https://stomatologiyatrn.ivano-frankivsk.ua/[/url] .
[url=https://synthroidam.online/]synthroid 175[/url]
Ефективні методи лікування
10. Як підготуватися до відвідування стоматолога
стоматологічна клініка сім [url=https://stomatologiyatrn.ivano-frankivsk.ua/]стоматологічна клініка сім[/url] .
1. 10 лучших идей для дизайна интерьера
2. Топ-20 трендов в дизайне на 2021 год
3. Цветовые решения
4. Дизайн-проект
5. Дизайн нового поколения
6. Шаг за шагом: создание уютного дизайна спальни
7. Дизайн для маленькой квартиры
8. Природный дизайн
9. Баланс цветов и форм: основы хорошего дизайна
10. Дизайн-студия: секреты успешного бизнеса в сфере дизайна
11. Интересные факты о развитии дизайна в XXI веке
12. Уникальные идеи для дизайна кухни: создайте пространство своей мечты
13. Тенденции в сфере дизайна мебели: вдохновляющие идеи
14. Дизайн гостиной
15. Минимализм
16. Дизайн сада: принципы оформления участка с учетом ландшафта
17. Декорирование с текстилем
18. Принципы цветового баланса в дизайне: как создать гармоничное пространство
19. Книги по дизайну
20. Дизайн подростковой комнаты
проекты квартир [url=https://studiya-dizajna-intererov.ru/]проекты квартир[/url] .
https://reshaitzadachi.ru/
I wanted to send a brief word to thank you for those fantastic items you are showing on this website. My time intensive internet investigation has now been rewarded with reasonable content to exchange with my pals. 강화군출장안마I ‘d assert that most of us website visitors are really endowed to be in a really good site with very many perfect professionals with beneficial things.
Cytotec 200mcg price buy cytotec pills or buy cytotec pills online cheap
https://maps.google.com.gh/url?q=https://misoprostol.top cytotec abortion pill
[url=https://cse.google.vg/url?q=https://misoprostol.top]Cytotec 200mcg price[/url] buy cytotec in usa and [url=http://yslit.com/home.php?mod=space&uid=650530]п»їcytotec pills online[/url] cytotec online
cytotec buy online usa [url=http://misoprostol.top/#]cytotec buy online usa[/url] buy cytotec pills online cheap
http://diflucan.icu/# diflucan generic cost
[url=http://motomagazinvfdvgd.vn.ua/uk/v-ekipirovka/]мотоекіпіровка[/url]
В ТЕЧЕНИЕ нашем мотомагазине вы выкроите запасные части чтобы байков, скутеров, снегоходов равно квадроциклов. ЯЗЫК нас ваша милость хронически выищете масла чтобы мотоциклов, фильтра, цепи.
https://motomagazinvfdvgd.vn.ua
vibramycin 100 mg: doxycycline pills – buy generic doxycycline
[url=http://azithromycinmds.com/]azithromycin for sale uk[/url]
nolvadex steroids: tamoxifen cyp2d6 – tamoxifen side effects forum
Amplificadores de senal gsm
Adios a las llamadas perdidas con un amplificador de senal movil
[url=https://my.archdaily.com/us/@neillopez23]https://my.archdaily.com/us/@neillopez23[/url]
1. 10 лучших идей для дизайна интерьера
2. Тренды в дизайне
3. Как выбрать идеальный цветовой акцент в дизайне
4. Секреты успешного дизайн-проекта
5. Инновационные подходы к дизайну: отражение современности
6. Дизайн спальни
7. Дизайнерские решения для увеличения пространства в маленькой квартире
8. Природный дизайн
9. Основы дизайна
10. Дизайнерский бизнес
11. Интересные факты о развитии дизайна в XXI веке
12. Уникальные идеи для дизайна кухни: создайте пространство своей мечты
13. Тенденции в сфере дизайна мебели: вдохновляющие идеи
14. Мастер-класс по созданию стильного дизайна гостиной
15. Искусство минимализма: создание современного дизайна в своем доме
16. Дизайн сада: принципы оформления участка с учетом ландшафта
17. Декорирование дома с использованием текстиля: советы и идеи
18. Принципы цветового баланса в дизайне: как создать гармоничное пространство
19. Книги по дизайну
20. Дизайн подростковой комнаты
студия дизайна интерьера [url=https://studiya-dizajna-intererov.ru/]https://studiya-dizajna-intererov.ru/[/url] .
sandyterrace.com
Fang Jifan은 앉아서 “허 환주를 마실까요? “라고 물었습니다.
buy doxycycline monohydrate buy doxycycline without prescription or doxycycline monohydrate
https://cse.google.com.cu/url?sa=t&url=https://doxycyclinest.pro doxycycline hyc
[url=https://www.google.az/url?sa=t&url=http://doxycyclinest.pro]doxy[/url] buy doxycycline online uk and [url=https://forex-bitcoin.com/members/341328-plorlujkhr]100mg doxycycline[/url] generic for doxycycline
buy cipro online canada [url=http://ciprofloxacin.guru/#]ciprofloxacin 500mg buy online[/url] buy generic ciprofloxacin
Отечественный производитель реализует тренировочные диски на ресурсе https://diski-dlya-shtang.ru/ для напряженной работы в коммерческих тренажерных центрах и в домашних условиях. Завод из России создает тренировочные блины разного посадочного диаметра и любого востребованного веса для сборных штанг и гантелей. Рекомендуем к покупке обрезиненные блины для силовых занятий. Они не скользят, не шумят и более безопасны. Выпускаемые изделия не нуждаются в постоянном обслуживании и рассчитаны на длительную работу в клубах. Рекомендуем обширный ассортимент любительских дисков с любым видом защитного покрытия. Закажите веса с необходимой массой и посадочным диаметром по доступным ценам напрямую у отечественного завода.
ciprofloxacin generic price: buy generic ciprofloxacin – buy cipro
tamoxifen and osteoporosis tamoxifen dose or tamoxifen adverse effects
http://www.christopheweber.de/homepage/gemeinsam/ext_link.php?url=http://nolvadex.icu tamoxifen and bone density
[url=https://bizmandu.com/redirect?url=http://nolvadex.icu]raloxifene vs tamoxifen[/url] how to prevent hair loss while on tamoxifen and [url=http://www.zhuangxiuz.com/home.php?mod=space&uid=814534]nolvadex half life[/url] nolvadex 10mg
toasterovensplus.com
素晴らしい洞察力と情報の提供、本当にありがとうございます。
liquid tamoxifen: tamoxifen pill – who should take tamoxifen
diflucan canadian pharmacy: buy diflucan generic – diflucan buy online usa
vibramycin 100 mg [url=http://doxycyclinest.pro/#]doxycycline 100mg price[/url] doxycycline vibramycin
[url=http://oprednisone.com/]prednisone 5 mg tablet rx[/url]
Вывоз мусора с грузчиками https://vivozmusora67.ru/
cipro 500mg best prices: buy cipro cheap – ciprofloxacin generic
doxycycline medication: buy doxycycline – doxylin
cipro ciprofloxacin mail online or buy cipro online canada
http://mx2.radiant.net/Redirect/ciprofloxacin.guru/wiki/GM_Vortec_engine buy ciprofloxacin
[url=https://cse.google.com.pk/url?q=http://ciprofloxacin.guru]buy cipro cheap[/url] buy cipro online canada and [url=http://bbs.cheaa.com/home.php?mod=space&uid=3105389]ciprofloxacin generic[/url] cipro pharmacy
diflucan 6 tabs [url=https://diflucan.icu/#]over the counter diflucan pill[/url] diflucan pill uk
ciprofloxacin generic: ciprofloxacin generic – buy generic ciprofloxacin
сплит кондиционер купить [url=https://split-sistema-kupit.ru/]https://split-sistema-kupit.ru/[/url] .
http://doxycyclinest.pro/# buy doxycycline for dogs
[url=http://valtrexid.com/]valtrex canada[/url]
вентиляция сплит система [url=https://split-sistema-kupit.ru/]https://split-sistema-kupit.ru/[/url] .
where to buy diflucan 1 [url=https://diflucan.icu/#]diflucan canada prescription[/url] diflucan 150 mg tabs
[url=http://drugstorepp.online/]canada drugstore pharmacy rx[/url]
[url=http://oprednisone.com/]where to buy prednisone online[/url]
[url=[Link deleted]zithromax z-pak[/url]
<a href=[Link deleted]
The meal went without incident although a couple of times she had to avert her gaze from Dan for fear of bursting out laughing. Dan went up to his room saying he wanted to listen to music, he laid on his bed playing with himself waiting for his father to leave. He thought about the events of the last two weeks it had been the craziest time of his life.
He put it all down to Mary Harris, she had been his girlfriend for two years, he liked her a lot, she was pretty and intelligent two things that rarely combined in his experience, the problem was she steadfastly refused to let him put his cock inside her, he had thought he was getting somewhere when he took his cock out that evening in the cinema when she had finally allowed him to get his hand inside her panties, it was the first time she had allowed him to do any more than play with her tits. He had taken her hand and placed it on his erection, initially he had been pleased to hear her sharp intake of breath when she felt the size of him and he was encouraged when she began stroking him.
It was later that the problem started, he had her in the car park, they were kissing, her sweater was pushed up together with her bra and he was sucking on her nipples. He managed to get her laid across the front of one of the cars, his hand up her skirt, trying to pull down her panties. That was when she had stopped him.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Flirt.com is a scam
Hi all, got scammed by this website. Saw that there were a couple of post informing about this but just wanted to give more details
Paid for the three day offer and with the confirmation of the subscription, got two mails from hornycontacts.com and loveaholics.com asking me to confirm my email. Didn’t pay attention and deleted them.
I immediately canceled the subscription in flirt.com without any issue and on the last day it changed to a standard membership so since it was bs site, cancelled the account as well.
So I was happy and watching a movie when I got an sms from my card provider telling me that I got a 71.78 euros charge from fry frtlsp.com. Never heard of them, so I called my card provider and cancelled my card and will request the return of the money as well.
Then I realized that maybe these two websites also by some miracle signed me up to a paid subscription… so I logged in… had to recover the passwords because they were not the one I used in flirt.com… and surprise, loveaholics.com did signed me up for a paid subscription without me being aware (pretty sure that somewhere during the signing process in flirt there was something checked and didn’t pay attention.). So I had to cancel subscription and account in these two other sites.
So, sorry for the long post but in summary…. do not use flirt.com at all!!!
Yes, FLIRT.COM it is a scamming website. It sign you on multiple websites like askme4date.com . It bombard you with emails that you receive messages, and you need to pay to see them. After you pay you see the messages. All messages are from BOTS. No real person.
It’s subscribing to automatic renewal and it’s hard to cancel renewal. They push you to a complicated scheme. I’m not even sure the renewal canceling works. After
[url=[Link deleted]metformin from canada[/url]
[url=[Link deleted]250[/url]
Amplificadores de senal gsm
Haz que tu movil funcione como nunca con un amplificador de senal de calidad
[url=[Link deleted]
[url=[Link deleted]prescription online[/url]
[url=[Link deleted]pharmacy dubai[/url]
[url=[Link deleted]pharmacy no prescription[/url]
[url=[Link deleted]20 mg purchase[/url]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Flirt.com is a scam
Hi all, got scammed by this website. Saw that there were a couple of post informing about this but just wanted to give more details
Paid for the three day offer and with the confirmation of the subscription, got two mails from hornycontacts.com and loveaholics.com asking me to confirm my email. Didn’t pay attention and deleted them.
I immediately canceled the subscription in flirt.com without any issue and on the last day it changed to a standard membership so since it was bs site, cancelled the account as well.
So I was happy and watching a movie when I got an sms from my card provider telling me that I got a 71.78 euros charge from fry frtlsp.com. Never heard of them, so I called my card provider and cancelled my card and will request the return of the money as well.
Then I realized that maybe these two websites also by some miracle signed me up to a paid subscription… so I logged in… had to recover the passwords because they were not the one I used in flirt.com… and surprise, loveaholics.com did signed me up for a paid subscription without me being aware (pretty sure that somewhere during the signing process in flirt there was something checked and didn’t pay attention.). So I had to cancel subscription and account in these two other sites.
So, sorry for the long post but in summary…. do not use flirt.com at all!!!
Yes, FLIRT.COM it is a scamming website. It sign you on multiple websites like askme4date.com . It bombard you with emails that you receive messages, and you need to pay to see them. After you pay you see the messages. All messages are from BOTS. No real person.
It’s subscribing to automatic renewal and it’s hard to cancel renewal. They push you to a complicated scheme. I’m not even sure the renewal canceling works. After
[url=[Link deleted]10 mg tablet cost[/url]
[url=[Link deleted]12.5 mg[/url]
[url=[Link deleted]250 mg[/url]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Flirt.com is a scam
Hi all, got scammed by this website. Saw that there were a couple of post informing about this but just wanted to give more details
Paid for the three day offer and with the confirmation of the subscription, got two mails from hornycontacts.com and loveaholics.com asking me to confirm my email. Didn’t pay attention and deleted them.
I immediately canceled the subscription in flirt.com without any issue and on the last day it changed to a standard membership so since it was bs site, cancelled the account as well.
So I was happy and watching a movie when I got an sms from my card provider telling me that I got a 71.78 euros charge from fry frtlsp.com. Never heard of them, so I called my card provider and cancelled my card and will request the return of the money as well.
Then I realized that maybe these two websites also by some miracle signed me up to a paid subscription… so I logged in… had to recover the passwords because they were not the one I used in flirt.com… and surprise, loveaholics.com did signed me up for a paid subscription without me being aware (pretty sure that somewhere during the signing process in flirt there was something checked and didn’t pay attention.). So I had to cancel subscription and account in these two other sites.
So, sorry for the long post but in summary…. do not use flirt.com at all!!!
Yes, FLIRT.COM it is a scamming website. It sign you on multiple websites like askme4date.com . It bombard you with emails that you receive messages, and you need to pay to see them. After you pay you see the messages. All messages are from BOTS. No real person.
It’s subscribing to automatic renewal and it’s hard to cancel renewal. They push you to a complicated scheme. I’m not even sure the renewal canceling works. After
[url=[Link deleted]tablet[/url]
[url=[Link deleted]rated canadian pharmacy[/url]
[url=[Link deleted]india[/url]
[url=[Link deleted]225 mcg[/url]
[url=[Link deleted]pharmacy online[/url]
<a href="[Link deleted]
Fang Jifan은 계속해서 펜을 들고 펜 끝을 깨물고 원고에 대해 깊은 생각에 빠졌습니다.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Flirt.com is a scam
Hi all, got scammed by this website. Saw that there were a couple of post informing about this but just wanted to give more details
Paid for the three day offer and with the confirmation of the subscription, got two mails from hornycontacts.com and loveaholics.com asking me to confirm my email. Didn’t pay attention and deleted them.
I immediately canceled the subscription in flirt.com without any issue and on the last day it changed to a standard membership so since it was bs site, cancelled the account as well.
So I was happy and watching a movie when I got an sms from my card provider telling me that I got a 71.78 euros charge from fry frtlsp.com. Never heard of them, so I called my card provider and cancelled my card and will request the return of the money as well.
Then I realized that maybe these two websites also by some miracle signed me up to a paid subscription… so I logged in… had to recover the passwords because they were not the one I used in flirt.com… and surprise, loveaholics.com did signed me up for a paid subscription without me being aware (pretty sure that somewhere during the signing process in flirt there was something checked and didn’t pay attention.). So I had to cancel subscription and account in these two other sites.
So, sorry for the long post but in summary…. do not use flirt.com at all!!!
Yes, FLIRT.COM it is a scamming website. It sign you on multiple websites like askme4date.com . It bombard you with emails that you receive messages, and you need to pay to see them. After you pay you see the messages. All messages are from BOTS. No real person.
It’s subscribing to automatic renewal and it’s hard to cancel renewal. They push you to a complicated scheme. I’m not even sure the renewal canceling works. After
Why users still make use of to read news papers when in this technological globe everything is accessible on net?
#be#jk3#jk#jk#JK##
<a href=[Link deleted]номер телефона США
В современном мире, где диплом является началом удачной карьеры в любой области, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед каждым человеком, который стремится начать трудовую деятельность или учиться в университете.
В данном контексте мы предлагаем максимально быстро получить этот важный документ. Вы сможете заказать диплом нового или старого образца, что является отличным решением для всех, кто не смог закончить обучение, потерял документ или желает исправить свои оценки. диплом изготавливается с особой аккуратностью, вниманием ко всем элементам. На выходе вы сможете получить продукт, максимально соответствующий оригиналу.
Преимущество такого подхода заключается не только в том, что можно быстро получить свой диплом. Весь процесс организовывается удобно, с нашей поддержкой. Начав от выбора подходящего образца до консультаций по заполнению личных данных и доставки по России — все под абсолютным контролем квалифицированных специалистов.
Для тех, кто ищет оперативный способ получить требуемый документ, наша компания предлагает отличное решение. Заказать диплом – это значит избежать долгого процесса обучения и сразу перейти к достижению личных целей, будь то поступление в ВУЗ или начало карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем обществе, где диплом становится началом удачной карьеры в любой отрасли, многие ищут максимально простой путь получения качественного образования. Факт наличия официального документа переоценить попросту невозможно. Ведь диплом открывает дверь перед любым человеком, желающим начать профессиональную деятельность или продолжить обучение в университете.
Предлагаем очень быстро получить этот необходимый документ. Вы можете заказать диплом, и это становится выгодным решением для человека, который не смог завершить образование или потерял документ. Любой диплом изготавливается аккуратно, с особым вниманием к мельчайшим деталям. В результате вы получите 100% оригинальный документ.
Преимущества данного подхода заключаются не только в том, что вы оперативно получите диплом. Процесс организовывается удобно, с профессиональной поддержкой. От выбора нужного образца до консультаций по заполнению персональных данных и доставки по стране — все будет находиться под абсолютным контролем наших специалистов.
В итоге, для всех, кто ищет максимально быстрый способ получить необходимый документ, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать долгого процесса обучения и сразу переходить к важным целям, будь то поступление в ВУЗ или начало карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
<a href=[Link deleted]
В современном мире, где диплом становится началом удачной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь диплом открывает двери перед всеми, кто желает вступить в профессиональное сообщество или учиться в высшем учебном заведении.
Мы предлагаем оперативно получить любой необходимый документ. Вы имеете возможность приобрести диплом, что будет отличным решением для человека, который не смог закончить обучение, утратил документ или желает исправить плохие оценки. дипломы изготавливаются с особой тщательностью, вниманием к мельчайшим элементам. На выходе вы сможете получить продукт, 100% соответствующий оригиналу.
Плюсы данного подхода состоят не только в том, что вы сможете максимально быстро получить свой диплом. Весь процесс организовывается комфортно, с профессиональной поддержкой. От выбора требуемого образца диплома до консультации по заполнению личной информации и доставки в любое место страны — все находится под абсолютным контролем опытных специалистов.
Всем, кто ищет быстрый и простой способ получить требуемый документ, наша компания может предложить выгодное решение. Заказать диплом – это значит избежать длительного процесса обучения и сразу переходить к достижению личных целей: к поступлению в университет или к началу успешной карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем обществе, где диплом – это начало успешной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения образования. Необходимость наличия документа об образовании переоценить просто невозможно. Ведь именно он открывает дверь перед любым человеком, желающим начать трудовую деятельность или учиться в высшем учебном заведении.
Мы предлагаем оперативно получить этот необходимый документ. Вы можете приобрести диплом старого или нового образца, что будет удачным решением для человека, который не смог завершить обучение, утратил документ или хочет исправить плохие оценки. Все дипломы выпускаются аккуратно, с особым вниманием ко всем нюансам. В итоге вы сможете получить полностью оригинальный документ.
Преимущество такого решения заключается не только в том, что вы быстро получите диплом. Весь процесс организован комфортно, с нашей поддержкой. От выбора требуемого образца до правильного заполнения персональных данных и доставки по стране — все находится под абсолютным контролем качественных мастеров.
Для всех, кто пытается найти быстрый и простой способ получения требуемого документа, наша компания предлагает отличное решение. Приобрести диплом – значит избежать длительного обучения и сразу переходить к личным целям, будь то поступление в университет или начало удачной карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем мире, где диплом является началом удачной карьеры в любой области, многие стараются найти максимально простой путь получения качественного образования. Необходимость наличия официального документа об образовании трудно переоценить. Ведь именно диплом открывает дверь перед любым человеком, желающим начать профессиональную деятельность или продолжить обучение в каком-либо ВУЗе.
В данном контексте наша компания предлагает очень быстро получить этот важный документ. Вы сможете заказать диплом нового или старого образца, и это становится выгодным решением для всех, кто не смог закончить обучение, утратил документ или хочет исправить плохие оценки. Все дипломы выпускаются с особой аккуратностью, вниманием ко всем деталям. На выходе вы получите 100% оригинальный документ.
Плюсы данного решения заключаются не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организован комфортно, с нашей поддержкой. Начав от выбора нужного образца диплома до правильного заполнения личных данных и доставки в любое место страны — все находится под абсолютным контролем опытных специалистов.
В результате, для тех, кто ищет быстрый способ получить требуемый документ, наша компания готова предложить выгодное решение. Заказать диплом – это значит избежать длительного обучения и не теряя времени переходить к своим целям, будь то поступление в университет или старт карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Understanding COSC Validation and Its Importance in Watchmaking
COSC Accreditation and its Strict Criteria
COSC, or the Official Swiss Chronometer Testing Agency, is the authorized Switzerland testing agency that certifies the accuracy and precision of wristwatches. COSC certification is a mark of quality craftsmanship and dependability in timekeeping. Not all watch brands seek COSC accreditation, such as Hublot, which instead follows to its proprietary strict standards with mechanisms like the UNICO, attaining comparable precision.
The Art of Exact Chronometry
The core system of a mechanical watch involves the spring, which provides energy as it loosens. This system, however, can be susceptible to external elements that may influence its precision. COSC-accredited movements undergo demanding testing—over 15 days in various circumstances (five positions, 3 temperatures)—to ensure their durability and reliability. The tests evaluate:
Mean daily rate precision between -4 and +6 secs.
Mean variation, maximum variation levels, and effects of temperature changes.
Why COSC Certification Is Important
For watch enthusiasts and collectors, a COSC-certified watch isn’t just a item of technology but a proof to lasting excellence and precision. It signifies a timepiece that:
Presents outstanding dependability and accuracy.
Offers assurance of quality across the whole construction of the watch.
Is likely to retain its worth more efficiently, making it a smart choice.
Popular Timepiece Brands
Several renowned manufacturers prioritize COSC certification for their watches, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, presents collections like the Record and Soul, which highlight COSC-certified movements equipped with advanced materials like silicone balance springs to improve durability and performance.
Historic Context and the Evolution of Timepieces
The concept of the chronometer dates back to the requirement for precise chronometry for navigation at sea, highlighted by John Harrison’s work in the 18th century. Since the official establishment of Controle Officiel Suisse des Chronometres in 1973, the accreditation has become a standard for assessing the accuracy of high-end watches, sustaining a legacy of superiority in watchmaking.
Conclusion
Owning a COSC-certified timepiece is more than an aesthetic selection; it’s a commitment to quality and precision. For those valuing accuracy above all, the COSC certification provides peacefulness of mind, guaranteeing that each certified watch will perform reliably under various circumstances. Whether for individual satisfaction or as an investment, COSC-validated timepieces distinguish themselves in the world of horology, bearing on a legacy of careful timekeeping.
<a href=[Link deleted]
Son Dönemin En Fazla Gözde Bahis Sitesi: Casibom
Casino oyunlarını sevenlerin artık duymuş olduğu Casibom, nihai dönemde adından sıkça söz ettiren bir bahis ve kumarhane platformu haline geldi. Ülkemizin en başarılı bahis web sitelerinden biri olarak tanınan Casibom'un haftalık olarak değişen açılış adresi, alanında oldukça yenilikçi olmasına rağmen emin ve kazandıran bir platform olarak ön plana çıkıyor.
Casibom, muadillerini geride bırakıp eski kumarhane web sitelerinin önüne geçmeyi başarmayı sürdürüyor. Bu sektörde uzun soluklu olmak önemlidir olsa da, katılımcılarla etkileşimde olmak ve onlara erişmek da benzer miktar değerli. Bu noktada, Casibom'un gece gündüz servis veren canlı destek ekibi ile rahatlıkla iletişime geçilebilir olması önemli bir artı sağlıyor.
Hızlıca genişleyen oyuncu kitlesi ile dikkat çekici olan Casibom'un gerisindeki başarı faktörleri arasında, sadece ve yalnızca kumarhane ve gerçek zamanlı casino oyunları ile sınırlı olmayan geniş bir hizmetler yelpazesi bulunuyor. Sporcular bahislerinde sunduğu kapsamlı alternatifler ve yüksek oranlar, katılımcıları çekmeyi başarıyor.
Ayrıca, hem atletizm bahisleri hem de casino oyunlar katılımcılara yönlendirilen sunulan yüksek yüzdeli avantajlı bonuslar da dikkat çekiyor. Bu nedenle, Casibom hızla alanında iyi bir pazarlama başarısı elde ediyor ve büyük bir katılımcı kitlesi kazanıyor.
Casibom'un kar getiren promosyonları ve ünlülüğü ile birlikte, siteye üyelik hangi yollarla sağlanır sorusuna da bahsetmek gereklidir. Casibom'a mobil cihazlarınızdan, PC'lerinizden veya tabletlerinizden internet tarayıcı üzerinden kolaylıkla erişilebilir. Ayrıca, sitenin mobil uyumlu olması da büyük önem taşıyan bir avantaj sağlıyor, çünkü artık hemen hemen herkesin bir akıllı telefonu var ve bu akıllı telefonlar üzerinden hızlıca ulaşım sağlanabiliyor.
Hareketli cihazlarınızla bile yolda gerçek zamanlı iddialar alabilir ve maçları canlı olarak izleyebilirsiniz. Ayrıca, Casibom'un mobil uyumlu olması, ülkemizde kumarhane ve kumarhane gibi yerlerin kanuni olarak kapatılmasıyla birlikte bu tür platformlara erişimin büyük bir yolunu oluşturuyor.
Casibom'un emin bir kumarhane platformu olması da önemli bir avantaj getiriyor. Lisanslı bir platform olan Casibom, sürekli bir şekilde keyif ve kazanç sağlama imkanı sağlar.
Casibom'a abone olmak da son derece basittir. Herhangi bir belge koşulu olmadan ve ücret ödemeden web sitesine kolayca abone olabilirsiniz. Ayrıca, platform üzerinde para yatırma ve çekme işlemleri için de birçok farklı yöntem mevcuttur ve herhangi bir kesim ücreti alınmamaktadır.
Ancak, Casibom'un güncel giriş adresini takip etmek de gereklidir. Çünkü canlı bahis ve casino platformlar moda olduğu için sahte siteler ve dolandırıcılar da görünmektedir. Bu nedenle, Casibom'un sosyal medya hesaplarını ve güncel giriş adresini periyodik olarak kontrol etmek elzemdir.
Sonuç, Casibom hem emin hem de kar getiren bir casino sitesi olarak dikkat çekiyor. yüksek promosyonları, geniş oyun seçenekleri ve kullanıcı dostu mobil uygulaması ile Casibom, kumarhane sevenler için ideal bir platform getiriyor.
LhaneGax
Приветики, дорогие мои!!
Использование онлайн-материалов сделало диплом более доступным для выполнения.
На нашем сайте можно заказать и купить диплом с гарантией и доставкой в любой регион РФ.
Желаю всем отличных отметок!
купить сертификат специалиста
купить диплом с занесением в реестр
купить диплом в чайковском
купить диплом в новоалтайске
купить диплом в артеме
<a href=[Link deleted]диплом в мурманске
<a href=[Link deleted]диплом образцы
<a href=[Link deleted]диплом в нефтекамске
<a href=[Link deleted]диплом о среднем
<a href=[Link deleted]диплом в евпатории
<a href="[Link deleted]
この記事は非常に有益でした。感謝します!
[url=[Link deleted]canadian pharmacy[/url]
[url=[Link deleted]canadian pharmacy rx[/url]
[url=[Link deleted]0.5 mg[/url]
[url=[Link deleted]pharmacy delivery delhi[/url]
<a href=[Link deleted]watches
Understanding COSC Validation and Its Importance in Watchmaking
COSC Validation and its Stringent Standards
Controle Officiel Suisse des Chronometres, or the Official Swiss Chronometer Testing Agency, is the official Swiss testing agency that verifies the accuracy and accuracy of wristwatches. COSC accreditation is a mark of quality craftsmanship and trustworthiness in chronometry. Not all watch brands seek COSC validation, such as Hublot, which instead follows to its own stringent criteria with movements like the UNICO, attaining similar accuracy.
The Art of Exact Chronometry
The central mechanism of a mechanical watch involves the mainspring, which supplies energy as it unwinds. This system, however, can be vulnerable to external elements that may affect its precision. COSC-certified mechanisms undergo strict testing—over fifteen days in various conditions (5 positions, 3 temperatures)—to ensure their resilience and reliability. The tests evaluate:
Mean daily rate accuracy between -4 and +6 secs.
Mean variation, highest variation levels, and effects of temperature changes.
Why COSC Validation Is Important
For watch aficionados and connoisseurs, a COSC-accredited timepiece isn’t just a item of technology but a demonstration to enduring quality and precision. It signifies a watch that:
Offers exceptional dependability and precision.
Provides guarantee of superiority across the entire construction of the timepiece.
Is probable to maintain its worth more efficiently, making it a sound choice.
Popular Timepiece Brands
Several famous brands prioritize COSC certification for their watches, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, offers collections like the Archive and Spirit, which showcase COSC-certified mechanisms equipped with innovative substances like silicone equilibrium springs to boost durability and performance.
Historic Background and the Development of Timepieces
The concept of the timepiece originates back to the requirement for exact chronometry for navigational at sea, highlighted by John Harrison’s work in the eighteenth century. Since the official establishment of COSC in 1973, the certification has become a benchmark for assessing the precision of high-end timepieces, sustaining a legacy of superiority in horology.
Conclusion
Owning a COSC-accredited watch is more than an visual selection; it’s a commitment to excellence and precision. For those appreciating precision above all, the COSC accreditation provides peace of mind, guaranteeing that each validated timepiece will perform dependably under various conditions. Whether for personal satisfaction or as an investment decision, COSC-accredited timepieces distinguish themselves in the world of watchmaking, maintaining on a tradition of meticulous timekeeping.
[url=[Link deleted]to buy synthroid 1mg in canada[/url]
Today, I went to the beachfront with my children. I found a sea shell and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She placed the shell to her ear and screamed. There was a hermit crab inside and it pinched her ear. She never wants to go back! LoL I know this is totally off topic but I had to tell someone!
<a href=[Link deleted]реалистик из китая цены
Earnestjab
Всем хорошего дня!
Диплом заставил меня перейти на ночной режим работы, что пагубно сказалось на здоровье.
Приобретите диплом университета с гарантированной доставкой в любой город России с оплатой после получения.
Желаю каждому положительных оценок!
купить диплом в тольятти
купить диплом инженера механика
купить диплом в иркутске
купить диплом гознак
купить свидетельство о разводе
<a href=[Link deleted]диплом в новочеркасске
<a href=[Link deleted]диплом фитнес инструктора
купить диплом в донском
<a href=[Link deleted]диплом в вологде
<a href=[Link deleted]диплом в глазове
Hi! Do you use Twitter? I’d like to follow you if that would be okay. I’m absolutely enjoying your blog and look forward to new posts.
<a href=[Link deleted]сайт вован казино
Spin to Win Cash Prizes in Kenya
best online casino games kenya [url=[Link deleted]that pay real money in kenya[/url] .
Сегодня, когда диплом является началом отличной карьеры в любом направлении, многие ищут максимально быстрый путь получения образования. Важность наличия документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед каждым человеком, желающим начать трудовую деятельность или продолжить обучение в ВУЗе.
В данном контексте мы предлагаем быстро получить этот важный документ. Вы можете купить диплом, и это является удачным решением для человека, который не смог закончить обучение, потерял документ или хочет исправить свои оценки. Любой диплом изготавливается аккуратно, с максимальным вниманием ко всем деталям, чтобы в результате получился 100% оригинальный документ.
Превосходство данного решения заключается не только в том, что можно быстро получить свой диплом. Процесс организовывается удобно и легко, с профессиональной поддержкой. От выбора нужного образца документа до точного заполнения персональной информации и доставки в любое место России — все под полным контролем опытных мастеров.
Всем, кто ищет максимально быстрый способ получения необходимого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать длительного обучения и сразу переходить к достижению своих целей: к поступлению в ВУЗ или к началу удачной карьеры.
[Link deleted]
Обучение игре в казино
[url=[Link deleted]олимп[/url]
로드스탁과의 레버리지 방식의 스탁: 투자 전략의 참신한 분야
로드스탁을 통해 공급하는 레버리지 방식의 스탁은 주식 시장의 투자의 한 방식으로, 상당한 이익율을 목적으로 하는 투자자들을 위해 매혹적인 선택입니다. 레버리지를 이용하는 이 방법은 투자자가 자신의 투자금을 넘어서는 자금을 투자할 수 있도록 하여, 증권 시장에서 훨씬 큰 작용을 행사할 수 있는 기회를 제공합니다.
레버리지 스탁의 원리
레버리지 스탁은 원칙적으로 투자금을 대여하여 사용하는 방식입니다. 예시를 들어, 100만 원의 자본으로 1,000만 원 상당의 증권을 구매할 수 있는데, 이는 투자자가 일반적인 투자 금액보다 훨씬 훨씬 더 많은 주식을 사들여, 주식 가격이 상승할 경우 해당하는 훨씬 더 큰 수익을 얻을 수 있게 합니다. 하지만, 주식 값이 내려갈 경우에는 그 손실 또한 커질 수 있으므로, 레버리지를 사용할 때는 신중해야 합니다.
투자 전략과 레버리지 사용
레버리지는 특히 성장 잠재력이 상당한 회사에 투자할 때 효과적입니다. 이러한 기업에 상당한 비중으로 적용하면, 성공적일 경우 막대한 수입을 가져올 수 있지만, 반대 경우의 경우 상당한 위험도 짊어져야 합니다. 따라서, 투자자는 자신의 위험성 관리 능력을 가진 장터 분석을 통해, 어떤 회사에 얼마만큼의 자금을 투자할지 결정하게 됩니다 합니다.
레버리지의 이점과 위험 요소
레버리지 방식의 스탁은 상당한 이익을 제공하지만, 그만큼 큰 위험성 수반합니다. 주식 장의 변화는 예측이 어렵기 때문에, 레버리지 사용을 이용할 때는 늘 장터 경향을 면밀히 살펴보고, 피해를 최소로 줄일 수 있는 전략을 마련해야 합니다.
맺음말: 세심한 선택이 필요
로드스탁에서 공급하는 레버리지 스탁은 강력한 투자 수단이며, 적절히 활용하면 큰 이익을 가져다줄 수 있습니다. 하지만 상당한 위험성도 고려해야 하며, 투자 결정은 필요한 정보와 세심한 생각 후에 이루어져야 합니다. 투자자 본인의 재정적 상태, 리스크 감수 능력, 그리고 시장 상황을 고려한 안정된 투자 전략이 중요합니다.
<a href="[Link deleted]
그 소식이 너무 갑작스러워서 많은 사람들이 패닉에 빠졌습니다.
[url=[Link deleted]to buy prednisone online without a script[/url]
<a href=[Link deleted]güncel
Nihai Dönemsel En Fazla Gözde Kumarhane Platformu: Casibom
Kumarhane oyunlarını sevenlerin artık duymuş olduğu Casibom, son dönemde adından çoğunlukla söz ettiren bir şans ve oyun platformu haline geldi. Ülkemizdeki en başarılı casino platformlardan biri olarak tanınan Casibom’un haftalık göre değişen giriş adresi, sektörde oldukça yeni olmasına rağmen emin ve kazanç sağlayan bir platform olarak ön plana çıkıyor.
Casibom, muadillerini geride bırakarak eski casino platformların üstünlük sağlamayı başarmayı sürdürüyor. Bu sektörde uzun soluklu olmak önemli olsa da, oyuncularla iletişimde bulunmak ve onlara erişmek da benzer kadar değerli. Bu durumda, Casibom’un 7/24 hizmet veren canlı destek ekibi ile rahatlıkla iletişime ulaşılabilir olması büyük bir artı sağlıyor.
Hızlıca artan oyuncuların kitlesi ile ilgi çeken Casibom’un arkasındaki başarılı faktörleri arasında, yalnızca casino ve canlı olarak casino oyunlarıyla sınırlı olmayan geniş bir servis yelpazesi bulunuyor. Sporcular bahislerinde sunduğu kapsamlı alternatifler ve yüksek oranlar, katılımcıları ilgisini çekmeyi başarmayı sürdürüyor.
Ayrıca, hem spor bahisleri hem de kumarhane oyunlar katılımcılara yönlendirilen sunulan yüksek yüzdeli avantajlı bonuslar da dikkat çekiyor. Bu nedenle, Casibom hızla alanında iyi bir reklam başarısı elde ediyor ve büyük bir oyuncuların kitlesi kazanıyor.
Casibom’un kazandıran ödülleri ve tanınırlığı ile birlikte, web sitesine abonelik ne şekilde sağlanır sorusuna da değinmek gereklidir. Casibom’a taşınabilir cihazlarınızdan, PC’lerinizden veya tabletlerinizden web tarayıcı üzerinden kolayca erişilebilir. Ayrıca, sitenin mobil uyumlu olması da büyük önem taşıyan bir artı sunuyor, çünkü artık hemen hemen herkesin bir akıllı telefonu var ve bu telefonlar üzerinden hızlıca erişim sağlanabiliyor.
Taşınabilir cep telefonlarınızla bile yolda canlı tahminler alabilir ve yarışmaları canlı olarak izleyebilirsiniz. Ayrıca, Casibom’un mobil uyumlu olması, ülkemizde casino ve casino gibi yerlerin yasal olarak kapatılmasıyla birlikte bu tür platformlara girişin büyük bir yolunu oluşturuyor.
Casibom’un emin bir bahis platformu olması da önemli bir artı sunuyor. Lisanslı bir platform olan Casibom, kesintisiz bir şekilde eğlence ve kar elde etme imkanı sağlar.
Casibom’a abone olmak da oldukça basittir. Herhangi bir belge koşulu olmadan ve ücret ödemeden siteye kolayca kullanıcı olabilirsiniz. Ayrıca, site üzerinde para yatırma ve çekme işlemleri için de birçok farklı yöntem mevcuttur ve herhangi bir kesim ücreti talep edilmemektedir.
Ancak, Casibom’un güncel giriş adresini izlemek de önemlidir. Çünkü canlı şans ve kumarhane web siteleri popüler olduğu için hileli siteler ve dolandırıcılar da ortaya çıkmaktadır. Bu nedenle, Casibom’un sosyal medya hesaplarını ve güncel giriş adresini periyodik olarak kontrol etmek elzemdir.
Sonuç olarak, Casibom hem güvenilir hem de kazandıran bir kumarhane sitesi olarak ilgi çekiyor. yüksek bonusları, geniş oyun seçenekleri ve kullanıcı dostu mobil uygulaması ile Casibom, oyun hayranları için mükemmel bir platform sunuyor.
Как стать профессиональным игроком в казино
[url=[Link deleted]казино[/url]
<a href="[Link deleted]
누군가가 갑자기 말했다. "절름발이야, 절름발이야."
[url=[Link deleted]prednisone without prescription[/url]
로드스탁과의 레버리지 방식의 스탁: 투자법의 신규 분야
로드스탁을 통해 제공되는 레버리지 방식의 스탁은 주식 시장의 투자법의 한 방식으로, 상당한 이익율을 목적으로 하는 투자자들을 위해 유혹적인 선택입니다. 레버리지를 사용하는 이 방법은 투자하는 사람들이 자신의 투자금을 초과하는 투자금을 투자할 수 있도록 하여, 주식 시장에서 더 큰 힘을 가질 수 있는 방법을 줍니다.
레버리지 방식의 스탁의 원리
레버리지 스탁은 기본적으로 자금을 빌려 투자하는 방법입니다. 사례를 들어, 100만 원의 자금으로 1,000만 원 상당의 증권을 취득할 수 있는데, 이는 투자자가 일반적인 자본보다 훨씬 더 많은 증권을 사들여, 증권 가격이 상승할 경우 관련된 더 큰 이익을 얻을 수 있게 해줍니다. 하지만, 증권 값이 떨어질 경우에는 그 손실 또한 크게 될 수 있으므로, 레버리지 사용을 사용할 때는 신중하게 생각해야 합니다.
투자 계획과 레버리지
레버리지는 특히 성장 가능성이 큰 사업체에 투자할 때 도움이 됩니다. 이러한 사업체에 상당한 비율로 투자하면, 잘 될 경우 큰 이익을 가져올 수 있지만, 그 반대의 경우 많은 리스크도 감수하게 됩니다. 그렇기 때문에, 투자자는 자신의 위험 관리 능력과 시장 분석을 통해, 어느 사업체에 얼마만큼의 자금을 투입할지 선택해야 합니다.
레버리지 사용의 장점과 위험 요소
레버리지 방식의 스탁은 큰 이익을 제공하지만, 그만큼 상당한 위험도 따릅니다. 증권 거래의 변화는 예측이 곤란하기 때문에, 레버리지를 이용할 때는 언제나 상장 동향을 정밀하게 살펴보고, 손해를 최소화할 수 있는 전략을 마련해야 합니다.
결론: 세심한 선택이 필요
로드스탁을 통해 제공하는 레버리지 스탁은 막강한 투자 도구이며, 잘 사용하면 상당한 수입을 가져다줄 수 있습니다. 그렇지만 큰 위험성도 고려해야 하며, 투자 결정이 충분히 많은 데이터와 조심스러운 생각 후에 이루어져야 합니다. 투자자 본인의 재정적 상태, 리스크 감수 능력, 그리고 시장의 상황을 반영한 안정된 투자 방법이 핵심입니다.
В современном мире, где диплом является началом отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения образования. Наличие официального документа переоценить невозможно. Ведь именно диплом открывает дверь перед всеми, кто стремится начать профессиональную деятельность или продолжить обучение в каком-либо институте.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы можете заказать диплом старого или нового образца, и это является удачным решением для всех, кто не смог закончить обучение или утратил документ. Все дипломы производятся с особой тщательностью, вниманием ко всем деталям. В результате вы получите 100% оригинальный документ.
Преимущества данного подхода заключаются не только в том, что можно максимально быстро получить свой диплом. Весь процесс организовывается комфортно и легко, с нашей поддержкой. От выбора необходимого образца до консультаций по заполнению персональных данных и доставки в любое место России — все находится под абсолютным контролем опытных мастеров.
Всем, кто ищет максимально быстрый способ получить требуемый документ, наша компания предлагает отличное решение. Купить диплом – значит избежать продолжительного процесса обучения и сразу переходить к достижению собственных целей, будь то поступление в университет или старт профессиональной карьеры.
[Link deleted]
[url=[Link deleted]canadian pharmacy[/url]
[url=[Link deleted]to order valtrex online[/url]
В современном мире, где диплом – это начало успешной карьеры в любой сфере, многие ищут максимально простой путь получения образования. Важность наличия официального документа об образовании сложно переоценить. Ведь именно он открывает дверь перед каждым человеком, желающим начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
Наша компания предлагает быстро получить этот важный документ. Вы сможете заказать диплом, что будет выгодным решением для человека, который не смог закончить обучение или потерял документ. Все дипломы изготавливаются с особой тщательностью, вниманием к мельчайшим элементам. В результате вы сможете получить 100% оригинальный документ.
Плюсы этого решения заключаются не только в том, что вы максимально быстро получите свой диплом. Процесс организован комфортно, с нашей поддержкой. Начиная от выбора подходящего образца диплома до точного заполнения личной информации и доставки в любое место России — все будет находиться под абсолютным контролем наших мастеров.
Всем, кто пытается найти быстрый и простой способ получить необходимый документ, наша компания может предложить отличное решение. Заказать диплом – значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению своих целей: к поступлению в ВУЗ или к началу удачной карьеры.
[Link deleted]
[url=[Link deleted]synthroid[/url]
Сегодня, когда диплом – это начало удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Важность наличия документа об образовании сложно переоценить. Ведь именно диплом открывает дверь перед людьми, желающими начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
Предлагаем быстро получить этот важный документ. Вы имеете возможность купить диплом, что становится удачным решением для всех, кто не смог завершить образование или утратил документ. Любой диплом изготавливается с особой аккуратностью, вниманием к мельчайшим деталям, чтобы на выходе получился полностью оригинальный документ.
Преимущество подобного решения состоит не только в том, что можно быстро получить свой диплом. Весь процесс организован комфортно и легко, с профессиональной поддержкой. От выбора нужного образца до консультаций по заполнению персональных данных и доставки в любое место России — все будет находиться под полным контролем качественных специалистов.
Для тех, кто пытается найти быстрый и простой способ получить необходимый документ, наша компания предлагает отличное решение. Приобрести диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к своим целям, будь то поступление в университет или начало карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Лучшие стратегии для игры в казино
Все о казино: правила игры, секреты успеха
[url=[Link deleted]казино[/url]
<a href="[Link deleted]
情報がとても整理されていて、理解しやすかったです。
В нашем мире, где диплом становится началом удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Факт наличия официального документа переоценить попросту невозможно. Ведь диплом открывает дверь перед людьми, желающими вступить в профессиональное сообщество или учиться в высшем учебном заведении.
Наша компания предлагает быстро получить этот важный документ. Вы сможете заказать диплом старого или нового образца, и это является отличным решением для всех, кто не смог завершить образование или утратил документ. дипломы выпускаются с особой аккуратностью, вниманием ко всем элементам, чтобы на выходе получился 100% оригинальный документ.
Превосходство такого подхода состоит не только в том, что вы максимально быстро получите свой диплом. Процесс организован просто и легко, с нашей поддержкой. От выбора подходящего образца диплома до точного заполнения персональной информации и доставки в любое место России — все под абсолютным контролем качественных мастеров.
Для всех, кто пытается найти быстрый и простой способ получения требуемого документа, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать продолжительного обучения и сразу переходить к своим целям: к поступлению в университет или к началу успешной карьеры.
[Link deleted]
[url=[Link deleted]canada no prescription[/url]
Попробуйте уникальные слоты и рулетку в онлайн казино Беларусь с привлекательными условиями
онлайн казино Беларусь [url=[Link deleted]онлайн казино в Беларуси[/url] .
Побеждайте вместе с друзьями в онлайн казино Беларусь на платформе с высокими оценками
онлайн казино Беларусь [url=[Link deleted]казино Беларусь[/url] .
Наслаждайтесь азартом в онлайн казино Беларусь с бонусами за регистрацию
онлайн казино Беларусь [url=[Link deleted]казино Беларусь[/url] .
Thank you, I have recently been searching for info about this subject for a while and yours is the best I have discovered till now. However, what about the conclusion? Are you sure about the source?
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем мире, где диплом становится началом удачной карьеры в любой области, многие ищут максимально быстрый путь получения качественного образования. Наличие документа об образовании переоценить попросту невозможно. Ведь именно он открывает двери перед каждым человеком, который собирается начать профессиональную деятельность или учиться в каком-либо ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы можете заказать диплом нового или старого образца, что становится отличным решением для человека, который не смог завершить образование или утратил документ. Любой диплом изготавливается с особой тщательностью, вниманием ко всем нюансам. В итоге вы получите документ, полностью соответствующий оригиналу.
Превосходство этого подхода заключается не только в том, что вы сможете быстро получить диплом. Весь процесс организован просто и легко, с нашей поддержкой. Начав от выбора нужного образца диплома до правильного заполнения личных данных и доставки в любой регион страны — все под абсолютным контролем квалифицированных мастеров.
В результате, для всех, кто хочет найти максимально быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать длительного обучения и сразу переходить к личным целям, будь то поступление в ВУЗ или начало карьеры.
[Link deleted]
[url=[Link deleted]88 lowest cost[/url]
[url=[Link deleted]buy online[/url]
[url=[Link deleted]pharmacy prices[/url]
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения образования. Факт наличия документа об образовании переоценить невозможно. Ведь именно диплом открывает дверь перед любым человеком, желающим начать профессиональную деятельность или продолжить обучение в любом университете.
В данном контексте наша компания предлагает максимально быстро получить этот важный документ. Вы сможете купить диплом старого или нового образца, что является удачным решением для человека, который не смог закончить обучение или утратил документ. диплом изготавливается с особой тщательностью, вниманием ко всем нюансам. В итоге вы сможете получить продукт, максимально соответствующий оригиналу.
Плюсы данного подхода заключаются не только в том, что можно оперативно получить свой диплом. Процесс организован удобно и легко, с профессиональной поддержкой. Начиная от выбора нужного образца документа до консультаций по заполнению персональной информации и доставки в любое место России — все будет находиться под полным контролем опытных мастеров.
Таким образом, для тех, кто пытается найти быстрый и простой способ получения требуемого документа, наша компания может предложить отличное решение. Заказать диплом – значит избежать длительного процесса обучения и не теряя времени перейти к своим целям: к поступлению в университет или к началу успешной карьеры.
[Link deleted]
[url=[Link deleted]prescription prenisone[/url]
DichaelVab
Добрый день!
Диплом теперь продвигается благодаря обширным онлайн-материалам.
На нашем сайте вы можете купить диплом ВУЗа, недорого, с оплатой после получения, поддержка 24/7.
Желаю всем пятерочных) оценок!
купить диплом косметолога
купить диплом переводчика
купить диплом в ставрополе
купить диплом в перми
купить диплом мастера маникюра и педикюра
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]price canada[/url]
[url=[Link deleted]online pharmacy[/url]
<a href="[Link deleted]
그러나 사실 왕수인은 이상한 이론으로 그를 당황하게 만들었다.
[url=[Link deleted]family store viagra[/url]
В нашем мире, где диплом – это начало удачной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения образования. Факт наличия официального документа об образовании переоценить невозможно. Ведь диплом открывает двери перед всеми, кто собирается начать профессиональную деятельность или учиться в университете.
Наша компания предлагает быстро получить этот важный документ. Вы сможете купить диплом старого или нового образца, и это будет удачным решением для всех, кто не смог закончить обучение или потерял документ. Любой диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим деталям, чтобы в результате получился продукт, максимально соответствующий оригиналу.
Преимущество этого подхода состоит не только в том, что вы оперативно получите свой диплом. Процесс организовывается комфортно и легко, с нашей поддержкой. От выбора подходящего образца диплома до точного заполнения личной информации и доставки в любой регион России — все под полным контролем опытных специалистов.
Всем, кто хочет найти быстрый и простой способ получения требуемого документа, наша компания может предложить выгодное решение. Купить диплом – это значит избежать продолжительного процесса обучения и сразу перейти к достижению личных целей: к поступлению в ВУЗ или к началу удачной карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В современном мире, где диплом – это начало удачной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Факт наличия официального документа переоценить невозможно. Ведь именно он открывает двери перед каждым человеком, который собирается начать трудовую деятельность или продолжить обучение в университете.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы сможете заказать диплом, и это становится выгодным решением для человека, который не смог завершить образование, потерял документ или хочет исправить плохие оценки. Все дипломы выпускаются аккуратно, с особым вниманием ко всем деталям. На выходе вы сможете получить полностью оригинальный документ.
Преимущества такого подхода заключаются не только в том, что можно оперативно получить свой диплом. Процесс организован просто и легко, с нашей поддержкой. От выбора подходящего образца документа до грамотного заполнения персональных данных и доставки по России — все под абсолютным контролем качественных мастеров.
Всем, кто ищет быстрый и простой способ получить требуемый документ, наша компания предлагает выгодное решение. Купить диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к достижению личных целей: к поступлению в ВУЗ или к началу удачной карьеры.
[Link deleted]
[url=[Link deleted]purchase[/url]
DichaelVab
Всем хорошего дня!
Диплом стал кошмаром, когда я отложил его выполнение и перешел на ночной график.
Приобретайте диплом университета без предоплаты у нас с доставкой в любой город России, гарантированное качество и безопасность.
Желаю всем положительных оценок!
купить диплом в крыму
купить диплом в брянске
купить диплом в прокопьевске
купить диплом в анапе
купить диплом в балашихе
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Анализ Tether на нетронутость: Каким образом защитить собственные цифровые финансы
Все больше граждан обращают внимание для секурити собственных криптовалютных средств. Каждый день мошенники предлагают новые методы кражи цифровых средств, и также владельцы криптовалюты оказываются страдающими их обманов. Один из методов обеспечения безопасности становится тестирование бумажников в присутствие нелегальных средств.
Зачем это полезно?
Прежде всего, с тем чтобы обезопасить свои средства против мошенников или украденных монет. Многие специалисты сталкиваются с риском потери личных активов из-за обманных схем или грабежей. Тестирование кошельков позволяет обнаружить сомнительные транзакции а также предотвратить потенциальные убытки.
Что наша группа предоставляем?
Мы предоставляем сервис проверки электронных кошельков или операций для обнаружения начала фондов. Наша платформа анализирует информацию для обнаружения противозаконных операций и также оценки риска для вашего портфеля. Благодаря этой проверке, вы сможете избегать проблем с регуляторами и также предохранить себя от участия в противозаконных операциях.
Как происходит процесс?
Наша фирма сотрудничаем с лучшими аудиторскими компаниями, например Cure53, для того чтобы гарантировать аккуратность наших тестирований. Мы применяем современные технологии для выявления потенциально опасных транзакций. Ваши данные обрабатываются и сохраняются согласно с высокими нормами безопасности и конфиденциальности.
Как проверить собственные Tether на прозрачность?
При наличии желания убедиться, что ваши Tether-кошельки чисты, наш сервис предоставляет бесплатное тестирование первых пяти кошельков. Просто введите место личного кошелька на нашем сайте, а также наша команда предоставим вам подробный отчет о его положении.
Гарантируйте безопасность для ваши фонды уже сегодня!
Не рискуйте попасть в жертву дельцов или оказаться в неблагоприятную ситуацию по причине незаконных сделок. Посетите нашей команде, для того чтобы обезопасить ваши электронные активы и предотвратить неприятностей. Предпримите первый шаг к сохранности вашего криптовалютного портфеля сегодня!
[url=[Link deleted]1000mg online[/url]
В нашем мире, где диплом является началом удачной карьеры в любом направлении, многие ищут максимально простой путь получения качественного образования. Наличие официального документа об образовании трудно переоценить. Ведь именно диплом открывает двери перед всеми, кто стремится начать трудовую деятельность или продолжить обучение в каком-либо ВУЗе.
В данном контексте мы предлагаем оперативно получить любой необходимый документ. Вы сможете заказать диплом нового или старого образца, что становится выгодным решением для всех, кто не смог завершить образование, утратил документ или желает исправить плохие оценки. дипломы выпускаются с особой аккуратностью, вниманием ко всем нюансам, чтобы на выходе получился документ, максимально соответствующий оригиналу.
Плюсы подобного подхода состоят не только в том, что можно оперативно получить свой диплом. Процесс организован комфортно, с профессиональной поддержкой. Начиная от выбора требуемого образца до консультации по заполнению персональных данных и доставки по России — все находится под полным контролем качественных специалистов.
Всем, кто пытается найти быстрый способ получить требуемый документ, наша компания может предложить отличное решение. Купить диплом – это значит избежать продолжительного обучения и не теряя времени переходить к личным целям, будь то поступление в ВУЗ или начало трудовой карьеры.
[Link deleted]
[url=[Link deleted]otc uk[/url]
[url=[Link deleted]to get synthroid[/url]
В нашем обществе, где диплом – это начало отличной карьеры в любой отрасли, многие ищут максимально быстрый путь получения образования. Наличие официального документа переоценить попросту невозможно. Ведь диплом открывает двери перед людьми, стремящимися вступить в профессиональное сообщество или продолжить обучение в ВУЗе.
В данном контексте наша компания предлагает быстро получить этот необходимый документ. Вы сможете приобрести диплом, что будет удачным решением для человека, который не смог завершить образование, утратил документ или желает исправить плохие оценки. дипломы производятся с особой аккуратностью, вниманием ко всем нюансам, чтобы в результате получился 100% оригинальный документ.
Плюсы этого подхода заключаются не только в том, что вы сможете быстро получить свой диплом. Весь процесс организован удобно, с профессиональной поддержкой. От выбора необходимого образца диплома до правильного заполнения персональной информации и доставки по стране — все находится под абсолютным контролем квалифицированных специалистов.
Всем, кто пытается найти максимально быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать продолжительного процесса обучения и не теряя времени переходить к достижению своих целей, будь то поступление в ВУЗ или начало трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
<a href=[Link deleted]USDT на чистоту
Анализ USDT на чистоту: Как защитить свои цифровые состояния
Все более граждан заботятся для безопасность собственных электронных активов. Каждый день шарлатаны предлагают новые схемы разграбления цифровых средств, и держатели криптовалюты оказываются страдающими своих интриг. Один из методов обеспечения безопасности становится тестирование кошельков в присутствие незаконных денег.
Зачем это важно?
Прежде всего, для того чтобы сохранить личные средства от дельцов а также украденных монет. Многие участники сталкиваются с потенциальной угрозой утраты своих фондов в результате хищных планов или кражей. Осмотр кошельков позволяет выявить подозрительные операции а также предотвратить возможные убытки.
Что мы предлагаем?
Мы предоставляем подход проверки криптовалютных кошельков а также транзакций для выявления начала средств. Наша платформа анализирует данные для выявления нелегальных транзакций или оценки опасности вашего портфеля. Благодаря этой проверке, вы сможете избегнуть недочетов с регуляторами а также обезопасить себя от участия в противозаконных операциях.
Каким образом это работает?
Мы сотрудничаем с передовыми проверочными агентствами, вроде Kudelsky Security, с целью обеспечить точность наших проверок. Мы используем передовые технологии для выявления потенциально опасных операций. Ваши данные проходят обработку и сохраняются согласно с высокими нормами безопасности и конфиденциальности.
Как проверить свои USDT для чистоту?
В случае если вы желаете проверить, что ваши USDT-кошельки чисты, наш сервис предлагает бесплатную проверку первых пяти кошельков. Просто введите положение личного кошелька на на сайте, и мы предоставим вам детальный доклад о его статусе.
Гарантируйте безопасность для ваши активы уже сегодня!
Не подвергайте риску стать жертвой дельцов либо оказаться в неприятную обстановку вследствие нелегальных операций. Свяжитесь с нашей команде, с тем чтобы сохранить ваши цифровые средства и избежать сложностей. Совершите первый шаг к безопасности вашего криптовалютного портфеля уже сейчас!
[url=[Link deleted]online usa[/url]
Здравствуйте!
Закажите диплом ВУЗа с гарантированной подлинностью и доставкой по России без предварительной оплаты – просто, надежно, выгодно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
У нас на сайте можно недорого заказать и купить диплом с гарантией и доставкой покупателю в любой регион РФ
<a href="[Link deleted]
수도 전체가 Wang Zuo의 움직임을 면밀히 주시했습니다.
Добрый день всем!
Приобретите диплом ВУЗа с гарантированной доставкой по России и без предварительной оплаты – надежно и выгодно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
На нашем сайте вы можете заказать диплом Вуза с постоплатой и круглосуточной поддержкой.
[url=[Link deleted]cost of synthroid 100mcg[/url]
[url=[Link deleted]family store pharmacy viagra[/url]
<a href="[Link deleted]
素晴らしい記事。非常に役立つ情報を提供してくれてありがとうございます。
[url=[Link deleted]diuretic[/url]
Привет, дорогой читатель!
Компания предлагает купить диплом Вуза России недорого, без предоплаты и с гарантией возврата средств.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Получите российский диплом с гарантированной подлинностью и доставкой по всей стране без предварительной оплаты – просто и удобно!
[url=[Link deleted]brand[/url]
[url=[Link deleted]canadian pharmacy rx[/url]
For newest information you have to go to see world-wide-web and on world-wide-web I found this site as a best web page for latest updates.
<a href="[Link deleted]
StephenRom
Приветики, дорогие мои!!
В интернете я нашел ресурсы для диплома, которые помогли мне ускорить написание.
Приобретайте диплом университета без предоплаты с доставкой по всей России.
Желаю вам всем отличных отметок!
купить диплом в верхней пышме
купить диплом в нефтеюганске
купить диплом штукатура
купить диплом в волжском
купить диплом в елабуге
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Привет всем!
Получите российский диплом с гарантированной доставкой в любую точку страны без предварительной оплаты – просто и надежно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Предлагаем всем желающим приобрести диплом университетов России по низкой цене с доставкой в руки под ключ
[url=[Link deleted]otc pharmacy[/url]
[url=[Link deleted]0.125[/url]
Привет всем!
Приобретите диплом ВУЗа с гарантированной доставкой по России и без предварительной оплаты – надежно и выгодно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Наши услуги позволят вам заказать документы об образовании всех ВУЗов России с доставкой по РФ и оплатой после получения – надежно и удобно!
[url=[Link deleted]pharmacy pain relief[/url]
[url=[Link deleted]family pharmacy[/url]
<a href="[Link deleted]
Wang Shouren과 Tang Yin은 일제히 서로를 바라보다가… 심호흡을 했습니다.
Приветики!
Получите документ ВУЗа без предоплаты и доставку в руки по России – просто, удобно, безопасно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Приобретите диплом института или колледжа недорого с доставкой по РФ и гарантией качества без предварительной оплаты!
In diesem Kapitel gehen wir daher auf die verschiedenen Risiken ein, mit denen Anlegerinnen und Anleger konfrontiert sind, wenn sie in Kryptowährungen investieren. Anleger können selbst entscheiden, welche Strategie für sie geeignet ist. Durch den limitierten Zugang zu börsengehandelten Bitcoin ETFs steht das Angebot von Bitcoin ETF Token häufig ganz oben auf der Wunschliste von Krypto-Tradern. Doch Sie sollten unbedingt über die Unterschiede informiert sein. Die nachfolgende Tabelle zeigt genau auf, worin sich Bitcoin ETF Token und Bitcoin ETFs unterschieden. Der Bitcoin entstand 2009. Er ist in den vergangenen Jahren (fälschlicherweise) zu einem Synonym für andere digitale Währungen wie Ethereum, Ripple, Litecoin oder Peercoin geworden. Der Begriff Bitcoin stammt aus dem Englischen. Auf Deutsch heißt er „digitale Münze“. Im Gegensatz zu Euro, Dollar oder Pfund existieren digitale Währungen lediglich virtuell. Um sie besser zu verstehen, helfen einige zentrale Punkte:
[Link deleted]
KLICKE AUF DIESEN LINK, UM IN KRYPTOWÄHRUNGEN BEI COINBASE ZU INVESTIEREN! Von den Tätern werden die Betrugsopfer detailliert angeleitet, wie sie sich mit Bitcoin “eindecken” können und wohin die Coins zu schicken sind. Natürlich in die privaten Wallets der Abzocker, doch das wissen die Betroffenen nicht. Für eine fehlerfreie Darstellung verwenden Sie bitte einen anderen Browser, beispielsweise: Microsoft Edge, Mozilla Firefox, Google Chrome oder Apple Safari. Video laden Mit einem Mining Pool treten Tausende von Minern in einer Gruppe auf, die sich gemeinsam auf die Suche nach neuen Datenblöcken machen. Warum ist das aber überhaupt nötig? Mit der Einführung des Bitcoins im Jahr 2009 wurde für neue Miner eine Belohnung von 50 BTC festgelegt, um dem Netzwerk zu einem schnellen Wachstum zu verhelfen. Mehr als ein Jahrzehnt später haben sich allerdings so viele Anhänger dem Ökosystem angeschlossen, dass die Aufgaben zur Entschlüsselung eines Datenblocks für Einzelpersonen nicht mehr machbar sind.
[url=[Link deleted]non prescription pharmacies[/url]
[url=[Link deleted]60 tablets 1000 mg[/url]
[url=[Link deleted]prednisone daily[/url]
Привет, дорогой читатель!
Закажите диплом института или техникума по доступной цене с гарантированной доставкой в любой уголок России без предоплаты!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
У нас вы можете заказать диплом Гознака по специальной цене с доставкой в любой регион России без предоплаты – надежно и выгодно!
В нашем мире, где диплом является началом успешной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа сложно переоценить. Ведь именно диплом открывает двери перед любым человеком, который желает вступить в сообщество профессионалов или продолжить обучение в университете.
В данном контексте мы предлагаем быстро получить любой необходимый документ. Вы сможете приобрести диплом старого или нового образца, что является отличным решением для человека, который не смог закончить обучение или потерял документ. диплом изготавливается с особой аккуратностью, вниманием ко всем деталям. В результате вы получите документ, полностью соответствующий оригиналу.
Плюсы подобного подхода состоят не только в том, что можно максимально быстро получить свой диплом. Процесс организован просто и легко, с профессиональной поддержкой. От выбора нужного образца до грамотного заполнения личной информации и доставки в любой регион России — все под полным контролем качественных мастеров.
Таким образом, для тех, кто ищет максимально быстрый способ получить требуемый документ, наша услуга предлагает отличное решение. Купить диплом – значит избежать продолжительного процесса обучения и не теряя времени перейти к достижению собственных целей, будь то поступление в ВУЗ или старт успешной карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]to buy azithromycin over the counter[/url]
[url=[Link deleted]10 mg online no prescription[/url]
Everything You Need to Know
2. Aviator Games: Test Your Flying Skills in this Exciting Challenge
3. Get Ready to Soar: Aviator Games for Thrill Seekers
4. Master the Sky: Aviator Games for Aviation Enthusiasts
5. Take Flight with Aviator Games: A High-Flying Adventure
6. Challenge Yourself with Aviator Games: Are You Ready to Take On the Sky?
7. The Sky’s the Limit: Aviator Games for Daredevils
8. Aviator Games: The Perfect Way to Experience the Thrill of Flying
9. Fly High with Aviator Games: An Exciting Journey Awaits
10. Unleash Your Inner Pilot: Aviator Games for Flying Enthusiasts
11. Reach New Heights with Aviator Games: The Sky Awaits
12. Aviator Games: A Test of Skill and Courage in the Sky
13. Take to the Skies with Aviator Games: A Thrilling Adventure Awaits
14. Aviator Games: Where Every Landing is a Victory
15. Ready for Takeoff: Aviator Games for the Brave and Bold
16. Conquer the Clouds with Aviator Games: A Challenge Like No Other
17. Aviator Games: Prepare for a High-Flying Experience
18. Fly Like a Pro with Aviator Games: The Sky’s the Limit
19. Aviator Games: The Ultimate Test for Aspiring Pilots
20. Soar to New Heights with Aviator Games: Are You Ready for the Challenge?
aviator slot [url=[Link deleted]slot[/url] .
[url=[Link deleted]valtrex generic[/url]
1. The Ultimate Aviator Games Guide
aviator slot [url=[Link deleted]peru[/url] .
GichardCiz
Добрый день!
Написание диплома стало менее обременительным благодаря онлайн-ресурсам, которые я нашел.
Закажите диплом у нас и получите его быстро и безопасно с оплатой по факту доставки, отправка в любой регион России.
Желаю каждому прекрасных отметок!
купить диплом в калуге
купить диплом в елабуге
купить диплом в керчи
купить диплом в новомосковске
купить диплом в кисловодске
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Здравствуйте!
Получите документ об образовании по выгодной цене с доставкой по РФ и оплатой после получения.
Приобретите документ об образовании по выгодной цене с доставкой по РФ и оплатой после получения ваших руками!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
1. The Ultimate Aviator Games Guide
juego del avion casino [url=[Link deleted]del aviator[/url] .
[url=[Link deleted]200mg[/url]
[url=[Link deleted]pharmacy online[/url]
[url=[Link deleted]zpak[/url]
В современном мире, где диплом – это начало успешной карьеры в любой отрасли, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие официального документа об образовании переоценить просто невозможно. Ведь именно он открывает дверь перед людьми, желающими вступить в профессиональное сообщество или учиться в ВУЗе.
Наша компания предлагает быстро получить этот важный документ. Вы сможете заказать диплом, и это будет выгодным решением для человека, который не смог завершить образование, утратил документ или желает исправить плохие оценки. Каждый диплом изготавливается с особой тщательностью, вниманием ко всем элементам. В результате вы получите 100% оригинальный документ.
Превосходство данного решения состоит не только в том, что вы быстро получите диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. От выбора подходящего образца до консультаций по заполнению личных данных и доставки в любое место России — все находится под абсолютным контролем квалифицированных мастеров.
В результате, для всех, кто ищет оперативный способ получения необходимого документа, наша компания предлагает отличное решение. Купить диплом – это значит избежать длительного процесса обучения и не теряя времени переходить к достижению своих целей: к поступлению в ВУЗ или к началу трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Привет, дорогой читатель!
На нашем сайте вы можете заказать диплом ВУЗа недорого с возможностью оплаты после получения и круглосуточной поддержкой!
Закажите диплом Вуза по выгодной цене с доставкой в любой регион России без предоплаты и уверенностью в его законности.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]hcl 1000 mg[/url]
<a href="[Link deleted]カジノ スロット
この記事は本当に役に立ちました。素晴らしい仕事を続けてください。
Привет всем!
Купите диплом ВУЗа по выгодной цене с гарантией качества и доставкой в любой город России без предоплаты – просто и надежно!
Закажите диплом ВУЗа по выгодной цене с доставкой в любой регион России без предоплаты и с полной уверенностью в его законности!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем обществе, где диплом является началом удачной карьеры в любой сфере, многие стараются найти максимально быстрый и простой путь получения качественного образования. Важность наличия официального документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед людьми, желающими начать трудовую деятельность или продолжить обучение в любом университете.
В данном контексте наша компания предлагает очень быстро получить этот важный документ. Вы сможете приобрести диплом, что является удачным решением для всех, кто не смог закончить обучение или утратил документ. дипломы выпускаются с особой тщательностью, вниманием ко всем деталям. На выходе вы сможете получить продукт, 100% соответствующий оригиналу.
Превосходство такого решения заключается не только в том, что вы быстро получите диплом. Процесс организован удобно, с нашей поддержкой. Начав от выбора подходящего образца до консультации по заполнению персональной информации и доставки в любой регион страны — все под абсолютным контролем качественных специалистов.
Всем, кто ищет быстрый и простой способ получить требуемый документ, наша компания может предложить отличное решение. Заказать диплом – это значит избежать продолжительного обучения и сразу перейти к своим целям: к поступлению в ВУЗ или к началу трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем обществе, где диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить попросту невозможно. Ведь именно он открывает двери перед любым человеком, который хочет вступить в профессиональное сообщество или учиться в высшем учебном заведении.
В данном контексте наша компания предлагает быстро получить этот важный документ. Вы можете купить диплом, что будет удачным решением для человека, который не смог завершить образование или потерял документ. Все дипломы изготавливаются аккуратно, с максимальным вниманием ко всем нюансам, чтобы в итоге получился полностью оригинальный документ.
Превосходство подобного решения заключается не только в том, что вы сможете максимально быстро получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. Начиная от выбора требуемого образца документа до консультаций по заполнению персональной информации и доставки в любой регион России — все находится под полным контролем наших специалистов.
В результате, для тех, кто ищет максимально быстрый способ получения необходимого документа, наша компания готова предложить отличное решение. Заказать диплом – значит избежать длительного обучения и сразу переходить к своим целям, будь то поступление в университет или начало карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
<a href="[Link deleted]
사실 쉬징… 양젠은 여전히 좋은 인상을 가지고 있습니다.
В нашем обществе, где диплом становится началом удачной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Необходимость наличия документа об образовании переоценить просто невозможно. Ведь именно он открывает двери перед любым человеком, желающим вступить в профессиональное сообщество или учиться в высшем учебном заведении.
Предлагаем максимально быстро получить этот важный документ. Вы сможете купить диплом нового или старого образца, что будет удачным решением для человека, который не смог закончить обучение или утратил документ. диплом изготавливается аккуратно, с максимальным вниманием к мельчайшим элементам, чтобы в итоге получился продукт, 100% соответствующий оригиналу.
Преимущество данного подхода состоит не только в том, что вы сможете максимально быстро получить свой диплом. Весь процесс организован удобно, с нашей поддержкой. Начав от выбора нужного образца до консультации по заполнению персональной информации и доставки в любое место России — все под абсолютным контролем наших специалистов.
Для тех, кто ищет быстрый и простой способ получить требуемый документ, наша компания предлагает выгодное решение. Купить диплом – значит избежать длительного обучения и сразу перейти к достижению своих целей, будь то поступление в университет или старт трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]without rx[/url]
<a href=[Link deleted]от сво
С началом СВО уже спустя полгода была объявлена первая волна мобилизации. При этом прошлая, в последний раз в России была аж в 1941 году, с началом Великой Отечественной Войны. Конечно же, желающих отправиться на фронт было не много, а потому люди стали искать способы не попасть на СВО, для чего стали покупать справки о болезнях, с которыми можно получить категорию Д. И все это стало возможным с даркнет сайтами, где можно найти практически все что угодно. Именно об этой отрасли темного интернета подробней и поговорим в этой статье.
[url=[Link deleted]cialis online australia[/url]
[url=[Link deleted]india[/url]
[url=[Link deleted]cheap lisinopril 40 mg no prescription[/url]
<a href="[Link deleted]
포르투갈 총독은 그것에 대해 생각했지만 곧 평정을 되찾았습니다.
67. Клининговая компания в Челябинске предоставляет услуги по уборке после крупных мероприятий, таких как конференции, выставки и фестивали, включая сбор мусора, уборку торговых зон, мойку полов и другие работы для восстановления порядка.
[url=[Link deleted]Челябинск[/url] .
3. Клининговая компания “Челябинск” специализируется на генеральной уборке помещений любой сложности. Наши профессиональные уборщицы используют современное оборудование и экологически безопасные средства для тщательной очистки вашего дома или офиса.
[url=[Link deleted]Челябинск[/url] .
[url=[Link deleted]250 mg buy online[/url]
[url=[Link deleted]family store[/url]
21.
[url=[Link deleted]Челябинск[/url] .
[url=[Link deleted]generic canada[/url]
В нашем обществе, где диплом – это начало отличной карьеры в любом направлении, многие стараются найти максимально быстрый и простой путь получения образования. Наличие официального документа переоценить просто невозможно. Ведь именно он открывает дверь перед любым человеком, желающим начать трудовую деятельность или учиться в ВУЗе.
Предлагаем максимально быстро получить любой необходимый документ. Вы имеете возможность купить диплом, и это будет выгодным решением для человека, который не смог завершить образование, утратил документ или хочет исправить свои оценки. дипломы производятся с особой тщательностью, вниманием ко всем деталям. На выходе вы сможете получить продукт, максимально соответствующий оригиналу.
Преимущества данного решения заключаются не только в том, что вы сможете максимально быстро получить диплом. Процесс организован удобно, с нашей поддержкой. Начав от выбора нужного образца до точного заполнения персональных данных и доставки в любое место России — все под абсолютным контролем опытных мастеров.
Всем, кто пытается найти оперативный способ получить требуемый документ, наша компания может предложить отличное решение. Купить диплом – значит избежать длительного процесса обучения и не теряя времени перейти к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
В нашем обществе, где диплом – это начало успешной карьеры в любой отрасли, многие стараются найти максимально быстрый и простой путь получения образования. Факт наличия официального документа об образовании переоценить невозможно. Ведь диплом открывает дверь перед людьми, желающими вступить в профессиональное сообщество или учиться в университете.
В данном контексте наша компания предлагает очень быстро получить этот необходимый документ. Вы имеете возможность купить диплом, и это является выгодным решением для человека, который не смог закончить обучение, утратил документ или хочет исправить плохие оценки. Все дипломы изготавливаются с особой аккуратностью, вниманием к мельчайшим элементам, чтобы в результате получился полностью оригинальный документ.
Плюсы этого решения заключаются не только в том, что вы сможете быстро получить диплом. Весь процесс организован комфортно, с нашей поддержкой. Начиная от выбора нужного образца документа до консультации по заполнению личной информации и доставки в любое место России — все находится под полным контролем качественных мастеров.
Всем, кто хочет найти оперативный способ получения требуемого документа, наша компания может предложить отличное решение. Приобрести диплом – значит избежать продолжительного обучения и не теряя времени переходить к достижению личных целей: к поступлению в университет или к началу трудовой карьеры.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Its like you read my mind! You seem to know a lot about this, like you wrote the book in it or something. I think that you can do with a few pics to drive the message home a bit, but other than that, this is excellent blog. A great read. I’ll definitely be back.
<a href=[Link deleted]
[url=[Link deleted]2.5 tablet[/url]
Где купить диплом высшего образования
купить диплом [url=[Link deleted].
<a href="[Link deleted]
이에 반해 북도 밖의 반란은 속속 일어났다.
무료로 즐길 수 있는 프라그마틱 슬롯로 새로운 게임을 경험하고 보상을 획득하세요.
<a href="[Link deleted]
프라그마틱 관련 내용 감사합니다! 또한, 제 사이트에서도 프라그마틱에 대한 유용한 정보를 공유하고 있어요. 함께 서로 이야기하며 더 많은 지식을 쌓아가요!
[Link deleted]
[Link deleted]
[Link deleted]
На сегодняшний день, когда диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения образования. Наличие официального документа переоценить невозможно. Ведь именно диплом открывает дверь перед всеми, кто хочет начать трудовую деятельность или продолжить обучение в ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы сможете заказать диплом нового или старого образца, что будет удачным решением для всех, кто не смог закончить обучение или утратил документ. Все дипломы изготавливаются с особой тщательностью, вниманием ко всем деталям, чтобы в итоге получился документ, полностью соответствующий оригиналу.
Преимущества такого подхода состоят не только в том, что можно максимально быстро получить диплом. Весь процесс организован удобно, с профессиональной поддержкой. Начав от выбора подходящего образца до точного заполнения персональных данных и доставки в любое место России — все находится под полным контролем качественных мастеров.
Для тех, кто ищет максимально быстрый способ получить требуемый документ, наша услуга предлагает выгодное решение. Купить диплом – это значит избежать длительного обучения и не теряя времени перейти к важным целям: к поступлению в ВУЗ или к началу трудовой карьеры.
<a href=[Link deleted]
<a href="[Link deleted]カジノ バニー
このブログは本当に役立つ情報が満載で、大好きです。
[url=[Link deleted]otc canada[/url]
[url=[Link deleted]canada[/url]
Здравствуйте!
У нас вы можете заказать диплом Гознака по специальной цене с доставкой в любой регион России без предоплаты – надежно и выгодно!
Компания предлагает купить диплом Вуза России недорого, без предоплаты и с гарантией возврата средств.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Привет, дорогой читатель!
Приобретите российский диплом по выгодной цене с гарантией прохождения проверок и доставкой в любой город РФ!
Приобретите диплом колледжа недорого с доставкой по РФ и гарантией качества без предварительной оплаты – просто и надежно!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]pharmaceutical prices[/url]
[url=[Link deleted]shop[/url]
Доброго всем дня!
Закажите российский диплом у нас по доступной цене с гарантией прохождения проверок и доставкой по РФ.
Купите диплом ВУЗа по выгодной цене с гарантией качества и доставкой в любой город России без предоплаты!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]i order lisinopril online[/url]
[url=[Link deleted]135 mcg[/url]
[url=[Link deleted]family store coupon code pharmacy[/url]
[url=[Link deleted]tadalafil 5mg[/url]
В современном мире, где диплом – это начало отличной карьеры в любой сфере, многие стараются найти максимально простой путь получения качественного образования. Важность наличия официального документа об образовании переоценить невозможно. Ведь именно он открывает двери перед людьми, стремящимися вступить в сообщество профессиональных специалистов или учиться в любом ВУЗе.
В данном контексте наша компания предлагает оперативно получить этот необходимый документ. Вы имеете возможность заказать диплом, что будет выгодным решением для человека, который не смог закончить обучение или потерял документ. дипломы производятся с особой тщательностью, вниманием к мельчайшим деталям. В итоге вы сможете получить документ, максимально соответствующий оригиналу.
Превосходство такого решения состоит не только в том, что вы максимально быстро получите диплом. Процесс организовывается удобно, с профессиональной поддержкой. От выбора требуемого образца документа до правильного заполнения личной информации и доставки в любой регион России — все находится под полным контролем квалифицированных мастеров.
В результате, всем, кто пытается найти быстрый способ получить необходимый документ, наша компания готова предложить выгодное решение. Заказать диплом – значит избежать продолжительного процесса обучения и сразу перейти к достижению своих целей: к поступлению в университет или к началу удачной карьеры.
<a href=[Link deleted]
В нашем мире, где диплом – это начало успешной карьеры в любой области, многие ищут максимально простой путь получения качественного образования. Факт наличия документа об образовании переоценить просто невозможно. Ведь диплом открывает дверь перед всеми, кто собирается вступить в сообщество профессионалов или учиться в высшем учебном заведении.
В данном контексте мы предлагаем оперативно получить этот важный документ. Вы имеете возможность приобрести диплом старого или нового образца, что становится выгодным решением для человека, который не смог завершить образование, потерял документ или желает исправить свои оценки. дипломы производятся аккуратно, с особым вниманием ко всем элементам. В результате вы получите продукт, 100% соответствующий оригиналу.
Превосходство этого подхода заключается не только в том, что можно оперативно получить диплом. Весь процесс организовывается просто и легко, с профессиональной поддержкой. Начав от выбора требуемого образца до консультаций по заполнению персональной информации и доставки по России — все будет находиться под абсолютным контролем качественных мастеров.
Для тех, кто ищет быстрый способ получения необходимого документа, наша услуга предлагает отличное решение. Приобрести диплом – это значит избежать продолжительного обучения и не теряя времени переходить к достижению своих целей: к поступлению в ВУЗ или к началу удачной карьеры.
<a href=[Link deleted]
Tremendous issues here. I am very satisfied to look your article. Thanks so much and I am looking ahead to contact you. Will you please drop me a e-mail?
<a href=[Link deleted]
<a href="[Link deleted]
Liu Xiunv는 약간의 두려움으로 Zhu Houzhao의 시선을 바라보며 소심하게 고개를 끄덕였습니다.
Привет, дорогой читатель!
Недорого предлагаем заказать диплом без предоплаты с доставкой курьером по РФ, под ключ!
Хотите купить диплом Вуза недорого и получить его почтой без предоплаты? Мы можем помочь вам сделать это.
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
No, you can’t withdraw your Slots Empire bonuses right after you claim them. All offers on this casino site (and all other casinos) are subject to different wagering requirements that range from 20x to 50x. You’ll need to play through them so make sure to check out the terms and conditions for the specific bonus code you’re using. The same casino as lucky hippo casino , by design. i got very easily no deposit bonus, but i lost it all also very easily. I tried on at least 15 slots with minimal bet, but games are just too tight. Slots Empire no deposit casino bonus for US players offer an attractive bonus for both new and experienced players. This bonus allows players to explore the casino’s selection of games without having to risk any of their own money, which can be a great way to get to know the casino before making a deposit. With this bonus, players can enjoy their favorite casino games without spending money.
[Link deleted]
Play Game of Thrones Slots Casino free online slots today! Join Zynga Poker for some fun with your friends, or enjoy a little friendly competition against millions of other users, 24 7, 365 days a year. If you are looking for valid and shared gifts from other gamers are here. Also freebies from others sites, official Facebook page, Twitter page, Instagram account of the game and others are also here! We are always trying to update this newly freebies and giveaways. Collect all this gifts and freebies that your great game to offer. Scatter slots free coins 2. Log in every day to collect daily bonuses, which can be redeemed for coins and spins. world series of poker free chips Whose side are you on? Spin in The Greens & the Blacks today for a chance at extra rewards!Free Coins: gotslots.onelink.me bOrX qrgfk79z Restrictions may apply.
<a href=[Link deleted]
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
В нашем мире, где диплом – это начало удачной карьеры в любом направлении, многие пытаются найти максимально быстрый и простой путь получения качественного образования. Наличие документа об образовании переоценить невозможно. Ведь диплом открывает двери перед любым человеком, желающим вступить в профессиональное сообщество или учиться в любом ВУЗе.
Мы предлагаем быстро получить этот важный документ. Вы сможете заказать диплом, и это является выгодным решением для всех, кто не смог закончить образование, утратил документ или желает исправить свои оценки. Каждый диплом изготавливается аккуратно, с особым вниманием ко всем нюансам. На выходе вы получите полностью оригинальный документ.
Превосходство данного подхода состоит не только в том, что вы сможете максимально быстро получить диплом. Весь процесс организовывается удобно, с профессиональной поддержкой. Начиная от выбора необходимого образца диплома до консультаций по заполнению личных данных и доставки по России — все находится под полным контролем квалифицированных мастеров.
Таким образом, для тех, кто ищет быстрый способ получения требуемого документа, наша компания предлагает выгодное решение. Заказать диплом – это значит избежать продолжительного обучения и сразу перейти к своим целям, будь то поступление в университет или начало карьеры.
<a href=[Link deleted]
В современном мире, где диплом – это начало успешной карьеры в любой сфере, многие ищут максимально быстрый путь получения качественного образования. Важность наличия документа об образовании переоценить попросту невозможно. Ведь диплом открывает двери перед любым человеком, желающим начать профессиональную деятельность или продолжить обучение в университете.
Наша компания предлагает очень быстро получить этот необходимый документ. Вы имеете возможность приобрести диплом, и это является удачным решением для всех, кто не смог закончить обучение или утратил документ. Все дипломы изготавливаются с особой аккуратностью, вниманием к мельчайшим деталям, чтобы в итоге получился продукт, полностью соответствующий оригиналу.
Плюсы подобного решения состоят не только в том, что вы сможете оперативно получить свой диплом. Весь процесс организовывается удобно, с нашей поддержкой. Начав от выбора нужного образца диплома до грамотного заполнения личной информации и доставки в любой регион России — все под абсолютным контролем наших мастеров.
Всем, кто ищет оперативный способ получить необходимый документ, наша услуга предлагает отличное решение. Заказать диплом – значит избежать длительного процесса обучения и не теряя времени перейти к важным целям, будь то поступление в ВУЗ или начало профессиональной карьеры.
<a href=[Link deleted]
[url=[Link deleted]european online pharmacy[/url]
[url=[Link deleted]neighbor pharmacy[/url]
[url=[Link deleted]in australia[/url]
<a href=[Link deleted]
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
[url=[Link deleted]brand name in usa[/url]
<a href="[Link deleted]
사실 반란군은 조직이 전혀 없습니다.
[url=[Link deleted]scripts com pharmacies[/url]
[url=[Link deleted]10 mg prices[/url]
В современном мире, где диплом – это начало успешной карьеры в любой сфере, многие ищут максимально быстрый и простой путь получения образования. Необходимость наличия официального документа об образовании переоценить невозможно. Ведь диплом открывает двери перед людьми, стремящимися начать трудовую деятельность или учиться в высшем учебном заведении.
Наша компания предлагает очень быстро получить этот важный документ. Вы имеете возможность заказать диплом нового или старого образца, и это становится отличным решением для человека, который не смог закончить обучение или потерял документ. Все дипломы выпускаются аккуратно, с максимальным вниманием ко всем деталям. В результате вы получите полностью оригинальный документ.
Превосходство этого подхода состоит не только в том, что можно оперативно получить свой диплом. Весь процесс организовывается комфортно, с нашей поддержкой. Начав от выбора требуемого образца до консультации по заполнению персональной информации и доставки в любой регион России — все будет находиться под полным контролем наших специалистов.
Таким образом, для всех, кто ищет максимально быстрый способ получить требуемый документ, наша компания может предложить выгодное решение. Приобрести диплом – значит избежать длительного процесса обучения и сразу переходить к достижению своих целей: к поступлению в ВУЗ или к началу трудовой карьеры.
<a href=[Link deleted]
프라그마틱 슬롯에 대한 설명 감사합니다! 또한, 제 사이트에서도 프라그마틱과 관련된 정보를 얻을 수 있어요. 함께 이야기 나누면서 더 많은 지식을 얻어가요!
<a href="[Link deleted]
프라그마틱 슬롯에 대한 정보가 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 내용을 찾아보세요. 함께 이야기 나누면서 더 많은 지식을 얻어가요!
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]10mg for sale[/url]
[url=[Link deleted]of synthroid 75 mcg[/url]
[url=[Link deleted]medication valtrex[/url]
[url=[Link deleted]5 mg price in india[/url]
<a href="[Link deleted]
내가 성인과 성인의 책을 읽고 공덕과 계율과 말을 했을 때, 내가 어떻게 립 서비스가 될 수 있겠습니까?
<a href="[Link deleted]カジノ kyc
素晴らしい情報源です。いつも参考になります。
[url=[Link deleted]canadian online pharmacies[/url]
Why visitors still use to read news papers when in this technological world everything is accessible on net?
[Link deleted]
[url=[Link deleted]metformin online[/url]
В современном мире, где диплом – это начало отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения образования. Наличие документа об образовании сложно переоценить. Ведь именно он открывает дверь перед любым человеком, который хочет начать трудовую деятельность или продолжить обучение в университете.
В данном контексте наша компания предлагает оперативно получить этот важный документ. Вы сможете заказать диплом старого или нового образца, и это является удачным решением для всех, кто не смог завершить образование, утратил документ или желает исправить свои оценки. Все дипломы изготавливаются аккуратно, с максимальным вниманием ко всем деталям, чтобы в результате получился документ, 100% соответствующий оригиналу.
Превосходство такого решения состоит не только в том, что можно оперативно получить свой диплом. Весь процесс организован удобно, с профессиональной поддержкой. Начиная от выбора требуемого образца до консультации по заполнению персональных данных и доставки по России — все находится под абсолютным контролем наших мастеров.
Для всех, кто ищет быстрый способ получить требуемый документ, наша компания предлагает выгодное решение. Приобрести диплом – это значит избежать длительного обучения и не теряя времени перейти к достижению личных целей, будь то поступление в университет или начало карьеры.
http://www.vuzdiploma.ru
[url=[Link deleted]10 best price[/url]
Hi there, You have done an incredible job. I will certainly digg it and personally recommend to my friends. I am sure they’ll be benefited from this website.
[Link deleted]
[url=[Link deleted]cheap lisinopril[/url]
Автор 24 – это надежный сервис для заказа многочисленных академических работ. Он занимается на рефератах, а также задачах. Кроме того, на платформе Автор 24 можно купить эссе, презентации. Это эффективный способ получить профессиональную помощь.
Автор 24 официальный [url=[Link deleted]24 ру[/url] .
Привет, дорогой читатель!
Получите диплом ВУЗа без предварительной оплаты с доставкой по всей России – просто, надежно, выгодно!
Закажите диплом ВУЗа с доставкой по всей России без предоплаты и с гарантией качества!
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
[Link deleted]
Автор 24 – это высококачественный сервис для приобретения различных академических работ. Он специализируется на рефератах, а также чертежах. Кроме того, на Автор 24 можно купить очерки, отчеты о прохождении практики. Это удобный способ повысить свои академические результаты.
Автор 24 [url=[Link deleted]24[/url] .
[url=[Link deleted]20mg for sale[/url]
<a href="[Link deleted]
Liu Wenshan은 어쩔 수 없이 쓴웃음을 지었지만 스승을 고맙게 바라보았습니다.
[url=[Link deleted]pharmacy delivery delhi[/url]
[url=[Link deleted]pharmacy viagra 50 mg[/url]
[url=[Link deleted]prednisone online cheap[/url]
[url=[Link deleted]100 mcg price[/url]
<a href="[Link deleted]
미래를 통제할 수 있는 자는 천하무적이다.
[url=[Link deleted]pills price[/url]
프라그마틱 슬롯에 대한 설명 정말 감사합니다! 더불어, 제 사이트에서도 프라그마틱과 관련된 내용을 찾아보세요. 함께 발전하며 더 많은 지식을 얻어가요!
<a href="[Link deleted]홈페이지
프라그마틱 슬롯에 대한 내용이 정말 도움이 되었어요! 더불어, 제 사이트에서도 프라그마틱과 관련된 정보를 찾아보세요. 함께 서로 이야기하며 더 많은 지식을 쌓아가요!
[Link deleted]
[Link deleted]
[Link deleted]
Заказать купленный диплом, не выходя из дома.
Доступные цены на дипломы для продажи, подробности здесь.
Купить диплом с гарантией качества, важная информация.
Опыт успешной покупки диплома, все секреты.
Купить диплом легко, без риска.
Купить диплом по выгодной цене, интересные варианты.
Купить диплом срочно и недорого, спешите.
Скрытая покупка дипломов, проверенные решения.
Как быстро купить диплом, срочно и выгодно.
Покупка диплома: безопасность и качество, подробности у нас.
Официальные документы для покупки, гарантированное качество.
Легальная покупка дипломов, подробности на сайте.
Купить диплом без обмана, гарантированный результат.
Как выбрать и купить диплом, подробности на сайте.
Купить диплом без риска, гарантированная доставка.
Купить дипломы легко, гарантированный результат.
Официальная покупка диплома, подробности здесь.
Почему стоит заказать диплом на нашем сайте, безопасность на первом месте.
купить диплом [url=[Link deleted].
Приобрести диплом без лишних хлопот, онлайн.
Доступные цены на дипломы для продажи, без заморочек.
Купить диплом с гарантией качества, советы от профессионалов.
Опыт успешной покупки диплома, подробности.
Как купить диплом безопасно, с гарантией.
Купить диплом по выгодной цене, интересные варианты.
Дипломы на заказ по лучшим ценам, подробности на сайте.
Скрытая покупка дипломов, важная информация.
Где купить действующий диплом, срочно и выгодно.
Как купить диплом онлайн, гарантированный результат.
Почему стоит купить диплом у нас, гарантированное качество.
Легальная покупка дипломов, лучшие условия.
Официальные дипломы для покупки, гарантированный результат.
Дипломы на всех условиях, подробности на сайте.
Легальная покупка дипломов безопасно, безопасность на первом месте.
Какой диплом выбрать для покупки, интересные варианты.
Заказать диплом онлайн без проблем, подробности здесь.
Как купить диплом безопасно и быстро, подробности у нас.
купить диплом [url=7arusak-diploms.com]7arusak-diploms.com[/url] .
Приобрести диплом без лишних хлопот, не выходя из дома.
Доступные цены на дипломы для продажи, узнайте сейчас.
Какой диплом купить, советы от профессионалов.
Опыт успешной покупки диплома, рассказываем.
Где купить диплом без проблем, без риска.
Лучшие предложения по покупке диплома, важные моменты.
Купить диплом срочно и недорого, подробности на сайте.
Скрытая покупка дипломов, наши преимущества.
Как быстро купить диплом, только актуальная информация.
Купить диплом срочно и законно, подробности у нас.
Почему стоит купить диплом у нас, гарантированное качество.
Как купить диплом срочно, лучшие условия.
Купить диплом без обмана, подробности у нас.
Дипломы на всех условиях, лучшие предложения.
Легальная покупка дипломов безопасно, безопасность на первом месте.
Купить дипломы легко, подробности на сайте.
Официальная покупка диплома, подробности здесь.
Как купить диплом безопасно и быстро, гарантированный результат.
купить диплом [url=[Link deleted].
Thanks for sharing your thoughts. I truly appreciate your efforts and I will be waiting for your next post thank you once again.
<a href=[Link deleted]
<a href=[Link deleted]
Cá Cược Thể Thao Trực Tuyến RGBET
Thể thao trực tuyến RGBET cung cấp thông tin cá cược thể thao mới nhất, như tỷ số bóng đá, bóng rổ, livestream và dữ liệu trận đấu. Đến với RGBET, bạn có thể tham gia chơi tại sảnh thể thao SABA, PANDA SPORT, CMD368, WG và SBO. Khám phá ngay!
Giới Thiệu Sảnh Cá Cược Thể Thao Trực Tuyến
Những sự kiện thể thao đa dạng, phủ sóng toàn cầu và cách chơi đa dạng mang đến cho người chơi tỷ lệ cá cược thể thao hấp dẫn nhất, tạo nên trải nghiệm cá cược thú vị và thoải mái.
Sảnh Thể Thao SBOBET
SBOBET, thành lập từ năm 1998, đã nhận được giấy phép cờ bạc trực tuyến từ Philippines, Đảo Man và Ireland. Tính đến nay, họ đã trở thành nhà tài trợ cho nhiều CLB bóng đá. Hiện tại, SBOBET đang hoạt động trên nhiều nền tảng trò chơi trực tuyến khắp thế giới.
Xem Chi Tiết »
Sảnh Thể Thao SABA
Saba Sports (SABA) thành lập từ năm 2008, tập trung vào nhiều hoạt động thể thao phổ biến để tạo ra nền tảng thể thao chuyên nghiệp và hoàn thiện. SABA được cấp phép IOM hợp pháp từ Anh và mang đến hơn 5.000 giải đấu thể thao đa dạng mỗi tháng.
Xem Chi Tiết »
Sảnh Thể Thao CMD368
CMD368 nổi bật với những ưu thế cạnh tranh, như cung cấp cho người chơi hơn 20.000 trận đấu hàng tháng, đến từ 50 môn thể thao khác nhau, đáp ứng nhu cầu của tất cả các fan hâm mộ thể thao, cũng như thoả mãn mọi sở thích của người chơi.
Xem Chi Tiết »
Sảnh Thể Thao PANDA SPORT
OB Sports đã chính thức đổi tên thành "Panda Sports", một thương hiệu lớn với hơn 30 giải đấu bóng. Panda Sports đặc biệt chú trọng vào tính năng cá cược thể thao, như chức năng "đặt cược sớm và đặt cược trực tiếp tại livestream" độc quyền.
Xem Chi Tiết »
Sảnh Thể Thao WG
WG Sports tập trung vào những môn thể thao không quá được yêu thích, với tỷ lệ cược cao và xử lý đơn cược nhanh chóng. Đặc biệt, nhiều nhà cái hàng đầu trên thị trường cũng hợp tác với họ, trở thành là một trong những sảnh thể thao nổi tiếng trên toàn cầu.
Xem Chi Tiết »
<a href="[Link deleted]カジノ 絵師
このブログのファンになりました!素晴らしい情報源です。
[url=[Link deleted]accutane online canada pharmacy[/url]
[url=[Link deleted]ventolin online no prescription[/url]
[url=[Link deleted]you buy amoxicillin over the counter uk[/url]
<a href=[Link deleted]2024
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
[url=[Link deleted]500 tablet[/url]
[url=[Link deleted]price[/url]
국외선물의 출발 골드리치증권와 함께하세요.
골드리치는 길고긴기간 회원분들과 함께 선물마켓의 행로을 공동으로 동행해왔으며, 회원님들의 안전한 자금운용 및 알찬 수익률을 지향하여 항상 최선을 기울이고 있습니다.
왜 20,000+명 초과이 골드리치와 동참하나요?
신속한 서비스: 쉽고 빠른속도의 프로세스를 마련하여 누구나 용이하게 이용할 수 있습니다.
보안 프로토콜: 국가당국에서 사용하는 높은 등급의 보안체계을 도입하고 있습니다.
스마트 인가절차: 모든 거래내용은 부호화 처리되어 본인 외에는 그 누구도 내용을 접근할 수 없습니다.
확실한 수익률 공급: 리스크 부분을 낮추어, 보다 한층 확실한 수익률을 공개하며 그에 따른 리포트를 공유합니다.
24 / 7 지속적인 고객센터: 연중무휴 24시간 즉각적인 상담을 통해 투자자분들을 모두 뒷받침합니다.
제휴한 파트너사: 골드리치증권는 공기업은 물론 금융계들 및 다수의 협력사와 함께 여정을 했습니다.
국외선물이란?
다양한 정보를 알아보세요.
외국선물은 외국에서 거래되는 파생금융상품 중 하나로, 명시된 기초자산(예: 주식, 화폐, 상품 등)을 바탕로 한 옵션 계약을 지칭합니다. 근본적으로 옵션은 명시된 기초자산을 미래의 특정한 시점에 일정 가격에 사거나 팔 수 있는 자격을 제공합니다. 외국선물옵션은 이러한 옵션 계약이 외국 마켓에서 거래되는 것을 의미합니다.
외국선물은 크게 매수 옵션과 풋 옵션으로 구분됩니다. 콜 옵션은 명시된 기초자산을 미래에 정해진 가격에 사는 권리를 허락하는 반면, 매도 옵션은 명시된 기초자산을 미래에 정해진 금액에 팔 수 있는 권리를 허락합니다.
옵션 계약에서는 미래의 명시된 일자에 (만기일이라 불리는) 정해진 금액에 기초자산을 사거나 매도할 수 있는 권리를 보유하고 있습니다. 이러한 가격을 행사 금액이라고 하며, 만료일에는 해당 권리를 행사할지 여부를 선택할 수 있습니다. 따라서 옵션 계약은 투자자에게 미래의 가격 변동에 대한 안전장치나 수익 창출의 기회를 허락합니다.
해외선물은 마켓 참가자들에게 다양한 운용 및 매매거래 기회를 마련, 환율, 상품, 주식 등 다양한 자산유형에 대한 옵션 계약을 포함할 수 있습니다. 거래자는 풋 옵션을 통해 기초자산의 낙폭에 대한 안전장치를 받을 수 있고, 콜 옵션을 통해 활황에서의 이익을 타깃팅할 수 있습니다.
외국선물 거래의 원리
실행 가격(Exercise Price): 국외선물에서 행사 금액은 옵션 계약에 따라 특정한 가격으로 약정됩니다. 만기일에 이 금액을 기준으로 옵션을 실현할 수 있습니다.
만료일(Expiration Date): 옵션 계약의 만기일은 옵션의 행사가 불가능한 마지막 일자를 지칭합니다. 이 날짜 다음에는 옵션 계약이 만료되며, 더 이상 거래할 수 없습니다.
매도 옵션(Put Option)과 콜 옵션(Call Option): 매도 옵션은 기초자산을 지정된 가격에 매도할 수 있는 권리를 허락하며, 콜 옵션은 기초자산을 특정 금액에 매수하는 권리를 제공합니다.
옵션료(Premium): 해외선물 거래에서는 옵션 계약에 대한 옵션료을 지불해야 합니다. 이는 옵션 계약에 대한 가격으로, 마켓에서의 수요량와 공급에 따라 변동됩니다.
실행 방안(Exercise Strategy): 거래자는 종료일에 옵션을 실행할지 여부를 선택할 수 있습니다. 이는 마켓 상황 및 투자 플랜에 따라 상이하며, 옵션 계약의 수익을 극대화하거나 손해를 감소하기 위해 결정됩니다.
마켓 위험요인(Market Risk): 해외선물 거래는 마켓의 변동성에 작용을 받습니다. 시세 변화이 기대치 못한 진로으로 일어날 경우 손실이 발생할 수 있으며, 이러한 마켓 리스크를 감소하기 위해 투자자는 전략을 수립하고 투자를 계획해야 합니다.
골드리치와 동반하는 외국선물은 안전하고 확신할 수 있는 운용을 위한 가장좋은 선택입니다. 투자자분들의 투자를 뒷받침하고 안내하기 위해 우리는 전력을 다하고 있습니다. 함께 더 나은 미래를 지향하여 전진하세요.
<a href="[Link deleted]
이어 칙령을 내린 내시 앞에서 치우징이 칙령을 공개했다.
[url=[Link deleted]for lyrica 75 mg[/url]
[url=[Link deleted]for sale usa[/url]
[url=[Link deleted]you buy furosemide over the counter in canada[/url]
[url=[Link deleted]medication[/url]
<a href=[Link deleted]
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
[url=[Link deleted]azithromycin online[/url]
[url=[Link deleted]pharmacy[/url]
<a href="[Link deleted]
Zhu Houzhao는 Fang Jifan을 신중하게 바라 보았습니다. "그래서 Lao Fang이 의미하는 것은 …"
<a href=[Link deleted]
해외선물의 시작 골드리치와 동참하세요.
골드리치는 오랜기간 투자자분들과 함께 선물시장의 진로을 공동으로 여정을했습니다, 회원님들의 안전한 투자 및 높은 수익성을 향해 계속해서 전력을 기울이고 있습니다.
무엇때문에 20,000+인 이상이 골드리치증권와 동참하나요?
신속한 서비스: 간단하며 빠른 프로세스를 갖추어 누구나 수월하게 활용할 수 있습니다.
안전보장 프로토콜: 국가기관에서 적용한 상위 등급의 보안체계을 도입하고 있습니다.
스마트 인증: 모든 거래내용은 암호화 보호되어 본인 외에는 그 누구도 정보를 열람할 수 없습니다.
안전 수익성 공급: 리스크 부분을 감소시켜, 더욱 한층 확실한 수익률을 제시하며 이에 따른 리포트를 공유합니다.
24 / 7 지속적인 고객센터: året runt 24시간 신속한 지원을 통해 투자자분들을 모두 뒷받침합니다.
함께하는 파트너사: 골드리치증권는 공기업은 물론 금융기관들 및 많은 협력사와 공동으로 동행해오고.
외국선물이란?
다양한 정보를 참고하세요.
외국선물은 해외에서 거래되는 파생상품 중 하나로, 특정 기초자산(예시: 주식, 화폐, 상품 등)을 바탕로 한 옵션 약정을 지칭합니다. 기본적으로 옵션은 특정 기초자산을 향후의 어떤 시기에 일정 금액에 매수하거나 팔 수 있는 권리를 부여합니다. 국외선물옵션은 이러한 옵션 계약이 해외 시장에서 거래되는 것을 의미합니다.
국외선물은 크게 콜 옵션과 매도 옵션으로 구분됩니다. 콜 옵션은 특정 기초자산을 미래에 정해진 금액에 사는 권리를 허락하는 반면, 풋 옵션은 명시된 기초자산을 미래에 일정 금액에 매도할 수 있는 권리를 제공합니다.
옵션 계약에서는 미래의 명시된 일자에 (만료일이라 불리는) 정해진 금액에 기초자산을 매수하거나 팔 수 있는 권리를 보유하고 있습니다. 이러한 금액을 실행 금액이라고 하며, 만료일에는 해당 권리를 행사할지 여부를 선택할 수 있습니다. 따라서 옵션 계약은 거래자에게 미래의 가격 변동에 대한 안전장치나 수익 창출의 기회를 허락합니다.
국외선물은 마켓 참가자들에게 다양한 투자 및 매매거래 기회를 열어주며, 외환, 상품, 주식 등 다양한 자산군에 대한 옵션 계약을 포함할 수 있습니다. 투자자는 풋 옵션을 통해 기초자산의 하향에 대한 보호를 받을 수 있고, 콜 옵션을 통해 호황에서의 수익을 겨냥할 수 있습니다.
국외선물 거래의 원리
행사 금액(Exercise Price): 외국선물에서 행사 금액은 옵션 계약에 따라 지정된 금액으로 약정됩니다. 만료일에 이 가격을 기준으로 옵션을 행사할 수 있습니다.
종료일(Expiration Date): 옵션 계약의 만료일은 옵션의 행사가 불가능한 최종 일자를 의미합니다. 이 일자 이후에는 옵션 계약이 소멸되며, 더 이상 거래할 수 없습니다.
매도 옵션(Put Option)과 매수 옵션(Call Option): 매도 옵션은 기초자산을 지정된 가격에 팔 수 있는 권리를 허락하며, 콜 옵션은 기초자산을 지정된 금액에 사는 권리를 부여합니다.
옵션료(Premium): 해외선물 거래에서는 옵션 계약에 대한 프리미엄을 납부해야 합니다. 이는 옵션 계약에 대한 비용으로, 시장에서의 수요량와 공급에 따라 변경됩니다.
행사 방안(Exercise Strategy): 거래자는 종료일에 옵션을 행사할지 여부를 판단할 수 있습니다. 이는 시장 환경 및 투자 전략에 따라 상이하며, 옵션 계약의 수익을 최대화하거나 손실을 최소화하기 위해 결정됩니다.
마켓 리스크(Market Risk): 외국선물 거래는 시장의 변동성에 효과을 받습니다. 가격 변화이 기대치 못한 진로으로 일어날 경우 손실이 발생할 수 있으며, 이러한 마켓 위험요인를 감소하기 위해 거래자는 전략을 수립하고 투자를 계획해야 합니다.
골드리치와 함께하는 국외선물은 보장된 신뢰할 수 있는 운용을 위한 가장좋은 대안입니다. 투자자분들의 투자를 지지하고 인도하기 위해 우리는 최선을 다하고 있습니다. 함께 더 나은 미래를 향해 나아가요.
[url=[Link deleted]propecia australia[/url]
[url=[Link deleted]price south africa[/url]
[url=[Link deleted]dexamethasone[/url]
[url=[Link deleted]250[/url]
프라그마틱의 게임은 항상 다양한 테마로 놀라워요. 이 사이트에서 더 자세한 정보를 찾아보세요!
<a href="[Link deleted]슬롯 무료
프라그마틱의 빙고 게임은 항상 즐겁고 흥미로워요. 여기에서 더 많은 빙고 게임 정보를 확인하세요!
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]zithromax z-pak[/url]
국외선물의 출발 골드리치증권와 동참하세요.
골드리치는 길고긴기간 고객님들과 더불어 선물마켓의 진로을 함께 걸어왔으며, 고객분들의 보장된 자금운용 및 알찬 수익률을 향해 언제나 최선을 다하고 있습니다.
어째서 20,000+명 이상이 골드리치와 함께할까요?
신속한 솔루션: 쉽고 빠른속도의 프로세스를 갖추어 어느누구라도 수월하게 사용할 수 있습니다.
안전보장 프로토콜: 국가기관에서 사용하는 높은 등급의 보안시스템을 적용하고 있습니다.
스마트 인증: 전체 거래데이터은 암호처리 보호되어 본인 이외에는 아무도 누구도 내용을 열람할 수 없습니다.
안전 이익률 공급: 리스크 부분을 낮추어, 보다 한층 안전한 수익률을 제공하며 이에 따른 리포트를 제공합니다.
24 / 7 상시 고객지원: 연중무휴 24시간 즉각적인 지원을 통해 투자자분들을 모두 뒷받침합니다.
함께하는 동반사: 골드리치증권는 공기업은 물론 금융권들 및 다수의 협력사와 함께 여정을 했습니다.
국외선물이란?
다양한 정보를 확인하세요.
해외선물은 외국에서 거래되는 파생금융상품 중 하나로, 지정된 기반자산(예: 주식, 화폐, 상품 등)을 기초로 한 옵션 약정을 의미합니다. 근본적으로 옵션은 지정된 기초자산을 미래의 특정한 시점에 정해진 가격에 매수하거나 매도할 수 있는 권리를 제공합니다. 외국선물옵션은 이러한 옵션 계약이 외국 마켓에서 거래되는 것을 뜻합니다.
외국선물은 크게 콜 옵션과 풋 옵션으로 나뉩니다. 콜 옵션은 지정된 기초자산을 미래에 일정 가격에 매수하는 권리를 부여하는 반면, 풋 옵션은 명시된 기초자산을 미래에 일정 가격에 팔 수 있는 권리를 허락합니다.
옵션 계약에서는 미래의 명시된 날짜에 (종료일이라 불리는) 일정 가격에 기초자산을 사거나 팔 수 있는 권리를 가지고 있습니다. 이러한 가격을 실행 가격이라고 하며, 만기일에는 해당 권리를 실행할지 여부를 결정할 수 있습니다. 따라서 옵션 계약은 거래자에게 미래의 가격 변동에 대한 안전장치나 이익 창출의 기회를 제공합니다.
국외선물은 시장 참가자들에게 다양한 투자 및 매매거래 기회를 열어주며, 환율, 상품, 주식 등 다양한 자산군에 대한 옵션 계약을 포함할 수 있습니다. 투자자는 풋 옵션을 통해 기초자산의 낙폭에 대한 안전장치를 받을 수 있고, 콜 옵션을 통해 상승장에서의 이익을 노릴 수 있습니다.
외국선물 거래의 원리
행사 가격(Exercise Price): 외국선물에서 행사 금액은 옵션 계약에 따라 명시된 가격으로 약정됩니다. 종료일에 이 금액을 기준으로 옵션을 실현할 수 있습니다.
만료일(Expiration Date): 옵션 계약의 만료일은 옵션의 행사가 허용되지않는 마지막 날짜를 의미합니다. 이 날짜 다음에는 옵션 계약이 만료되며, 더 이상 거래할 수 없습니다.
풋 옵션(Put Option)과 매수 옵션(Call Option): 풋 옵션은 기초자산을 지정된 가격에 매도할 수 있는 권리를 허락하며, 매수 옵션은 기초자산을 지정된 가격에 사는 권리를 부여합니다.
프리미엄(Premium): 국외선물 거래에서는 옵션 계약에 대한 프리미엄을 지불해야 합니다. 이는 옵션 계약에 대한 비용으로, 시장에서의 수요와 공급량에 따라 변동됩니다.
행사 방식(Exercise Strategy): 투자자는 종료일에 옵션을 실행할지 여부를 판단할 수 있습니다. 이는 시장 환경 및 거래 플랜에 따라 상이하며, 옵션 계약의 수익을 극대화하거나 손해를 감소하기 위해 결정됩니다.
시장 리스크(Market Risk): 해외선물 거래는 시장의 변화추이에 작용을 받습니다. 시세 변화이 예상치 못한 방향으로 발생할 경우 손실이 발생할 수 있으며, 이러한 시장 위험요인를 감소하기 위해 거래자는 계획을 수립하고 투자를 계획해야 합니다.
골드리치와 동반하는 해외선물은 보장된 확신할 수 있는 투자를 위한 가장좋은 옵션입니다. 투자자분들의 투자를 지지하고 안내하기 위해 우리는 최선을 다하고 있습니다. 함께 더 나은 내일를 향해 나아가요.
[url=[Link deleted]diflucan no prescription[/url]
[url=[Link deleted]for pain[/url]
[url=[Link deleted]can i buy nolvadex[/url]
<a href="[Link deleted]
양가의 젊은 주인은 만지기 쉽지 않고 여전히 그의 집세를 빚지고 있습니다.
[url=[Link deleted]bactrim[/url]
<a href="[Link deleted]カジノ リベート
初めてこのブログを読みましたが、すぐにファンになりました。楽しみにしています!
[url=[Link deleted]250 mg price in india[/url]
[url=[Link deleted]in india[/url]
[url=[Link deleted]150 mg price[/url]
[url=[Link deleted]generic accutane[/url]
[url=[Link deleted]mg baclofen[/url]
<a href="[Link deleted]
Fang Jifan은 고개를 들고 Liu Jian이 그를 의심스럽게 바라보는 것을 보았습니다.
[url=[Link deleted]tablets[/url]
[url=[Link deleted]generic brand[/url]
<a href="[Link deleted]
하지만 동시에 마음속에 숨겨진 걱정을 느끼지 않을 수 없었다.
[url=[Link deleted]online canada[/url]
[url=[Link deleted]azithromycin online[/url]
프라그마틱플레이의 다채로운 슬롯으로 특별한 순간을 즐겨보세요.
<a href="[Link deleted]슬롯
프라그마틱 관련 내용 정말 재미있게 읽었어요! 또한, 제 사이트에서도 프라그마틱과 관련된 정보를 공유하고 있어요. 함께 교류하며 더 많은 지식을 쌓아가요!
[Link deleted]
[Link deleted]
[Link deleted]
[url=[Link deleted]retin a no prescription fast shipping[/url]
<a href="[Link deleted]
즉시 … Qi Zhiyuan은 진지한 표정으로 말했습니다. "자금 동원은 어떻게 진행되고 있습니까?"
you’re truly a just right webmaster. The web site loading speed is incredible. It seems that you’re doing any unique trick. Moreover, The contents are masterpiece. you’ve performed a wonderful task in this topic!
<a href=[Link deleted]online
[url=[Link deleted]1200 mg daily[/url]
[url=[Link deleted]much is augmentin 625mg[/url]
[url=[Link deleted]gel[/url]
[url=[Link deleted]augmentin online usa[/url]
<a href="[Link deleted]k8
素晴らしい記事でした。いつも新しい発見があって感謝しています!
[url=[Link deleted]purchase[/url]
<a href="[Link deleted]
Hongzhi 황제와 그의 신하들은 나를보고 나는 당신을 봅니다.
<a href="[Link deleted]カジノ レート
実用性が高く、読んでよかったです。素晴らしい記事です!
[url=[Link deleted]40 mg generic[/url]
<a href="[Link deleted]
"아버지." Shen Ao는 행복하게 앞으로 나아갔습니다. "아버지가 왜 여기에 있습니까?"
<a href="[Link deleted]
Zhu Houzhao는 깜짝 놀랐고 즉시 긴장했습니다. "그럼 서둘러, 서둘러."
Useful information. Fortunate me I found your website by chance, and I’m surprised why this accident didn’t took place earlier! I bookmarked it.
<a href=[Link deleted]
<a href="[Link deleted]
그렇게 말하면서 그는 무심코 찻잔 두 개가 놓인 책상 옆으로 다가갔다.
Картинка Диплом О Высшем Образовании
Для этого Вам нужно лишь выбрать и оформить заказ на нашем сайте. Для этого Вам нужно лишь выбрать и оформить заказ на нашем сайте. Мы предлагаем купить диплом в Пятигорске, который будет максимально схож с оригиналом высшего учебного заведения. Купить диплом о высшем образовании в Тольятти с нашей компанией можно очень быстро и просто. Купить диплом о высшем образовании в Норильске с нашей компанией можно очень быстро и просто. Он пройдет любую проверку на подлинность. Фото – Диплом магистра 2004-2009 года Сейчас купить диплом в Туле или любом другом регионе России не так сложно, можно прибегнуть к картинкам Диплом О Высшем Образовании сайтов объявлений, или найти фирму и приобрести диплом.
<a href=[Link deleted]Нужно Ли Подтверждать Диплом Медсестры
Магистратура – это возможность получить более качественное образование, позволяющее в дальнейшем работать по специальности. В этом случае нет ничего предосудительного в том, чтобы воспользоваться нашими услугами. Наличие образования это не просто требование работодателя, а непременное условие на нынешнем рынке труда.
Как Выглядит Аттестат За 9 Класс 2023
Международная деятельность Отдел по международным связям Лингвистический образовательный центр Обучение иностранных граждан Университеты-партнеры For Foreign Citizens. Диплом доктора наук Диплом кандидата наук Международный диплом Диплом магистра Диплом бакалавра Диплом специалиста Диплом мл. специалиста Диплом о переподготовке. Каждый управленец должен обладать базовыми знаниями, но это вовсе не означает, что их можно получить только в стенах высшего учебного заведения.
[url=[Link deleted]pharmacy[/url]
<a href="[Link deleted]
Liang Ruying은 Fang Jifan을 보았을 때 서둘러 절하고 스승의 의식을 수행했습니다.
<a href="[Link deleted]
천 장사를 하려는 상인들은 먼저 천을 구입해야 합니다.
<a href="[Link deleted]
두 사람은 봉천사 주변을 거닐다가 누군가 그들 앞에 달려드는 것을 보았다.
<a href="[Link deleted]
폐하는 정말 원시적이고 예측할 수 없으며 감탄, 감탄입니다!
<a href="[Link deleted]
Hongzhi 황제의 눈에는 "다행히 인생은 수치스럽지 않고 위대한 승리입니다! "라는 여섯 단어가 분명히 나타났습니다.
<a href="[Link deleted]오브 올림푸스
Zhou Tao는 현재 상황을 생각하면서 우울한 얼굴을 가졌습니다. 이 대출은 절대 상환해서는 안됩니다.
<a href="[Link deleted]
주된 이유는 그들이 이 거대한 괴물에 겁을 먹고 항상 이곳이 안전하지 않다고 느끼기 때문입니다.
В нашем обществе, где диплом является началом отличной карьеры в любом направлении, многие стараются найти максимально простой путь получения образования. Необходимость наличия официального документа переоценить невозможно. Ведь именно диплом открывает дверь перед людьми, стремящимися начать профессиональную деятельность или продолжить обучение в высшем учебном заведении.
Наша компания предлагает максимально быстро получить этот необходимый документ. Вы можете купить диплом, что становится удачным решением для человека, который не смог закончить обучение или потерял документ. дипломы выпускаются аккуратно, с особым вниманием к мельчайшим деталям. В итоге вы сможете получить 100% оригинальный документ.
Превосходство подобного решения заключается не только в том, что можно оперативно получить диплом. Весь процесс организован комфортно и легко, с профессиональной поддержкой. От выбора подходящего образца документа до точного заполнения персональной информации и доставки в любой регион страны — все будет находиться под полным контролем опытных мастеров.
Всем, кто ищет оперативный способ получения необходимого документа, наша компания может предложить выгодное решение. Купить диплом – значит избежать продолжительного процесса обучения и сразу перейти к достижению собственных целей: к поступлению в ВУЗ или к началу успешной карьеры.
<a href=[Link deleted]
Thanks a bunch for sharing this with all of us you really understand what you are talking about! Bookmarked. Please also seek advice from my website =). We could have a hyperlink alternate contract between us
<a href=[Link deleted]Mar Energy
Do you have a spam issue on this blog; I also am a blogger, and I was curious about your situation; we have developed some nice practices and we are looking to swap methods with others, be sure to shoot me an e-mail if interested.
<a href=[Link deleted]company Venice Italy
<a href="[Link deleted]주소
“이미 알고 있습니다.” 왕수인은 침착하게 “당신은 말을 아주 잘합니다.”라고 말했다.
В нашем мире, где диплом – это начало успешной карьеры в любой области, многие пытаются найти максимально простой путь получения образования. Наличие официального документа переоценить невозможно. Ведь диплом открывает двери перед каждым человеком, желающим начать трудовую деятельность или продолжить обучение в высшем учебном заведении.
Наша компания предлагает очень быстро получить любой необходимый документ. Вы можете купить диплом нового или старого образца, и это будет выгодным решением для человека, который не смог завершить образование или утратил документ. дипломы изготавливаются с особой тщательностью, вниманием к мельчайшим деталям, чтобы на выходе получился продукт, полностью соответствующий оригиналу.
Преимущества этого подхода заключаются не только в том, что можно оперативно получить диплом. Процесс организовывается комфортно, с профессиональной поддержкой. От выбора нужного образца до грамотного заполнения персональной информации и доставки в любое место страны — все находится под абсолютным контролем качественных мастеров.
Всем, кто ищет быстрый и простой способ получить необходимый документ, наша компания предлагает выгодное решение. Купить диплом – это значит избежать длительного обучения и сразу перейти к достижению своих целей, будь то поступление в университет или начало карьеры.
<a href=[Link deleted]
<a href="[Link deleted]웨스트 골드
그러나 Fang Jifan은 “폐하, 저는 … 제가 말해야할지 말아야할지 모르겠습니다. “라고 말했습니다.
<a href="[Link deleted]
"손자의 병법이 중요한가요?" Fang Jifan은 잠시 생각했습니다.
<a href="[Link deleted]리치스
그러나 Hongzhi 황제를보고 … Fang Jifan은 즉시 “폐하, 걱정하지 마십시오 …”라고 말했습니다.
В нашем обществе, где диплом – это начало отличной карьеры в любом направлении, многие ищут максимально быстрый и простой путь получения качественного образования. Наличие официального документа переоценить просто невозможно. Ведь именно он открывает дверь перед любым человеком, который желает начать трудовую деятельность или продолжить обучение в университете.
В данном контексте мы предлагаем оперативно получить этот необходимый документ. Вы сможете купить диплом нового или старого образца, что является отличным решением для человека, который не смог закончить обучение или утратил документ. Любой диплом изготавливается аккуратно, с максимальным вниманием ко всем элементам. На выходе вы получите продукт, 100% соответствующий оригиналу.
Преимущества этого решения состоят не только в том, что вы сможете быстро получить свой диплом. Процесс организовывается комфортно, с профессиональной поддержкой. От выбора необходимого образца до точного заполнения персональных данных и доставки по России — все будет находиться под полным контролем наших специалистов.
Для тех, кто ищет быстрый способ получения требуемого документа, наша компания готова предложить выгодное решение. Купить диплом – это значит избежать длительного обучения и сразу переходить к достижению личных целей: к поступлению в университет или к началу успешной карьеры.
<a href=[Link deleted]диплом юриста
Wow that was unusual. I just wrote an extremely long comment but after I clicked submit my comment didn’t appear. Grrrr… well I’m not writing all that over again. Anyway, just wanted to say excellent blog!
@@G@@
<a href=[Link deleted]
<a href="[Link deleted]오브 올림푸스
모두가 기운을 내어 쌍안경을 들고 찾아다녔다.
I was able to find good advice from your blog articles.
@@G@@
<a href=[Link deleted]
сайт bitz casino
<a href=[Link deleted]битц казино
<a href="[Link deleted]도메인
그러나 그렇게 믿을 수 없어 보이는 사람이 실제로 사건을 철저히 조사했습니다.
<a href="[Link deleted]도그 하우스 메가웨이즈
Fang Xiaofan이 듣고 나서 그의 눈이 빛났습니다. “질문이 하나 더 있습니다 …”
Why users still make use of to read news papers when in this technological globe all is available on net?
<a href=[Link deleted]
Hey! Do you know if they make any plugins to safeguard against hackers? I'm kinda paranoid about losing everything I've worked hard on. Any tips?
Greetings I am so excited I found your site, I really found you by error, while I was browsing on Aol for something else, Anyways I am here now and would just like to say thanks for a fantastic post and a all round thrilling blog (I also love the theme/design), I don’t have time to look over it all at the moment but I have saved it and also added in your RSS feeds, so when I have time I will be back to read a great deal more, Please do keep up the great work.
<a href=[Link deleted]
What a material of un-ambiguity and preserveness of precious familiarity regarding unexpected emotions.
<a href="[Link deleted]슬롯 게임
Hongzhi 황제는 “이 스웨터의 출력은 어떻습니까? “라고 즐거워했습니다.
<a href="[Link deleted]킹
부끄럽게도 나는 아직 아버지가 있다는 사실을 거의 잊고 있었다.
What’s up, yes this post is truly good and I have learned lot of things from it concerning blogging. thanks.
<a href=[Link deleted]
<a href="[Link deleted]오브 아즈텍
Liu Jian은 찻잔을 들고 그를 바라보며 침착하게 말했습니다.
<a href="[Link deleted]뉴 베가스
곰곰이 생각해보니 홍치제가 마음에 이런 생각을 품은 것도 바로 이것 때문이었다.
<a href="[Link deleted]무료 사이트
여러 내시들이 급히 그를 누에방으로 데려갔다.
<a href="[Link deleted]슬롯
Xu Jing과 함께 오랫동안 해외를 방황한 끝에 그의 목표는 곧 달성될 것입니다.
It’s awesome to pay a quick visit this site and reading the views of all friends concerning this post, while I am also zealous of getting knowledge.
telegra.ph/Pokupka-diploma-SHag-v-budushchee-bez-usilij-05-14
we-are-family.ru/contact.htm
metkonstrukt.ru/kupit-kalitku/
raisenex.com/blogs/6172/Where-can-I-order-a-diploma-or-certificate-at-a
russiajoy.ru/page/12
Thanks for any other wonderful article. Where else may just anybody get that type of info in such a perfect means of writing? I have a presentation subsequent week, and I am at the search for such information.
self-test.ufoproger.ru/test/default/view/10?page-comments=10&per-page-comments=10
worldgonews.ru/page/37
ruyanamerica.com/News/News.cfm?NewsID=1003
marsaxlokkfc.com/200405/friendlies20042005.html
mybaltika.info/ru/print/587/7892/
Можете приобрести гантельные грифы на <a href=[Link deleted]недорогим ценамнеобходимой длины. В изготовлении надежных снарядов применяются инновационные марки металла. Грифы гантельные изготавливаются в трех популярных диаметрах. Комплектующие предназначены для силовых занятий и выполнены с разметкой для правильного размещения рук и накаткой для хвата. Изделия покрываются защитным составом хрома и никеля. Российская компания производит достойный ассортимент тренировочного инвентаря для дома и фитнес клуба. Это многофункциональный инструмент для силовых занятий в любых условиях.
I’m gone to say to my little brother, that he should also pay a quick visit this website on regular basis to obtain updated from latest information.
textualheritage.org/en/the-materials-of-the-conference-el-manusctipt-2014/82.html
financetimenews.ru/page/14/
http://www.360nhadep.com/tag/dong-tu-menh-hop-huong-nao/
avtovladelez.ru/page/4
sinopipefittings.com/e_Feedback/?page=10995
<a href="[Link deleted]슬롯
이것은 왕자님 같지 않고, 길거리의 거지라고 해도 과언이 아니다.
Hello! I know this is kinda off topic but I’d figured I’d ask. Would you be interested in trading links or maybe guest writing a blog post or vice-versa? My blog addresses a lot of the same topics as yours and I feel we could greatly benefit from each other. If you are interested feel free to shoot me an email. I look forward to hearing from you! Terrific blog by the way!
arsenalaction.com/forum/posting.php?mode=reply&f=4&t=1558
cuscino.vn/danh-muc/san-pham-khac/ruot-goi
indicouple.com/blogs/525/Where-to-buy-a-diploma-or-certificate-at-a-bargain?lang=tr_tr
politikforum.ru/member.php?u=13387008
triumph-flowers.ru/bukety-nevesty/yarkij-buket-nevesty/
I loved as much as you will receive carried out right here. The sketch is tasteful, your authored material stylish. nonetheless, you command get got an impatience over that you wish be delivering the following. unwell unquestionably come more formerly again as exactly the same nearly very often inside case you shield this increase.
clickandconnectclubs.com/index.php?do=/public/blog/view/id_119636/title_-2024/
katuganka.in.ua/forum/index.php?id=1062347
http://www.rrsclub.ru/member.php?tab=visitor_messaging&u=1164&page=7
forum.infinite-soul.org/viewtopic.php?p=52657
boxer-forum.ru/topic3653.html?view=next
An impressive share! I have just forwarded this onto a friend who had been conducting a little homework on this. And he in fact bought me breakfast simply because I found it for him… lol. So let me reword this…. Thank YOU for the meal!! But yeah, thanx for spending time to discuss this topic here on your website.
amisite.ru/phpBB2/memberlist.php?mode=joined&order=ASC&start=6850
ditichlichsuvanhoa.com/dttc/DEN-VA-DINH-CAO-DAI-a407.html
http://www.projetdexpert.fr/site/produits.php?categorie=5
stephenireland.com/charity/details.php?10-000-RAISED-FOR-FRANCIS-HOUSE-CHILDREN-S-HOSPICE-3
sewmir.ru/index.php?links_exchange=yes&page=479&show_all=yes
you’re really a excellent webmaster. The site loading pace is amazing. It seems that you are doing any distinctive trick. In addition, The contents are masterpiece. you have done a fantastic process on this topic!
reguitti.com.ua/services.html
obozrevatelevents.ru/page/11/
childtemperament.org/index.php?lang=es
familylevel.com/blogs/19/Why-is-the-demand-and-popularity-of-universities-decreasing-today
moysamogon.ru/comment-page-30/
Hi there, You’ve done a fantastic job. I’ll definitely digg it and personally recommend to my friends. I am sure they will be benefited from this website.
ufawedding.ru/forum/index.php?action=reminder
maisoncarlos.com/UserProfile/tabid/42/UserID/1942955/Default.aspx
dveribiz.ru/shop/vkhodnye-dveri/ekonom-klass/
websize.hu/webaruhaz-keszites/
effective-herbal-cure.com/hoodia-gordonii-extract/fast-fat-reduction.htm
<a href="[Link deleted]웨이즈 2
즉시 Zhu Houzhao는 소매에서 “자신을 찾으십시오”라는 편지지 사본을 꺼냈습니다.
Wow, awesome blog layout! How long have you been blogging for? you made blogging look easy. The overall look of your site is excellent, as well as the content!
<a href=[Link deleted]Mar Energy
<a href="[Link deleted]게임 무료
하지만…Xiao Jing은 정말 어떻게 봐야할지 몰랐습니다.
<a href="[Link deleted]슬롯
“두려워하지 마세요!” Fang Jifan이 그를 격려했습니다. “나는 죽을 수 없습니다!”
<a href="[Link deleted]커뮤
Liu Tianzheng은 깜짝 놀랐고 그의 턱은 충격으로 떨어지는 것 같았습니다.
Hey everyone,
I recently stumbled upon a coin called HGL on the TON network, and I found its address: EQASgMtBU2QP9JMRfR1jKeLcPMUUT2RGigp_cVcjQuCyaZDw
There are some whispers that this coin might see some significant developments soon, but it’s still pretty low-key. Here’s the link I found on GeckoTerminal: [Link deleted]
I got a bit curious and bought a small amount since the price is still quite low. Has anyone here heard anything about HGL or know more about what’s going on with this project? Would love to hear your thoughts!
Thanks!
<a href="[Link deleted]슬롯
“우리…우리…” 모두들 말을 잘못할까 두려워 떨었다.
<a href="[Link deleted]
Zhu Houzhao는 "당신은 이해하지 못합니다. 내가 명성을 원하지 않습니까?"
<a href="[Link deleted]슬롯 사이트
성을 바꾸고나서 이제부터 정말 평생 고개를 못들겠다.
<a href="[Link deleted]슬롯 사이트
그는 어쩔 수 없이 말했습니다. “전하…무슨…이게 무슨 뜻이죠?”
<a href="[Link deleted]검증
멈출 수없는 Hongzhi 황제도 쪼그리고 앉았습니다.
<a href="[Link deleted]메이저 사이트
간단히 말해서, 그는 북경의 몇몇 사람들과 비밀리에 장사를 했습니다.
<a href="[Link deleted]커뮤
“무슨 일이야?” 누군가 낮은 포르투갈어 목소리로 욕을 퍼부었다.
<a href="[Link deleted]슬롯
홍지 12년, 수많은 사람들의 운명을 결정짓는 시험이 마침내 시작되었다.
<a href="[Link deleted]보증
마음 속으로 외쳤어, 이건 속아서 죽는 리듬이야!
<a href="[Link deleted]슬롯
폐하의 성차가 아직 도착하지 않았고 여기가 엉망이고 모두가 분명히 기분이 좋습니다.
<a href="[Link deleted]사이트
Hongzhi 황제는 호랑이 얼굴을했습니다. “말도 안되는 소리 그만하세요.”
<a href="[Link deleted]토토
1에이커도 안 되는 땅인데 가격이 천정부지로 치솟고 있다.